International Journal of Sports and Exercise Medicine
The Original Compared with Terminal in Anterior or Posterior Cruciate Ligament Tear
Denglu Yan1,2*, Yancheng Song3, Zhaojie Wang4 and Zhi Zhang5
1Orthopaedics, The First Affiliated Hospital of Guangdong Pharmaceutical University, Nonglinxia Road, Guangzhou, 510030, People's Republic of China
2Orthopaedics, Shenzhen Nanshan hospital of Guangdong Medical University, Taoyuan Road, Shenzhen, 512182, People's Republic of China
3Orthopaedics, Third Hospital of Nanfang Medical University, Guangzhou 510630, People's Republic of China
4Orthopaedics, Yantai Hospital of Binzhou Medical College, Yantai 264100, People's Republic of China
5Orthopaedics, Third Hospital of Guangzhou Medical University, Guangzhou 5101500, People's Republic of China
*Corresponding author: Denglu Yan, Orthopaedics, The First Affiliated Hospital of Guangdong Pharmaceutical University, Nonglinxia Road, Guangzhou, Guangdong, 510030, People's Republic of China, E-mail: ydlywl@126.com
Int J Sports Exerc Med, IJSEM-1-023, (Volume 1, Issue 4), Research Article; ISSN: 2469-5718
Received: February 01, 2015 | Accepted: October 25, 2015 | Published: October 29, 2015
Citation: Yan D, Song Y, Wang Z, Zhang Z (2015) The Original Compared with Terminal in Anterior or Posterior Cruciate Ligament Tear. Int J Sports Exerc Med 1:023. 10.23937/2469-5718/1510023
Copyright: © 2015 Yan D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: It currently remains unclear why the anterior cruciate ligament (ACL) is most commonly torn from its proximal attachment on the femur and the posterior cruciate ligament (PCL) is torn from its distal attachment on the tibia. This study is designed to evaluate the difference of ligament attachment in bone through a comparison of the origin with the terminal ends in both the ACL and PCL.
Methods: A sample population of 203 knee patients was assessed through magnetic resonance imaging (MRI) and the difference of ACL/PCL femur and tibia attachment were evaluated, and a total of 1146 patients with an ACL injury of the knee and 112 patients with a PCL injury was assessed through MRI imaging and arthroscopy to evaluate the damage according to the specific tear location and type of ACL/PCL injury.
Results: The magnetic resonance imaging (MRI) of normal knee joint shows the ACL/PCL originates from the epiphyseal plate and inserts into the tibial and femur bone at a terminal attachment site. The patient research data suggests the ACL ruptures closer to its femoral attachment and PCL mostly ruptures closer to the tibial attachment.
Conclusion: This study revealed the ACL/PCL originated in the epiphyseal plate of distal femur and proximal tibia, and terminates in the tibial/femoral bone by fibrous ligament tissues that are directly grown into the bone. However, there were no fibrous ligament tissues directly grown into the originate bone of ACL/PCL in the femur and tibia. Comparing the terminal and originate structure of ACL/PCL, the originate site was more commonly the site of injury.
Keywords
Anterior cruciate ligament, Posterior cruciate ligament, Originate, Terminal, Epiphyseal plate, Attachment
Introduction
The Anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) play a vital role in maintaining normal knee function, which contributes to both anterior-posterior translation of the knee and rotational stability [1-3]. The ACL finds its origin on the medial surface of the lateral femoral condyle, runs an oblique course within the knee joint from lateral and posterior to medial and anterior, and inserts into a broad area of the central tibial plateau [4-7]. The PCL arises from a depression posterior to the intraarticular upper surface of the tibia anteromedial and behind the ACL to the lateral surface of the medial femoral condyle [8-11]. As a structure composed of numerous fascicles of dense connective tissue that connect the distal femur and the proximal tibia, the ACL and PCL (ACL/PCL) are prone to injury [12,13]. However, the overall structure and organization of a native ACL/PCL insertion site are not reproduced after ACL/PCL reconstruction and reflect an inability to recapitulate the events that occur during embryonic development with current surgical techniques [14-16].
The ACL is most commonly torn from its proximal attachment on the femur, and the PCL is most commonly torn from its distal attachment on the tibia [3,17-20]. The ACL/PCL inserts to bone via a direct type of insertion, similar to the transition seen from tendon to bone [4,7]. Microscopic examination of the sites of bony attachment show inter digitation of the collagen fibers with bone through four distinct transition zones: tendon, demineralized fibrocartilage, mineralized fibrocartilage, and bone [21]. This graduated change in stiffness allows for transmission of complex mechanical loads from soft tissue to bone while minimizing peak stresses at any single point along the ligament [21]. Cartilage-specific collagens including type II, VI, IX, X, and XI are found in the fibrocartilage insertion site. Collagen VI and X play key roles in maintaining the interface between mineralized and unmineralized zones [22-24].
A clear understanding of the anatomy of the native ACL/PCL is critical in determining the ligament will be reconstructed [7,25,26]. Improved awareness of the anatomy and biomechanical properties of the normal ACL/PCL may lead to improvements in techniques for ACL/PCL reconstruction and an associated improvement in outcomes over traditional results [27-29]. In view of the ACL/PCL formation and the location of injury, the origin of ACL/PCL may be involved in the mechanism of ACL is mostly torn from its proximal attachment on the femur and the PCL on the distal attachment of the tibia [30]. However, no research studies have been published in regards to this matter. In this study, it has been demonstrated that the ACL originates from the distal epiphyseal plate of femur and PCL originates from the proximal epiphyseal plate of tibia. The fibers of the ACL/PCL extend in opposing directions from the originate sites (forming the characteristic "x" shape) and become embedded into a broad area of the bone on the medial condyle surface. The anatomical structure of this terminal site is not the same as where it originates from the epiphyseal plate.
Materials and Methods
This study involved 203 patients with history of knee pain (ACL/PCL were normal) and 1146 patients with ACL torn and 112 patients with PCL torn. Magnetic resonance imaging (MRI) of the knee joint was taken after the clinical examination. MR imaging was performed with 1.5-T system (Phillips Medical Systems) at Institute of Radiology in the hospital. Two experienced radiologists reviewed the images blindly with no previous knowledge of patient history. The standardized MR imaging protocol consisted of sagittal, coronal and axial sequences, in section thickness of 3-5 mm. The ACL/PCL was considered normal when it appeared as a band of fibers of low to intermediate signal intensity on both sagittal and coronal dual images. The ACL/PCL was considered to be partially torn when there was abnormal signal intensity within the ligament or when otherwise intact fibers appeared wavy on sagittal or coronal dual images. The ACL/PCL was considered to be completely torn if there was disruption of all fibers or if it was not discernible at all on MRI. For statistical analysis purposes, we considered normal as one group and complete tears and partially torn ligaments as another group.
After the composite data of ACL/PCL images via MRI were collected and arthroscopy performed to confirm lesion location, the patients were divided into three categories: originate, middle, and terminal. Upon confirmation of the injury site, the type of lesions was grouped into two subcategories: ligament rupture and avulsion fractures from attachment (ACL avulsion fractures of tibia tubercle or PCL posterior tibia attachment site avulsion fractures). All arthroscopic procedures were performed under standard hospital policy, on consented patients, and by experienced arthroscopic surgeons. Operative findings were documented in the patient's official document, which included the survey of the entire joint and anatomical structure, lesions involved with the presence or absence of tear, its location, status of the cartilage and the tibiofemoral joint functionality.
Statistical Analysis
Statistical analyses were performed using SPSS Version 16.0 software. The data was expressed as the mean ± SD and was analyzed using analysis of variance (ANOVA). In the case of heterogeneity of variance, transformations were used to stabilize the variance. Results were considered statistically significant if the p value was less than 0.05 for continuous variables.
Results
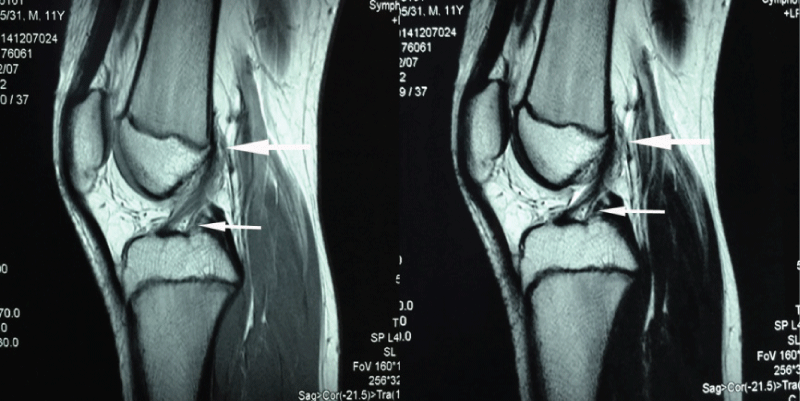
The MRI of ACL/PCL normal knee joint is shown in figure 1, 2, 3. The normal knee joint study group of 203 patients consisted of 137 men (67.5%) and 66 women (32.5%), and average age was 13.5 years (range: 8 - 15 years). The knee composite of the femur, tibia, ACL and PCL, and epiphyseal plate were shown clearly. The ACL finds its origin from epiphyseal plate on the medial surface of the lateral femoral condyle, runs an oblique course within the knee joint and inserts into the central tibial plateau (Figure 1).
.
Figure 1: MR images (sagittal view) of the ACL originate (big arrow) and terminate (small arrow). The big arrow indicates the ligament directed originate from the epiphyseal plate, and the small arrow indicates the ligament terminated the bone which it attachment.
View Figure 1
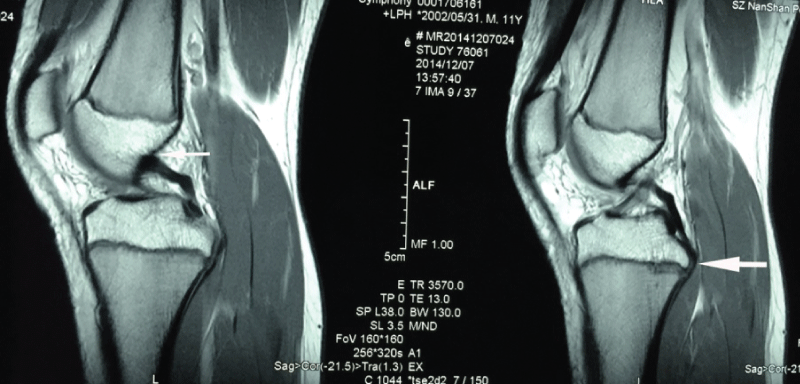
The PCL arises from a depression posterior to the intraarticular upper surface of the tibia epiphyseal plate and courses anteromedially behind the ACL and inserts into the medial femoral condyle (Figure 2).
.
Figure 2: MR images (sagittal view) of the PCL originate (big arrow) and terminate (small arrow). The big arrow indicates the ligament directed originate from the epiphyseal plate, and the small arrow indicates the ligament terminated the bone which it attachment.
View Figure 2
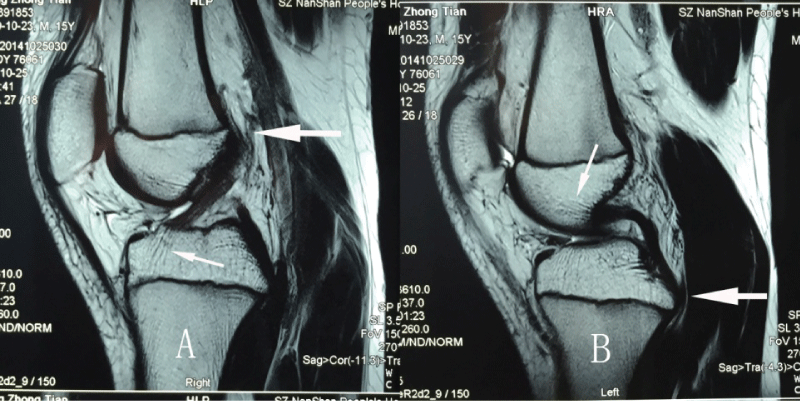
It's very clear that the ACL/PCL originated in the epiphyseal plate of distal femur and proximal tibia, and terminates in the tibia and femur by a fibrous ligament tissue directly grown into the bone tissue (Figure 3). However, there were no fibrous ligament tissue directly grown into the originate bone of ACL/PCL in femur and tibia.
.
Figure 3: MR images (sagittal view) of the ACL (A) and PCL (B) originates (big arrows) and terminates (small arrows). The big arrow indicates the ligament directed originate from the epiphyseal plate, and the small arrow indicates the ligament terminate fibrous tissue directly grown into the bone which it attachment.
View Figure 3
The data of patients with ACL/PCL lesion were shown in table 1. The study group of 1146 patients consisted of 769 men (67.1%) and 377 women (32.9%) in ACL and 112 patients consisted of 81 men (72.3%) and 31 women (27.7%) in PCL. The average age was 26.5 years (range: 15 - 47 years) in ACL and 29.3 years (range: 18 - 51 years) in PCL. Maximum number of patients (n = 746) who suffered knee injuries were in the age group of 21-30 years in ACL and 51 patients in 30 - 42 years in PCL. The right knee was involved in 635 cases (55.41%) and the left knee in 511 (44.59%) in ACL and 76 cases (62.81%) in right and 45 (37.19%) in left knee in PCL.
![]()
Table 1: The data of ACL/PCL ruptures patients
View Table 1
The ACL ruptures rate based on the MRI and arthroscopy criteria was 81.23% (931/1146) in the femur attachment, 9.34% (107/1146) in the middle, and 4.45% (51/1146) in the tibial attachment (P < 0.05). The PCL ruptures rate based on the MRI and arthroscopy criteria was 59.50% (72/121) in the tibial attachment, 13.22% (16/121) in the middle, and 11.57% (14/121) in the femur attachment (P < 0.05). There were no avulsion fractures in femur attachment of ACL and PCL, and 4.98% (57/1146) case of ACL avulsion fractures of tibial tubercle and 15.70% (19/121) cases of PCL avulsion fractures of posterior tibial attachment.
Discussion
The purpose of this study was to assess the original and terminal sites of the ACL/PCL. The ACL finds its origin on the medial surface of the lateral femoral condyle (LFC), runs an oblique course within the knee joint from lateral and posterior to medial and anterior, and inserts into a broad area of the central tibial plateau [31,32]. The PCL arises from a depression posterior to the intraarticular upper surface of the tibia and courses anteromedially behind the ACL to the lateral surface of the medial femoral condyle. In this study, the MRI examinations demonstrate the ACL originate from epiphyseal plate on the medial surface of the lateral femoral condyle and the PCL originate from the tibia epiphyseal plate. These findings show that there was a relative tendency of originate end to be the site of injury because it not as anchored as the terminal end of ACL/PCL.
The ACL is most commonly torn from its proximal attachment on the femur, and the PCL is most commonly torn from its distal attachment on the tibia [9,33]. A direct insertion is observed in the ACL/PCL whereby the ligament attaches to the bone, similar in the transition of tendon to bone [4,7]. Microscopic examination of the sites of bony attachment show inter digitation of the collagen fibers with bone through four distinct transition zones, and this graduated change in stiffness allows for transmission of complex mechanical loads from soft tissue to bone while minimizing peak stresses at any single point along the ligament [21,22,24]. In the current study, the ACL/PCL originated in the epiphyseal plate of distal femur and proximal tibia, and terminates in the tibia and femur by ligament fibrous tissue directly grown into the bone tissue.
A clear understanding of the anatomy of the native ACL/PCL is critical in determining the ligament will be reconstructed [34]. The discussion regarding the avulsion of the PCL from its femoral attachment is has not been studied with sufficient data [35]. However, the avulsion fracture of PCL tibial attachment were common [19]. A leading hypothesis holds that the ACL originates as a ventral condensation of the fetal blastula and gradually migrated posteriorly with the formation of the intercondylar space. Another proposed mechanism of fetal ACL formation is from a confluence between ligamentous collagen fibers and fibers of the periosteum. Rather than regenerating the four organized zones of direct insertion, the graft heals with an interposed zone of vascular, highly cellular granulation tissue between the graft and the tunnel wall.
In this study, the ACL ruptures mostly in the femur attachment and PCL mostly in tibial attachment. There were no avulsion fractures in femur attachment of ACL and PCL, and all avulsion fractures were in the tibial tubercle of ACL and in the posterior tibial attachment of PCL. These clinical data analyses were consistent with the MRI findings. Improved awareness of the anatomy and biomechanical properties of the normal ACL/PCL may lead to improvements in techniques for ACL/PCL reconstruction and an associated improvement in outcomes over traditional results [36,37].
Conclusions
The ACL/PCL originated in the epiphyseal plate of distal femur and proximal tibia, and terminates in the tibia and femur bone tissue by ligament fibrous tissue directly grown. However, there were no ligament fibrous tissue directly grown into the originate bone of ACL/PCL in femur and tibia. Comparing the terminal and originate structure of ACL/PCL, originate was much more easily prone to become injured.
Competing interests
The authors declare that they have no competing interests.
Authors' contributions
DY participated in the design of the study and drafted the manuscript. HZ, YS and ZW participated in the design of the study and coordination and helped to draft the manuscript. All authors read and approved the final manuscript.
Acknowledgement
This research was funded by National Natural Science Foundation of China (81271937) and Health and family planning commission of Shenzhen foundation (201302198).
References
-
Shefelbine SJ, Ma CB, Lee KY, Schrumpf MA, Patel P, et al. (2006) MRI analysis of in vivo meniscal and tibiofemoral kinematics in ACL-deficient and normal knees. J Orthop Res 24: 1208-1217.
-
Scarvell JM, Smith PN, Refshauge KM, Galloway H, Woods K (2005) Comparison of kinematics in the healthy and ACL injured knee using MRI. J Biomech 38: 255-262.
-
Yan D, Song Y, Pei F (2014) Allograft ligament transplantation in anterior cruciate ligament reconstruction patients with meniscal tears. Arch Orthop Trauma Surg 134: 521-527.
-
Smigielski R, Zdanowicz U, Drwiega M, Ciszek B, Ciszkowska-Lyson B, et al. (2014) Ribbon like appearance of the midsubstance fibres of the anterior cruciate ligament close to its femoral insertion site: a cadaveric study including 111 knees. Knee Surg Sports Traumatol Arthrosc 23: 3143-3150
-
Tantisricharoenkul G, Linde-Rosen M, Araujo P, Zhou J, Smolinski P, et al. (2014) Anterior cruciate ligament: an anatomical exploration in humans and in a selection of animal species. Knee Surg Sports Traumatol Arthrosc 22: 961-971.
-
Swami VG, Mabee M, Hui C, Jaremko JL (2014) MRI Anatomy of the Tibial ACL Attachment and Proximal Epiphysis in a Large Population of Skeletally Immature Knees: Reference Parameters for Planning Anatomic Physeal-Sparing ACL Reconstruction. Am J Sports Med 42: 1644-1651.
-
Triantafyllidi E, Paschos NK, Goussia A, Barkoula NM, Exarchos DA, et al. (2013) The shape and the thickness of the anterior cruciate ligament along its length in relation to the posterior cruciate ligament: a cadaveric study. Arthroscopy 29: 1963-1973.
-
Westermann RW, Sybrowsky C, Ramme AJ, Amendola A, Wolf BR (2013) Three-dimensional characterization of the femoral footprint of the posterior cruciate ligament. Arthroscopy 29: 1811-1816.
-
Van Hoof T, Cromheecke M, Tampere T, D'herde K, Victor J, et al. (2013) The posterior cruciate ligament: a study on its bony and soft tissue anatomy using novel 3D CT technology. Knee Surg Sports Traumatol Arthrosc 21: 1005-1010.
-
Miller MD, Harner CD (1995) The anatomic and surgical considerations for posterior cruciate ligament reconstruction. Instr Course Lect 44: 431-440.
-
Osti M, Tschann P, Kunzel KH, Benedetto KP (2012) Anatomic characteristics and radiographic references of the anterolateral and posteromedial bundles of the posterior cruciate ligament. Am J Sports Med 40: 1558-1563.
-
Song EK, Park HW2, Ahn YS, Seon JK3 (2014) Transtibial versus tibial inlay techniques for posterior cruciate ligament reconstruction: long-term follow-up study. Am J Sports Med 42: 2964-2971.
-
Lee DW, Jang HW, Lee YS, Oh SJ, Kim JY, et al. (2014) Clinical, Functional, and Morphological Evaluations of Posterior Cruciate Ligament Reconstruction With Remnant Preservation: Minimum 2-Year Follow-up. Am J Sports Med 42: 1822-1831.
-
Tompkins M, Keller TC, Milewski MD, Gaskin CM, Brockmeier SF, et al. (2013) Anatomic femoral tunnels in posterior cruciate ligament reconstruction: inside-out versus outside-in drilling. Am J Sports Med 41: 43-50.
-
Piontek T, Ciemniewska-Gorzela K, Szulc A, Naczk J, Wardak M, et al. (2013) Arthroscopically assisted combined anterior and posterior cruciate ligament reconstruction with autologous hamstring grafts-isokinetic assessment with control group. PLoS One 8: e82462.
-
Morgan CD, Kalman VR, Grawl DM (1997) The anatomic origin of the posterior cruciate ligament: where is it? Reference landmarks for PCL reconstruction. Arthroscopy 13: 325-331.
-
Meyers MH (1975) Isolated avulsion of the tibial attachment of the posterior cruciate ligament of the knee. J Bone Joint Surg Am 57: 669-672.
-
Xu X, Huang T, Liu Z, Wen H, Ye L, et al. (2014) Hamstring tendon autograft versus LARS artificial ligament for arthroscopic posterior cruciate ligament reconstruction in a long-term follow-up. Arch Orthop Trauma Surg 134: 1753-1759.
-
Singla R, Devgan A, Gogna P, Batra A (2014) Fixation of delayed union or non-union posterior cruciate ligament avulsion fractures. J Orthop Surg (Hong Kong) 22: 70-74.
-
Wasmaier J, Kubik-Huch R, Pfirrmann C, Grehn H, Bieg C, et al. (2013) Proximal anterior cruciate ligament tears: the healing response technique versus conservative treatment. J Knee Surg 26: 263-271.
-
Dai C, Guo L, Yang L, Wu Y, Gou J, et al. (2015) Regional fibrocartilage variations in human anterior cruciate ligament tibial insertion: a histological three-dimensional reconstruction. Connect Tissue Res 56: 18-24.
-
Durigan JL, Peviani SM, Delfino GB, de Souza Jose RJ, Parra T, et al. (2014) Neuromuscular electrical stimulation induces beneficial adaptations in the extracellular matrix of quadriceps muscle after anterior cruciate ligament transection of rats. Am J Phys Med Rehabil 93: 948-961.
-
Sardone F, Traina F, Tagliavini F, Pellegrini C, Merlini L, et al. (2014) Effect of mechanical strain on the collagen VI pericellular matrix in anterior cruciate ligament fibroblasts. J Cell Physiol 229: 878-886.
-
Stepien-Slodkowska M, Ficek K, Eider J, Leonska-Duniec A, Maciejewska-Karlowska A, et al. (2013) The +1245g/t polymorphisms in the collagen type I alpha 1 (col1a1) gene in polish skiers with anterior cruciate ligament injury. Biol Sport 30: 57-60.
-
Kennedy NI, Wijdicks CA, Goldsmith MT, Michalski MP, Devitt BM, et al. (2013) Kinematic analysis of the posterior cruciate ligament, part 1: the individual and collective function of the anterolateral and posteromedial bundles. Am J Sports Med 41: 2828-2838.
-
Mochizuki T, Fujishiro H, Nimura A, Mahakkanukrauh P, Yasuda K, et al. (2014) Anatomic and histologic analysis of the mid-substance and fan-like extension fibres of the anterior cruciate ligament during knee motion, with special reference to the femoral attachment. Knee Surg Sports Traumatol Arthrosc 22: 336-344.
-
Yim JH, Seon JK, Kim YK, Jung ST, Shin CS, et al. (2015) Anterior translation and rotational stability of anterior cruciate ligament-deficient knees during walking: speed and turning direction. J Orthop Sci 20: 155-162.
-
Yang DL, Cheon SH, Oh CW, Kyung HS (2014) A comparison of the fixation strengths provided by different intraosseous tendon lengths during anterior cruciate ligament reconstruction: a biomechanical study in a porcine tibial model. Clin Orthop Surg 6: 173-179.
-
Sun L, Wu B, Tian M, Liu B, Luo Y (2013) Comparison of graft healing in anterior cruciate ligament reconstruction with and without a preserved remnant in rabbits. Knee 20: 537-544.
-
Zauleck MK, Gabriel S, Fischmeister MF, Hirtler L (2014) Origin of the anterior cruciate ligament and the surrounding osseous landmarks of the femur. Clin Anat 27: 1103-1110.
-
Wan C, Hao ZX, Wen SZ (2014) The effect of the material property change of anterior cruciate ligament by ageing on joint kinematics and biomechanics under tibial varus/valgus torques. Biomed Mater Eng 24: 1375-1382.
-
Chhabra A, Starman JS, Ferretti M, Vidal AF, Zantop T, et al. (2006) Anatomic, radiographic, biomechanical, and kinematic evaluation of the anterior cruciate ligament and its two functional bundles. J Bone Joint Surg Am 88 Suppl 4: 2-10.
-
Tsukada S, Fujishiro H, Watanabe K, Nimura A, Mochizuki T, et al. (2014) Anatomic variations of the lateral intercondylar ridge: relationship to the anterior margin of the anterior cruciate ligament. Am J Sports Med 42: 1110-1117.
-
Udagawa K, Niki Y, Enomoto H, Toyama Y, Suda Y (2014) Factors influencing graft impingement on the wall of the intercondylar notch after anatomic double-bundle anterior cruciate ligament reconstruction. Am J Sports Med 42: 2219-2225.
-
Drucker MM, Wynne GF (1975) Avulsion of the posterior cruciate ligament from its femoral attachment: an isolated ligamentous injury. J Trauma 15: 616-617.
-
Lim BO, Shin HS, Lee YS (2014) Biomechanical comparison of rotational activities between anterior cruciate ligament- and posterior cruciate ligament-reconstructed patients. Knee Surg Sports Traumatol Arthrosc 23: 1231-1238.
-
Osti M, Krawinkel A, Gohm A, Muxel B, Benedetto KP (2014) The effectiveness of skeletal imaging for quality assessment in posterior cruciate ligament reconstruction: reliability and validity of radiographs and computed tomography. Arch Orthop Trauma Surg 134: 1731-1737.





