International Journal of Surgery Research and Practice
Videothoracoscopic Ligation of Bulla via Single Utility-Incision for Spontaneous Pneumothorax: A Convenient Surgical Approach in a Developing Country
Bo Wei1*, Jinfang Yi2 and Fusheng Jiang1
1Department of Thoracic Surgery, Beijing Shijitan Hospital, Capital Medical University, Beijing, People’s Republic of China
2Department of Surgery, People’s Hospital of Fucheng County, Hebei Province, People’s Republic of China
*Corresponding author:
Dr. Wei, Department of Thoracic Surgery, Beijing Shijitan Hospital Affiliated to Capital Medical University, No.10 Tieyi Road, Haidian District, Beijing, 100038, People’s Republic of China, Tel: +86 13651043973, E-mail: weibos@126.com
Int J Surg Res Pract, IJSRP-4-049, (Volume 4, Issue 1), Case Report; ISSN: 2378-3397
Received: May 18, 2016 | Accepted: February 22, 2017 | Published: February 25, 2017
Citation: Wei B, Yi J, Jiang F (2017) Videothoracoscopic Ligation of Bulla via Single Utility-Incision for Spontaneous Pneumothorax: A Convenient Surgical Approach in a Developing Country. Int J Surg Res Pract 4:049. 10.23937/2378-3397/1410049
Copyright: © 2017 Wei B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The ideal video thoracoscopic surgery for spontaneous pneumothorax should maximize the benefits of minimally invasive surgery but minimize the surgical cost; thereby reducing chest wall trauma using the fewest incisions and the least money possible without compromising therapeutic efficiency. Described here include a complete single utility-incision thoracoscopic approach and bulla ligation with a deep hypodesmus technique, so as to reduce the use of the multiple endostapling cartridges typically required during bulla resection. 31 patients with spontaneous pneumothorax were submitted to this technique during the past 6 years. All the processes were smoothly without any prolonged air leakage and recurrence up to now. We believe this technique can be considered a valid alternative to stapling technology during video thoracoscopic procedure for spontaneous pneumothorax, and could be widely recommended in the developing countries.
The ideal video thoracoscopic surgery for spontaneous pneumothorax should maximize the benefits of minimally invasive surgery, thereby minimizing chest wall trauma using the fewest incisions possible without compromising therapeutic efficiency. The routine utilized endostapling devices would add to the cost of the operation and present potential malfunction risks from dislodgement, user errors, mechanical failures, and application difficulties [1,2]. In light of our preliminary experience with a simple and secure ligation technique facilitating minithoracotomy [3], we also tested this approach in the case of pulmonary blebs or bullae management during thoracoscopic surgery. We hypothesize this non-GIA technique will reduce surgery costs. Here we describe the technique and the early outcomes afterward.
Keywords
Single-Access, Videothoracoscopic surgery, Bulla ligation, Pneumothorax
Operative Technique
Patient positioning and port placement
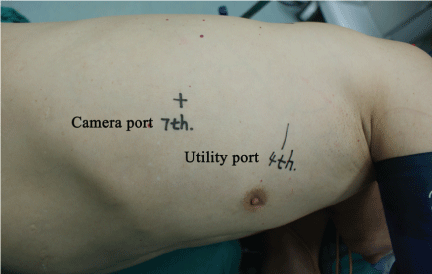
Patients were selected for this technique on the basis of the recurrent spontaneous pneumothorax and sometimes primary spontaneous pneumothorax, from poverty-stricken areas in China. The patient is placed in the maximally flexed lateral decubitus position; the surgeon and the assistant are both positioned on the anterior (abdominal) side of the patient, with the surgeon positioned cranially. This setup is independent of all the kinds of pneumothorax. Two incisions are used: a 3 cm-5 cm utility incision without rib spreading, and a camera port that is later used for chest tube placement (Figure 1). The soft tissues of the utility incision sometimes need to be separated by means of a retractor to facilitate passage of instruments in and out of the chest and to avoid loss of pneumothorax when suction is applied.
During the majority of the procedure, the surgeon operates in a bimanual fashion with one or two instruments in the utility incisions. The whole process is performed under total thoracoscopic visualization.
Ligation of bulla
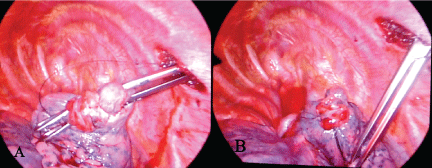
The rigid wall of the thoracic cavity provides an ideal cavity for minimally invasive surgery without the need for the cumbersome CO2 insufflation that is essential to perform laparoscopic surgery. And by that, the novel ligation technique facilitating minithoracotomy which we reported in 2009 [3], is possible to be tested during intrathoracic ligation process under thoracoscopic visualization. Rapid control of the visceral bulla by ligation is made possible with a common curved oval forceps clamping, followed by the new hypodesmus approach (Figure 2A). Once the suture begins to tighten, the oval forceps should be unclasped gradually and withdraw from the pleural cavity as well (Figure 2B). Afterwards, pleural abrasion is done to obliterate the pleural cavity. Pleurodesis was achieved by electrocauterizing the upper surface of the parietal pleura in a patchy fashion.
.
Figure 2: Intraoperative view of ligatured bulla in apex of right lung; A) Pulmonary bulla was clamped; B) Bulla ligation finished.
View Figure 2
Results
31 patients with spontaneous pneumothorax were submitted to this technique during the past 6 years. The median operational time and the length of stay were 1.5 hours, 4 days respectively. The whole process was smoothly without any prolonged air leakage and recurrence up to now.
Discussion
The established three-port VATS procedure for pneumothorax typically needs the use of multiple reloadable stapler cartridges. However, the mechanical stapling approach sometimes can be associated with stapler failure, resulting in bleeding [4], pulmonary parenchymal contusion, or staple line dehiscence, leading to hematoma or fistula [5]. In addition, the mechanical stapling devices require the use of multiple cartridge firings and will be associated with increased operative costs [6]. Whether it is worth using these highly expensive instruments must be questioned in depth. As early as 2009, we developed a novel knot-tying method promotes the expeditious formation of secure square knots in deep-seated operating fields via a small incision [3]. Now, we believe it can be considered a valid alternative to stapling technology during videothoracoscopic procedure sometimes. Most patients in this study came from remote, poverty-striking rural areas; they actually could not afford the endostapling devices. This cost-saving approach, for them, was the one and only way to cure their disease with minimally invasive surgery.
Not with standing three ports thoracoscopic surgery with stapling technology for spontaneous pneumothorax has been well established, our single utility-incision thoracoscopic technique without rib spreading can be considered a valid alternative in this setting. The use of this technique could potentially lead to decreased surgery costs by reducing the use of the multiple endostapling cartridges typically required during blebs or bullae resection. Larger prospective series with long-term results and cost/benefit analyses are necessary to better define the utility of this technology before its use can be widely recommended in the developing countries.
References
-
Chan D, Bishoff JT, Ratner L, Kavoussi LR, Jarrett TW (2000) Endovascular gastrointestinal stapler device malfunction during laparoscopic nephrectomy: early recognition and management. J Urol 164: 319-321.
-
Deng DY, Meng MV, Nguyen HT, Bellman GC, Stoller ML (2002) Laparoscopic linear cutting stapler failure. Urology 60: 415-419.
-
Bo W, Fusheng J, Tianyou W (2009) A novel ligation technique facilitating minithoracotomy. Ann Thorac Surg 88: 1989-1992.
-
Ruffini E, Oliaro A, Manusco M, Cavallo A, Filosso P, et al. (1994) Successful management of hemorrhage from the pulmonary artery stump after lobectomy for bronchogenic carcinoma. J Cardiovasc Surg 35: 257-259.
-
Asamura H, Kondo H, Tsuchiya R (2000) Management of the bronchial stump in pulmonary resections: A review of 533 consecutive recent bronchial closures. Eur J Cardiothorac Surg 17: 106-110.
-
Casali G, Walker WS (2009) Video-assisted thoracic surgery lobectomy: Can we afford it? Eur J Cardiothorac Surg 35: 423-428.