International Journal of Surgery Research and Practice
The Surgical Checklist Revisited
Caroline Daggett BA1* and Amanda Daggett MD2
1University of Mississippi School of Medicine, USA
2Cedars-Sinai Medical Center, USA
*Corresponding author:
Caroline Daggett, BA, First Year Medical Student, University of Mississippi School of Medicine, 2500 N. State Street, Jackson, MS 39216, USA, Tel: 601-953-4780, E-mail: cmdaggett1@gmail.com
Int J Surg Res Pract, IJSRP-4-051, (Volume 4, Issue 1), Case Report; ISSN: 2378-3397
Received: October 26, 2016 | Accepted: February 23, 2017 | Published: February 27, 2017
Citation: Caroline D, Amanda D (2017) The Surgical Checklist Revisited. Int J Surg Res Pract 4:051. 10.23937/2378-3397/1410051
Copyright: © 2017 Caroline D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
It is estimated that in-hospital adverse surgical events occur in the range of 3 to 17%. This paper reviews the use of surgical checklists as a tool for reducing preventable errors. It uses the work of Dr. Peter Pronovost, Dr. Atul Gawande, and the World Health Organization (WHO) to revisit the evidence-based proof that checklists do work in the right setting and under the right circumstances.
Keywords
Checklist, Surgical, Adverse events, Preventable, WHO, Pronovost, Gawande
It is estimated that over 250 million surgeries are performed worldwide every year [1]. Various studies from around the world estimate adverse events from hospital surgery occur in the range of 3 to 17% [2]. The cost in human lives and to healthcare systems is enormous. Positive disruptions to this unacceptably high complication rate were essentially non-existent until one physician created a simple checklist, which has impacted these errors in a very significant way. The use of the checklist in healthcare has been around for many years, but not until Dr. Peter Pronovost from Johns Hopkins Hospital developed such a list for the intensive care unit (ICU) did its impact have scientific data to demonstrate its usefulness.
Anesthesiologist and critical care specialist, Pronovost designed a small study using his checklist for central line placement, which had a very high infection rate in the ICU. Its implementation produced unexpected and dramatic results, a reduction of the ten-day infection rate from 11 to 0%. Despite these staggering results and his efforts to spread his data and message around the country, many were skeptical of his one-hospital conclusions. However, two years later, the Michigan Health and Hospital Association approached Pronovost about expanding his study in their state. This became known as the Keystone Initiative [3]. Results from the state of Michigan's use of a checklist in their ICUs showed an infection rate reduction of 66%, saving 175 million dollars and 1500 lives [4].
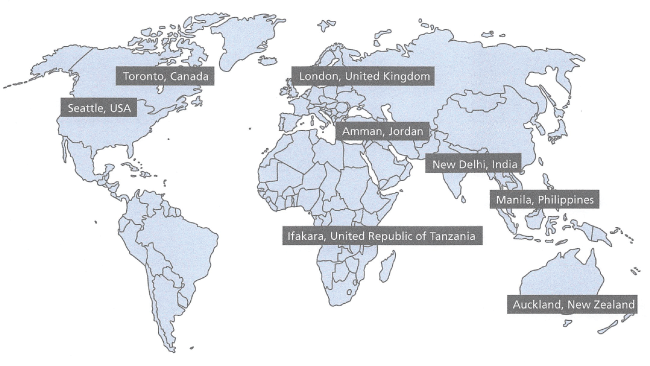
In 2007, the World Health Organization (WHO) convened an international group consisting of doctors, nurses, patients, and safety experts to address ways to reduce preventable, adverse events in surgical patients. From this initial meeting came the Safe Surgery Saves Lives Program and Checklist. The group then tested the checklist in a pilot study in eight hospitals around the world with differing economic status and resources (Figure 1).
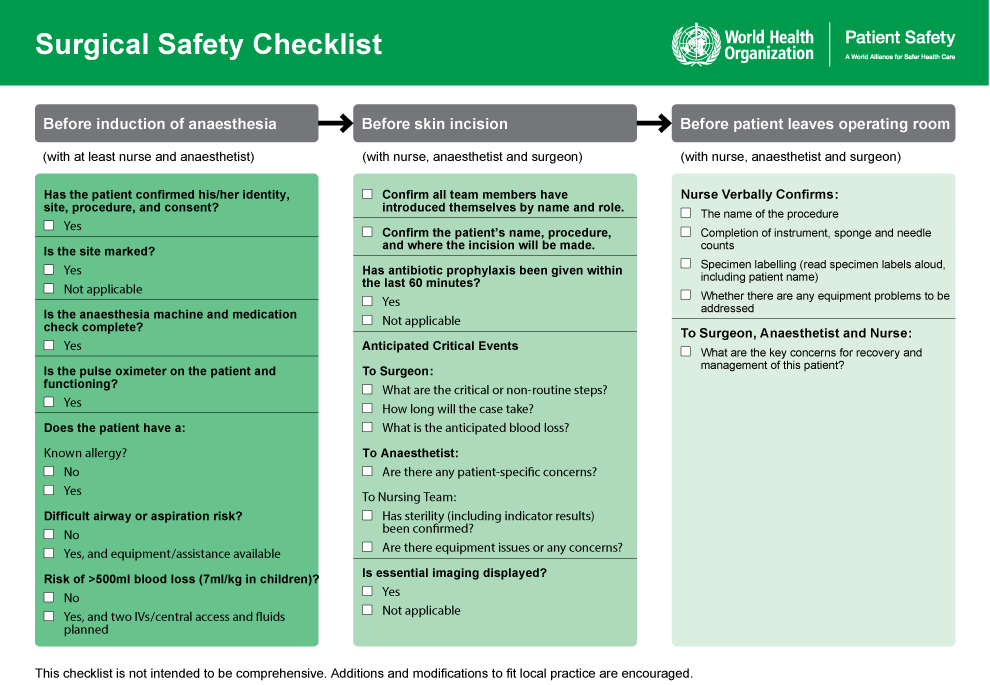
Again, the positive results were remarkable. Infection rates dropped by one-third and death rates were halved [5]. Released in 2008, the WHO recommended all hospitals adopt the 19-item Surgical Safety Checklist [6]. The National Health Service (NHS) in the United Kingdom (UK) required all of its treatment centers to implement it, and some 2,000 hospitals worldwide have since tried it [7]. The list has been modified to fit specific procedures by different hospitals and organizations such as the Mayo Clinic, Brigham and Women's Hospital, and the Society of Thoracic Surgeons just to name a few [6] (Figure 2).
One of the members of the Safe Surgery Saves Lives Team and a leader of the pilot study conducted by the WHO was Atul Gawande, a surgeon at the Brigham and Women's Hospital in Boston. Dr. Gawande published The Checklist Manifesto: How to Get Things Right in 2009 [3]. The book brought national and world attention to the checklist as a safety mechanism for reducing errors and adverse events. That same year, the checklist even made an appearance on NBC's ER [6].
Despite the early success achieved from the use of checklists, there has been reluctance from healthcare team members to embrace their usage, and replication of these results has been difficult to produce in some hospitals. There are a number of factors influencing the success of the checklist. For example, how the checklist is introduced has been an important component to its success. Success is more likely if administration officials are invested in implementation to the same degree as the team in the surgical theatre. Consequently, the WHO has worked to develop an adaptation guide to improve its usage based on the hospital, its resources, and its staff [6]. The field of implementation science is also looking at this phenomenon in order to improve usage and success. What appears to happen is oftentimes the staff do not see the benefit of the checklist and feel it is cumbersome to use, slowing them down with patient care. Therefore, they choose not to use it. On the other hand, when the staff was asked, "If they were having an operation would they want the checklist to be used? ...93% said yes" [3].
There is also something termed the normalization of deviance that occurs within organizations and has been identified among healthcare teams [7]. It is defined as: "The gradual process through which unacceptable practice or standards become acceptable. As the deviant behavior is repeated without catastrophic results, it becomes the social norm for the organization". This has been vividly demonstrated in a UK study of 7,000 surgical procedures at five NHS hospitals. The researchers found the checklist was available to the team in 97% of the surgical cases but was only implemented 62% of the time [8,9]. Failure to complete the checklist with no adverse consequences desensitized the team, and the practice of not using the list became the norm. In contrast, other research shows that as checklist compliance increases, i.e., as more items on the checklist are completed, the lower the complication rate and the better the outcomes [10].
Surgical safety checklists do work. From Peter Pronovost's study in 2001 until today, the evidence is clear. Better outcomes occur when a checklist is in place and properly executed. Fittingly, checklist use has spread to other fields such as obstetrics, radiology, cardiology, and dermatology. Through diligent investigation, most of the obstacles to the universal use of checklists have been identified and are being addressed on the local, national, and global level. Quality management teams are being formed to develop strategies for overcoming the challenges of incorporating the checklist into the clinical setting [11]. As this evolves, evidence supports the checklist's pivotal role in achieving the goal of reducing preventable errors to zero across all aspects of medicine.
References
-
Weiser TG, Regenbogen SE, Thompson KD, Haynes AB, Lipsitz SR, et al. (2008) An estimation of the global volume of surgery: A modelling strategy based on available data. Lancet 372: 139-144.
-
Walker IA, Reshamwalla S, Wilson IH (2012) Surgical safety checklists: do they improve outcomes? Br J Anaesth 109: 47-54.
-
Gawande A (2009) The Checklist Manifesto: How to Get Things Right. New York: Metropolitan.
-
Pronovost P, Needham D, Berenholtz S, Sinopoli D, Chu H, et al. (2006) An Intervention to Decrease Catheter-Related Bloodstream Infections in the ICU. N Engl J Med 355: 2725-2732.
-
Haynes AB, Weiser TG, Berry WR, Lipsitz SR, Breizat AH, et al. (2009) A Surgical Safety Checklist to Reduce Morbidity and Mortality in a Global Population. N Engl J Med 360: 491-499.
-
(2016) Safesurg.org.
-
Banja J (2010) The normalization of deviance in healthcare delivery. Bus horiz 53: 139.
-
Anthes E (2015) Hospital Checklists Are Meant to Save Lives-So Why Do They Often Fail? Nature 523: 516-518.
-
Mayer EK, Sevdalis N, Rout S, Caris J, Russ S, et al. (2016) Surgical Checklist Implementation Project. Ann Surg 263: 58-63.
-
Stephanie J Russ , Nick Sevdalis, Krishna Moorthy, Erik K Mayer, Shantanu Rout, et al. (2015) A Qualitative Evaluation of the Barriers and Facilitators Toward Implementation of the WHO Surgical Safety Checklist Across Hospitals in England. Ann Surg 261: 81-91.
-
Weiser TG, Haynes AB, Lashoher A, Dziekan G, Boorman DJ, et al. (2010) Perspectives in quality: Designing the WHO Surgical Safety Checklist. Int J Qual Health Care 22: 365-370.