International Journal of Surgery Research and Practice
Percutaneous Closure of an Atrial Septal Defect in a Child with Congenitally Corrected Transposition of Great Arteries
Hasim Olgun* and Naci Ceviz
Division of Pediatric Cardiology, Department of Pediatrics, Ataturk University, Erzurum, Turkey
*Corresponding author: Haşim Olgun, Division of Pediatric Cardiology, Department of Pediatrics, Ataturk University, Erzurum, 29 Blok, No: 5, 25240 Erzurum, Turkey, Tel: +90-442-3446848, Fax: +90-442-2361301, E-mail: drholgun@hotmail.com
Int J Surg Res Pract, IJSRP-4-052, (Volume 4, Issue 1), Case Report; ISSN: 2378-3397
Received: January 26, 2017 | Accepted: March 17, 2017 | Published: March 20, 2017
Citation: Olgun H, Ceviz N (2017) Percutaneous Closure of an Atrial Septal Defect in a Child with Congenitally Corrected Transposition of Great Arteries. Int J Surg Res Pract 4:052. 10.23937/2378-3397/1410052
Copyright: © 2017 Olgun H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Congenitally corrected transposition of the great arteries with a hemodynamically significant isolated atrial septal defect is rare. The treatment includes surgical or transcatheter closure techniques. With the introduction of percutaneous closure devices, close associated cardiac defects have been achieved without increasing the risk of surgery. Herein, we report a pediatric case of congenitally corrected transposition of the great arteries with atrial septal defect which was successfully closed using an atrial septal occluder.
Keywords
Congenitally corrected transposition of the great arteries, Children, Atrial septal defect, Transcatheter closure, Supraventricular tachycardia
Introduction
Congenitally corrected transposition of the great arteries (ccTGA), also known as ventricular inversion (VI), is an uncommon cardiac malformation characterized by atrioventricular (AV) and ventriculoarterial (VA) discordance [1]. It accounts for approximately 0.5% of clinically apparent congenital heart diseases [1]. In this anomaly, the right atrium enters the morphological left ventricle (LV), which gives a rise to the pulmonary artery, and the left atrium communicates with the morphological right ventricle (RV), which gives a rise to the aorta. Thus, AV and VA discordance exists, and although the blood flows in the normal direction, it passes through the false ventricular chamber [2]. Therefore, this double discordance results in the term ccTGA, which is, indeed, a misnomer. It can be associated with other congenital cardiac abnormalities. Congenitally corrected transposition of the great arteries with an isolated atrial septal defect (ASD) is rare [1,3]. In patients with ccTGA, cardiac surgery poses certain risks, particularly related to the conduction system [4]. The development of percutaneous closure devices potentially offers the opportunity to close associated cardiac defects without increasing the risk of surgery. To the best of our knowledge, transcatheter closure of ASD in children with ccTGA has not been reported previously. Herein, we report a pediatric case of ccTGA with an ASD which was successfully closed using an atrial septaloccluder (ASO).
Case Report
A 12-year-old patient with ccTGA and hemodynamically significant ostium secundum type ASD was followed annually with transthoracic echocardiography in our outpatient clinic. Lately, his exercise capacity began to decline, and mild right-sided morphological mitral valve regurgitation developed. Transesophageal echocardiography (TEE) demonstrated a single ASD. The maximum diameter of the ASD was measured as 16 mm on TEE. The rims of the defect were found to be adequate. In particular, the pulmonary AV valve (structurally the mitral valve) had an enough long rim.
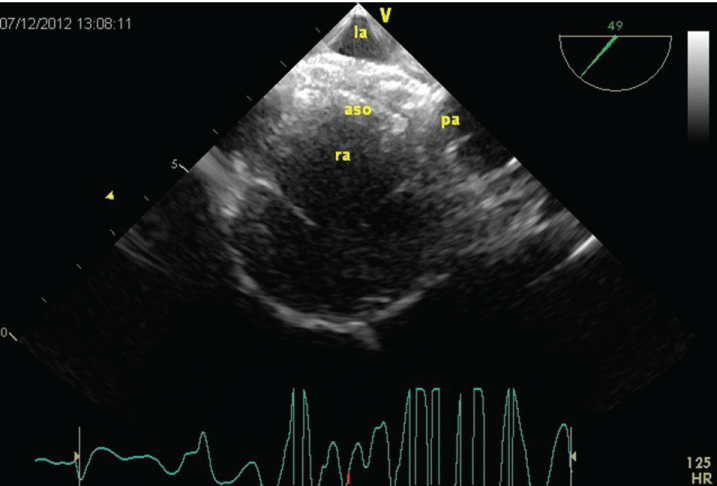
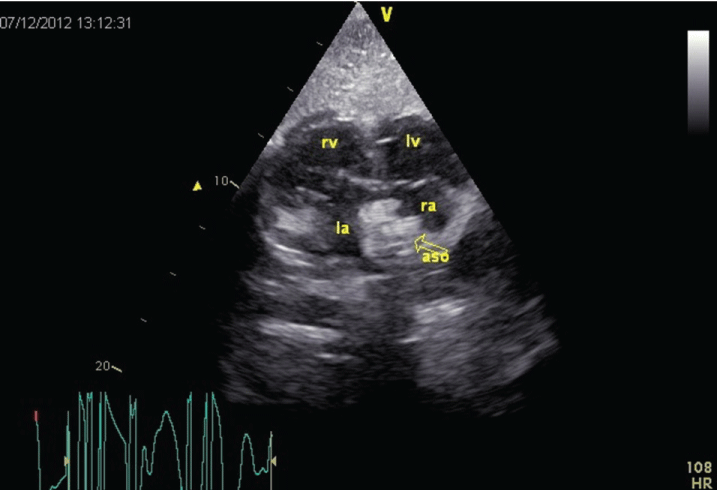
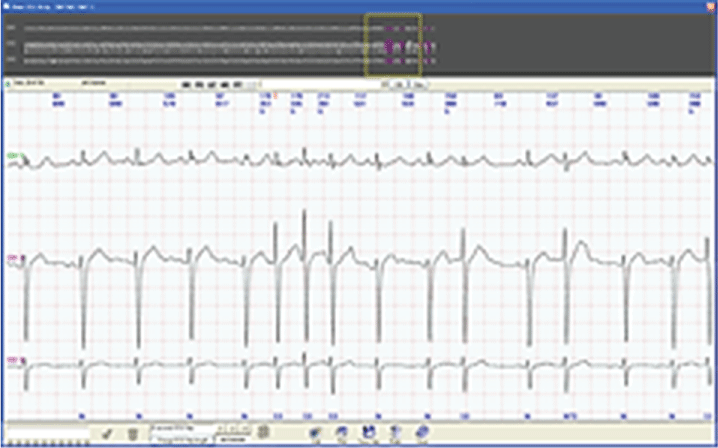
A written informed consent was obtained from the parents. The patient underwent transcatheter closure under general anesthesia and TEE guidance. The left and right heart catheterization showed a significant intra-cardiac shunt (Qp/Qs = 2.41) on oximetry with normal pulmonary artery pressures. The ASD was sized as 17.5 mm with scope during balloon sizing. A 19 mm Amplatzer (AGA Medical Corporation, MN, USA) septal occluder was deployed successfully with good stability without any evidence of a residual intra-cardiac shunt (Figure 1). Final TEE confirmed that the device was in its proper position with a satisfactory capture of all the rims without no residual shunt or no contact with the AV valves (Figure 2). During the first 24-hour of closure, the patient developed palpitation. A 24-hour Holter monitorization revealed frequent supraventricular premature beats (SVPCs), couplets, and non-sustained supraventricular tachycardia (NSVT) episodes (Figure 3).
.
Figure 1: A transesophageal echocardiographic image showing the atrial septal occluder with a good stability. aso: atrial septal occluder, la: left atrium, pa: pulmonary artery, ra: right atrium.
View Figure 1
.
Figure 2: A transesophageal echocardiographic subcostal four-chamber view of the device. aso: atrial septal occluder, la: left atrium, lv: left ventricle, ra: right atrium, rv: right ventricle.
View Figure 2
The patient was discharged from hospital on the next day with anti-platelet therapy of aspirin and beta-blocker therapy of metaprolol. At the first week, palpitations resolved. The first month 24-hour Holter monitorization showed seldom supraventricular couplets and no supraventricular runs. At three months, echocardiographic examination showed mild tricuspid valve regurgitation, and disappearance of the mitral regurgitation. Anti-arrhythmic drugs were discontinued at six months, and arrhythmia did not relapse. At three years following ASD closure, echocardiographic examination and 24-hour Holter monitorization findings were normal.
.
Figure 3: Non-sustained supraventricular tachycardia on 24-hour Holter monitorization.
View Figure 3
Discussion
Patients with ccTGA have both AV and VA discordance, thereby, leading to a morphological RV and delicate tricuspid valve in the systemic position [2]. Associated defects, such as abnormalities of the tricuspid valve, ventricular septal defect (VSD), and pulmonary stenosis occur in the majority of patients [5]. A hemodynamically significant isolated ASD is rarely accompanied by ccTGA [5]. The management of ccTGA with an isolated ASD depends on the age of the patient, anatomy of the tricuspid valve, and systemic right ventricular functions.
In patients with ccTGA, cardiac surgery poses certain risks. Surgically induced complete heart block was a common cause of morbidity early in the history of surgical treatment of ccTGA, after the closure of VSDs, in particular [5]. Cardiac surgery can also precipitate generalized ventricular dysfunction and tricuspid regurgitation. Mild preoperative tricuspid regurgitation may become severe postoperatively even in patients in whom the tricuspid valve is not manipulated [3].
The safety and efficacy of percutaneous secundum ASD closure have been well-established in children [6,7]. Percutaneous ASD occlusion offers many advantages over surgical closure, including avoidance of cardiopulmonary bypass and sternotomy scars, shorter hospitalization length, and a potentially lower incidence of post-procedural complications [7]. In addition, percutaneous transcatheter closure is related to lesser detrimental psychological effects [7]. Indeed, the absence of skin scars, shorter hospitalization length, and avoidance of admission to an intensive care unit are widely appreciated by both patients and parents. There may be also some advantages during follow-up; the absence of a scar on atrial myocardium may reduce the incidence of incisional arrhythmias [7]. On the other hand, device closure is not risk-free, and some device-related complications including nickel allergy, cardiac conduction abnormalities, valvular damage, and device endocarditismay develop. Although rare, some of these complications may be potentially life-threatening and result in sudden death, even [6,8].
In recent years, ASDs of secundum type in patients with otherwise normal heart have been closed using percutaneous devices with a low procedural morbidityrate [7]. However, its efficiency in children with ccTGA still remains to be elucidated. To the best of our knowledge, no reported pediatric case in this research field is available in the literature. Hence, this is the first case of transcatheter ASD closure in a child with ccTGA.
Nonetheless, ASD closure in patients with ccTGA may have certain challenges, compared to ASD closure in patients with otherwise normal heart. The posterior margin in hearts with ccTGA is shorter than in normal heart. The coronary sinus isthmus is also significantly shorter. Also, the coronary sinus opening into the right atrium is on the same side of the eustachian valve, as the inferior caval veinin patients with ccTGA.
During transcatheter closure, the shorter posterior septal margin can result several difficulties during the device placement. The shorter coronary sinus isthmus and its abnormal location opening in some of these hearts may pose a challenge for the displacement of the device and obstruction the coronary sinus orifice [9]. The aforementioned anatomical atrial abnormalities can make the procedure more challenging than in ASD closure of an otherwise normal heart. Therefore, Careful imaging with TEE and precise device sizing are of utmost importance for the procedural success.
On the other hand, device thrombosis and cardiac erosion are the most severe late complications of the device closure of an ASD, whereas atrial arrhythmias are the most common complications [10]. Transient complete AV block, transient junctional rhythm was reported during the procedure [11]. Supraventricular and ventricular premature beats and intermittent sinus arrest was demonstrated by 24-hour ambulatory electrocardiography monitoring Hill, et al. [11]. Also demonstrated that ambulatory Holter monitoring immediately following transcatheter closure of an ASD was associated with a statistically significant increase in SVPBs, including NSVT. In patients without pre-existent arrhythmias, the rate of atrial fibrillation increases after closure, as shown in the recently published Danish nationwide cohort. These authors reported that patients with an ASD had a higher risk of new-onset of atrial arrhythmias after closure; however, no significant difference was found between transcatheter and surgical approaches [12]. In patients with closure before the age of 25 years, atrial fibrillation developed in 21% during follow-up [13]. Frequent SVPC, couplets, and NSVT episodes were established on Holter monitorization in our case following the transcatheter closure. We believe that SVPCs and SVT were related to the device placement, and NSVT improved with anti-arrhythmic therapy. However, there is a limited number of data on how to manage such arrhythmias in the literature [14]. A few number of articles offers management with anti-arrhythmic drugs, whereas refractory cases can be treated using catheter ablation [15].
In conclusion, our case suggests that transcatheter closure of an ASD is acceptable for pediatric cases with ccTGA. By this way, one can avoid from the possible harmful effects of open heart surgery. However, patients must be closely monitored for possible atrial arrhythmias.
References
-
Atallah J, Rutledge JM, Dyck JD (2013) Congenitally corrected transposition of the great arteries (Atrioventricular and ventriculoarterial discordance). In: Allen HD, Driscoll DJ, Shaddy RE, Feltes TF, Moss and Adams' Heart Disease in infants, children and adolescents including the fetus and young adults. (8th edn), Lippincott Williams, Philadelphia, 1147-1158.
-
Warnes CA (1996) Congenitally corrected transposition: the uncorrected misnomer. J Am Coll Cardiol 27: 1244-1245.
-
Graham TP Jr, Bernard YD, Mellen BG, Celermajer D, Baumgartner H, et al. (2000) Long-term outcome in congenitally corrected transposition of the great arteries: a multi-institutional study. J Am Coll Cardiol 36: 255-261.
-
Wilkinson JL, Smith A, Lincoln C, Anderson RH (1978) Conducting tissues in congenitally corrected transposition with situs inversus. Br Heart J 40: 41-48.
-
Warnes CA (2006) Transposition of the great arteries. Circulation 114: 2699-2709.
-
Jalal Z, Hascoet S, Baruteau AE, Iriart X, Kreitmann B, et al. (2016) Long-term Complications After Transcatheter Atrial Septal Defect Closure: A Review of the Medical Literature. Can J Cardiol 32: 1315.e11-1315.e18.
-
Butera G, De Rosa G, Chessa M, Rosti L, Negura DG, et al. (2003) Transcatheter closure of atrial septal defect in young children: results and follow-up. J Am Coll Cardiol 42: 241-245.
-
Reddy BT, Patel JB, Powell DL, Michaels AD (2009) Interatrial shunt closure devices in patients with nickel allergy. Catheter Cardiovasc Interv 74: 647-651.
-
Juneja R, Rowland E, Ho SY (2002) Atrial morphology in hearts with congenitally corrected transposition of the great arteries: implications for the interventionist. J Cardiovasc Electrophysiol 13: 158-163.
-
Szkutnik M, Lenarczyk A, Kusa J, Białkowski J (2008) Symptomatic tachy- and bradyarrhythmias after transcatheter closure of interatrial communications with Amplatzer devices. Cardiol J 15: 510-516.
-
Hill SL, Berul CI, Patel HT, Rhodes J, Supran SE, et al. (2000) Early ECG abnormalities associated with transcatheter closure of atrial septal defects using the Amplatzer septal occluder. J Interv Card Electrophysiol 4: 469-474.
-
Du ZD, Hijazi ZM, Kleinman CS, Silverman NH, Larntz K, et al. (2002) Comparison between transcatheter and surgical closure of secundum atrial septal defect in children and adults: results of a multicenter nonrandomized trial. J Am Coll Cardiol 39: 1836-1844.
-
Kutty S, Hazeem AA, Brown K, Danford CJ, Worley SE, et al. (2012) Long-term (5 to 20-year) outcomes after transcatheter or surgical treatment of hemodynamically significant isolated secundum atrial septal defect. Am J Cardiol 109: 1348-1352.
-
Khairy P, Van Hare GF, Balaji S, Berul CI, Cecchin F, et al. (2014) PACES/HRS expert consensus statement on the recognition and management of arrhythmias in adult congenital heart disease: developed in partnership between the Pediatric and Congenital Electrophysiology Society (PACES) and the Heart Rhythm Society (HRS). Endorsed by the governing bodies of PACES, HRS, the American College of Cardiology (ACC), the American Heart Association (AHA), the European Heart Rhythm Association (EHRA), the Canadian Heart Rhythm Society (CHRS), and the International Society for Adult Congenital Heart Disease (ISACHD). Can J Cardiol 30: e1-e63.
-
Li X, Wissner E, Kamioka M, Makimoto H, Rausch P, et al. (2014) Safety and feasibility of transseptal puncture for atrial fibrillation ablation in patients with atrial septal defect closure devices. Heart Rhythm 11: 330-335.





