International Journal of Transplantation Research and Medicine
The Impact of Renal Transplantation on Lower Limb Perfusion
Paul Alexander1*, Emma Aitken2, David Mansouri2 and David Kingsmore2
1University of Glasgow Medical School, Glasgow, UK
2Department of Renal Surgery, Western Infirmary, Glasgow, UK
*Corresponding author:
Paul Alexander, Department of Renal Surgery, Western Infirmary, Glasgow, G11 6NY, UK, E-mail: 0801247a@student.gla.ac.uk
Int J Transplant Res Med,
IJTRM-1-013, (Volume 1, Issue 3),
Research Article
Received: October 17, 2015: Accepted: November 23, 2015: Published: November 25, 2015
Citation: Alexander P, Aitken E, Mansouri D, Kingsmore D (2015) The Impact of Renal Transplantation on Lower Limb Perfusion. Int J Transplant Res Med 1:013
Copyright: © 2015 Alexander P. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: The benefits of renal transplantation are now more accessible to older, more comorbid patients. Currently, those with peripheral vascular disease are often excluded partly due to the theoretical risk of post transplantation limb ischemia, where blood is diverted away from an already under-perfused leg. This study aims to determine if renal transplantation affects lower limb perfusion.
Methods: Lower limb perfusion was measured on 18 patients' pre and post-transplant using strain gauge plethysmography (SGP) and ankle brachial pressure index (ABPI). Perfusion change in the ipsilateral leg was compared to the change in the contralateral leg, giving an internal control for each patient.
Results: SGP: There was no significant postoperative blood flow change in either the ipsilateral leg (-0.63 ± 0.63 cm3/100 cm3/min) or the contralateral leg (-0.15 ± 0.60 cm3/100 cm3/min), nor was there any significant difference between the legs (p = 0.379). ABPI: There was no significant ABPI change in either the ipsilateral leg (-0.02 ± 0.03) or contralateral leg (0.02 ± 0.02), nor was there any significant difference between the legs (p = 0.718).
Conclusion: In a cohort of general transplant recipients, renal transplantation has no significant impact on lower limb perfusion. It is unreasonable to exclude patients from transplantation based solely on the concern of a postoperative reduction in lower limb perfusion. Further study into a more at-risk cohort of patients warranted.
Keywords
Renal, Perfusion, Leg, Complications, Ischemia
Abbreviations
ABPI: Ankle Brachial Pressure Index, SGP: Strain Gauge Plethysmography
Introduction
Renal transplantation is the preferred method of renal replacement therapy, having been shown to increase life expectancy, improve quality of life and be more cost-effective compared to continued dialysis [1,2]. There has been a recent push to extend the benefits of transplantation to older patients with more comorbidities. Despite a perceived increased risk of complications, current literature indicates that outcomes remain positive in these patients [3]. However, as no universally agreed guidelines exist for selecting transplant recipients, the point at which the risks outweigh the benefits is unclear.
One of the concerns when considering an older patient for transplantation is peripheral vascular disease (PVD), which is present in around 25% of patients with end stage renal disease [4]. In addition to a clustering of common risk factors, patients on dialysis often suffer from hyperphosphataemia and hypercalcaemia, predisposing them to vascular calcification [5]. PVD is used as a marker of coronary and cerebral artery disease; however, it has also been hypothesised that a transplanted kidney anastomosed to one of the iliac arteries may divert blood away from a previously under-perfused leg [6-9]. This is a theoretical risk, but one that has not been fully explored in the literature.
Current practice in deciding suitability for transplantation varies between centres, but is primarily based on clinical history, examination and in selected patients, CT angiography [10]. With no evidence regarding the impact of renal transplantation on lower limb perfusion, it is unclear which pre-operative investigations are appropriate for these patients. Ultimately, with a lack of universal guidelines, patients with significant PVD may be excluded from the transplantation waiting list due to a non-proven risk.
This is a pilot study, which aims to measure the impact of renal transplantation on lower limb blood flow using strain gauge plethysmography (SGP) and ankle brachial pressure index (ABPI) in an unselected group of renal transplant recipients.
Patients and Methods
Study population
All potential adult renal transplant recipients in a single transplant centre from 16th January 2014 to 23rd March 2014 were considered for inclusion in this prospective study. Written consent was obtained from each patient before inclusion. Those with previous lower limb amputation, a femoral arteriovenous fistula, calf circumference over 40 cm, significant intraoperative vessel damage or suspected/confirmed deep vein thrombosis were excluded. These patients were excluded due to equipment limitations and patient safety concerns.
Ethical approval
Ethical approval was obtained from the West of Scotland Research Ethics Committee (REC reference number: 11/WS/0033).
Data collection
Collected data included age, sex, cause of renal failure, dialysis history, past medical history and smoking status. At the time of each measurement, weight, blood pressure and current medications were recorded, along with the size of strain gauge used for the plethysmograph. Any intraoperative or postoperative complications before discharge were also noted.
Measurement process
Patients were rested supine for at least ten minutes; with both legs exposed from the knee down. Plethysmography measurements were taken first followed by ABPI calculation.
Repeat measurements were taken between four and sixteen days postoperatively under the assumption that auto regulation would be complete by day four. The timing of the second measurement beyond four days was based on the patient's clinical condition. A single researcher carried out all measurements and analysis.
Strain gauge plethysmography (SGP)
SGP involves measuring the change in calf diameter when venous return is occluded at the distal thigh. As arterial inflow is still maintained, blood will fill the leg distal to the occlusion, causing the calf to expand at a rate proportional to arterial inflow.
A written protocol was devised before recruitment began, with reference to the plethysmograph manual and previous studies [11,12]. This protocol was further optimised and validated in a cohort of six healthy volunteers.
After a ten-minute rest period, the first leg to be measured was elevated 27 cm by resting the patient's heel on a box and pillow. The hip was slightly externally rotated and the knee slightly flexed. Calf circumference was measured at the point of maximal girth and a strain gauge 2-3 cm smaller than this value was selected and secured around the patient's calf. Care was taken to ensure that the strain gauge leads did not overlap and remained parallel. The strain gauge was then connected to the plethysmograph (Hokanson EC6) and a rapid inflation cuff (Hokanson SC10D) was secured around the patient's distal thigh. A cuff inflation system (Hokanson E20/AG101) allowed instantaneous inflation and deflation of the cuff to a specified pressure. In this study, a venous occlusion pressure of 50 mmHg was selected. Hokanson NIVP3 software (version 5.29d) was used to record and interpret output from the plethysmograph.
Before taking measurements, venous capacitance was maximized by twice inflating the cuff for 45 seconds, separated by a 45 second period of deflation. During this time, the rate of calf expansion was subjectively assessed and an appropriate output range was chosen to give the best trace resolution. An ideal range setting would make use of most of the graph amplitude during the inflation time. Typically this was 0.2%. The NIVP3 software was triggered to record and the cuff was inflated for 8 seconds, followed by a deflation period of 14 seconds. The cuff was inflated and deflated a further two times so that each measurement was recorded in triplicate. An average of the three measurements was used to minimise bias and intraobserver variability.
Plethysmography analysis
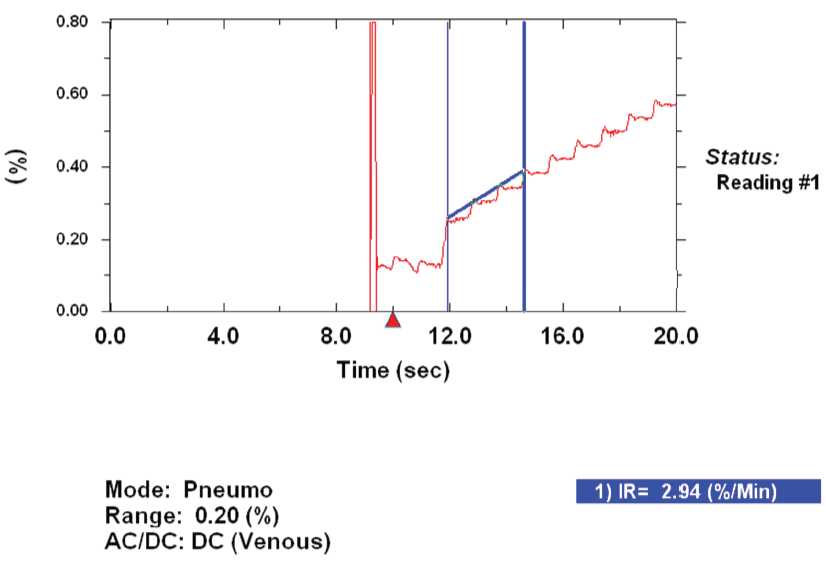
After measurements were completed, analysis was carried out on each inflow curve (Figure 1). The trace shows the percentage change in calf volume with respect to time. Each peak represents a heartbeat. To calculate the average rate of change, a calliper feature was used to draw a straight line between two suitable peaks, with the NIVP3 software automatically finding the maximal point of the peak. Percentage change is displayed in the form of %/min, equivalent to cm3 of blood flow/100cm3 tissue/min. This value is referred to as calf blood flow.
.
Figure 1: Screenshot of Curve Analysis on NIVP3 Software.
Pulsatile trace is representative of increasing calf volume. The caliper tool is shown connecting two peaks to give an estimate of the rate of volume increase. This is reported in the lower right corner.
View Figure 1
To account for confounding factors that could affect blood flow in both legs equally, the change in calf blood flow was calculated for each leg and then compared. To do this, the preoperative measurement was subtracted from the postoperative measurement so that a postoperative reduction in calf blood flow would give a negative number.
Ankle-brachial pressure index (ABPI)
ABPI is calculated by dividing the systolic pressure at each ankle by the highest brachial systolic pressure. Systolic pressures were measured using an 8 MHz handheld Doppler (Huntleigh SDII) and an aneroid sphygmomanometer (WelchAllyn). The measurement technique followed national guidelines [13].
Statistics
Data were analysed using SPSS statistical software (version 21). Within subject variables were assessed for normality and then analysed using paired Student's T-Test. Values of p < 0.05 were considered statistically significant. Data are presented as mean ± standard error of the mean (SEM).
Results
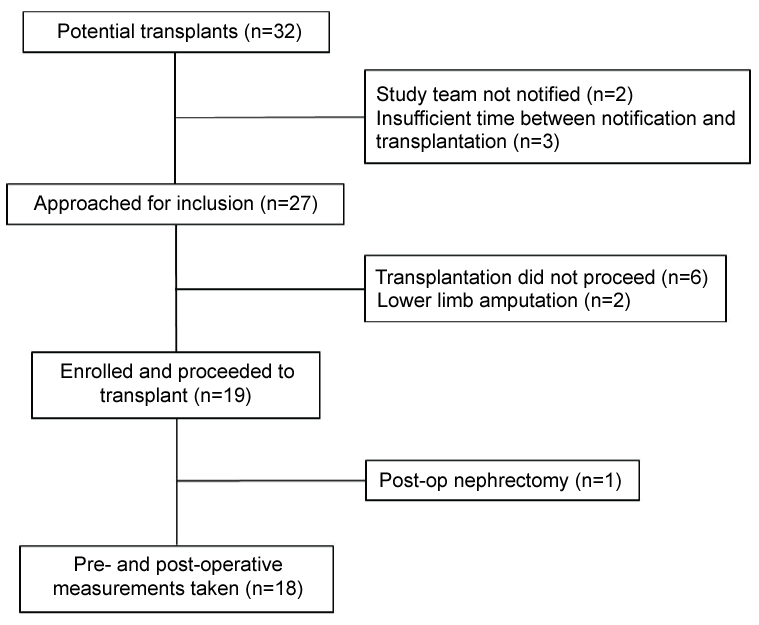
There were 32 potential renal transplants in a single Scottish transplant centre between 16th January and 23rd March 2014. Twenty-seven of these patients were approached for inclusion. Six of the potential transplants did not proceed and two patients were excluded due to previous lower limb amputation. A further patient was excluded due to a postoperative nephrectomy. This left a cohort of eighteen patients with both preoperative and postoperative SGP measurements. During ABPI measurement, one patient was found to have non-compressible lower limb vessels. This left seventeen patients with preoperative and postoperative ABPIs (Figure 2).
Baseline characteristics
The mean patient age was 48.1 years (89.9% male). Median time on dialysis was 24 months and 11.1% had a previous renal transplant. Cadaveric transplantations made up 61.1% of total transplants (Table 1).
![]()
Table 1: Patient Characteristics.
View Table 1
SGP
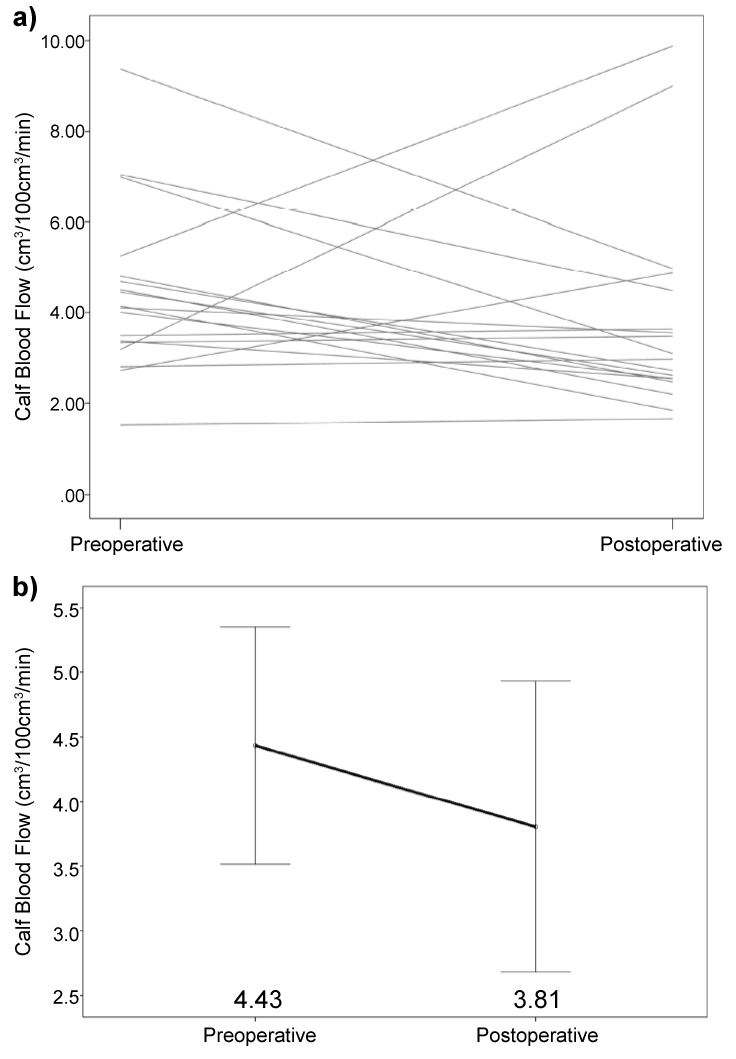
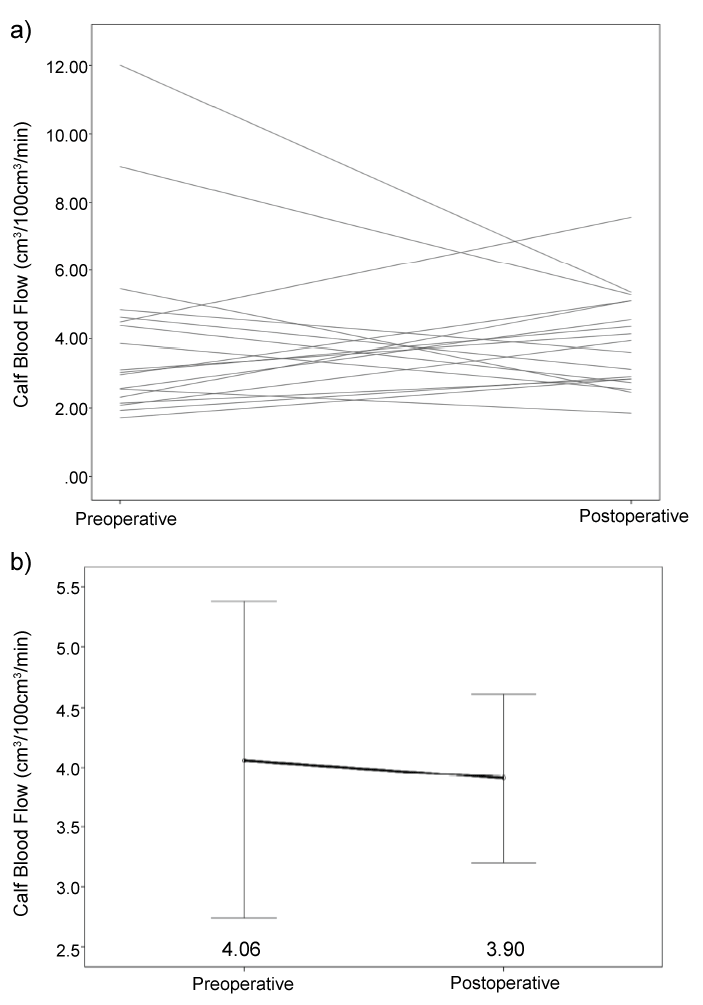
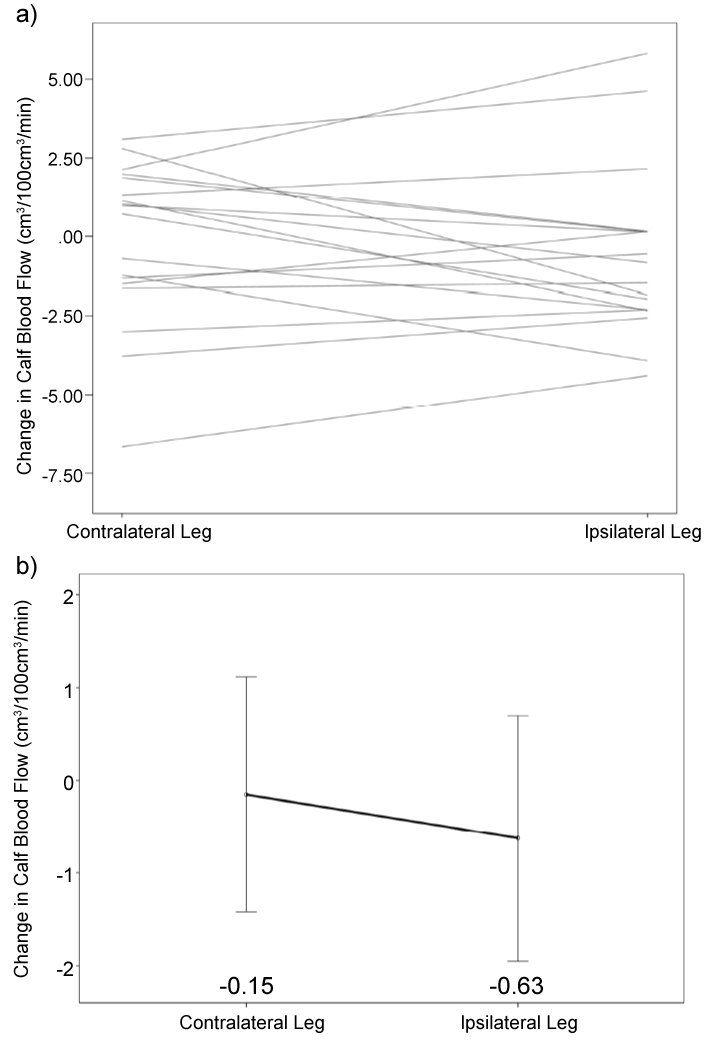
There was no significant difference in calf blood flow between the leg ipsilateral to transplantation and the leg contralateral to transplantation, either preoperatively or postoperatively (preoperative: 4.43 ± 0.44 vs. 4.06 ± 0.63 cm3/100cm3/min [p = 0.323]; postoperative: 3.81 ± 0.53 vs. 3.90 ± 0.34 cm3/100 cm3/min [p = 0.778] (Figure 3 and Figure 4)). The postoperative change in calf blood flow was not significantly different between the ipsilateral leg and the contralateral leg (-0.63 ± 0.63 vs. -0.15 ± 0.60 cm3/100 cm3/min [p = 0.379] (Figure 5)).
.
Figure 3: Calf Blood Flow Change in the Ipsilateral Leg.
a) Change in calf blood flow with each line representing an individual patient
b) Mean change in calf blood flow with error bars depicting 95% confidence interval
View Figure 3
.
Figure 4: Calf Blood Flow Change in the Contralateral Leg.
a) Change in calf blood flow with each line representing an individual patient
b) Mean change in calf blood flow with error bars depicting 95% confidence interval
View Figure 4
ABPI
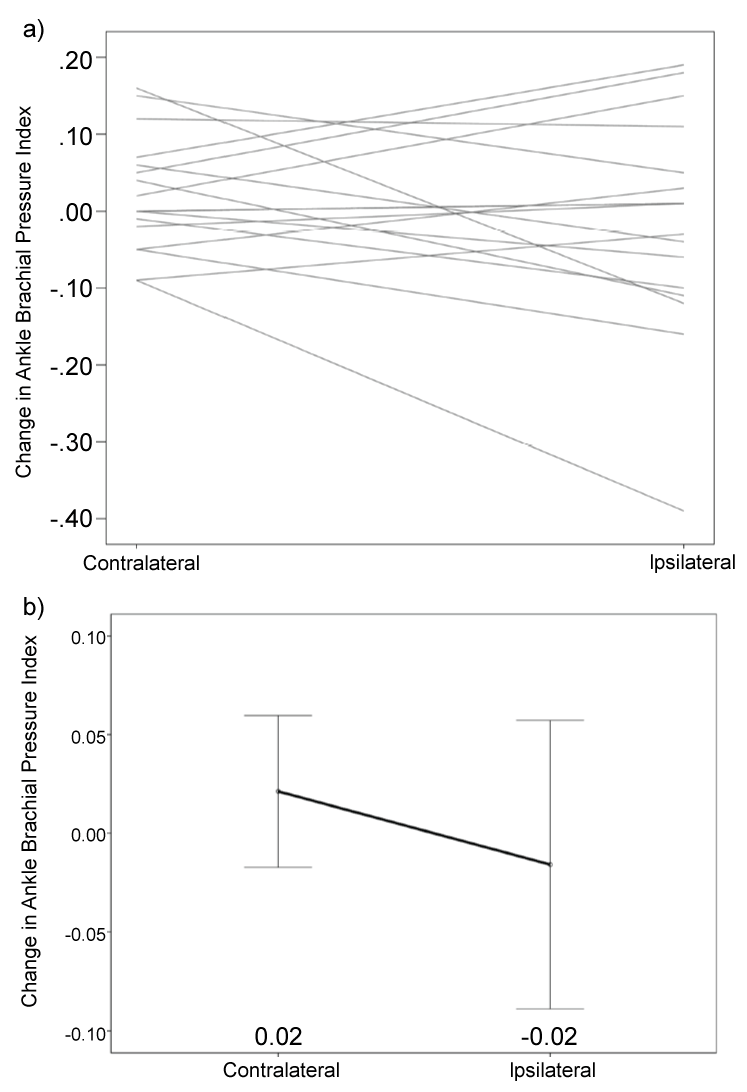
There was no significant difference in ABPI between the leg ipsilateral to transplantation and contralateral to transplantation either preoperatively or postoperatively (preoperative: 1.18 ± 0.03 vs 1.12 ± 0.05 [p = 0.256] postoperative: 1.16 ± 0.03 vs 1.14 ± 0.05 [p = 0.718]). There was also no significant preoperative to postoperative difference in the change in ABPI between the leg ipsilateral to transplant and the leg contralateral to transplant (-0.02 ± 0.03 vs 0.02 ± 0.02 [p = 0.257]) (Figure 6).
.
Figure 5: Difference in Calf Blood Flow (Contralateral vs. Ipsilateral Leg).
a) Difference in calf blood flow with each line representing an individual patient
b) Mean difference in calf blood flow with error bars depicting 95% confidence interval
View Figure 5
.
Figure 6: Difference in ABPI (Contralateral vs. Ipsilateral Leg).
ABPI: Ankle Brachial Pressure Index
a) Difference in calf blood flow with each line representing an individual patient
b) Mean difference in calf blood flow with error bars depicting 95% confidence interval
View Figure 6
Discussion
The peripheral circulation is under dual control: centrally from the nervous system and locally through various chemical mediators. In normal situations, a balance of both these systems ensures that adequate blood flow reaches all peripheral tissues [14]. Resting blood flow through the femoral artery is maintained at around 400 ml/min, rising to over 2000 ml/min during times of increased demand [15,16]. The inability to adequately compensate for this increased demand is a key feature of PVD [16]. When a donor kidney is anastomosed onto one of the iliac arteries, it draws around 700 ml of blood per minute [17]. Given that limb perfusion deficits are rarely seen after transplantation in the absence of direct trauma, it is likely that autoregulation ensures distal blood flow is not significantly compromised. Potentially, in the presence of PVD, this may not be fully possible. The population in this study is made up of general transplant recipients, with only one patient having a confirmed diagnosis of PVD. Despite no apparent blood flow deficit in this cohort, it is still unknown if lower limb perfusion would be significantly compromised in a population with more profound PVD. In addition, flow measurements were obtained at rest. It is possible that a deficit would only become apparent in times of increased vascular demand, which would only be evident on post exercise testing.
The use of venous occlusion plethysmography was first described by Hewlett and van Zwaluwenburg in 1909 [18]. Apart from computerisation and the introduction of mercury-in-silastic strain gauges, the technique has remained essentially unchanged. Within-subject reproducibility has been assessed by several groups, with a reported variation coefficient of between 11% and 15% [11,12,19]. Calf blood flow measured by SGP has been shown to correlate strongly with femoral blood flow measured by both Doppler ultrasound [11,20] and direct limb perfusion via cannulation of the femoral artery and vein [21]. It is considered to be a reliable and accurate measure of blood flow to the extremities.
ABPI is a simple, non-invasive and inexpensive method of diagnosing arterial insufficiency in the lower limbs [22]. In healthy individuals, systolic pressure tends to be higher at the ankles, with a normal ABPI range in the supine position of 1.0-1.2 [23]. This is due to differences in the downstream vascular beds [24]. The ABPI of patients with intermittent claudication is around 0.5-0.8 while those with critical limb ischemia have an ABPI of less than 0.3 [23]. An exception to this is when patients have extensive calcification of their vessels that renders them non-compressible, resulting in an abnormally elevated ABPI above 1.3 [25]. The reproducibility of ABPI has been reported as between 9 and 21% [26,27]. It has been shown to be in independent risk factor for PVD (as proven by angiography) and cardiovascular mortality [25].
This is the first study to measure at rest the impact that renal transplantation has upon lower limb perfusion in a general transplant population. The prospective nature and wide inclusion criteria provides an accurate representation of this centre's current transplant recipient population. Lower limb perfusion was measured using two separate techniques and inter-observer variability was removed by using a single researcher for all measurements and analysis. Despite renal transplantation being an intricate and fast moving area of surgery, this study has shown that it is feasible to undertake a non-interventional study in the perioperative period without negatively impacting on the patient's clinical journey.
Twenty-seven patients were recruited into the study, eighteen of which progressed to successful transplantation. A number of potential recipients did not proceed to transplant, mainly because potential recipients are admitted on notification of a potential donor. This helps reduce cold ischaemic time, but may result in unnecessary hospital admission if the donor is found to be unsuitable.
A post-hoc power calculation showed that with eighteen patients our study would have the power to detect a flow change of just under 50%. Undertaking a formal sample size calculation before recruitment was not possible due to the absence of any previous studies of this sort in renal transplantation. For withholding transplantation to be justified, a limb threatening reduction in perfusion should be demonstrated. Critical limb ischemia generally requires an ABPI reduction from normal to 0.3. We therefore believe that any reduction in blood flow of a magnitude able to cause ischemia would have been apparent with a cohort of this size.
From the currently available literature and the work carried out in the present study, we believe that it is unreasonable to exclude patients from renal transplantation solely on the concern of a postoperative reduction in lower limb blood flow. We have demonstrated that it is possible to undertake such a study, and have shown that an unselected group of transplant recipients are not negatively affected. Future research should focus on targeting the population of transplant recipients who have established PVD, ideally identifying these patients while they are on the waiting list. Scottish guidelines suggest that a resting ABPI < 0.9 be considered abnormal [13] and several clinical studies have shown a cut-off point of 0.9 to be highly sensitive and specific of angiogram proven disease [28]. We propose that a study of similar methodology to the present study be carried out in patients with a resting ABPI < 0.9. To achieve the required numbers, recruitment would likely take place over an extended timescale and in multiple centres.
In conclusion, this study has found no evidence that renal transplantation has any significant impact on resting lower limb perfusion, as measured by SGP and ABPI, in a representative population of renal transplant recipients.
Authorship
PA: Undertook all data collection and analysis, participated in research design, contributed to writing of the paper
EA: Participated in research design, contributed to writing of the paper
DM: Participated in research design
DK: Participated in research design, contributed to writing of the paper
References
-
Wolfe RA, Ashby VB, Milford EL, Ojo AO, Ettenger RE, et al. (1999) Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N Engl J Med 341: 1725-1730.
-
de Wit GA, Ramsteijn PG, de Charro FT (1998) Economic evaluation of end stage renal disease treatment. Health Policy 44: 215-232.
-
Eufrasio P, Moreira P, Parada B, Nunes P, Figueiredo A, et al. (2011) Renal transplantation in recipients over 65 years old. Transplant Proc 43: 117-119.
-
Rajagopalan S, Dellegrottaglie S, Furniss AL, Gillespie BW, Satayathum S, et al. (2006) Peripheral arterial disease in patients with end-stage renal disease: observations from the Dialysis Outcomes and Practice Patterns Study (DOPPS). Circulation 114: 1914-1922.
-
Combe C, Albert JM, Bragg-Gresham JL, Andreucci VE, Disney A, et al. (2009) The burden of amputation among hemodialysis patients in the Dialysis Outcomes and Practice Patterns Study (DOPPS). Am J Kidney Dis 54: 680-692.
-
Subesinghe M, Cherukuri A, Ecuyer C, Baker RJ (2011) Who should have pelvic vessel imaging prior to renal transplantation? Clin Transplant 25: 97-103.
-
Orlic P, Vukas D, Drescik I, Ivancic A, Blecic G, et al. (2003) Vascular complications after 725 kidney transplantations during 3 decades. Transplantation proceedings 35: 1381-1384.
-
Northcutt A ZG, Zhang WW (2012) Does kidney transplanted to iliac artery deteriorate ischaemia to ipsilateral lower extremitywith peripheral artery disease. 40th Annual Sympo-sium Society for Clinical Vascular Surgery, Las Vegas.
-
Sung RS, Althoen M, Howell TA, Merion RM (2000) Peripheral vascular occlusive disease in renal transplant recipients: risk factors and impact on kidney allograft survival. Transplantation 70: 1049-1054.
-
Pham PT, Pham PA, Pham PC, Parikh S, Danovitch G (2010) Evaluation of adult kidney transplant candidates. Semin Dial 23: 595-605.
-
Kooijman M, Poelkens F, Rongen GA, Smits P, Hopman MT (2007) Leg blood flow measurements using venous occlusion plethysmography during head-up tilt. Clin Auton Res 17: 106-111.
-
Corrigan JH, Burns J, Huggett RJ, Mackintosh AF, Mary DASG (2008) The direct effect of leg position on calf blood flow measured by venous occlusion plethysmography. Artery Research 2: 44-48.
-
Hainsworth T (2006) Guidelines on the management of peripheral arterial disease. Nurs Times 102: 23-24.
-
Berne RM, Levy MN, Koeppen BM, Stanton BA (2008) Berne & Levy physiology (6th edition). Philadelphia, PA: Mosby/Elsevier.
-
Kingwell BA, Formosa M, Muhlmann M, Bradley SJ, McConell GK (2003) Type 2 diabetic individuals have impaired leg blood flow responses to exercise: role of endothelium-dependent vasodilation. Diabetes Care 26: 899-904.
-
Paaske WP (2002) Regulation of Distal Blood Perfusion: Local Control of the Peripheral Circulation in Functional and Critical Ischemia, and in Patients with Abdominal Aortic Aneurysm. Perspectives in Vascular Surgery and Endovascular Therapy 15: 59-68.
-
Myers BD, Sommer FG, Li K, Tomlanovich S, Pelc N, et al. (1994) Determination of blood flow to the transplanted kidney. A novel application of phase-contrast, cine magnetic resonance imaging. Transplantation 57: 1445-1450.
-
Hewlett A, van Zwaluwenburg J (1909) The Rate of Blood Flow in the Arm. Heart 1: 87-97.
-
Roberts DH, Tsao Y, Breckenridge AM (1986) The reproducibility of limb blood flow measurements in human volunteers at rest and after exercise by using mercury-in-Silastic strain gauge plethysmography under standardized conditions. Clin Sci (Lond) 70: 635-638.
-
Green S, Thorp R, Reeder EJ, Donnelly J, Fordy G (2011) Venous occlusion plethysmography versus Doppler ultrasound in the assessment of leg blood flow during calf exercise. Eur J Appl Physiol 111: 1889-900.
-
Englund N, Hallbook T, Ling LG (1972) The validity of strain gauge plethysmography. Scand J Clin Lab Invest 29: 155-158.
-
Nam SC, Han SH, Lim SH, Hong YS, Won JH, et al. (2010) Factors affecting the validity of ankle-brachial index in the diagnosis of peripheral arterial obstructive disease. Angiology 61: 392-396.
-
Caruana MF, Bradbury AW, Adam DJ (2005) The validity, reliability, reproducibility and extended utility of ankle to brachial pressure index in current vascular surgical practice. Eur J Vasc Endovasc Surg 29: 443-451.
-
Al-Qaisi M, Nott DM, King DH, Kaddoura S (2009) Ankle brachial pressure index (ABPI): An update for practitioners. Vasc Health Risk Manag 5: 833-841.
-
Adragao T, Pires A, Branco P, Castro R, Oliveira A, et al. (2012) Ankle--brachial index, vascular calcifications and mortality in dialysis patients. Nephrol Dial Transplant 27: 318-325.
-
Johnston KW, Hosang MY, Andrews DF (1987) Reproducibility of noninvasive vascular laboratory measurements of the peripheral circulation. J Vasc Surg 6: 147-151.
-
Fisher CM, Burnett A, Makeham V, Kidd J, Glasson M, et al. (1996) Variation in measurement of ankle-brachial pressure index in routine clinical practice. J Vasc Surg 24: 871-875.
-
Fowkes FG (1988) The measurement of atherosclerotic peripheral arterial disease in epidemiological surveys. Int J Epidemiol 17: 248-254.