International Journal of Transplantation Research and Medicine
Anonymous Altruistic Living Kidney Donation in the US: Reality and Practice
Abby S Kazley1*, Raj Amarnath2, Arun Palanisamy2, David Taber2, Kenneth Chavin2, Prabhakar Baliga2 and Wendy Balliet3
1Department of Health Care Leadership and Management, Medical University of South Carolina, USA
2Department of Surgery, Medical University of South Carolina, USA
3Department of Psychiatry and Behavioral Sciences, Medical University of South Carolina, USA
*Corresponding author:
Abby S Kazley, PhD, Department of Health Care Leadership and Management, Medical University of South Carolina, 151 Rutledge Avenue Box 962, Charleston, SC 29425, USA, Tel: 843-792-0012, Fax: 843-792-3327, E-mail: swansoaj@musc.edu
Int J Transplant Res Med, IJTRM-2-021, (Volume 2, Issue 2), Research Article
Received: June 20, 2016; Accepted: September 18, 2016; Published: September 21, 2016
Citation: Kazley AS, Amarnath R, Palanisamy A, Taber D, Chavin K, et al. (2016) Anonymous Altruistic Living Kidney Donation in the US: Reality and Practice. Int J Transplant Res Med 2:021.
Copyright: © 2016 Kazley AS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Living kidney donors have emerged as the best option to overcome the severe shortage of transplantable kidneys. A growing number of these living donor kidneys come from anonymous altruistic donors who are not related to the recipients according to UNOS data. This study examines the process of anonymous altruistic kidney donation and identifies barriers and variance in transplant center practices. Using a mock patient caller, 73 transplant centers were contacted and asked about the process of altruistic anonymous kidney donation and then scored using objective and subjective metrics. We use SRTR data to measure the relationship between altruistic donation and transplant volume, competition, and quality and scored responses as subjective (how nice and responsive the person was) and objective (follow up, etc). Sixty-seven of the 73 transplant centers contacted perform anonymous altruistic donations. The mean subjective score was 53.60, and the mean objective score was 53.88. A majority of centers were willing or highly willing to answer questions (56.8%), but more than half (56.8%) answered them inadequately or used jargon. Models including a center's characteristics (competition, waitlist and transplant volume and quality measures) were capable of significantly predicting which programs would have higher objective (C-stat 0.846) and subjective scores (C-stat 0.749). The process for anonymous altruistic donation is highly variable by center. These inconsistencies in practice can potentially lead to confusion, public misperception and discourage motivated individuals from donation.
Keywords
Altruistic donation, Living kidney donation, Transplantation
Introduction
The incidence of end stage renal disease (ESRD) has quadrupled in the United States in the past three decades, from 86 per million population in 1980 to 371.1 per million population in 2011 [1]. This has resulted in a six-fold increase in the prevalence of ESRD nationally, which had reached almost 1,969 per million populations in 2011. Although the largest year-on-year percentage increases were observed during the 1980s (between 9 and 16%), the percentage of Americans living with diagnosed ESRD continues to climb annually by between 2% and 3% [1].
Kidney transplant is the best therapeutic treatment for ESRD, yet the number of donated organs from deceased donors for transplant is not sufficient to meet the need [2]. Living kidney transplantation allows living donors to give one of their kidneys for transplant while continuing to lead a full and healthy life [3]. The five year outcomes of living donor kidney recipients have been found to be superior to the outcomes of deceased donor kidney transplants and dialysis [4].
Altruistic kidney donation is a living donation made by an individual who does not know the recipient of his or her donation. Sometimes called anonymous donation, has been occurring for at least a decade, and according to a UNOS data report, 1,360 altruistic kidney donations have taken place between January 1, 2001 and October 22, 2013. The number of anonymous altruistic donors by center, however, varies and ranges from zero to forty-seven over this same time period [5]. This variation illustrates the propensity for some centers to be more supportive of anonymous altruistic donation than others. A significant barrier to anonymous altruistic donation may be the health care provider's (transplant center) attitudes towards this particular type of donation. This variance may be a reflection of varying comfort levels with anonymous altruistic donors and the corresponding processes for evaluation in place.
The screening of potential living donors, both related and anonymous altruistic varies by center but includes rigorous evaluation of physical, social, and psychological fitness [6]. In the case of anonymous altruistic donation, the center will likely consider and evaluate the motivation of the individual before allowing him or her to make a donation. Likewise, some centers have been more amenable to anonymous altruistic donation while others have discouraged or not allowed it out of fear of liability. In fact, there have been documented instances where an anonymous altruistic donor has contacted one center and been turned down, but then contacted another center where the donation took place [7]. Transplant centers have complete discretion of whether to allow altruistic kidney donors, and the legal and clinical practice of altruistic living kidney donation have discouraged some transplant centers from pursuing donors that they perceive to be risky. Transplant centers may fear legal or social ramifications or poor clinical outcomes from altruistic donors, despite the fact that no study has shown evidence of such consequences.
Some programs have specific protocol for dealing with inquiries about altruistic kidney donation. For example, Washington University reported their experience with inquiries and screening over a 30 month period. They had 731 donor inquiries [8]. Of these 731, 131 called back after receiving information in the mail, 47 initiated evaluations, 19 completed the evaluation process, and seven actually donated. This example illustrates the potential barriers in the process that anonymous altruistic donors face in considering donation, and may also demonstrate that appropriate measures to assess and protect living donors are in place with education and screening.
The purpose of this study is to identify barriers in the process of anonymous altruistic living kidney donation and demonstrate the variance in procedures that exists by transplant center. The research question asks: what variance exists in centers for altruistic kidney donation?
Methods
In this study, we use a mock patient to call transplant programs and identify steps, barriers and facilitators of altruistic kidney donation. The transplant centers were selected as a convenience sample to be geographically diverse. A list of transplant centers was taken from the Kidney and Kidney/Pancreas Transplant Center Programs found on the Scientific Registry of Transplant Recipients website (srtr.org) (AL9). Contact information was taken from transplant center websites. If there was no direct number to the transplant program, the hospital operator number was used. The steps needed to find the correct contact at each transplant program was recorded. Centers that no longer did transplants or did not deal with living/altruistic donors were recorded, but excluded from analysis. The centers were called by a single individual (Physician Researcher) between September 2012 and May 2013. The individual caller claimed to be an individual interested in altruistic kidney donation when calling each of the centers and inquired about how to proceed. The caller used a script that was developed by an interdisciplinary team of two transplant surgeons, a health services researcher, a psychologist, and a transplant coordinator and was first tested on individual transplant coordinators at the study site center. Discrepancies in scoring or questions about responses were discussed with the team on a weekly basis.
The script is provided in the appendix and was specifically designed to represent a low risk anonymous altruistic donor. The researcher presented himself as Neal Johnson, a 33 y/o Caucasian software engineer in ideal health. Mr. Johnson was given an ideal BMI, B+ blood type, clean medical and family history and was in the process of moving to the locale of whatever transplant center he was calling. The script also included answers to likely questions such has why he wanted to donate, and why he was calling before moving. A Google Voice number and local address were set up should the transplant center require contact info. Upon calling a transplant center, the researcher immediately made an altruistic offer of kidney donation. During the course of the call, the researcher also asked about how potential donors were evaluated, whether this changed for altruistic donors, how recipients were selected, and what would happen if a donor did not match to any recipients on the center's list. The researcher also asked about paired kidney exchange if not mentioned by the transplant center contact. Any screening questions asked by the transplant center contact, steps in the donor evaluations, who the researcher talked to, and the researcher's impressions on the reaction to altruistic donation, willingness to answer questions, and ability to explain paired kidney exchange were recorded. Any additional calls made by the transplant center to the researcher after this initial call or additional efforts were also recorded. If the transplant center sent any materials to the researcher, these were examined for anything directed toward altruistic donors. Twelve centers were randomly selected and then called again more than a year later and asked the same questions with a different name to test the reliability of the responses.
The data from each of the calls was compiled into a database created for the study, and SPSS was used to analyze the data. The study was IRB approved by MUSC, and deception was used because there is no other reasonable way to collect the data showing transplant center response to altruistic anonymous donation. One on hand, the deception was not honest, but the team felt that it was a necessary means to gather the information of interest since we doubt that transplant centers recognize how "altruistic friendly" they are if we were to ask them in a focus group. Additionally, since we will not identify any of the transplant centers individually, we perceive the risks to be minimal. We made a point to pilot test the script on our own transplant center as we were curious to know what we would find. The team further developed a scoring rubric (Appendix) to rate each of the transplant centers' responses to the caller. The subjective scoring rubric gauged the interest score of the transplant center and took the reaction to the altruistic offer, willingness to answer questions, mention and explanation of a paired kidney exchange, ease of finding the right person to talk to about the process, explanation of tests and procedures, and adequacy of questions answered into account. Bonus points were given in the scores if the person at the center provided an additional contact or made additional offers for help or information. Objective measures were also considered and include whether the mailed packet contains materials for altruistic donors, whether the mailed packet presents paired kidney exchange, the time between the call and the postmark date on the packet, and whether the calls were returned within one week. For the objective measures, centers were awarded more points for developing their own materials that present altruistic anonymous donation because we believe the materials would present more detailed and specific information to the process at such a center and the development of such materials would represent an investment in the development of an altruistic anonymous donation program. The centers were then individually scored using the following equation:
Data from the Scientific Registry of Transplant Recipients (SRTR) was merged with the collected data to examine the relationship between a center's individual characteristics and their respective objective and subjective scores. Characteristics that were analyzed included measures related to competition (number of transplant centers per region and number of centers per OPO), quality (being cited by SRTR for higher than expected waiting list mortality, graft loss or death). Additional characteristics included in the modeling were transplant volume (deceased and living donor), numbers on the waiting list and numbers added to the waiting list. Modelling was conducted using backward conditional binary logistic regression, with the dependent variable set as above the median score. Separate models were developed for objective and subjective scores. Model performance and predictability was assessed by analyzing the R2 and the ROC curve characteristics. Data was compiled and analyzed using SPSS version 22.0 (IBM Corp, Armonk, NY).
Results
During the study, 73 transplant centers were called. Of these 73, 67 received scores. The other six centers were not scored because they did not perform anonymous altruistic donations. Of the 73, 29 were in the Northeast, 19 were in the Southeast, 15 were in the West, and 10 were in the Midwest. The majority of the calls were sent straight to the living donor coordinator (n = 41, 56.2%) who handled the process. A smaller number were screened by an assistant and then went to the living donor coordinator (n = 9, 12.3%), screened by electronic or paper means before being sent to the living donor coordinator (n = 5, 6.8%), or handled by an assistant only (n = 3, 4.1%). Five (6.8%) were handled in some other way, The additional ten centers either did not identify the role of the person. The responses collected in the second calls to twelve random selected transplant centers were nearly identical demonstrating reliability.
For the objective measures, the highest score was 133 with a mean of 53.88 and a standard deviation of 31.51. The mean of the transplant centers' subjective scores was 53.60 with a standard deviation of 17.879 and a range of 0-93. These scores and ranges illustrate the wide range of reactions to anonymous altruistic kidney donation and are illustrated in table 1, table 2 and table 3. For the bonus areas, one center offered follow up calls or contact more than three times, five centers made additional contact once or twice, and 55 centers did not make additional contact after the initial conversation. Two of the programs made offers of additional resources provided by the transplant center, and 59 did not. For the subjective measures, nearly an equal percentage had no reaction to the call or a positive reaction to the call (36.5 vs. 37.8%) as opposed to a negative reaction (4.1%) or a highly positive reaction (5.4%). A majority of the calls resulted in the center being willing or highly willing to answer questions (56.8%). Nearly an equal number of those did not mention paired exchange (39.2%) versus those that did mention and explain it or provide an excellent explanation (37.8%). While a majority answered the procedures and tests adequately (63.5%), in another question, we found that a majority also answered questions inadequately or using jargon (56.8%). 14.9% provided no opportunity to ask questions.
![]()
Table 1: Subjective measures.
View Table 1
![]()
Table 2: Objective measures.
View Table 2
Table 1 shows that approximately half of the centers had a positive or highly positive message about altruistic donation, while more than half of the centers were willing or very willing to provide information and answer questions. At the same time, more than half of the centers used jargon or provided information that might be difficult for an altruistic donor to understand.
![]()
Table 3: Descriptive statistics of objective and subjective total scores.
View Table 3
For the objective measures, approximately one third (29.7%) provided a mailed packet for anonymous altruistic donors. Most of these sent the packet within one week of the call, and 54.1% mentioned the paired kidney exchange.
Eighteen of the centers had different processes for anonymous altruistic donors as opposed to other living donors. These other processes included additional steps such as a requirement to meet with a psychologist of social worker before beginning the clinical evaluation or a requirement for a cool down period to ensure the person really wanted to be a donor.
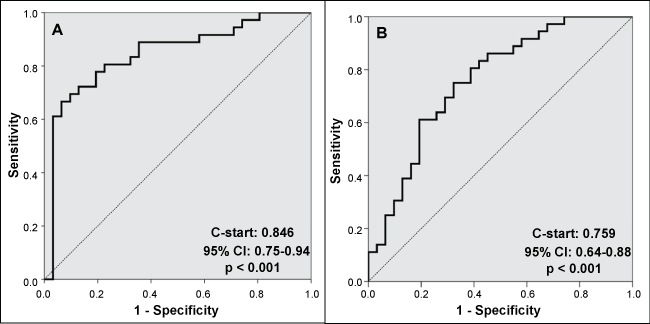
The analysis associating SRTR reported transplant center characteristics with the mean objective and subjective scores resulted in a number of statistically significant findings. Binary logistic regression demonstrated that a model including six variables (total transplants per year, number of centers per region, average centers per OPO, number of new additions to the waiting list, SRTR citation for higher than expected graft loss, and transplant rate for deceased donors) was capable of adequately predicting which centers were above the median objective score (R2 = 0.373, p < 0.001). The ROC curve for this model resulting in very good predictability (C-stat: 0.846 (95% CI 0.75-0.94, see Figure 1A), with a positive predictive value (PPV) of 77% and a negative predictive value (NPV) of 78%. A similar model was developed for the subjective score and demonstrated good performance as well. This model included similar variables to the objective score model (number of patients added to the waiting list, transplant rate and SRTR performance measures for transplant outcomes) and was able to discern which centers were above the median subjective score in (R2 = 0.278, PPV = 72%, NPV = 68%). Figure 1B displays the ROC curve for the subjective model, demonstrating a C-stat of 0.759 (95% CI 0.64-0.888).
.
Figure 1: Displays the ROC curves, analyzing the predictability of SRTR reported transplant center characteristics for being above median (a) objective score, and (b) subjective score.
View Figure 1
Discussion
Transplant centers and other stakeholders have struggled for more than a decade to deal with altruistic donors wondering about their motivations, despite a purported high prevalence of willingness from the population [9-12]. According to Henderson, et al, "Studies indicate that 11% to 54% of individuals surveyed would consider donating a kidney, while alive, to a stranger. The idea of 'living anonymous donors' (LADs) as a donor source, however, has not been embraced by the medical community. Reservations focus on the belief that LADs might be psychologically unstable and thus unsuitable donors" [13]. Altruistic behavior has been studied in several different disciplines including psychology, anthropology, religious studies, and economics [14-18]. Theories of altruism have included reciprocal altruism, whereby one does something "good" with the expectation that someone else will do something good for them in return, a desire to "win prestige, respect, friendship, and other social and psychological objectives" [19], or a desire to, "avoid scorn of others to receive social acclaim" [20]. Despite the clear logic of these theories, they have been found to have poor predictive power in application, and they do not focus on the process of transplantation, but instead the individual motivations for donating [21]. Donors have reported various motivations for donating including religious duty, belief in karma, a sense of moral duty, imagining oneself in the position of the recipient, or the desire to save a life [7,22,23]. Rodrigue and colleagues examined psychosocial and functional outcomes of altruistic anonymous donation and found similar motives, psychological benefits, and feelings following the donation as traditional living donors [23].
The most significant finding of this study is that there is wide variance in the acceptability and process of altruistic, attitudes of transplant center staff towards altruistic donors, anonymous donation by transplant center, potentially resulting in inconsistency or confusion for potential donors. Given the shortage of donated kidneys for donation, and the impact that one donation may have by sparking a paired kidney exchange or chain, it seems that providing a positive and consistent response to an individual interested in making an altruistic anonymous donation is essential. Despite this variance, the responses were overall positive or highly positive, indicating that there is an overall acceptance and process in place to facilitate altruistic, anonymous donation. Our results relate to a study in Australia that found that altruistic donation was "relatively silent" on hospital websites, indicating a need of sources of reliable information related to such opportunities [24].
Another interesting finding was the strong relationships that were identified when comparing a transplant center's SRTR reported characteristics (competition, volume and quality) and being above the median objective or subjective survey scores. These results may be explained by a number of scenarios. Certainly, centers that face more competition might be more motivated to develop formal altruistic donor programs to offset having lower numbers of deceased donor organs available. This would also apply to centers that have higher than expected waiting list mortality or lower than expected transplant rates and volumes. However, in addition to these factors, the decision to facilitate altruistic donors by developing a formal program may also be influenced by the culture, history, and risk tolerance within the transplant center. Certain centers may approach donation in a more "aggressive" way than others, but the authors do not mean to imply that aggressive is better than another different approach.
While there is great danger in not responding in a positive way when an altruistic, anonymous donor makes an inquiry, there is even greater danger in facilitating a donation in an inappropriate or dangerous way. Providers must balance the risk between these two alternative extremes and develop practices and procedures in a fair, equitable, and non-coercive way to facilitate altruistic, anonymous donations for individuals who wish to make such a gift. Baskin proposed in a commentary that the increasing need for organs has led to greater acceptance of altruistic donation while also presenting challenges in how to respond to such offers and evaluate altruistic donors [25]. Barriers to the altruistic process include a lack of information available to potential donors and inconsistent practices and responses based on which center is called.
The identification and promotion of best practices for facilitating the process of altruistic anonymous donation should be sought from transplant centers in the US. While there may be a number of ways to approach the process in a positive and productive way, centers might seek evidence of practices that lead to best outcomes for donors, recipients, and centers, which reduce unnecessary risk. Sharing best practices from transplant centers that facilitate the process for altruistic anonymous donors can help guide and reduce the confusion that may occur when individual potential donors receive different information or responses based on which centers they call. There may be additional physical, social, and psychological fitness assessments that are necessary for evaluation. There might also be information that is tailored specifically to altruistic donors or information gathered on paired kidney donation.
Our study does have limitations. First, there is no control group for the study, and it is possible that variation exists in all aspects of donor evaluation, much like it does in other areas of health care including mitral valve repair, acute myocardial infarction, diabetes and hyperglycemia, and post-acute care and is likely the result of practice styles, supply of services, and local regulatory practices [26-29]. Second, we have developed and utilized a new tool to collect data and score centers on their responses. We relied upon expert development and validity for this tool and also field tested it before use. Third, we used a single mock caller who also scored all of the centers. While this led to greater reliability, it also has limitations that we attempted to overcome by meeting and discussing any scoring discrepancies. Finally, we did repeat the measure of data collection by calling centers more than one time to ensure consistency of response. A challenge of this research is that there may be variance in who answers the inquiry calls based on timing, and allowing for follow up required use of a cellular phone with a different area code and an address, which led to questions about why the individual would be interested in donating at that center. The caller explained he planned an impending move to the city where the transplant center was located.
This study demonstrates the varying responses and processes that potential altruistic donors may face in their search for a transplant center and evaluation. We recommend that best practices of transplant centers for altruistic donation be identified, shared, and replicated to allow for the best management of this group of donors who have potential to reduce the number of patients who waiting for a life-saving kidney transplant. Future studies should consider collecting more information about specific altruistic donor practices and may consider linking this information to transplant center volumes and outcomes.
References
-
(2011) U.S. Renal Data System, USRDS 2011 Annual Data Report: Atlas of Chronic Kidney Disease and End-Stage Renal Disease in the United States. National Institute of Diabetes and Digestive and Kidney Diseases, Bethesda, USA.
-
UNOS Website.
-
Ibrahim HN, Foley R, Tan L, Rogers T, Bailey RF, et al. (2009) Long-term consequences of kidney donation. N Engl J Med 360: 459-469.
-
Matas AJ, Smith JM, Skeans MA, Lamb KE, Gustafson SK, et al. (2013) OPTN/SRTR 2011 Annual Data Report: kidney. Am J Transplant 13: 11-46.
-
OPTN Data.
-
Dew MA, Olenick D, Davis CL, Bolton L, Waterman AD, et al. (2011) Successful follow-up of living organ donors: strategies to make it happen. Prog Transplant 21: 94-96.
-
Gohh RY, Morrissey PE, Madras PN, Monaco AP (2001) Controversies in organ donation: the altruistic living donor. Nephrol Dial Transplant 16: 619-621.
-
Jendrisak MD, Hong B, Shenoy S, Lowell J, Desai N, et al. (2006) Altruistic living donors: evaluation for nondirected kidney or liver donation. Am J Transplant 6: 115-120.
-
Mueller PS, Case EJ, Hook CC (2008) Responding to offers of altruistic living unrelated kidney donation by group associations: an ethical analysis. Transplant Rev (Orlando) 22: 200-205.
-
Challenor J, Watts J (2014) It seemed churlish not to: how living non-directed kidney donors construct their altruism. Health (London) 18: 388-405.
-
Kaplan BS, Polise K (2000) In defense of altruistic kidney donation by strangers. Pediatr Nephrol 14: 518-522.
-
Spital A (2001) Public attitudes toward kidney donation by friends and altruistic strangers in the United States. Transplantation 71: 1061-1064.
-
Henderson AJ, Landolt MA, McDonald MF, Barrable WM, Soos JG, et al. (2003) The living anonymous kidney donor: lunatic or saint? Am J Transplant 3: 203-213.
-
Barclay P, Willer R (2007) Partner choice creates competitive altruism in humans. Proc Biol Sci 274: 749-753.
-
Bereczkei, Bela Birkas, Zsuzsanna Kerekes (2007) Public charity offer as a proximate factor of evolved reputation-building strategy: an experimental analysis of a real-life situation. Evolution and Human Behavior 28: 277-284.
-
Bereczkei, Bela Birkas, Zsuzsanna Kerekes (2010) Altruism towards strangers in need: costly signaling in an industrial society. Evolution and Human Behavior 31: 95-103.
-
Simon HA (1993) 'Altruism and Economics', American Economic Review 83: 156-161.
-
Montague PR, Chiu PH (2007) For goodness sake. Nat Neurosci 10: 137-138.
-
Olson M (1965) The Logic of Collective Action. Harvard University Press, London, UK.
-
Becker GS (1974) A theory of social interactions. Journal of Political Economy 82: 1063-1093.
-
Andreoni J (1990) Impure altruism and donations to public goods: a theory of warm-glow giving. The Economic Journal 100: 464-477.
-
McCann K (2010) I could save a life- that's all that matters. The Telegraph.
-
Rodrigue JR, Schutzer ME, Paek M, Morrissey P (2011) Altruistic kidney donation to a stranger: psychosocial and functional outcomes at two US transplant centers. Transplantation 91: 772-778.
-
Bramstedt KA, Dave S (2013) The silence of Good Samaritan kidney donation in Australia: a survey of hospital websites. Clin Transplant 27: E244-248.
-
Baskin JH (2009) Giving until it hurts?: Altruistic donation of solid organs. J Am Acad Psychiatry Law 37: 377-379.
-
Vassileva C, DiGennaro J, Boley T, Markwell S, Hazelrigg S (2012) Geographic variation in procedure selection and hospital mortality in mitral valve surgery. J Heart Valve Dis 21: 48-55.
-
Laskey W, Spence N, Zhao X, et al. (2010) Regional differences in quality of care and outcomes for the treatment of acute coronary syndromes: an analysis from the get with the guidelines coronary artery disease program. Crit Pathw Cardiol 9: 1-7.
-
Cook CB, Elias B, Kongable GL, Potter DJ, Sheperd KM, et al. (2010) Diabetes and hyperglycemia quality improvement efforts in hospitals in the United States: current status, practice variation, and barriers to implementation. Endocr Pract 16: 219-230.
-
Kane RL, Lin WC, Blewett LA (2002) Geographic variation in the use of post-acute care. Health Serv Res 37: 667-682.





