International Journal of Transplantation Research and Medicine
Complications after Heart Transplantation: Hope for the Best, but Prepare for the Worst
Ana Carolina Alba*, Eva Bain, Nicholas Ng, Madeleine Stein, Kathleen O'Brien, Farid Foroutan and Heather Ross
Division of Cardiology, Toronto General Hospital - University Health Network, Canada
*Corresponding author:
Carolina Alba, Division of Cardiology, Toronto General Hospital - University Health Network, Toronto, Canada, E-mail: Carolina.Alba@uhn.ca
Int J Transplant Res Med, IJTRM-2-022, (Volume 2, Issue 2), Review Article
Received: June 27, 2016; Accepted: October 08, 2016; Published: October 10, 2016
Citation: Alba C, Bain E, Ng N, Stein M, Brien KO, et al. (2016) Complications after Heart Transplantation: Hope for the Best, but Prepare for the Worst. Int J Transplant Res Med 2:022.
Copyright: © 2016 Alba C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
For selected patients living with the most advanced stages of heart failure, cardiac transplantation is considered the gold-standard treatment, providing substantial improvements in survival and quality of life. However, heart transplantation is not without risk, and almost all transplant recipients will suffer some form of complication, from mild to potentially fatal,and should be informed of this prior to transplant. This review highlights the most frequent complications following heart transplant, including rejection, cardiac allograft vasculopathy, graft dysfunction, chronic kidney disease, infection, and malignancy. A detailed overview of the incidence, risk factors, consequences, and treatments of these complications are discussed. Health care professionals must work closely with patients and their families to prevent, identify, and treat such complications if and when they do arise. Such collaboration is crucial in helping to meet the ultimate goals of heart transplantation: improved survival and quality of life.
Keywords
Cardiac transplantation, Complications, Outcomes, Rejection, Cardiac allograft vasculopathy, Graft dysfunction, Renal failure, Infection, Malignancy
Introduction
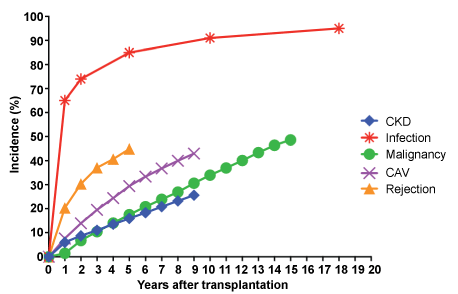
Heart transplant is the accepted treatment option for selected advanced heart failure patients with a median survival ~12 to 13 years and an improved quality of life. Unfortunately, heart transplant is not a definitive cure and patients are at risk for developing different complications during the post-transplant period. Some of the most common complications are rejection, cardiac allograft vasculopathy, graft dysfunction, chronic kidney disease (CKD), infection and malignancy with increasing incidence during post-transplant follow-up (Figure 1). Virtually all heart transplant recipients will suffer at least one complication. Consequently patient quality of life and survival may be impaired depending on the complication severity. This article reviews the most frequent complications after heart transplantation describing their frequency, risk factors, consequences and treatment strategies. Table 1 provides a summary of main points discussed in this paper.
![]()
Table 1: Main complications after heart transplantation. Incidence, risk factors, main consequences and therapeutic and prophylactic strategies. Refer to each complication section in the text for detailed information.
View Table 1
Rejection
The recipient's body may reject a donor organ through hyperacute rejection, acute cellular rejection, or antibody-mediated rejection [1,2]. The risk for developing rejection is the highest in the first six months following heart transplantation, with a decrease as the time from transplantation increases [3]. Sex and age are both linked to rejection risk, with females and younger individuals being at higher risk [4]. Similarly, patients of black race [2] are also at a higher risk of rejection. A higher rate of rejection one-year post-transplant has been reported in patients who received induction therapy, however, this may represent selection bias with higher risk patients receiving induction [4].
Hyperacute rejection
During the immediate post-transplant phase, after cross clamp removal, hyperacute rejection may occur when the recipient has pre-existing donor directed human leukocyte antigen (HLA) antibodies [5,6]. In a 1991 study of 463 heart transplant patients, 18 patients were diagnosed with hyperacute rejection (approximately 4%) [7]. Fortunately, hyperacute rejection is now uncommon as a result of both antibody screening prior to transplantation (panel reactive antibodies (PRA)), and blood type matching [2].
Acute cellular rejection
This remains a frequent complication post-transplant [2]. It involves recipient T-cells recognizing donor HLA molecules by means of antigen-presenting cells [1]. Around 20 to 40% of patients will experience acute cellular rejection between 6 and 12 months post-transplant [8], though most patients are asymptomatic without allograft dysfunction [3].
Antibody-mediated rejection
This type of rejection is characterized by an antibody-driven immune response to vascular endothelial antigens in the allograft, involving both B-cells and T-cells [3]. Though not as common as acute cellular rejection [3], antibody-mediated rejection has an estimated incidence of 10 to 20% in the first year post-transplant [9]. Mixed rejection -simultaneous acute cellular rejection and antibody mediated rejection-can be seen in as many as 25% of acute rejection cases [3].
An important risk factor for antibody-mediated rejection is sensitization to HLA molecules prior to transplantation [10]. Sensitized patients have pre-existing antibodies against HLA molecules [11], which can be quantified by their calculated PRA (cPRA) [8]. The cPRA is calculated based on HLA antigen profile of the population of potential donors [11].The cPRA represents the probability that a recipient will have an unacceptable donor based on the presence of incompatible antigens (a probability of 10% means that one in ten donors will be unacceptable for that particular recipient). Risk factors for sensitization include infection [12], pregnancy, blood transfusion, ventricular assist device (VAD), or previous transplant [13]. A United Network for Organ Sharing/Organ Procurement and Transplantation Network (UNOS/OPTN) database study reported that patients with a most recent pre-transplant PRA greater than 25% had a higher risk of treated rejection in their first year post-transplant versus patients with a 0% PRA (OR 1.4, 95% CI = 1.07-1.92) [14].
Donor-specific antibodies are also associated with increased risk of rejection. Donor-specific antibodies can develop after transplant. A recent single-center study of 224 heart transplant recipients who survived more than one-year post-transplant (follow up time 5-13 years) assessed the impact of de novo donor-specific antibodies. In this study, 33% of patients developed de novo donor-specific antibodies, with persistent de novo donor-specific antibodies (noted in at least 2 successive annual serum samples) accounting for 84% of these individuals. Patients with persistent de novo donor-specific antibodies had poorer overall survival (HR 4.3, 95% CI = 1.9-9.8). The presence of donor-specific antibodies was also significantly associated with the development of biopsy-proven rejection episodes in the first year post-transplant [15].
In order to minimize risks and consequences of rejection, antibodies are measured pre- and post-transplant [11]. When a potential donor heart is identified, a crossmatch is performed. The cross match compares donor antigens and recipients antibodies. It can be done prospectively (using donor blood and recipient's plasma before transplant is performed) [16], retrospectively (using donor blood and recipient's plasma after transplant is performed), or virtually (comparing donor identified antigen and recipient's known HLA antibodies prior to transplant) [17]. An advantage of the virtual crossmatch is that a comparison can be made to a national donor pool in an effort to find a negative match [18]. A prospective crossmatch may limit access to the local donor pool [18], as waiting to receive cells from a non-local donor in order to perform the prospective test may increase the ischemic time of the graft [19,20] potentially compromising its quality.
There are two strategies to manage highly sensitized patients (for example patients with a cPRA > 80%). One is to avoid antibodies (through use of cross matching) and the other is to use desensitization strategies to lower the amount of circulating antibodies, potentially making the patient a more suitable candidate for transplant [12]. The former strategy may delay transplantation. The latter strategy may increase the risk of rejection. A study of 523 heart transplant recipients compared outcomes of three groups of patients; sensitized patients receiving desensitization therapy, non-sensitized patients and sensitized patients who did not undergo desensitization. At five-year follow-up, the risk of rejection was higher in desensitized patients (43% risk of treated rejection vs. 15% in non-desensitized sensitized patients and 12.6% in non-sensitized patients); mortality, risk of cardiac allograft vasculopathy, infection and non-fatal major adverse cardiac events was similar amongst the groups [21].
Rejection can result in a number of complications. Initially, diastolic allograft dysfunction can be observed due to myocardial edema [3]. Ultimately patients may develop systolic dysfunction [3]. The clinical manifestations of rejection are varied, from absence of symptoms or general malaise; to more cardiac specific signs including arrhythmias (atrial and ventricular arrhythmias), pericardial effusions, and symptoms such as exertional dyspnea, fatigue, hypotension and less commonly cardiogenic shock [3,22]. Though symptoms of allograft dysfunction may not be apparent, rejection may result in sudden cardiac death [23].
Other adverse consequences associated with rejection include cardiac allograft vasculopathy [3]. Patients hospitalized due to rejection during the first five years post-transplant are at a ~ 2-fold higher risk of developing cardiac allograft vasculopathy OR 1.93, 95% CI = 1.23-3.05 [24]. Rejection remains a common cause of death, the ISHLT (International Society of Heart and Lung Transplantation) registry reports that acute rejection caused up to 11% of deaths between one and three years post-transplant [25]. The increased risk of death differs according to the type of rejection experienced, with antibody-mediated rejection or mixed rejection having a higher risk. In a study of 801 heart transplant recipients, early (within 3 months post-transplant) acute cellular rejection, antibody-mediated rejection and mixed rejection were associated with an overall risk of cardiovascular mortality of 12.6%, 21.2%, and 18.0%, respectively [26].
Traditionally, surveillance endomyocardial biopsies are performed to monitor for rejection [3]. Though the regularity of their use varies by institution, endomyocardial biopsies are often performed in the three months post-transplant and less frequently for the remainder of the first year [3]. This time frame is consistent with the increased risk of rejection in the first six months following transplantation [27]. The necessity of routine endomyocardial biopsies after one year post transplant is unclear [28], however, endomyocardial biopsies are still performed for ‘cause' if patients have symptoms or graft dysfunction [3]. As an endomyocardial biopsy is an invasive procedure [29] with a high complication rate (6% of cases) [30], efforts are being made to develop other reliable testing methods. Gene-expression profiling (GEP - Allomap test) is one possible tool [29]. For low risk patients, this non-invasive test may be used to rule out an acute cellular rejection diagnosis between 6 months and 5 years post-transplant [31-33].
Immunotherapy is used both to prevent and treat rejection [8]. The widely used triple-regimen of immunosuppression (IS) involves corticosteroids, calcineurin inhibitors (CNIs), and anti-metabolites [2,8]. Patients receive larger doses of drugs such as corticosteroids at the beginning of the post-transplant period, as well as during instances of acute rejection [2]. Though the IS regimen is critical for the prevention and treatment of rejection, it is important to minimize significant side effects associated with these drugs [8]. Induction therapy-aggressive antibody IS used at the time of transplantation in an effort to avoid rejection [8] - is used in approximately 50% of patients [34]. Induction therapy is often used in sensitized patients to minimize the rejection risk, or in those with renal dysfunction to delay the initiation of CNIs [1,35].
Cardiac Allograft Vasculopathy
Cardiac allograft vasculopathy is an accelerated form of intimal hyperplasia that occurs in the coronaries of the transplanted heart. It has historically been a limiting factor for the long-term survival of heart transplantation, responsible for 32% of deaths after 5 years [36]. According to the 2015 ISHLT report, cardiac allograft vasculopathy was detectable by angiography in 8% of survivors within the first year, 30% by 5 years, and 50% by 10 years after transplant [36]. The diffuse and progressive nature of cardiac allograft vasculopathy explains some of the challenges associated with interventional therapies.
The pathophysiology of cardiac allograft vasculopathy involves both immune and non-immune mediated endothelial damage with changes that can be seen as early as 6 months post-transplant [37]. The earliest changes are characterized by intimal thickening of the proximal arteries followed by fibrofatty atheromatous plaque and ultimately diffuse fibrous thickening of the intima which can have overlying atheromatous plaques [37]. Unlike the focal and proximal nature of non-transplant coronary artery disease, cardiac allograft vasculopathy affects distal vessels as well. Intimal progression is accompanied by fibrosis of the media; whereas the capillaries remain relatively unaffected due to a lack of smooth muscle cells [37].
A recent systematic review summarizing cardiac allograft vasculopathy risk factors revealed a lack of consistent evidence and strength of association which prevented pooling of the data [38]. Independent predictors identified are cited in Table 2. Factors which led to the variation in results across different studies included: inadequate description of participants, inappropriate statistical methods and varying definitions of cardiac allograft vasculopathy [38].
![]()
Table 2: Risk factors for the development of cardiac allograft vasculopathy identified in various single-center observational studies.
View Table 2
The most widely used cardiac allograft vasculopathy screening test is coronary angiography. The recent ISHLT guidelines on cardiac allograft vasculopathy nomenclature classifies cardiac allograft vasculopathy into four categories: 0 (non-significant), 1 (mild disease), 2 (severe) and 3 (severe cardiac allograft vasculopathy associated with graft dysfunction) [39]. Severity parallels the degree of stenosis where severe degree is reached if the left main is > 50% or other primary vessels reach > 70% [40]. A major drawback of coronary angiography is its low sensitivity, meaning that it detects cardiac allograft vasculopathy in only 10-20% of patients after 1 year of transplantation when referenced to histopathologic examination [41]. This is especially true for the detection of early vascular lesions which appear to have < 25% diameter reduction. This issue is largely addressed by intravascular ultrasound, the current gold standard, which detects cardiac allograft vasculopathy in 50% of patients at one year post-transplant [37]. However, the size of the catheter limits the use of intravascular ultrasound to larger epicardial vessels [42].
Dobutamine stress echocardiography is the non-invasive test of choice, with specificities of up to 88% when referenced to intravascular ultrasound [43]. Furthermore, its excellent negative predictive value ranging from 92-100% makes it potentially useful to lengthen the time interval between angiographic screening [44,45]. Cardiac magnetic resonance, a safe and versatile non-invasive modality, has been shown to have a high diagnostic accuracy for cardiac allograft vasculopathy when using myocardial perfusion reserve index as a surrogate measure of myocardial blood flow [46]. Newer technologies such as the use of 18-fluoro-deoxyglucose-positron emission tomography (FDG-PET) and measurement of the release of adenosine triphosphate from activated lymphocytes show promise in the diagnosis of early cardiac allograft vasculopathy [47,48].
Denervation of the transplanted heart limits the usefulness of typical symptoms of coronary disease such as angina; leading to more serious late clinical presentations, heart failure and sudden death. Rapid progression of cardiac allograft vasculopathy (≥ 0.5 mm intimal thickness within 1-year) is associated with an incidence of death/myocardial infarction of 51% compared to 16% in those who have a smaller change in intimal thickness [49]. In a report from the UNOS database, 6% of patients with cardiac allograft vasculopathy experienced sudden cardiac death, with 45% of all sudden cardiac deaths being attributed to cardiac allograft vasculopathy [50]. The most recent ISHLT report found that those diagnosed with cardiac allograft vasculopathy by angiography within 3 years of transplant had a mortality rate at 5 and 10 years of 28% and 50% respectively [36].
Statin therapy post-transplant has been shown to reduce the risk of cardiac allograft vasculopathy [51,52]. For established cardiac allograft vasculopathy, high-intensity statin therapy (80 vs. 10 mg atorvastatin) resulted in a 2.2% absolute reduction (or 22% relative risk reduction) in the rate of major cardiovascular events (death from cardiac allograft vasculopathy, nonfatal myocardial infarction, resuscitation after cardiac arrest, or fatal or nonfatal stroke) [53,54]. IS therapy with proliferation signal inhibitors such as everolimus and sirolimus, have been clinically shown to prevent/slow the progression of cardiac allograft vasculopathy. In two separate trials, patients treated with sirolimus or everolimus as compared to azathioprine or mycophenolate mofetil had a lower incidence of cardiac allograft vasculopathy (12.5% vs. 26.7%) between 1 and 2 years [55,56]. More recently, similar results were reported in the SCHEDULE trial comparing everolimus therapy and early withdrawal of cyclosporine versus standard CNI [57].
Other options to prevent cardiac allograft vasculopathy progression including IS augmentation with intravenous methylprednisolone and aggressive antibody IS (antithymocyte globulin) have been studied in a small study (22 patients with cardiac allograft vasculopathy) showing regression in established cardiac allograft vasculopathy [58].
A recent observational study found that percutaneous coronary intervention (PCI) was associated with a lower 5-year mortality in patients with treatable vessels in comparison to those patients who did not have technically suitable vessels (48.5% vs. 75% ) [59]. Similarly, in a small single-center study of coronary artery bypass grafting, 10/13 patients (77%) were alive after a mean follow-up of 3.25 years [60]. For selected patients with severe cardiac allograft vasculopathy retransplantation remains the best option [36].
Graft Dysfunction
Graft dysfunction occurs frequently post-heart transplant, either immediately after transplantation, within the first 30-days or late, appearing after one year of normal graft function.
Early graft dysfunction
A recent report from the ISHLT shows the incidence of early graft dysfunction to range between 2% to 28% [61]. This is due to a wide variety of definitions and criteria used for the diagnosis of graft dysfunction, ranging from death or need for re-transplantation, to reduced left ventricular ejection fraction (< 40%) or elevated intra-cardiac pressures (for diastolic dysfunction or right ventricular dysfunction) [61-63].
The ISHLT developed a consensus-based definition and classification for early graft failure to improve standardization [61]. Early graft failure is categorized as primary or secondary depending on the time and cause of onset. Early primary graft dysfunction (or simply primary graft dysfunction) occurs within the first 24-hour post-transplant with an unknown cause. Primary graft dysfunction is further classified as right or left ventricular in nature. Left ventricular primary graft dysfunction is further sub-classified according to the level of medical and mechanical support required; mild (need for low dose intravascular inotropes), moderate (need for high dose intravascular inotropes or intra-aortic balloon pump implant), or severe (need for mechanical circulatory support excluding intra-aortic balloon pump). Secondary early graft dysfunction is due to an identifiable cardiac insult such as hyper-acute or acute rejection, or pulmonary hypertension.
Risk factors for primary graft dysfunction are variable and difficult to put into context due to previous variability in its definition. Despite this, donor and recipient risk factors, and complications during the perioperative period play a role in modifying risk of primary graft dysfunction. Recipient risk factors include older recipient age (age ≥ 60 years, relative risk - RR - 1.9; 95% CI 1.1-3.7) [62], presence of pulmonary hypertension [61], bridging with inotropes or mechanical circulatory support, and use of mechanical ventilation prior to transplant (odds ratio-OR- /RR ranging from 2.1-10.29) [62,64,65]. Donor characteristics such as older age (RR 1.7; 95% CI 1.1-3.1) [62,64], sex mismatch (female donor to male recipient implying an undersized donor heart) (OR 1.23; 95% CI 1.03-1.47) [66], and causes of brain death such as trauma and intracerebral bleeding increase the risk of early primary graft failure (OR 2.45; p-value < 0.01) [67,68]. Perioperative factors such as prolonged ischemic time has also been shown to increase the risk of primary graft dysfunction (RR 1.9; 95% CI 1.1-3.5) [64,67].
Primary graft dysfunction is associated with decreased post-transplant survival. A recent study looking at the association of primary graft dysfunction with overall 1-year survival, using unadjusted analysis, found that with increasing severity in primary graft dysfunction, there is a decrease in survival at 1-year (94%, 75%, and 44% 1-year survival for mild, moderate, and severe respectively) [69].
Mechanical support, extracorporeal membrane oxygenation or ventricular assist devices may be used to treat cases of severe graft dysfunction [70-72]. In patients supported with extracorporeal membrane oxygenation, cannulation in the operating room or within the first seven days post-transplant has a success rate (survival to discharge) of 50% [70]. Selected patients with severe graft dysfunction may be considered for re-transplantation [72]. Registry data from UNOS and ISHLT suggests the probability of re-transplantation to be 0.1% at 30 days, and increasing to 14% at 3 months [64,73].
.
Figure 1: Cumulative incidence of complications during post-heart transplant period based on published data [73,89].
CKD: Chronic Kidney Disease; CAV: Cardiac Allograft Vasculopathy
*The incidence for rejection is only representative of patients who were hospitalized for rejection, reflecting that these cases are the most severe, and thus, of greatest relevance.
*The incidence for the various complications are not mutually exclusive, explicitly stated: patients in one category of complication may also have another.
*The data for CAV, CKD, and malignancy were derived from Kaplan-Meier survival curves.
*CKD defined as serum creatinine greater than 2.5 mg/dL.
View Figure 1
Late graft dysfunction
Late graft dysfunction remains a common cause of death, with an increasing cumulative incidence of 4.3%, 6.7%, and 9.9% at 1, 5, and 10 years respectively [73]. Late graft dysfunction, left ventricular ejection fraction ≤ 30%, has an incidence of 12% in a mean follow-up of four years [74]. The common causes of late graft dysfunctionare acute cellular rejection (325), cardiac allograft vasculopathy (27%) and antibody-mediated rejection (20%). Approximately 21% of late graft dysfunction is unexplained [75]. Patients with no identifiable cause for graft dysfunction have the worst prognosis, with a 62% mortality 1-year after diagnosis (30% in patients with graft dysfunction (left ventricular ejection fraction < 30%) due to antibody-mediated rejection and cardiac allograft vasculopathy, 19% due to cell-mediated rejection) [75]. Risk factors for late graft dysfunction overlap with those of cardiac allograft vasculopathy and rejection. Please refer to the respective sections discussing these two complications.
Late graft dysfunction is one of the major causes of death post heart transplant. Registry data from the ISHLT shows late graft failure to be responsible for 15.7% of deaths up to the first year, 29% from 1 to 3 years, and 17.5% from 10 to 15 years post-transplant [73]. Re-transplantation may be reasonable in eligible patients with late graft dysfunction [73]. Better risk prediction of graft dysfunction may allow for enhanced prognostication, earlier intervention, targeted therapies and potentially earlier assessment for re-transplantation. These in turn may reduce the number of deaths attributed to graft dysfunction.
Chronic Kidney Disease
The dramatic improvement in outcomes with heart transplantation over the last two decades can largely be attributed to the use of CNIs (cyclosporine or tacrolimus) [76]. Although these drugs play a critical role in preventing graft rejection, they have side effects, including nephrotoxicity [76]. In fact, by ten years post-transplant, 19.3% of heart transplant recipients will have developed CKD (defined as creatinine > 2.5 mg/dl) [73]. Certain individuals have a higher likelihood of developing CKD. Patients with a preoperative impaired renal function are the most susceptible, with a 3-fold higher risk in patients with pre-transplant glomerular filtration rate of < 60 ml/min/1.73 m2 [77]. Other important risk factors include active hepatitis C virus (HR 2.87, 95% CI 1.24-6.67), advancing age (HR 1.24, 95% CI 1.22-1.26; per 10 year increment), female sex (HR 1.97, 95% CI 1.56-2.50), and diabetes (HR 1.44, 95% CI 1.04-1.99) [77].
The development of acute kidney injury defined as an early increase in serum creatinine of ≥ 0.3 mg/dl [or 26 umol/L] or ≥ 50% increase in serum creatinine from pre-transplant, or the need of early post-operative dialysis) is a frequent complication during the post-operative period, affecting 25% of heart transplant recipients [78]. Acute kidney injury is also associated with an increased risk for developing CKD (RR 3.03, p < 0.05) [79] and markedly increased mortality. Patients with a serum creatinine level greater than the critical threshold (as defined above) have 6% increased mortality at 3-months post-transplant [78]. Additionally, patients that require early post-transplant dialysis have 18% increased mortality at 3 months post-transplantation, respectively [78].
While at-risk patients are now easily identifiable, preventing CKD is difficult. Preventing rejection episodes and atherosclerosis with statins and omega-3-fatty acids, reducing the number of coronary angiographies, treating hypertension and screening for renal artery stenosis may prevent the development of renal dysfunction [80]. However, despite these measures CKD remains a common complication.
The presence of CKD contributes to other comorbidities such as, hyperkalemia, hypertension, and proteinuria, reducing long term survival. In fact, mortality for patients with severe CKD is 14% greater by five years post-transplant, and 19% greater by ten years after transplantation, compared to patients that do not have CKD [73].
Given that the mainstay of IS therapy contributes substantially to CKD, one possible option is the use of alternative non-nephrotoxic IS drugs. Several studies have evaluated using alternate agents (such as sirolimus, everolimus, and mycophenolate mofetil), minimizing (lowering the dose), discontinuing (stopping the drug after exposure), or avoiding (never administering the drug) CNIs in an attempt to improve renal function. A recent study evaluating CNI minimization strategies based on addition of everolimus or mycophenolate mofetil found that creatinine clearance was stable in patients who received a very low dose of cyclosporine with everolimus, and was even better in patients that received low dose cyclosporine and mycophenolate mofetil [81,82]. However, there is a trend towards higher episodes of rejection in patients with a minimized dose of CNI [82].
CNI discontinuation and sirolimus initiation may also lead to improvements in renal function. Heart transplant recipients that were converted from CNI to sirolimus had improved creatinine clearance compared to patients that remained on CNI-based IS [83]. However, the risk of rejection was higher in the CNI-free group (of the 15 patients who experienced an episode of rejection, 14 were receiving the sirolimus-based CNI-free treatment) [83].
While both CNI minimization and discontinuation have been studied, CNI discontinuation appears to be more effective at improving renal function than CNI minimization. While creatinine clearance remained stable in patients that had a reduction in their CNI dose, it improved in patients that had their CNI dose withdrawn and sirolimus initiated [84]. Additionally, patients in the reduced dose of CNIs group required dialysis more frequently, and had more episodes of rejection, than patients that had their CNI discontinued [84]. However, there were a greater number of adverse events, such as: infection, edema, bone marrow toxicity, and gastrointestinal side effects, in patients who received sirolimus [84] highlighting the need to balance both the benefits and risks of each immunosuppressant carefully.
CNI avoidance was evaluated in a small study where eight heart transplant recipients were started on a CNI-free regimen consisting of mycophenolate mofetil, sirolimus, and prednisone, immediately after transplantation [85]. These patients experienced a decrease in serum creatinine; however, rejection episodes occurred in two patients [85]. This is consistent with the increased incidence of acute rejection (OR 1.74, 95% CI 1.08-2.81) that is seen in kidney transplant patients who receive a sirolimus-based CNI-free regimen compared to kidney transplant recipients treated only with CNIs [86].
In addition to modifying IS therapy, heart transplant recipients with CKD may need dialysis or renal transplantation. The risk of requiring chronic dialysis or renal transplantation by ten years after transplantation is 5.9% and 3.6%, respectively among overall transplant recipients [73]. A recent study found that patients that require chronic dialysis after cardiac transplantation have a 40% survival at five years post-transplant, compared to those requiring temporary or no dialysis; who have a survival of 78% and 82%, respectively [87]. In heart transplant recipients, renal graft survival is only 61% after five years [88]. However, it is important to note that heart transplant recipients that receive a renal transplant have a 43% greater chance of survival compared to patients that remain on dialysis [88]. Ultimately, clinicians must weigh the pros and cons associated with IS therapy modification, dialysis, and renal transplantation on a patient-by-patient basis.
Infection
IS therapy can lead to an increased risk of infection due to the suppression of the hosts immune response. Many heart transplant patients will develop an infection following transplant, with a cumulative incidence of 85% after 5 years [89]. In particular, immunocompromised individuals are at an increased risk of opportunistic viral and bacterial infections. Most infections involve the respiratory system, urinary tract, and the skin [90]. Commonly reported infections include cytomegalovirus, herpes simplex virus, Epstein-Barr virus, varicella zoster virus, tuberculosis, and pneumonia [91,92]. Invasive fungal infections, such as Aspergillus and Candida, are less common in heart-transplant recipients; however, they are associated with significant morbidity and mortality [93]. A more comprehensive list of infections based on time after transplant is available in Table 3.
![]()
Table 3: Prevalent infections based on post-transplant time [129,130].
View Table 3
Infections are common in the first 6 months after transplant with decreasing risk as IS is reduced over time and upon a better understanding of an individual patient's risk of rejection [91]. Specifically, there are 8.78 infectious episodes/1000 transplant days in the first month following heart transplant and 2.33 in months 2-6, but only 0.34 episodes after 6 months [94]. Both active and latent infections can be transmitted from the donor or derived/acquired from the recipient. Generally, the mode of infection follows a common pattern. In the first month, infections tend to be nosocomial, from months 1-6, opportunistic infections or previously latent infections tend to dominate, and infections after 6 months tend to be acquired in the community [91].
Several risk factors for post-transplant infections have been reported, and vary slightly across studies. In heart-transplant recipients, age is a strong predictor of infection, with both younger and older individuals having an increased risk of infection [95]. Other risk factors change depending on the time after transplant and the type of infection. Older studies have shown that, specifically for heart-transplant patients, risk factors for all infection in the first 6 months include ventilator support or ventricular assist devices at time of transplant, black donor race, female sex, and antibody induction therapy [96]. In comparison, more recent multivariate analyses have shown that, in solid-organ transplantation, risk factors for infection after 6 months include chronic graft dysfunction, re-operation, acute rejection in the early post-transplant period, relapsing viral infections other than cytomegalovirus, and previous bacterial infections [94].
While much progress has been made in reducing the risks and consequences of infection, it remains a significant cause of morbidity, mortality, and hospital readmissions in post-heart transplant patients [91]. Infection is one of the leading causes of death in the first year after transplant, being the primary cause of death in 25-32% of patients [25,97]. The risk of death due to infection is highest between 1 month and 1 year following transplant and then decreases significantly after the first year post-transplant [25]. Infection is also associated with 17% of hospital readmissions in the first year following heart transplant [73].
The specific consequences of infection vary depending on the micro-organism, the ability of the host to generate an effective immune response, and prescribed therapies. All infections have the potential to cause sepsis and multi-organ failure, which is associated with up to 50% mortality [98]. Severe infections may also necessitate decreases in IS, which can lead to an increased risk of allograft rejection [99].
Cytomegalovirus is an important infection in heart-transplant patients, affecting 47% of patients in the first year post-transplant despite pre-emptive and prophylactic therapies [100]. Clinical manifestations of cytomegalovirus can range from flu-like symptoms to organ infiltration and damage. Furthermore, cytomegalovirus can indirectly lead to cardiac allograft vasculopathy, post-transplant lymphoproliferative disorder, and suppression of the immune system, which can further predispose individuals to opportunistic infections and malignancy [101]. While cytomegalovirus infection is still associated with mortality (up to 0.7% of all deaths), the prognosis has improved over time [25,102]. This is likely due to implementation of donor/recipient serology testing, prophylactic use of ganciclovir in high-risk patients, and regular monitoring of viral load following transplant [102].
Infections should be treated in the potential recipient before transplantation to prevent exacerbation once IS is started [91]. In the case of chronic infections such as hepatitis C virus or human immunodeficiency virus (HIV), a positive recipient status does not necessarily preclude transplant. While there is some variability in the literature, after adjusting for donor and recipient factors, there is no difference in the survival of hepatitis C virus positive and negative recipients [103,104]. Similarly, limited available data suggests that carefully selected HIV-positive recipients can expect good outcomes [105]. Furthermore, 2016 guidelines have also noted that Chagas disease and tuberculosis (non-active disease) should not exclude nor delay recipients from transplantation, however close monitoring and appropriately timed treatment is required [106].
Donors and recipients should be screened, using serology testing, for common infections (Table 4). Recipients should be evaluated for sufficient immunization against common pathogens, and educated on how to prevent infection post-transplant [107].
![]()
Table 4: Recommendations for potential donor and recipient infection screening prior to transplantation [91,131].
View Table 4
In the early pre-operative period, the recipient should also be started on prophylactic anti-microbials, particularly against Staphylococcus aureus [107]. This is often administered as cefalosporins, or if patients have an allergy, as vancomycin [108]. Following transplant, ISHLT guidelines recommend differing antiviral strategies depending on the cytomegalovirus status of the donor and the recipient, which are summarized in Table 5. Furthermore, all patients should receive prophylactic anti-protozoals against Pneumocystis jiroveci pneumonia for 1-3 months, and prophylactic antifungals, such as nystatin, following extubation in order to prevent mucocutaneous candidiasis [107].
![]()
Table 5: ISHLT recommendations for anti-viral prophylaxis and pre-emptive therapies [107].
View Table 5
Following discharge, patients should also be routinely monitored for infections, particularly for viral loads of cytomegalovirus, and appropriate therapies should be started when infection is suspected [107]. Health care providers should also have a low tolerance for suspecting infection, as IS drugs may mask symptoms of infection such as fever [102]. When infection is suspected, it is recommended that therapy include broad-spectrum antibiotics, and in some cases, antiviral and antifungal agents, depending on clinical suspicion [99].
During an acute infectious episode, clinicians should consider decreasing the doses of IS as deemed necessary by the severity of the infection [99]. In the case of patients at a high risk of cytomegalovirus, everolimus is an option for IS therapy. This is due to its ability to reduce the odds of cytomegalovirus infection and cytomegalovirus disease compared to both standard IS and prophylactic drugs [109]. Finally, every attempt should be made to gradually taper doses of IS drugs following transplant, to reduce risk of infection and other long-term complications of IS [107].
Malignancies
Another life-threatening consequence of long-term IS following transplantation is cancer. IS drug regimens predispose individuals to malignancy through several mechanisms, including impaired immune responses against malignant cells and oncogenic viruses [110]. The incidence of malignancy increases with time following transplant, with 2.6%, 14.1%, and 27.9% of individuals developing any malignancy after 1, 5, and 10 years respectively [25]. This incidence is approximately 3 to 4-fold greater than age-matched controls in the general population [111].
Skin malignancies and lymphomas are the most commonly reported cancers, with skin malignancies affecting 19.8% of patients, and lymphomas 1.8% of patients 10 years following heart transplant [25]. The most prevalent skin malignancies following transplant include basal cell and squamous cell carcinomas [112]. In comparison, lymphomas are generally due to post-transplant lymphoproliferative disorder [113]. Early post-transplant lymphoproliferative disorder (within 1 year of transplant), is most commonly caused by infection with Epstein-Barr virus and typically affects B-cells. Late post-transplant lymphoproliferative disorder (> 1 year following transplant) is more likely to be Epstein-Barr virus negative and non-B cell [114]. Other reported cancers following heart transplant include Kaposi's sarcoma, adenocarcinoma, melanoma, as well as solid tumors affecting the prostate, lung, bladder, breast, cervix, colon, and kidney [25,115].
Risk factors for malignancy following heart transplant can be divided into general and cancer-specific categories. Generally, cancer risk following transplant is dependent on the duration and intensity of IS, as well as age [25,115].
Cancer-specific risk factors for skin malignancy following heart transplant include age over 40 at time of transplant, light skin type, and high sunlight exposure [116,117]. In comparison, risk factors for post-transplant lymphoproliferative disorder include Epstein-Barr virus infection, high intensity of IS, and antibody induction therapy using OKT3 [118,119]. Multivariate analyses have also demonstrated that strong risk factors for the development of non-skin malignancies following heart transplant include antibody induction agents (HR 2.38, 95% CI 1.40-4.07), donor history of cancer (HR 1.95, 95% CI 1.09-3.48), female sex (HR 1.87, 95% CI 1.26-2.78), as well as pacemaker prior to discharge (HR 1.81, 95% CI 1.17-2.80). Other reported risk factors in this analysis include recipient age, ischemic time, and implantable cardioverter defibrillator prior to discharge [25]. However, it should be noted that some of these identified risk factors from Lund, et al [25]. may only represent associations without a causative relationship.
Malignancy is one of the most common causes of death 3-5 years following transplant. In fact, up to 24% of deaths after 5 years following transplant are directly caused by malignancy. This is especially true of individuals who develop lymphomas as compared to skin malignancies [25].
Patients who develop malignancy may require a reduction in their IS doses, which can lead to acute rejection [113]. Such reduction is often performed in the case of post-transplant lymphoproliferative disorder, as minimizing IS has been shown to improve overall survival. However, this survival benefit is at the expense of a 10% increased risk of sudden cardiac death due to acute rejection, highlighting the challenge in balancing IS versus cancer risk [120]. Current guidelines suggest that IS should not be reduced in patients with solid tumors that are unrelated due to the lymphoid system, due to a lack of sufficient evidence to support the benefit [107]. Either way, reductions in IS doses should be closely monitored and individualized in an attempt to balance malignancy versus allograft rejection [121].
Specific IS drugs may prevent the recurrence of malignancy. Proliferation signal inhibitors, such as sirolimus, have been shown to have anti-neoplastic properties in addition to their IS actions [122]. This contrasts with the commonly used CNIs, which have been shown to promote malignancy independently of their IS functions [123]. In patients with malignancy, proliferation signal inhibitors may be useful in preventing cancer recurrence [122], however, there is no clear evidence that they reduce overall cancer risk [112].
Finally, to prevent malignancy, all heart transplant recipients should receive age appropriate screening for breast, colon, and prostate cancer, as well as increased skin cancer screening with yearly dermatologic exams [107]. Furthermore, high-risk patients should be evaluated closely for the development of post-transplant lymphoproliferative disorder through regular screening of Epstein-Barr virus load [124]. For those at particularly high risk of malignancy, reduction in chronic IS should be done if possible [25]. If cancer does occur, IS doses should be altered as appropriate, and patients should receive treatments specific to their cancer, such as chemotherapy or anti-B cell monoclonal antibodies in the case of post-transplant lymphoproliferative disorder [113]. With regular screening and balanced, individualized interventions, it may be possible to reduce this common complication.
Conclusions
Heart transplant is a life improving and life-saving therapy that is associated with a risk of significant complications. Physicians, patients and families should be prepared to deal with these risks by acting collaboratively to prevent, identify and treat complications as they arise, with the ultimate goal to improve survival and quality of life after heart transplant.
References
-
Lindenfeld J, Geraldine G Miller, Simon F Shakar, Ronald Zolty, Brian D Lowes, et al. (2004) New Drugs and Technologies: Drug Therapy in the Heart Transplant Recipient: Part 1: Cardiac Rejection and Immunosuppressive Drugs. Circulation 110: 3734-3740.
-
Mangini S, Bárbara Rubim Alves, Odílson Marcos Silvestre, Philippe Vieira Pires, Lucas José Tachotti Pires, et al. (2015) Heart transplantation: review. Einstein (São Paulo)13: 310-318.
-
Taylor DO, Bruno Meiser, Steven Webber, David A Baran, Michael Carboni, et al. (2010) The international society of heart and lung transplantation guidelines for the care of heart transplant recipients. J Hear Lung Transplant 29: 914-956.
-
Stehlik J, Edwards LB, Kucheryavaya AY, Aurora P, Christie JD, et al. (2010) The Registry of the International Society for Heart and Lung Transplantation: Twenty-seventh official adult heart transplant report-2010. J Hear Lung Transplant 29: 1089-1103.
-
Yusabai A, A Mehrnia, M Kamgar, M Sampaio, E Huang, et al. (2013) Risk Factors for Acute Rejection in Heart Transplant Recipients. Am J Transplant.
-
Parham P (2014) The Immune System, Fourth Edition, Garland Science.
-
Lavee J, Kormos RL, Duquesnoy RJ, Zerbe TR, Armitage JM, et al. (1991) Influence of panel-reactive antibody and lymphocytotoxic crossmatch on survival after heart transplantation. J Heart Lung Transplant 10: 921-929.
-
Chang DH, Kittleson MM and Kobashigawa Ja (2014) Immunosuppression following heart transplantation: prospects and challenges. Immunotherapy 6: 181-194.
-
Kobashigawa J, Crespo-Leiro MG, Ensminger SM, Reichenspurner H, Angelini A, et al. (2011) Report from a consensus conference on antibody-mediated rejection in heart transplantation. J Heart Lung Transplant 30: 252-269.
-
Reed EF, Demetris AJ, Hammond E, Itescu S, Kobashigawa JA, et al. (2006) Acute antibody-mediated rejection of cardiac transplants. J Heart Lung Transplant 25: 153-159.
-
Cecka JM (2010) Calculated PRA (CPRA): the new measure of sensitization for transplant candidates. Am J Transplant 10: 26-29.
-
Kobashigawa J, Mehra M, West L, Kerman R, George J, et al. (2009) Report from a consensus conference on the sensitized patient awaiting heart transplantation. J Heart Lung Transplant 28: 213-225.
-
Stewart S, Winters G, Fishbein MC, Tazelaar HD, Kobashigawa J, et al. (2005) Revision of the 1990 working formulation for the standardization of nomenclature in the diagnosis of heart rejection. J Heart Lung Transplant 24: 1710-1720.
-
Nwakanma LU, Williams JA, Weiss ES, Russell SD, Baumgartner WA, et al. (2007) Influence of pretransplant panel-reactive antibody on outcomes in 8,160 heart transplant recipients in recent era. Ann Thorac Surg 84: 1556-1562.
-
Smith JD, Banner NR, Hamour IM, Ozawa M, Goh A, et al. (2011) De novo donor HLA-specific antibodies after heart transplantation are an independent predictor of poor patient survival. Am J Transplant 11: 312-319.
-
Patel JK, Kobashigawa JA (2012) Improving survival during heart transplantation: diagnosis of antibody-mediated rejection and techniques for the prevention of graft injury. Future Cardiol 8: 623-635.
-
Kilic A, Emani S, Sai-Sudhakar CB, Higgins RS, Whitson BA (2014) Donor selection in heart transplantation. J Thorac Dis 6: 1097-1104.
-
Ross H, Tinckam K, Rao V and West LJ (2010) In praise of ventricular assist devices-mechanical bridge to virtual crossmatch for the sensitized patient. Journal of Heart and Lung Transplantation 29: 728-730.
-
Stehlik J, Islam N, Hurst D, Kfoury AG, Movsesian MA, et al. (2009) Utility of virtual crossmatch in sensitized patients awaiting heart transplantation. J Heart Lung Transplant 28: 1129-1134.
-
Zangwill S, Ellis T, Stendahl G, Zahn A, Berger S, et al. (2007) Practical application of the virtual crossmatch. Pediatr Transplant 11: 650-654.
-
Kobashigawa JA, Patel JK, Kittleson MM, Kawano MA, Kiyosaki KK, et al. (2011) The long-term outcome of treated sensitized patients who undergo heart transplantation. Clin Transplant 25: E61-67.
-
Fishbein MC, Kobashigawa J (2004) Biopsy-negative cardiac transplant rejection: etiology, diagnosis, and therapy. Curr Opin Cardiol 19: 166-169.
-
Chantranuwat C, Blakey JD, Kobashigawa JA, Moriguchi JD, Laks H, et al. (2004) Sudden, unexpected death in cardiac transplant recipients: an autopsy study. J Heart Lung Transplant 23: 683-689.
-
Taylor DO, Edwards LB, Mohacsi PJ, Boucek MM, Trulock EP, et al. (2003) The Registry of the International Society for Heart and Lung Transplantation: Twentieth Official Adult Heart Transplant Report--2003. J Hear Lung Transplant 22: 616-624.
-
Lund LH, Edwards LB, Kucheryavaya AY, Dipchand AI, Benden C, et al. (2013) The Registry of the International Society for Heart and Lung Transplantation: Thirtieth Official Adult Heart Transplant Report--2013; focus theme: age. J Heart Lung Transplant 32: 951-964.
-
Kfoury AG, Hammond ME, Snow GL, Drakos SG, Stehlik J, et al. (2009) Cardiovascular Mortality Among Heart Transplant Recipients With Asymptomatic Antibody-Mediated or Stable Mixed Cellular and Antibody-Mediated Rejection. J Hear Lung Transplant 28: 781-784.
-
Rizeq MN, Masek MA, Billingham ME (1994) Acute rejection: significance of elapsed time after transplantation. J Heart Lung Transplant 13: 862-868.
-
Stehlik J, Starling RC, Movsesian MA, Fang JC, Brown RN, et al. (2006) Utility of long-term surveillance endomyocardial biopsy: a multi-institutional analysis. J Heart Lung Transplant 25: 1402-1409.
-
Andrew J, Macdonald P (2015) Latest developments in heart transplantation: A Review. Clin Ther 37: 2234-2241.
-
Deckers JW, Hare JM, Baughman KL (1992) Complications of transvenous right ventricular endomyocardial biopsy in adult patients with cardiomyopathy: A seven-year survey of 546 consecutive diagnostic procedures in a tertiary referral center. J Am Coll Cardiol 19: 43-47.
-
Pham MX, Teuteberg JJ, Kfoury AG, Starling RC, Deng MC, et al. (2010) Gene-expression profiling for rejection surveillance after cardiac transplantation. N Engl J Med 362: 1890-1900.
-
Deng MC, Eisen HJ, Mehra MR, Billingham M, Marboe CC, et al. (2006) Noninvasive discrimination of rejection in cardiac allograft recipients using gene expression profiling. Am J Transplant 6: 150-160.
-
Keslar K, Rodriguez ER, Tan CD, Starling RC and Heeger PS (2008) Complement gene expression in human cardiac allograft biopsies as a correlate of histologic grade of injury. Transplantation 86: 1319-1321.
-
Stehlik J, Edwards LB, Kucheryavaya AY, Benden C, Christie JD, et al. (2011) The Registry of the International Society for Heart and Lung Transplantation: Twenty-eighth Adult Heart Transplant Report--2011. J Heart Lung Transplant 30: 1078-1094.
-
Uber PA, Mehra MR (2007) Induction therapy in heart transplantation: is there a role? J Heart Lung Transplant 26: 205-209.
-
Yusen RD, Edwards LB, Kucheryavaya AY, Benden C, Dipchand AI, et al. (2015) The Registry of the International Society for Heart and Lung Transplantation: Thirty second Official Adult Lung and Heart-Lung Transplantation Report--2015; Focus Theme: Early Graft Failure. J Hear Lung Transplant 34: 1264-1277.
-
Ramzy D, Rao V, Brahm J, Miriuka S, Delgado D, et al. (2005) Cardiac allograft vasculopathy: a review. Can J Surg 48: 319-327.
-
Braga JR, Santos IS, McDonald M, Shah PS, Ross HJ (2012) Factors associated with the development of cardiac allograft vasculopathy--a systematic review of observational studies. Clin Transplant 26: E111-124.
-
Mehra MR, Crespo-Leiro MG, Dipchand A, Ensminger SM, Hiemann NE, et al. (2010) International Society for Heart and Lung Transplantation working formulation of a standardized nomenclature for cardiac allograft vasculopathy-2010. Journal of Heart and Lung Transplantation 29: 717-727.
-
Schmauss D, Weis M (2008) Cardiac allograft vasculopathy: recent developments. Circulation 117: 2131-2141.
-
Johnson DE, Alderman EL, Schroeder JS, Gao SZ, Hunt S, et al. (1991) Transplant coronary artery disease: histopathologic correlations with angiographic morphology. J Am Coll Cardiol 17: 449-457.
-
Cai Q, Rangasetty UC, Barbagelata A, Fujise K, Koerner MM (2011) Cardiac allograft vasculopathy: advances in diagnosis. Cardiol Rev 19: 30-35.
-
Akosah KO, Mohanty PK, Funai JT, Jesse RL, Minisi AJ, et al. (1994) Noninvasive detection of transplant coronary artery disease by dobutamine stress echocardiography. J Heart Lung Transplant 13: 1024-1038.
-
Spes CH, Klauss V, Mudra H, Schnaack SD, Tammen AR, et al. (1999) Diagnostic and prognostic value of serial dobutamine stress echocardiography for noninvasive assessment of cardiac allograft vasculopathy: a comparison with coronary angiography and intravascular ultrasound. Circulation 100: 509-515.
-
Akosah KO, Olsovsky M, Kirchberg D, Salter D, Mohanty PK (1996) Dobutamine stress echocardiography predicts cardiac events in heart transplant patients. Circulation 94: II283-11288.
-
Chih S, AM Crean, AC Alba, CS Fan, C Manlhiot, et al. (2016) Perfusion cardiac magnetic resonance imaging in cardiac allograft vasculopathy. J Hear Lung Transplant 35: S196.
-
Sasaki M, Tahara N, Abe T, Ueno T, Fukumoto Y (2016) FDG-PET reveals coronary artery inflammation proceeding to cardiac allograft vasculopathy progression. Eur Heart J 37: 2413.
-
Cheng R, Azarbal B, Yung A, Patel JK, Chang DH, et al. (2016) Elevated immune monitoring as measured by increased adenosine triphosphate production in activated lymphocytes is associated with accelerated development of cardiac allograft vasculopathy after cardiac transplantation. J Hear Lung Transplant 35: 1018-1023.
-
Tuzcu EM, Kapadia SR, Sachar R, Ziada KM, Crowe TD, et al. (2005) Intravascular ultrasound evidence of angiographically silent progression in coronary atherosclerosis predicts long-term morbidity and mortality after cardiac transplantation. J Am Coll Cardiol 45: 1538-1542.
-
Vakil K, Taimeh Z, Sharma A, Abidi KS, Colvin M, et al. (2014) Incidence, predictors, and temporal trends of sudden cardiac death after heart transplantation. Heart Rhythm 11: 1684-1690.
-
Kobashigawa JA, Moriguchi JD, Laks H, Wener L, Hage A, et al. (2005) Ten-year follow-up of a randomized trial of pravastatin in heart transplant patients. J Heart Lung Transplant 24: 1736-1740.
-
Wenke K, Meiser B, Thiery J, Nagel D, von Scheidt W, et al. (2003) Simvastatin initiated early after heart transplantation: 8-year prospective experience. Circulation 107: 93-97.
-
LaRosa JC, Grundy SM, Waters DD, Shear C, Barter P, et al. (2005) Intensive lipid lowering with atorvastatin in patients with stable coronary disease. N Engl J Med 352: 1425-1435.
-
Sieg A, Weeks P, Krustchinsky L and Rajapreyar I (2016) Statin Therapy in Cardiac Allograft Vasculopathy Progression in Heart Transplant Patients: Does Potency Matter? Transpantation Rev 30: 178-186.
-
Kobashigawa Ja, Pauly DF, Starling RC, Eisen H, Ross H, et al. (2013) Cardiac allograft vasculopathy by intravascular ultrasound in heart transplant patients: substudy from the Everolimus versus mycophenolate mofetil randomized, multicenter trial. JACC Heart Fail 1: 389-399.
-
Keogh A, Richardson M, Ruygrok P, Spratt P, Galbraith A, et al. (2004) Sirolimus in de novo heart transplant recipients reduces acute rejection and prevents coronary artery disease at 2 years: a randomized clinical trial. Circulation 110: 2694-2700.
-
Andreassen AK, B Andersson, F Gustafsson, H Eiskjær, G Rådegran, et al. (2015) Three Year Follow Up of the Randomized SCHEDULE Trial with Everolimus initiation and Early Withdrawal of Calcineurin Inhibitor Therapy in De Novo Heart Transplant Recipients- A Multicenter, Randomized Scandinavian Trial. J Hear Lung Transplant 34: S129-S130.
-
Lamich R, Ballester M, Martí V, Brossa V, Aymat R, et al. (1998) Efficacy of augmented immunosuppressive therapy for early vasculopathy in heart transplantation. J Am Coll Cardiol 32: 413-419.
-
Agarwal S, Parashar A, Kapadia SR, Tuzcu EM, Modi D, et al. (2014) Long-term mortality after cardiac allograft vasculopathy: implications of percutaneous intervention. JACC Heart Fail 2: 281-288.
-
Bhama JK, Nguyen DQ, Scolieri S, Teuteberg JJ, Toyoda Y, et al. (2009) Surgical revascularization for cardiac allograft vasculopathy: Is it still an option? J Thorac Cardiovasc Surg 137: 1488-1492.
-
Kobashigawa J, Zuckermann A, Macdonald P, Leprince P, Esmailian F, et al. (2014) Report from a consensus conference on primary graft dysfunction after cardiac transplantation. J Heart Lung Transplant 33: 327-340.
-
Segovia J, Cosío MD, Barceló JM, Bueno MG, Pavía PG, et al. (2011) RADIAL: a novel primary graft failure risk score in heart transplantation. J Heart Lung Transplant 30: 644-651.
-
Siniawski H, Dandel M, Lehmkuhl HB, Hiemann N, Kemper D, et al. (2012) Clinical, haemodynamic and echocardiographic features of early cardiac graft dysfunction. Kardiol Pol 70: 1010-1016.
-
Russo MJ, Iribarne A, Hong KN, Ramlawi B, Chen JM, et al. (2010) Factors associated with primary graft failure after heart transplantation. Transplantation 90: 444-450.
-
Young JB, Hauptman PJ, Naftel DC, Ewald G, Aaronson K, et al. (2001) Determinants of early graft failure following cardiac transplantation, a 10-year, multi-institutional, multivariable analysis. J Hear Lung Transplant 20: 212.
-
Hong KN, Iribarne A, Worku B, Takayama H, Gelijns AC, et al. (2011) Who is the high-risk recipient? Predicting mortality after heart transplant using pretransplant donor and recipient risk factors. Ann Thorac Surg 92: 520-527.
-
D'Alessandro C, Golmard JL, Barreda E, Laali M, Makris R, et al. (2011) Predictive risk factors for primary graft failure requiring temporary extra-corporeal membrane oxygenation support after cardiac transplantation in adults. Eur J Cardio-thoracic Surg 40: 962-969.
-
Yamani MH, Lauer MS, Starling RC, Pothier CE, Tuzcu EM, et al. (2004) Impact of donor spontaneous intracranial hemorrhage on outcome after heart transplantation. Am J Transplant 4: 257-261.
-
Lima B, JJ Squiers, G Saracino, T Chamogeorgakis, JC MacHannaford, et al. (2016) Application of the ISHLT Criteria for Primary Graft Dysfunction After Cardiac Transplantation: Risk Factors and Outcomes from a High-Volume Center. J Hear Lung Transplant 35: S167
-
Chou NK, Chi NH, Yu HY, Lin JW, Wang CH, et al. (2013) Extracorporeal rescue for early and late graft failure after cardiac transplantation: short result and long-term followup. Scientific World Journal.
-
Lima EB, Claudio Ribeiro da Cunha, Vitor Salvatore Barzilai, Marcelo Botelho Ulhoa, Maria Regina de Barros, et al. (2015) Experience of ECMO in Primary Graft Dysfunction after Orthotopic Heart Transplantation. Arq Bras Cardiol 105: 285-291.
-
Subramaniam K (2012) Early graft failure after heart transplantation: prevention and treatment. Int Anesthesiol Clin 50: 202-227.
-
Lund L, Edwards LB, Kucheryavaya AY, Benden C, Dipchand AI, et al. (2015) The Registry of the International Society for Heart and Lung Transplantation: Thirty second Official Adult Lung and Heart-Lung Transplantation Report-2015; Focus Theme: Early Graft Failure. J Hear Lung Transplant 34: 1244-1254.
-
Takeda K, Takayama H, Kalesan B, Uriel N, Colombo PC, et al. (2015) Outcome of cardiac transplantation in patients requiring prolonged continuous-flow left ventricular assist device support. J Heart Lung Transplant 34: 89-99.
-
Shahzad K, Aziz QA, Leva JP, Cadeiras M, Ho EK, et al. (2011) New-onset graft dysfunction after heart transplantation incidence and mechanism-related outcomes. J Hear Lung Transplant 30: 194-203.
-
Flechner SM, Kobashigawa J and Klintmalm G (2008) Calcineurin inhibitor-sparing regimens in solid organ transplantation: Focus on improving renal function and nephrotoxicity. Clinical Transplantation 22: 1-15.
-
Thomas HL, Banner NR, Murphy CL, Steenkamp R, Birch R, et al. (2012) Incidence, determinants, and outcome of chronic kidney disease after adult heart transplantation in the United Kingdom. Transplantation 93: 1151-1157.
-
Gude E, Andreassen AK, Arora S, Gullestad L, Grov I, et al. (2010) Acute renal failure early after heart transplantation: Risk factors and clinical consequences. Clin Transplant 24.
-
Ojo A, Held P, Port F, Wolfe R, Leichtman A, Young E, Arndorfer J, et al. (2003) Chronic renal failure after transplantation of a nonrenal organ. N Engl J Med 349: 931-940.
-
Herlitz H, Lindelow B (2000) Renal failure following cardiac transplantation. Nephrol Dial Transplant 3: 311-314.
-
Potena L, Prestinenzi P, Bianchi IG, Masetti M, Romani P, et al. (2012) Cyclosporine lowering with everolimus versus mycophenolate mofetil in heart transplant recipients: Long-term follow-up of the SHIRAKISS randomized, prospective study. J Heart Lung Transplant 31: 565-570.
-
Angermann CE, Störk S, Costard-Jäckle A, Dengler TJ, Siebert U, et al. (2004) Reduction of cyclosporine after introduction of mycophenolate mofetil improves chronic renal dysfunction in heart transplant recipients--the IMPROVED multi-centre study. Eur Heart J 25: 1626-1634.
-
Zuckermann A, Keogh A, Crespo-Leiro MG, Mancini D, Vilchez FG, et al. (2012) Randomized controlled trial of sirolimus conversion in cardiac transplant recipients with renal insufficiency. Am J Transplant 12: 2487-2497.
-
Groetzner J, Kaczmarek I, Schulz U, Stegemann E, Kaiser K, et al. (2009) Mycophenolate and sirolimus as calcineurin inhibitor-free immunosuppression improves renal function better than calcineurin inhibitor-reduction in late cardiac transplant recipients with chronic renal failure. Transplantation 87: 726-733.
-
Meiser B, Reichert B, Adamidis I, Überfuhr P and Kaczmarek I (2005) First experience with de novo calcineurin-inhibitor-free immunosuppression following cardiac transplantation. Am J Transplant 5: 827-831.
-
Yan HL, Zong HT, Cui YS, Li N and Zhang Y (2014) Calcineurin inhibitor avoidance and withdrawal for kidney transplantation: A systematic review and meta-analysis of randomized controlled trials. Transplant Proc 46: 1302-1313.
-
A Osborne, J Patel, M Kittleson, M Rafiei, D Chang, et al. (2013) Kidney dialysis after heart transplantation: The short and long term outcomes. American Journal of Transplantation 13: 454.
-
Lonze BE, Warren DS, Stewart ZA, Dagher NN, Singer AL, et al. (2009) Kidney transplantation in previous heart or lung recipients. Am J Transplant 9: 578-585.
-
van de Beek D, Kremers WK, Del Pozo JL, Daly RC, Edwards BS, et al. (2008) Effect of infectious diseases on outcome after heart transplant. Mayo Clin Proc 83: 304-308.
-
Montoya JG, Giraldo LF, Efron B, Stinson EB, Gamberg P, et al. (2001) Infectious complications among 620 consecutive heart transplant patients at Stanford University Medical Center. Clin Infect Dis 33: 629-640.
-
Fishman JA (2007) Infection in Solid-Organ Transplant Recipients. N Engl J Med 357: 2601-2614.
-
Cimino FM, Snyder KA (2016) Primary care of the solid organ transplant recipient. Am Fam Physician 93: 203-210.
-
Shoham S, Marr Ka (2012) Invasive fungal infections in solid organ transplant recipients. Future Microbiol 7: 639-655.
-
San Juan R, Aguado JM, Lumbreras C, Díaz-Pedroche C, López-Medrano F, et al. (2007) Incidence, clinical characteristics and risk factors of late infection in solid organ transplant recipients: data from the RESITRA study group. Am J Transplant 7: 964-971.
-
George JF, Pamboukian SV, Tallaj JA, Naftel DC, Myers SL, et al. (2010) Balancing rejection and infection with respect to age, race, and gender: Clues acquired from 17 years of cardiac transplantation data. J Hear Lung Transplant 29: 966-972.
-
Smart FW, Naftel DC, Costanzo MR, Levine TB, Pelletier GB, et al. (1996) Risk factors for early, cumulative, and fatal infections after heart transplantation: a multiinstitutional study. J Heart Lung Transplant 15: 329-341.
-
Tallaj JA, Pamboukian SV, George JF, Kirklin JK, Brown RN, et al. (2014) Have risk factors for mortality after heart transplantation changed over time? Insights from 19 years of Cardiac Transplant Research Database study. J Hear Lung Transplant 33: 1304-1311.
-
Chou NK, Ko WJ, Chi NH, Chen YS, Yu HY, et al. (2006) Sparing Immunosuppression in Heart Transplant Recipients With Severe Sepsis. Transplant Proc 38: 2145-2146.
-
Birati EY, Rame JE (2014) Post-heart transplant complications. Critical Care Clinics 30: 629-637.
-
Mendez-Eirin E, Paniagua-Martín MJ, Marzoa-Rivas R, Barge-Caballero E, Grille-Cancela Z, et al. (2012) Cumulative incidence of cytomegalovirus infection and disease after heart transplantation in the last decade: effect of preemptive therapy. Transplant Proc 44: 2660-2662.
-
Rubin RH (2000) Prevention and treatment of cytomegalovirus disease in heart transplant patients. J Hear Lung Transpl 19: 731-735.
-
Hoffman FM (2005) Outcomes and complications after heart transplantation: a review. J Cardiovasc Nurs 20: S31-42.
-
Lin MH, Chou NK, Chi NH, Chen YS, Yu HY, et al. (2012) The outcome of heart transplantation in hepatitis C-positive recipients. in Transplantation Proceedings 44: 890-893.
-
Fong TL, Hou L, Hutchinson IV, Cicciarelli JC and Cho YW (2009) Impact of hepatitis C infection on outcomes after heart transplantation. Transplantation 88: 1137-1141.
-
Uriel N, Jorde UP, Cotarlan V, Colombo PC, Farr M, et al. (2009) Heart Transplantation in Human Immunodeficiency Virus-Positive Patients. J Hear Lung Transplant 28: 667-669.
-
Mehra MR, Canter CE, Hannan MM, Semigran MJ, Uber PA, et al. (2016) The 2016 International Society for Heart Lung Transplantation listing criteria for heart transplantation: A 10-year update. J Hear Lung Transplant 35: 1-23.
-
Costanzo MR, Dipchand A, Starling R, Anderson A, Chan M, et al. (2010) The International Society of Heart and Lung Transplantation Guidelines for the care of heart transplant recipients. J Hear Lung Transplant 29: 914-956.
-
Hummel M (2011) Early postoperative therapy after heart transplantation: Prophylaxis, diagnosis and antibiotic, antimycotic and antiviral therapy of infections. Appl Cardiopulm Pathophysiol 15: 245-255.
-
Kobashigawa J, Ross H, Bara C, Delgado JF, Dengler T, et al. (2013) Everolimus is associated with a reduced incidence of cytomegalovirus infection following de novo cardiac transplantation. Transpl Infect Dis 15: 150-162.
-
Vial T, Descotes J (2003) Immunosuppressive drugs and cancer. in Toxicology 185: 229-240.
-
Ross K (2007) For organ transplant recipients, cancer threatens long-term survival. J Natl Cancer Inst 6: 421-422.
-
Chapman JR, Webster AC and Wong G (2013) Cancer in the transplant recipient. Cold Spring Harb Perspect Med 3.
-
Gottschalk S, Rooney CM and Heslop HE (2005) Post-transplant lymphoproliferative disorders. Annu Rev Med 56: 29-44.
-
Allen U, Preiksaitis J (2009) Epstein-Barr Virus and Posttransplant Lymphoproliferative Disorder in Solid Organ Transplant Recipients. Am J Transplant 9: S87-S96.
-
Dahlke E, Murray CA, Kitchen J and Chan A-W (2014) Systematic review of melanoma incidence and prognosis in solid organ transplant recipients. Transplant Res 3: 10.
-
Caforio AL, Fortina AB, Piaserico S, Alaibac M, Tona F, et al. (2000) Skin cancer in heart transplant recipients: risk factor analysis and relevance of immunosuppressive therapy. Circulation 102: III222-7.
-
Fortina AB, Caforio AL, Piaserico S, Alaibac M, Tona F, et al. (2000) Skin cancer in heart transplant recipients: frequency and risk factor analysis. J Heart Lung Transplant 19: 249-255.
-
Cockfield SM (2001) Identifying the patient at risk for post-transplant lymphoproliferative disorder. Transpl Infect Dis 3: 70-78.
-
Swinnen LJ, Costanzo-Nordin MR, Fisher SG, O'Sullivan EJ, Johnson MR, et al. (1990) Increased incidence of lymphoproliferative disorder after immunosuppression with the monoclonal antibody OKT3 in cardiac-transplant recipients. N Engl J Med 323: 1723-1728.
-
Aull MJ, Buell JF, Trofe J, First MR, Alloway RR, et al. (2004) Experience with 274 cardiac transplant recipients with posttransplant lymphoproliferative disorder : A report from the Israel Penn international transplant tumor registry. Transplantation 78: 1676-1682.
-
Abboud H, MacPhee I AM (2012) Individualized immunosuppression in transplant patients: Potential role of pharmacogenetics. Pharmgenomics Pers Med 5: 63-72.
-
Law BK (2005) Rapamycin: An anti-cancer immunosuppressant? Critical Reviews in Oncology/Hematology 56: 47-60.
-
Hojo M, Morimoto T, Maluccio M, Asano T, Morimoto K, et al. (1999) Cyclosporine induces cancer progression by a cell-autonomous mechanism. Nature 397: 530-534.
-
Gulley ML, Tang W (2010) Using epstein-barr viral load assays to diagnose, monitor, and prevent posttransplant lymphoproliferative disorder. Clinical Microbiology Reviews 23: 350-366.
-
Lietz K, John R, Mancini DM and Edwards NM, (2004) Outcomes in cardiac transplant recipients using allografts from older donors versus mortality on the transplant waiting list: Implications for donor selection criteria. Journal of the American College of Cardiology 43: 1553-1561.
-
Taylor DO, Stehlik J, Edwards LB, Aurora P, Christie JD, et al. (2009) Registry of the International Society for Heart and Lung Transplantation: Twenty-sixth Official Adult Heart Transplant Report-2009. J Hear Lung Transplant 28: 1077-1022.
-
Rickenbacher PR, Pinto FJ, Lewis NP, Hunt SA, Gamberg P, et al. (1995) Correlation of donor characteristics with transplant coronary artery disease as assessed by intracoronary ultrasound and coronary angiography. Am J Cardiol 76: 340-345.
-
Haddad M, Pflugfelder PW, Guiraudon C, Novick RJ, McKenzie FN, et al. (2005) Angiographic, pathologic, and clinical relationships in coronary artery disease in cardiac allografts. Journal of Heart and Lung Transplantation 24: 1218-1225.
-
Fishman JA (2009) Introduction: infection in solid organ transplant recipients. Am J Transplant 9: S3-S6.
-
Snydman DR (2001) Epidemiology of infections after solid-organ transplantation. Clin Infect Dis 33: S5-8.
-
Len O, Garzoni C, Lumbreras C, Molina I, Meije Y, et al. (2014) Recommendations for screening of donor and recipient prior to solid organ transplantation and to minimize transmission of donor-derived infections. Clinical Microbiology and Infection 20: 10-18.





