International Journal of Women's Health and Wellness
Spontaneous Ruptured Heterotopic Fallopian Tube Pregnancy: A Challenging Case
Olga Grechukhina1, Diana P English1*, Wei Hong2, Ravi Kaza1 and Elena Ratner1
1Department of Obstetrics, Gynecology & Reproductive Sciences, Yale University School of Medicine, USA
2Department of Pathology, Yale University School of Medicine, USA
*Corresponding author:
Diana P. English, Department of Obstetrics, Gynecology & Reproductive Sciences, Yale University School of Medicine, New Haven, Connecticut, USA, Tel: 203-785-7385, Fax: 203-737-4377, E-mail: Diana.english@yale.edu
Int J Womens Health Wellness, IJWHW-1-001, (Volume 1, Issue 1), Case Report; ISSN: 2474-1353
Received: July 23, 2015 | Accepted: August 07, 2015 | Published: August 09, 2015
Citation: Grechukhina O, English DP, Hong W, Kaza R, Ratner E (2015) Spontaneous Ruptured Heterotopic Fallopian Tube Pregnancy: A Challenging Case. Int J Womens Health Wellness 1:001. 10.23937/2474-1353/1510001
Copyright: © 2015 Grechukhina O, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Bilateral ectopic pregnancy is a rare entity encountered in 1 out of 750-1,580 of all ectopic pregnancies. Here we present a case report of a ruptured spontaneous bilateral tubal pregnancy.
Case report: This is a case of a 39 year old gravida 4 para 2-0-1-2 patient who presented to the emergency room with 1 week history of worsening left sided abdominal pain associated with vaginal bleeding. She had a positive pregnancy test and transvaginal ultrasound demonstrated an 11 x 9 x 7 cm retro-uterine mass concerning for hemorrhagic debris but no adnexa were identified. Surgery was complicated by conversion from laparoscopy to low transverse laparotomy due to hemorrhage and severe adhesive disease. Both tubes were dilated with evidence of ectopic pregnancy. A bilateral salpingostomy was performed and the pathology was consistent with products of conception in both fallopian tubes.
Discussion: Bilateral ectopic pregnancy is rarely anticipated preoperatively especially in the absence of assisted reproductive techniques and the diagnosis is usually made intra-operatively. Every patient with a suspected ectopic pregnancy should be evaluated for possible bilateral ectopic pregnancy with a thorough history, diagnostic modalities, counselling and careful surgical exploration and decision making in case of surgical management.
Introduction
Extra-uterine implantation occurs in approximately 1%-2% of all pregnancies and is still associated with severe maternal morbidity and mortality [1]. Bilateral ectopic pregnancy is a very rare entity that is hardly ever anticipated when the diagnosis of ectopic pregnancy is suspected. When bilateral tubal gestation occurs, the management of such patients is complicated as it is rarely diagnosed preoperatively. The diagnosis can even be missed intra-operatively and medical management is poorly studied. Surgical management may be challenging even in cases of prompt diagnosis.
We present a case of a spontaneous bilateral ruptured ectopic pregnancy diagnosed intra-operatively and managed with adhesiolysis and bilateral salpingostomy for fertility preservation.
Case Report
A 39 year old gravida 4 para 2-0-1-2 patient presented to the emergency room (ER) with a 1 week history of left lower quadrant pain worsening over time. Her last menstrual period was 30 days prior to presentation. The left lower quadrant pain did not respond to over the counter pain medications and was associated with low volume vaginal bleeding. She also reported nausea without vomiting and a new onset urinary retention which began a few hours prior to presentation. She denied fevers, anemic symptoms or other urinary symptoms. Her medical history included polysubstance abuse (cocaine, benzodiazepines, prescription drugs and heroin) and she was currently on methadone. She also has a history of chronic hepatitis C, diverticulitis, depression and obesity (BMI 30kg/m2).She had no known allergies and her medications included Methadone 125 mg daily, Miralax and Motrin as needed.
Surgical history included two cesarean sections and patellar surgery. Gynecologic history was notable for abnormal Pap smears with high grade squamous intraepithelial lesion in 2010 and 2013. She reported being in a monogamous relationship with a male partner for the last year and was not using any form of birth control. She had usually regular periods until a recent miscarriage that did not require intervention about 3 months prior and her periods had not been regular since then yet. Her coitarche was at age 15 and she had 20 lifetime male partners to date. She denied a history of sexually transmitted diseases except for HPV. Her social history is notable for former cigarette smoking (quit 2 years ago) and polysubstance abuse as outlined above as well as incarceration related to drug use. Evaluation in the ER revealed a positive urine pregnancy test and the trans-abdominal ultrasound findings were concerning for blood collection in pelvis and the gynecologic team was consulted.
On examination she was noted to have blood pressure 111/46 mmHg, heart rate 76 bpm, respiratory rate 24 bpm, temperature 36.6℃, O2 saturation of 100%. She appeared extremely uncomfortable. Pertinent physical exam findings included normoactive bowel sounds throughout the abdomen, tenderness to palpation in the left lower quadrant without guarding or rebound. Speculum exam revealed closed cervix and small amount of dark red blood in the vaginal vault without active bleeding. Digital exam revealed fullness along posterior vaginal wall and elicited extreme tenderness in the posterior cul de sac. Her uterine fundus and adnexa were not readily palpated.
Pertinent laboratory findings included white blood cell count of 8.3 x 1000/uL, hemoglobin 10.4g/dL, hematocrit 29% (stable from 3 months prior), normal complete metabolic panel with normal lipase/amylase, urinalysis with small blood and specific gravity of 1.026. Serum human chorionic gonadotropin (HCG) was 1,270 mIU/mL. She had normal coagulation tests and her blood type was B positive.
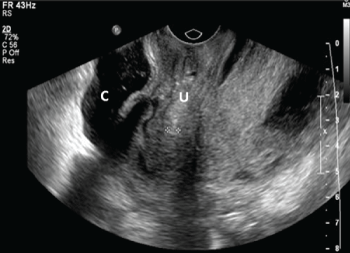
Transvaginal ultrasound was performed and revealed normal appearing uterus without masses or intrauterine pregnancy and a large heterogenous collection (11 x 9 x 7 cm) consistent with hemorrhagic debris posterior to the uterus. Within this collection a tubular structure was noted which could represent a dilated (~2cm) fallopian tube (Figure 1 and Figure 2). Neither adnexa could be identified. Given the high suspicion for ruptured ectopic pregnancy, a laparoscopy with possible laparotomy was recommended. The patient expressed that this was a desired pregnancy and wanted to keep this pregnancy if it was located in the uterus. She also stated her distinct wish to preserve her fertility if at all possible. She signed the consent form for diagnostic laparoscopy, possible right or left salpingostomy or salpingectomy and possible right or left oophorectomy after receiving the appropriate counseling regarding the risks versus benefits of the planned surgical procedure. She was then taken to the operating room where laparoscopy was initiated. Upon entry into the abdominal cavity, severe adhesive disease was noted with the omentum densely attached to the anterior abdominal wall in multiple sites and this obscured visualization of the pelvis. After some adhesiolysis, the pelvis was reached and there was significant blood in the pelvis with heavy bright red bleeding coming from what appeared to be left tube after gentle manipulation. Significant adhesive disease was also evident in the pelvis after suctioning. The procedure was as such converted to laparotomy via pfannenstiel incision. Upon entry into the abdominal cavity additional clots were evacuated instantaneously. The bleeding was noted to persist and identification of the source was extremely difficult as the pelvic structures were edematous and densely adherent, suggestive of a history of untreated pelvic inflammatory disease or possibly diverticulitis. After extensive dissection, the uterus and right fallopian tube were identified. The right fallopian tube appeared dilated in the ampulla region with an approximately 1 cm opening at the most dilated area with surrounding clot, suspicious for the location of rupture. The left fallopian tube was also identified and was noted to be even more dilated than the right tube. A right salpingostomy was then performed and brownish tubal contents were submitted to frozen section pathologic examination. However given the appearance of the left fallopian tube, a left salpingostomy was done and revealed dark red contents of larger diameter consistent with tubal pregnancy. The left tubal contents were submitted to permanent pathology (Figure 3). Both salpingostomy sites were found hemostatic. Intraoperative frozen section of the right tube contents revealed products of conception.
.
Figure 1: Transvaginal ultrasound sagittal image showing retro-uterine mass concerning for hemorrhagic debris and within this collection a tubular structure was noted which was thought to represent a dilated (~2cm) fallopian tube. (U) represents uterus and (C) is the retro-uterine collection with dilated fallopian tube.
View Figure 1
.
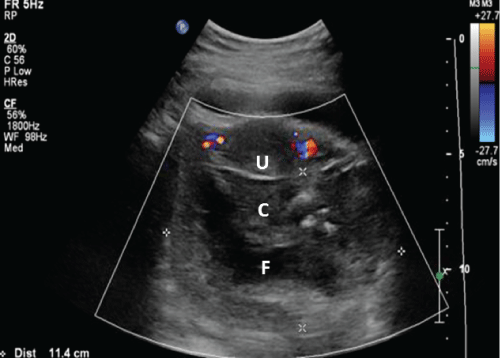
Figure 2: Transverse transvaginal ultrasound image showing (U) uterus, (C) represents collection posterior to uterus and (F) is the structure consistent with dilated fallopian tube.
View Figure 2
.
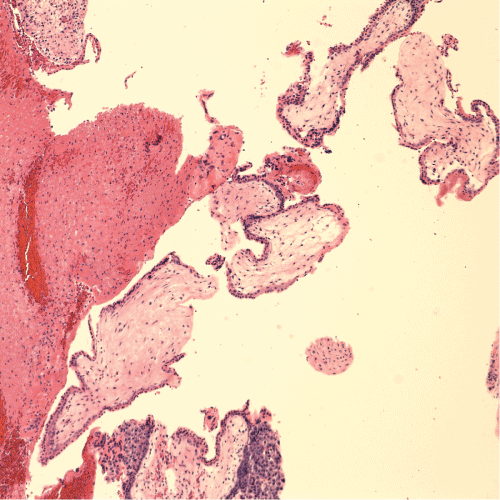
Figure 3: Microscopic appearance x100 view of left tubal contents showing chorionic villi admixed with fibrin.
View Figure 3
The decision was made not to perform bilateral salpingectomy given the patient's strong desire for future fertility. Total estimated blood loss was 900mls (300mls of which was in the form of clots) and the patient received 1 unit of packed red blood cells intra-operatively. Her postoperative course was complicated by pain control issues and spontaneous desaturation likely in the setting of atelectasis. She was eventually discharged home on postoperative day 3 after receiving Depo-Provera for contraception. Pathologic examination of left tubal contents also showed products of conception in keeping with a spontaneous bilateral fallopian tube ectopic pregnancy. Over the next month her beta HCG level trended down to <1mIU/mL.
Discussion
This case demonstrates an unusual finding of ruptured bilateral ectopic pregnancy. Twin ectopic pregnancy is a rare diagnosis that can present as twin tubal (in one tube), bilateral tubal (in both tubes) or heterotopic (in one tube and in the uterus) pregnancy [1]. The incidence of bilateral ectopic pregnancy is estimated to be 1:750-1:1580 of all ectopic pregnancies and 1 in 200,000 of all pregnancies [2,3]. Interestingly, the incidence of bilateral tubal pregnancy in native African population is estimated to be 1 in 51 ectopic pregnancies which is considered to be due to higher rate of twinning and untreated pelvic inflammatory disease (PID) [1]. The first report of bilateral ectopic pregnancy was published by McDonald et al. [4]. Subsequently, more than 200 cases were described in literature. In the period between 1997 to 2007, there were 42 cases reported [5]. Upon performing a PubMed search we came across another 23 case reports of bilateral ectopic pregnancies published since 2007, most of which were in the setting of artificial reproductive technologies (ART) due to multiple ovulation or multiple embryo transfer. The true incidence of bilateral ectopic pregnancy remains unknown due to both failures to make the diagnosis as well as under-reporting.
Classification of this entity distinguishes primary bilateral ectopic pregnancy (spontaneous) from secondary (in the setting of ART) due to different pathogenetic mechanisms [5]. In our case, this spontaneous (primary) bilateral ectopic pregnancy occurred likely in the setting of PID and severe pelvic adhesive disease. Although the patient did not report a history of PID, this is suspected given her history of HPV related disease, polysubstance abuse, multiple sexual partners and the severe adhesive disease encountered intraoperatively. Diverticulitis in the past and possibly the two prior cesarean sections may have also contributed to the development of pelvic scarring
Bilateral ectopic pregnancy is difficult to diagnose in the preoperative setting. This diagnosis however needs to be considered at all times when managing a suspected ectopic pregnancy as failure to make the diagnosis can lead to catastrophic consequences. In the vast majority of bilateral ectopic cases, the diagnosis is made intra-operatively with direct visualization of bilaterally dilated or ruptured fallopian tubes [6]. Thus the importance of visual inspection of both tubes during every surgery for suspected ectopic pregnancy can hardly be overstated.
As mentioned above, the incidence of bilateral ectopic pregnancies is very low, however it may still be good practice to address this possibility with the patient preoperatively in order to establish an appropriate management plan in case this is discovered during surgical exploration [6].
Our patient was counselled regarding possible need for unilateral salpingectomy, however during the surgery the team encountered the dilemma of bilateral salpingectomy versus bilateral salpingostomy. Bilateral salpingectomy would definitively compromise her ability to get pregnant in future without ART whereas bilateral salpingostomy put her at high risk of ectopic pregnancy recurrence with future pregnancy. The risk of ectopic pregnancy after unilateral salpingostomy is calculated as 12-44%. There are no data available on this risk after bilateral salpingostomies [7]. In our case, the patient desired future fertility (although she was 39 and had two children) as she was currently in a new relationship.
Upon careful review of this patient's history it was noted that the patient was seen in an ER 3 months prior to the current presentation. At that time she was complaining of severe generalized abdominal pain and had tenderness to palpation in epigastric and suprapubic areas. She then had a normal right upper quadrant ultrasound except for small amount of ascites of unclear etiology. She was discharged home with a diagnosis of gastritis. The patient reported that severe abdominal pain persisted for several days and was associated with small volume vaginal bleeding. A couple of days after her ER visit she had a positive home urine pregnancy test. She did not pursue obstetrical care then as her bleeding and pain stopped over the course of a week and the patient presumed that she had miscarried.
Given this history, there is a possibility of 2 pregnancies originating from ovulations during separate menstrual cycles. This sequence of events would explain different sizes of dilated tubes (left tube bigger than right) and the differing appearance of the tubes. The right tube may have contained an old resolving ectopic pregnancy with a small opening on the tube reflecting the point of rupture. The inflammatory changes in the pelvis may have been chronic and reactive to the ruptured ectopic pregnancy. If this is the case, the patient may have had a ruptured right sided tubal ectopic pregnancy that was missed, but, fortunately, did not result in a serious adverse event. Unfortunately, there is no reliable way to confirm or disprove this possibility. This consideration also would not have changed the management of the patient at the time of the current presentation.
However, it is worth mentioning that although every patient of reproductive age presenting with abdominal pain or vaginal bleeding should have a urine pregnancy test, there continues to be in some cases a delay in diagnosis of ectopic pregnancy or a misdiagnosis altogether when a pregnancy test is not performed.
In conclusion, this is a rare case of primary bilateral ectopic pregnancy diagnosed intra-operatively and treated with bilateral salpingostomy. This case raises multiple potential areas of discussion. Mainly, there needs to remain a high index of suspicion for ectopic pregnancy in women of reproductive age presenting with abdominal pain and vaginal bleeding. The standard of complete evaluation of the operative field at the time of surgical evaluation should never be compromised especially as the incidence of bilateral ectopic pregnancy may increase with the current trend of increased used of ART. In cases where ectopic pregnancy is suspected, thorough preoperative evaluation followed by appropriate counseling is paramount in all cases to ensure timely and suitable management depending on the patient's desire for future fertility.
References
-
Makinde OO, Ogunniyi SO (1990) Bilateral tubal and twin pregnancies in Ile-Ife, Nigeria. Int J Gynaecol Obstet 33: 365-367.
-
Farquhar CM (2005) Ectopic pregnancy. Lancet 366: 583-591.
-
Stewart HL, Jr (1950) Bilateral ectopic pregnancy. West J Surg Obstet Gynecol 58: 648-656.
-
McDonald E, Krieger WA (1913) BIlateral and multiple ectopic pregnancy. JAMA 60: 1766-1769
-
De Los Rios JF, Castaneda JD, Miryam A (2007) Bilateral ectopic pregnancy. J Minim Invasive Gynecol 14: 419-427.
-
Ryan MT, Saldana B (2000) Bilateral tubal ectopic pregnancy: a tale of caution. Acad Emerg Med 7: 1160-1163.
-
DeCherney AH, Maheaux R, Naftolin F (1982) Salpingostomy for ectopic pregnancy in the sole patent oviduct: reproductive outcome. Fertil Steril 37: 619-622.





