International Journal of Women's Health and Wellness
A Mixed-Methods Evaluation of Potential Distribution Channels for the V Condom in South Africa
Jenni Smit1, Nzwakie Mosery1, Lavanya Pillay1, Mags Beksinska1, Letitia Rambally-Greener1, Cecilia Milford1, Maggie Kilbourne-Brook2 and Patricia S. Coffey2*
1Department of Obstetrics and Gynecology, University of the Witwatersrand, South Africa
2PATH, Seattle, Washington, USA
*Corresponding author:
Patricia S. Coffey, PhD, MPH, Director, Health Technologies for Women and Children, Devices and Tools Global Program, PATH, Seattle, WA 98119, USA, Tel: 206-285-3500, E-mail: pcoffey@path.org
Int J Womens Health Wellness, IJWHW-1-007, (Volume 1, Issue 1), Original Article; ISSN: 2474-1353
Received: November 25, 2015 | Accepted: December 19, 2015 | Published: December 22, 2015
Citation: Smit J, Mosery N, Pillay L, Beksinska M, Rambally-Greener L, et al. (2015) A Mixed-Methods Evaluation of Potential Distribution Channels for the V Condom in South Africa 1:007. 10.23937/2474-1353/1510007
Copyright: © 2015 Smit J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Market tests in Durban, South Africa, assessed the feasibility of commercial and non-traditional public-sector distribution channels for the V Condom, a new female condom.
Methods: Between August 2014 and July 2015, data were collected from 119 women and 78 men who were potential and actual V Condom users (male and female students, male factory workers, and female and male sex workers) to assess uptake and acceptability across multiple distribution channels (a tertiary health service centre, a factory, and two nongovernmental organizations). This prospective evaluation included initial awareness-raising and distribution of currently available and V condoms to those interested. Baseline data collection included a quantitative survey and two focus group discussions. After one-month follow-up, V Condom use data were collected through self-completed condom logs and SMS text messages, four focus group discussions and three inventories, and in-depth interviews with three site coordinators.
Results: The quantitative results indicated high V Condom usage during the study period. Most sex acts were protected, with participants using more V Condoms than male condoms or other female condoms. Many participants reported preferring the V Condom over male and other female condoms. Ideal distribution channels included tertiary institutions, factories, government facilities, pharmacies, shops/supermarkets, schools, entertainment places, and tuck shops. Factors influencing preferred distribution channels were ease of access, convenience, operating hours, users' previous experiences, and peer influences. Most participants were willing to pay for the V Condom due to the perception that paying ensured a quality product and that free products are not as trustworthy.
Conclusions: There is a non-public-sector market for V Condoms in Durban, and some women and men are willing to pay for the V Condom at a price approaching the estimated market price. This novel mixed-methods approach to understanding consumer interest in a new female condom provided data relevant for both programmatic planning and future market introduction.
Keywords
Female condoms, Evaluation, Distribution, Channel, Mixed methods, South Africa
Abbreviations
C&G NGO: Nongovernmental organization providing counselling and growth programs; FC: Female condom; FGD: Focus group discussion; FSW: Female sex worker; IDI: In-depth interview; MC: Male condom; NGO: Nongovernmental organization; SRH NGO: Sexual and reproductive health nongovernmental organization; STI: Sexually transmitted infection.
Introduction
Increasing access to underutilized family planning methods is of global concern. The United Nations Commission on Life-Saving Commodities identified the female condom (FC) as one of 13 essential and overlooked commodities [1]. Male and female condoms are currently the only effective method of dual protection against unintended pregnancy and the transmission of sexually transmitted infections (STIs) including human immunodeficiency virus (HIV) [2-8]. A new design of female condom with special features to make it easy to use and acceptable to both women and men, the V Condom, has been evaluated in clinical studies in South Africa, China, and the United States and has achieved regulatory approvals in Europe (CE mark), China (Shanghai Food and Drug Administration), and South Africa. As the V Condom has been approved by the South African Bureau of Standards, a consumer interest assessment was conducted to (1) identify non-public-sector markets for the V Condom with the greatest opportunity of uptake and impact; (2) identify potential user groups; (3) identify distribution channels to effectively reach these users; (4) gather consumer feedback on the product, packaging, promotion, and price; and (5) better understand women's and men's attitudes toward the V Condom. Findings from this consumer interest assessment will be used to inform future programmatic planning and market development of the V Condom in South Africa.
Methods
Between August 2014 and July 2015, data were collected from women and men who were potential and actual V Condom users. The research team identified a range of organizations that were not in the public sector that were currently distributing male and female condoms and targeting diverse populations with differing socioeconomic status to gather a variety of opinions. Participants were sampled from four established sites that distributed male and female condoms (one private factory, one nongovernmental organization [NGO] providing counselling and growth programs [hereafter referred to as C&G NGO], one NGO providing sexual and reproductive health services [hereafter referred to as SRH NGO], and one tertiary education institution). All participants (male and female students, male factory workers, and female and male sex workers) were 18 years and older and currently sexually active. Table 1 describes each component of the study.
![]()
Table 1: Summary of participants according to study component and data collection tools.
View Table 1
After conducting a baseline survey on condom use, we tracked participant feedback on their male or female condom (FC2 and Cupid female condoms available in South Africa) and V Condom use over a one-month period using self-administered condom logs and SMS text messages. Participants were simply asked to send a text message each time they had sex. Data from the condom use logs were collected by the research team at the end of the one-month period. Additional V Condoms were available over the one-month period at each of the distribution sites, and participants could redeem up to ten V Condoms at a time using a resupply voucher given to them at baseline. Promotional focus group discussions (FGDs) were conducted with interested women who attended health awareness day demonstrations. Once the prospective evaluation components were completed (baseline surveys and condom logs), post-use evaluation FGDs and a user exit questionnaire were administered to a subset of users of the V Condom and in-depth interviews (IDIs) were conducted with site coordinators to explore the impact and demand of the V Condom promotion.
Condom use data were reported on the condom log and via cell phone text messages. Acceptability and preference data were obtained during both the enrolment baseline interview and during the discussions in the promotional and evaluation FGDs. Demographic data were captured during baseline interviews and FGDs. Site coordinator data were captured during IDIs.
Recruitment and screening
During the promotional events and condom demonstrations, individuals who showed interest in the V Condom were recruited and screened for eligibility. Participants were required to meet the following selection criteria for participation in each of the study components:
Study component 1:Prospective evaluation of condom use
• 18 years or older
• Own a cellular telephone
• Literate (able to read a newspaper or letter easily)
• Sexually active (defined as having at least two vaginal coital acts per week and not being abstinent in the month prior to enrolment)
• Willing to give written informed consent
• Willing to complete the condom use logs
• Willing to use the study product (V Condom) as directed
• Willing to adhere to the follow-up schedule and all study procedures
• Willing to provide research study staff with their phone number or other locator information while participating in the study
• Willing to participate in the study for the duration of approximately one month
Study component 2:Focus group discussions (FGDs) with potential female users of V Condom (promotional FGDs)
• Female
• 18 years or older
• Literate (able to read a newspaper or letter easily)
• Willing to give written informed consent
Study component 3:Focus group discussions with participants (male and female) from the prospective evaluation of condom use (evaluation FGDs)
• In addition to study component 2 criteria
• Participated and completed the prospective evaluation of condom use
• Used at least one V Condom
Study component 4:
In-depth interviews with site coordinators
• Coordinator or manager of one of the potential distribution sites
• 18 years or older
• Willing to give written informed consent
Data entry and analysis
Data from the quantitative data collection forms were entered into Epidata Version 3.1. After the dataset was cleaned and validated, the database was exported to STATA 13 IC (College Station, Texas, USA) for descriptive analysis. The FGDs and IDIs were content-coded for user preference using a relational analysis approach and analyzed using an iteratively developed codebook to explore emergent themes within the data and directional preference. Themes and sub-themes emerged through a systematic review of the data employing both inductive and deductive procedures for developing themes and organizing data within these themes through coding. During the coding process the data were continuously reviewed as new themes emerged.
Ethics review and approvals
All documents related to this consumer interest assessment were reviewed and approved by the Human Research Ethics Committee of the University of Witwatersrand, Johannesburg, South Africa, prior to study initiation and enrolment of participants (HREC approval #M140554). All participating organizations gave approval for the research conducted at their sites. The consent process and all checklists, condom use logs, and surveys used in the study were written and conducted in a language understandable to the participants. All relevant documents were translated into isiZulu. Written informed consent was obtained from all study participants prior to enrolment in all of the study components.
Study product
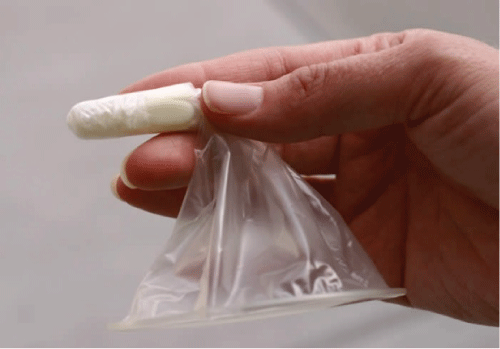
The V Condom is made of polyurethane and is inserted using an insertion capsule. The 227 mm-long condom sheath is tucked into the insertion capsule, which dissolves after insertion (Figure 1), releasing the condom within the vagina. The dissolving capsule is made of polyvinyl alcohol, the same material used to make contraceptive C-film. V Condoms are not pre-lubricated and a sachet of water-based lubricant is supplied with each condom.
The V Condom is provided in foil laminate pouches. The packaging displays the manufacturer's name, lot/batch number, and date of expiry (Figure 2). Each condom is presented within an outer packet (cardboard sleeve) that also encloses the lubricant sachet and the instructions (Figure 3).

.
Figure 3: Outer package opened showing instructions, lubrication, and the V Condom.
View Figure 3
Results
A total of 197 eligible participants from the four distribution sites were enrolled and participated in the assessment. The socio-demographic characteristics of the participants across all study components are shown in Table 2. Table 3 provides a summary of the sexual behaviour and practices of the sample. A total of 41 potential and actual product users participated in the qualitative assessments (18 in the promotional FGDs and 23 in the evaluation FGDs). Three IDIs were conducted with program coordinators/site managers at three of the four potential distribution sites after the V Condom promotion and evaluation activities were completed.
![]()
Table 2: Overall sample socio-demographic characteristics.
View Table 2
![]()
Table 3: Overall sample sexual and reproductive health status.
View Table 3
V Condom usage during the one-month study period
As part of the prospective evaluation, participants were given 10 V Condoms and asked to send a text message post coitus to indicate the number of male condoms (MCs) or FCs or V Condoms or no protection used (over the one-month study period). A total of 104 participants (tertiary students, female sex workers (FSW), and male sex workers (MSW) at the C&G NGO and factory employees sent at least one text message after sex. Males from the SRH NGO did not send text messages. The response rates are listed in Table 4.
![]()
Table 4: SMS response rates.
View Table 4
Protected and unprotected sex
In the prospective study, 620 sex acts were reported by 104 of the 197 participants. Protection with a V Condom or another product (male or another female condom) was used for 95.3% of the sex acts, with the remaining 4.7% being unprotected. Overall, participants reported using more V Condoms (61.6%) compared to male condoms (31.1%) or another female condom (2.6%).
V Condoms distributed by each site
The inventory of the V Condoms distributed by site is presented in Table 5. The total number of condoms received included: (1) condoms taken at the promotional demonstration table (2) condoms distributed to participants at the baseline interview (3) condoms distributed to participants at the promotional FGD and (4) condoms left at the site for participant resupply.
![]()
Table 5: Inventory of V Condoms supplied to and distributed by site.
View Table 5
Product packaging and user preference
During the FGDs and IDIs, participants and coordinators spoke at length about their impressions of the V Condom packaging; overall, most described the packaging as "nice/good", "unique", "attractive", "trendy", "classy" and "stylish". Almost all of the participants felt the design and colour were eye-catching.
"Its cover, it's like the cover of the CD, no one will notice what you carrying." (FGD1, female student)
"It is stylish; it is not obvious that you are carrying a condom. Even if you have it on your hand; no one will notice. It is well packaged." (FGD2, FSW)
However, all female students, some FSW, and all males felt that the product packaging was too large to fit into a toiletry bag or one's pocket. They expressed concern that this may hinder people who were embarrassed to be seen with condoms from using the V Condom or be difficult to conceal in public. Participants did not want the size of the V Condom to decrease despite concerns about the package size.
"Another thing that I will suggest is that the package is big, its package if maybe they can try and make a simply package you see, something that you can put on your pocket like when you wearing a jean, something you go somewhere and don't carry a bag you see, but if it a small package then you can put it on your pocket so it would be easy." (FGD5, FSW)
All who participated in qualitative data collection had experience using male condoms, and the majority who had used female condoms (prior to exposure to V Condoms) reported that they preferred male condoms to female condoms. This preference seemed to be largely due to a lack of alternative female condoms in the market. Most participants reported that they preferred the V Condoms over female condoms currently in the market. The participants who did not express a preference did so because they had never heard of, seen, or used a female condom before the promotional event. A few female students and FSWs from the promotional FGD stated that they had no idea female condoms were even available in South Africa. All participants felt that the V Condom could be used for every sex act-not just occasionally-and would recommend the V Condom to friends.
"The V Woman's Condom is for any day. Winter, summer, or autumn you don't have stress, yes." (FGD5, FSW)
"I think about the condom he would be happy and he would be more attractive, he likes things that are nicer and he likes to be safe." (FGD1, female student)
"Aaah, I think, I think he would be excited because there is like a lube and everything so, he probably like put more pressure on foreplay...I think he would actually enjoy it." (FGD1, female student)
"When I came home I just throw it on the bed when I reached him home and he asked me 'what is this beautiful thing?'" (FGD5, FSW)
Potential distribution channels
Participants in the prospective follow-up component of the study favoured obtaining the V Condom from their study location (distribution sites) the tertiary institution, C&G NGO, and factory. Government clinics/hospitals/health centres as distribution channels were also favoured across the sites. Approximately 40% of participants indicated the pharmacy as a suitable distribution site.
The shop/supermarket was considered a suitable distribution site by all participants except female factory employees. NGOs as possible distribution sites for obtaining V Condoms were mentioned by students, FSWs, males, MSWs at the C&G NGO, and male factory employees.
During FGDs, FSWs reported traditionally accessing condoms from clinics. However, they felt that this was a cumbersome and time consuming means of accessing condoms and would prefer to access the V Condom through NGOs or through medical mobile vans that come directly to their communities. Female students also felt that accessing FCs or even the V Condom at a clinic would be uncomfortable and embarrassing. However males (in both FGDs) were comfortable accessing V Condoms from hospitals and clinics and even suggested male clinics. FSWs and male students suggested taverns, bars, hotels, clubs, and similar public spaces where people might meet and engage in sexual activity. However, they cautioned that it should not be exclusively sold in these places and could even be sold in rural areas from small locally owned shops so that everyone can buy them.
The majority of FGD participants recommended advertising on social networks, providing examples such as Twitter, Facebook, and even instant messaging services (such as BlackBerry messaging or WhatsApp). Traditional media were also mentioned; billboards were highly ranked, then television advertisements, posters, and pamphlets and the lowest ranked were magazines, radio, and newspaper/print. Word of mouth was mentioned by all participants as they said it would be easy to talk about the V Condom to sexual partners, friends, and family. Participants suggested placing posters and pamphlets at taxi ranks, taverns, bars, hotels, clubs, and similar public spaces. FSWs did not think radio or television would work as they rarely listen to these and were not sure which stations or community papers would be best for advertising the V Condom. Conversely, the NGO-based IDI participants felt that television and billboards would be the most effective means of advertising the V Condom as well as in community spaces such as bars and taverns. A factory-based IDI participant felt that radio messaging would be more successful among rural populations, because those who cannot read or do not have access to community newspapers definitely listen to the radio.
"Cause when you look at it you can see that they can start by liking it, then following it after that, then they can be V Woman's Condom followers, even on WhatsApp when you put the V Condom picture maybe make it my profile picture then my friend is going to ask me "what is on your profile picture?" then I would tell her it a condom and it like this and this and this, then she will ask me more than that way that when everyone will know about it." (FGD5, FSW)
"You buy a condom in a supermarket and there is only education on the back. So I think maybe that is the question that we could raise and ask if you have feedback or maybe provide a contact number, a contact number on the package and say; if you have any questions, you can contact or call this call centre. I think that would be where specifically where places do not have clinic sister. So I think feedback from a centre would be good." (IDI2, female)
Willingness to pay
The majority of the potential V Condom users who participated in the baseline interview at each distribution site were willing to pay for the V Condom. Information garnered from V Condom users via the user exit questionnaire during the evaluation FGD showed that all V Condom users from the student population and male factory employees reported willingness to purchase the V Condom (100%). Many FSWs (85.7%) were willing to purchase the V Condom.
All participants involved in qualitative data collection were willing to pay for the V Condom even though they do not usually buy male condoms or even female condoms. Many felt that they would buy the V Condom over female condoms currently available for sale.
"They would buy this condom, the way it is designed, even the package is flashy." (FGD2, FSW)
Price willing to pay
V Condom user feedback at the exit survey indicates that the average amount willing to pay ranged between ZAR7.90 and ZAR11.30 (US$0.57-US$1.06) at time of publication.
Some male students in the evaluation FGD wondered if it would be cheaper to buy the lubricant separately as they often do buy lubricants as well as male condoms. Males in both evaluation FGDs felt it would be best to distribute the V Condom for free because the price will increase over time and one day will not be affordable. Interestingly, FSWs in the evaluation FGD were willing to pay more for the V Condom after using them over the course of the month. All participants felt that more than ZAR30.00 per V Condom would be too much and would prefer to buy a pack of three V Condoms rather than singles. Many felt that younger users (teenagers or people in their early 20s) would not be able to afford the V Condom if it was too expensive. Many explained that the motivation to pay for the V Condom was based on the idea that if you pay you will receive a quality product, and free products are not as safe or trusted as products you pay for.
"P1: And some people have this tendency that something for free is not quality.
P6: It is not okay.
P5: Price goes with quality, you see. So if you bought something then that thing is quality, which means that the Choice ones are fake or the ones you get for free are fake you see something like that, yah." (FGD4, male students)
"We have to buy condoms because they protect us from many different situations. Having STIs, pregnancy...perhaps I will have an infection in my private part, perhaps there would be some sort of discharge or get to bleed for the rest of my life if I had unprotected sex with that man. So I think it is okay to buy the condoms. There is one thing that I want to know my fellow sisters; why do we always want to have everything for free whilst we are the ones who are being protected?" (FGD2, FSW)
Discussion
Assessing appropriate distribution channels for introduction of a new product is complex and must be carefully planned using market data [9,10]. Our study used a novel mixed-methods approach to test various distribution channels for the introduction of a new female condom product in the South African market. We believe that the mixed methods used were able to capture relevant data about the elusive nature of future market behaviour.
These study results will allow us to apply the total market approach to increase access to the female condom market [11]. Previous analyses of the total market approach for male condoms in sub-Saharan Africa as well as Myanmar have shown the need to grow all market sectors to create sustainable product access [12]. Likewise, these study data will inform market strategies for the V Condom that shape private-sector/NGO reach. Greater private-sector participation in the female condom market could also provide greater contraceptive security [13].
The relatively high condom use shown during the study period was consistent with other reports from users regarding their preference for this female condom design [14,15]. This was not surprising because a user-centered process involving couples from four countries-including South Africa-was employed to design the V Condom. This user input resulted in special features that make the V Condom easy to use and acceptable to both women and men. The V Condom design was verified through user testing among 60 couples in three countries in 2004 [16]. More than 90% of couples in the design validation study, nearly half of whom had no previous experience with female condoms, were satisfied with the performance of the V Condom in regard to ease of use, stability, comfort, and sensation.
Packaging for the V Condom was also based on user input, and the appeal of the colour and design of the package reflects this. The appeal of the packaging across the wide range of market test participants confirms the design aesthetic as being attractive as well as unobtrusive. The relatively large size of the package in comparison to a male condom has been noted previously by other user groups [17]. Unfortunately, the V Condom design does not allow it to be folded for smaller packaging dimensions.
Participant preference for the V Condom was likely the result of a combination of liking both the product and packaging as an integrated unit that offers a good user experience. The attractiveness of the packaging was well-noted by study participants and should play an important role in demand generation going forward.
The market tests were successful in identifying suitable distribution channels for the V Condom. Although the majority of the sample identified government facilities as being an acceptable delivery channel, it is notable that female students were not comfortable with this approach. For students, accessing the condom through distribution sites on campus may be the most appropriate. Men and FSWs opted for accessing V Condoms at public places such as bars, hotels, and clubs [18]. Broadening the distribution channels to include access at public sites has been shown to increase demand among adolescents and young people [19,20].
Willingness to pay among potential users and an affordable price are key to growing the market for this product. The market strategies tested in this evaluation provide options for pricing (i.e., subsidized versus full commercial price). These potential distribution channels align well to the concept of a total market approach and the desire for equity across socioeconomic sectors. Next steps to increasing access to the V Condom in the southern Africa region include aligning product supply and demand volumes, designing and executing a market entry plan that utilizes the most promising distribution channels, and conducting targeted demand-generation efforts.
This study was limited in that the market tests were done in organizations that usually distribute condoms free of charge. Even so, study participants mentioned they would like the V Condom to be available for purchase in bars and other retail outlets. Additionally, data collection at the SRH NGO site was attempted for the evaluation FGD and the site coordinator IDI, but it was not possible because there were too few participants who only participated in the baseline interview and did not send SMS texts during the one-month study period. No V Condoms were distributed to these participants by the site coordinator. Follow-up at all sites was limited to one month with participants having ready access to free condoms. These findings may not necessarily be replicable over a longer-term and/or when condoms are available at a cost. It is likely that these short-term results could be generalizable to other large urban locations in southern and/or sub-Saharan Africa. Also, only 53% of participants (104 of 197 participants) reported their condom use behaviour after sex, suggesting that the remaining 93 participants may not have used condoms at all. Further research to understand this important target segment is warranted.
Conclusions
The quantitative results indicated high V Condom usage during the study period. Most of the reported sex acts were protected, with participants using more V Condoms than other female condoms and male condoms-in line with uptake of the V Condom at the distribution sites where participants from the C&G NGO, the tertiary institution, and the factory returned for a resupply of V Condoms during the study period.
V Condom users reported preferring the V Condom over the male condom and other female condoms. V Condom users reported their partners wanting both the V Condom and male condoms available, with some preferring the V Condom only. Despite the high reliance on male condoms in general, the majority of participants in the evaluation FGDs reported a preference for the V Condom over male condoms and other female condom products, and all participants indicated that they would be willing and able to use the V Condom to protect against HIV, STIs, and pregnancy.
According to the baseline data, the study sites (tertiary institution, C&G NGO, and factory), government clinics/hospitals/health centers, pharmacies, and shops/supermarkets were named as suitable channels from which to obtain the V Condom, as were workplaces, schools, entertainment places, and tuck shops. The qualitative analysis revealed mixed views on where V Condom should best be accessed-demonstrating the need for varied access points-as females were reluctant to access V Condoms from government clinics, and males were more interested in accessing V Condoms from government hospitals and clinics. Ideal distribution sites were reported to be public social gatherings, bars, clubs, places of work, and easily accessible shops with flexible opening times, and local nongovernmental organizations seemed to be preferred. Factors influencing preferred distribution channels were ease of access, convenience, operating hours, users' previous experiences, and peer influences.
Overall, the quantitative findings showed that most participants were willing to pay for the V Condom if it were available for purchase. Details garnered from the qualitative data showed that the motivation to pay for the V Condom was based on the belief that paying ensured a quality product, and free products are not as safe or trusted.
This novel mixed-methods approach to understanding consumer interest in a new female condom product worked well in terms of providing relevant data for both programmatic and market introduction.
Acknowledgments
The authors would like to thank students from the tertiary institution, clients of the C&G NGO, factory employees, and males at the SRH NGO for their participation in the study. The staff and management of each of the study sites are acknowledged for their support in the success of this project. We thank MatCH Research staff for their support during fieldwork and Abra Greene for preparing this manuscript. PATH would also like to acknowledge financial support from The Netherlands Ministry of Foreign Affairs for our project Expanding Access to the Woman's Condom through the Protection Options for Women Product Development Partnership.
References
-
http://www.rhsupplies.org/activities-resources/groups/newunderused-rh-technologies-caucus/
-
Trussell J, Sturgen K, Strickler J, Dominik R (1994) Comparative contraceptive efficacy of the female condom and other barrier methods. Fam Plann Perspect 26: 66-72.
-
Soper DE, Shoupe D, Shangold GA, Shangold MM, Gutmann J, et al. (1993) Prevention of vaginal trichomoniasis by compliant use of the female condom. Sex Transm Dis 20: 137-139.
-
Fontanet AL, Saba J, Chandelying V, Sakondhavat C, Bhiraleus P, et al. (1998) Protection against sexually transmitted diseases by granting sex workers in Thailand the choice of using the male or female condom: Results from a randomized controlled trial. AIDS 12: 1851-1859.
-
French PP, Latka M, Gollub EL, Rogers C, Hoover DR, et al. (2003) Use-effectiveness of the female versus male condom in preventing sexually transmitted disease in women. Sex Transm Dis 30: 433-439.
-
Hoke TH, Feldblum PJ, Van Damme K, Nasution MD, Grey TW, et al. (2007) Temporal trends in sexually transmitted infection prevalence and condom use following introduction of the female condom to Madagascar sex workers. Int J STD AIDS 18: 461-466.
-
http://www.path.org/publications/detail.php?i=1267
-
Johns Hopkins Bloomberg School of Public Health (2011) Family Planning: A Global Handbook for Providers. World Health Organization (WHO), United States Agency for International Development, Baltimore, USA.
-
Chapman S, Jafa K, Longfield K, Vielot N, Buszin J, et al. (2012) Condom social marketing in sub-Saharan Africa and the Total Market Approach. Sex Health 9: 44-50.
-
Hanson K, Kumaranayake L, Thomas I (2001) Ends versus means: the role of markets in expanding access to contraceptives. Health Policy Plan 16: 125-136.
-
http://www.psi.org/publication/total-market-approach/
-
Htat HW, Longfield K, Mundy G, Win Z, Montagu D (2015) A total market approach for condoms in Myanmar: the need for the private, public and socially marketed sectors to work together for a sustainable condom market for HIV prevention. Health Policy Plan 30: i14-22.
-
Sharma S, Dayaratna V (2005) Creating conditions for greater private sector participation in achieving contraceptive security. Health Policy 71: 347-357.
-
Joanis C, Beksinska M, Hart C, Tweedy K, Linda J, et al. (2011) Three new female condoms: which do South-African women prefer? Contraception 83: 248-254.
-
Schwartz JL, Barnhart K, Creinin MD, Poindexter A, Wheeless A, et al. (2008) Comparative crossover study of the PATH Woman's Condom and the FC Female Condom. Contraception 78: 465-473.
-
Coffey PS, Kilbourne-Brook M, Austin G, Seamans Y, Cohen J (2006) Short-term acceptability of the PATH Woman's Condom among couples at three sites. Contraception 73: 588-593.
-
Moore L, Beksinska M, Rumphs A, Festin M, Gollub EL (2015) Knowledge, attitudes, practices and behaviors associated with female condoms in developing countries: a scoping review. Open Access Journal of Contraception 6: 125-142.
-
Potts M (1984) Cabbages and condoms: packaging and channels of distribution. Clin Obstet Gynaecol 11: 799-809.
-
Denno DM, Hoopes AJ, Chandra-Mouli V (2015) Effective strategies to provide adolescent sexual and reproductive health services and to increase demand and community support. J Adolesc Health 56: S22-41.
-
Beksinska ME, Smit JA, Mantell JE (2012) Progress and challenges to male and female condom use in South Africa. Sex Health 9: 51-58.