International Journal of Women's Health and Wellness
Maternal Calcium Status in First Half of Pregnancy and Gestational Diabetes Mellitus
Kolsoom Safary1, Hamdia Mirkhan Ahmed1* and Lida Moghaddam-Banaem2
1Midwifery Department, College of Nursing, Hawler Medical University, Kurdistan Region, Iraq
2Department of Midwifery and Reproductive Health, Tarbiat Modares University, Tehran, Islamic Republic of Iran
*Corresponding author:
Dr. Hamdia Mirkhan Ahmed, Assistant Professor, Midwifery Department, College of Nursing, Hawler Medical University, Kurdistan Region, Iraq, Tel: 009647504478625, E-mail: hamdia76@gmail.com
Int J Womens Health Wellness, IJWHW-2-012, (Volume 2, Issue 1), Original Article; ISSN: 2474-1353
Received: January 11, 2016 | Accepted: February 22, 2016 | Published: February 24, 2016
Citation: Safary K, Ahmed HM, Moghaddam-Banaem L (2016) Maternal Calcium Status in First Half of Pregnancy and Gestational Diabetes Mellitus. Int J Womens Health Wellness 2:012. 10.23937/2474-1353/1510012
Copyright: © 2016 Safary K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Problem: Gestational Diabetes Mellitus is associated with the disorder in calcium homeostasis.
Background: Regarding this fact which alteration of calcium concentration may be involved in glucose metabolism in a number of pathways, the present study was designed to evaluate maternal calcium status in first half of pregnancy in relation to gestational diabetes mellitus.
Hypothesis: There are relationship between calcium supplementation, dietary calcium intake and urine calcium creatinine ratio and gestational diabetes.
Materials and Methods: A prospective longitudinal study was conducted on 1,033 healthy singleton childbearing women. Assessment of dietary intake of calcium and maternal urine calcium creatinine ratio are performed in 14-24 weeks of gestation. In 24-28 weeks of gestation, Glucose Challenge Test (GCT) were performed for screening of GDM, then all subjects with an abnormal GCT underwent 3-h 100-g Oral Glucose (OGTT) to the diagnosis of GDM.
Findings: Gestational diabetes occurred in 72 (6.96 %) of 1,033 women in the study. There were a statistical relationship between early pregnancy urine calcium creatinine ratio and calcium supplementation with gestational diabetes, mean (SD), 0.29 (0.78) vs. 0.06 (0.25) µg/dl, P value of < 0.001 and mean (SD), 133 (13.83%) vs. 22 (30.5%), P value of = 0.001 respectively. There was no statistical significant difference in calcium nutritional intake between groups. The receiver-operator characteristic curve identified that a maternal urine calcium creatinine ratio less than 0.076µg/dl in early pregnancy is the optimum cutoff value for predicting gestational diabetes.
Conclusion: The results of this study indicate that low urine calcium creatinine ratio and not using the calcium supplement in early pregnancy are related with gestational diabetes mellitus.
Keywords
Urine calcium creatinine ratio, Nutritional intake, Calcium supplementation, Gestational diabetes
Introduction
Gestational diabetes mellitus (GDM) is defined as any degree of glucose intolerance with onset or first recognition during pregnancy. The prevalence may range from 1 to 14% of all pregnancies depending on the population studied and the diagnostic tests employed [1].
The most common result of GDM is macrosomia, which increases in several adverse outcomes during birth, such as shoulder dystocia, perineal lacerations, blood loss, and increased caesarean birth. GDM also increases the risk of glucose metabolism disorders and type 2 diabetes in later life of the mother and the newborn [2].
GDM is a form of type 2 DM, in which a decrease of insulin secretion occurs by the pancreas in response to meals. During the second half of the pregnancy, glucose levels and insulin resistance increase, in part, as a result of diabetogenic hormones [3]. Insulin secretion is a calcium-dependent process [4]; therefore, alterations in calcium flux can have adverse effects on cell secretory function. Calcium is essential for insulin-mediated intracellular processes in insulin-responsive tissues such as skeletal muscle and adipose tissue [5-7], with a very narrow range of intracellular cytosolic calcium [Ca2+]i needed for optimal insulin-mediated functions [8]. Changes in [Ca2+]i in primary insulin target tissues may contribute to peripheral insulin resistance via impaired insulin signal transduction leading to decreased glucose transporter-4 activity [7].
GDM is associated with the disorder in calcium homeostasis and reduced skeletal muscle oxidative phosphorylation [9]. During pregnancy, requirement for calcium is increased; hence insufficient nutritional status might increase the risk of GDM. Calcium supplementation might affect metabolic profiles and oxidative stress through their effects on cell cycle regulation, activation of antioxidant enzymes and suppression of parathyroid hormone (PTH) [8]. In adults at risk of type 2 diabetes, short-term supplementation with cholecalciferol improved β cell function and had a marginal effect on attenuating the rise in Hb A1C [10].
Longitudinal observational studies show that calcium intake was contrarily associated with incident type 2diabetes [11,12]. Asemi et al. assessed the effect of calcium and vitamin D Co supplementation on GDM in a randomized, placebo-controlled study, and they observed calcium plus vitamin D supplementation in women with GDM had beneficial effects on their metabolic profile [13].
There are very limited and conflicting data that have directly examined the relationship between calcium status and gestational diabetes. The present study was designed to evaluate the relationship between calcium supplementation, dietary calcium and urine calcium creatinine ratio and gestational diabetes.
Subjects and Methods
Subjects
A longitudinal prospective research was done during September 2010 to October 2011, on 1,033 childbearing women who attended the prenatal clinics of Medical University Hospitals in Tehran city/ Iran. In 24-28 weeks of gestation, Glucose Challenge Test (GCT) were performed during the first working hours of the day, regardless of the time of the subject's last meal. All subjects with an abnormal GCT (blood glucose level of ≥ 140 mg/dl in one hour after 50 g glucose consumption) underwent 3-h 100 g Oral Glucose Tolerance Test (OGTT) which was classified according to the Carpenter and Coustan criteria for GDM. The OGTT was carried out by the subject in a sitting position after an overnight fasting of 8-14 h, while she was on an unrestricted diet and physical activity for at least 3 days. In 3-h 100-g oral GTT, after consumption of 100-g glucose, blood glucose levels were measured in the subsequent 3 hours. At least two of the four plasma glucose concentrations had to be abnormal for diagnosis of GDM (normal values, fasting < 95 mg/dl; 1 h < 180 mg/dl; 2 h < 155 mg/dl; and 3 h < 140 mg/dl). If only one of the four values was raised, a 3-h 100-g oral GTT was repeated at 32 weeks of pregnancy [2].
Inclusion criteria
• Healthy singleton childbearing women
• Aged 20-35 years
• Having gestational age more than 14 weeks
Exclusion criteria
• Women with history of miscarriage
• Women with preexisting diabetes or a disease affecting glucose metabolism
• Women with active infections
• Women with chronic illness
Food Frequency Questionnaire (FFQ)
Information on nutritional intakes of calcium in early pregnancy was obtained by using a FFQ in the first prenatal visit. This instrument was a semi quantitative food frequency questionnaire which was adapted by Malekshah [14] for simple monitoring of a regular diet over for e.g. the last month; an “ad hoc” questionnaire, designed by an expert dietitian, included a list of foods most frequently consumed in Tehran, Iran. Commonly consumed portions of each item were specified. Photographs were used to compare different portions of each item. Patients were asked to indicate how often a day and how many days a week they consumed every specific food during the past month. Data on cooking methods were also collected. The foods list completed by the expert and trained interviewer were entered into a software program (the computerized dietary analysis system Nutritionist IV, N4 Software).
Calcium supplementation
Some of participants took calcium (500 mg without vitamin D or as multivitamin) as ordered by physicians because of insufficient nutritional status of pregnant women as general in Iran and prevention of preeclampsia in high risk women. The researchers did not intervene with calcium supplementation among the study sample in means of encourage or inhibition.
Urine calcium and creatinine analyses (data measurements)
For assessment of maternal urine calcium creatinine ratio in 14-24 weeks of pregnancy, a 1.5 cc fasting urine sample was obtained from all participants. The oCPC method used for calculating urine calcium. This Calcium oCPC procedure is based on calcium ions (Ca2+) reacting with o-cresolphthalein complexion in an alkaline solution to form an intense violet colored complex which maximally absorbs at 577 nm [15,16]. 8-Hydroxyquinoline is added to remove interference by magnesium and iron [17]. In this method the absorbance of the Ca-oCPC complex is measured bichromatically at 570/660 nm. The resulting increase in absorbance of the reaction mixture is directly proportional to the calcium concentration in the sample. Determination of urine creatinine is carried out by Jaffe method. In 1886, Jaffe reported a reaction of creatinine and picric acid in an alkaline medium forming complex having absorbance maxima at 520 nm. The reaction has been brought to use for the measurement of creatinine by Folin and Wu in 1919. Since then, Jaffe’s reaction has been used [18]. Few biochemical markers have reflected calcium status. Fasting urinary calcium: creatinine ratios may hold promise as an easy, inexpensive method to indicate recent calcium status; therefore this method was applied in our study [19].
Statistical analysis
Nutritional data in the N4 Software were transferred to the SPSS Software version 11.5 for Windows (SPSS, Inc., Chicago, IL). The results were presented as mean (SD). Comparisons between groups were performed using Mann-Whitney, chi-square, and multiple logistic regression tests.
Ethics
Ethical approval for this study was obtained from the Ethics Committee of Tarbiat Modares University that corroborated its ethical considerations throughout the study process. The purpose of the study was explained to all the participants, and then, the informed written consent was taken from them.
Results
The mean (SD) of maternal age was 26.78 (4.4) years and 566 (54.8%) of percipients have normal BMI. A total of 361 patients (34.94) underwent a 3-h 100-g OGTT. Of these 361 patients, 72 were found to have GDM according to the Carpenter and Coustan criteria [2]. The overall incidence of GDM was found to be 6.96 %. Demographic and reproductive characteristics of participants are shown in Table 1. The mean of fasting blood sugar was significantly higher in women with gestational diabetes (93.8 ± 14.8) in comparison with normal women (83.9 ± 9.1).
![]()
Table 1: Demographic comparison of women with gestational diabetes mellitus and a group without gestational diabetes mellitus (n = 1,033).
View Table 1
On the basis of the questionnaire completed at the first prenatal visit, the mean (SD) of daily calcium intake from food for all the participants were 1004.06 (542.78) µg/dl. Maternal urine calcium creatinine ratio and dietary daily intakes of calcium in the diabetic group and normal women are shown in Table 2.
![]()
Table 2: Comparison of urine calcium creatinine ratio, calcium supplementation and dietary calcium intake between the group with gestational diabetes mellitus and group without gestational diabetes mellitus.
View Table 2
There was a significant adverse relationship between urine calcium creatinine ratio and GDM. Regarding the recommended dietary allowance (RDA), daily dietary intake of calcium for childbearing women is 1000 mg [20]. According to RDA, in present study 623(60.3%) of all childbearing women have insufficient nutritional intakes of calcium, 582(60.56%) of normal group and 4 (5.55%) of GDM group. In this respect, there were no statistical differences between groups. Table 2 shows maternal consumption of calcium supplement (500mg calcium) was significantly related to the GDM. However, the results remained unchanged after using the regression model for adjustment of potential risk factors and background characteristics such as age, pre pregnancy BMI, educational level, number of pregnancies, passive smoking, history of gestational diabetes, a history of family diabetes, urine calcium creatinine ratio, nutritional intake of calcium consumption of calcium supplement, and deficient dietary calcium (Table 3).
![]()
Table 3: Variables associated with gestational diabetes in multiple logistic regression analysis.
View Table 3
Figure 1 shows the ROC curve of various cutoff values of maternal urine calcium creatinine ratio in 14-24 weeks of gestation to predict gestational diabetes. The optimal cutoff value for predicting GDM was 0.021µg/dl (Figure 1). At this cutoff value the sensitivity, specificity, positive predictive value, and negative predictive value of urine calcium creatinine ratio were 72, 12, 15.9 and 94.1%, respectively.
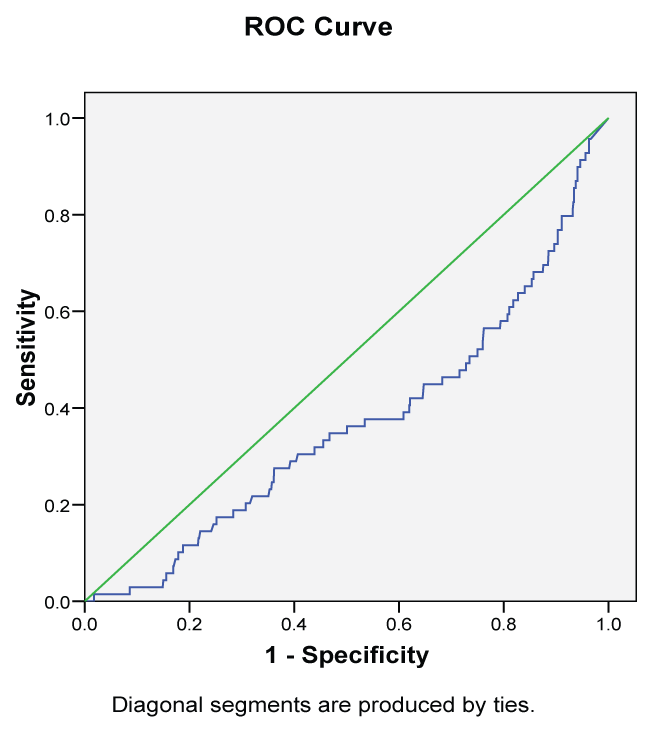
.
Figure 1: The receiver-operator characteristic (ROC) curve of various cutoff points of the maternal urine calcium creatinine ratio in 14-24 weeks of gestation to predict gestational diabetes.
View Figure 1
Discussion
In our study, the estimated prevalence of GDM in the typical population was 6.96% (72 out of 1,033 childbearing women) which was similar to other studies in Iran and other Mediterranean childbearing women [21].
Also, we investigated the possible association between nutritional intake of calcium, calcium supplementation and maternal urine calcium creatinine ratio in 14-24 weeks of gestation and the risk of gestational diabetes mellitus. Apart from a significantly lower maternal urine calcium creatinine ratio and less consumption of calcium supplement in the gestational diabetic group, no significant difference could be noted in the case of other factors studied between normal and GDM groups. This association was independent of established GDM risk factors, such as maternal age; smoking, education, and pre pregnancy BMI; gravidity; and history of gestational and family diabetes.
The major findings made in the current study are the discovery of significant correlations between urine calcium creatinine ratio and calcium supplementation with gestational diabetes mellitus in a large, healthy population.
Insulin secretion is a calcium-dependent biological process [22], and an elevation in calcium is required for both first- and second-phase insulin secretions [23]. Insulin resistance mainly arises from the insensitivity of liver, muscle, and/or adipose tissue to insulin [24]. Muscle is one of the major sites responsible for insulin resistance. Calcium plays a critical role in muscle contractions and in glucose uptake after insulin binds muscle cells. Furthermore, calcium influence the affinity of insulin receptor and sensitivity to insulin [25], whereas calcium and glucagon affect the liver plasma membrane [Ca2+] pump, which is thought to extrude cytosolic calcium of the cell [25].
The regulation of blood glucose and insulin involve many hormonal and physiological factors. Consequently, when trying to reveal true associations between calcium level and any variable of interest, it is critical to exclude possible confounding factors. We resolved this by using a regression model for data analysis, and we observed significant inverse correlations of Urine calcium creatinine ration and calcium supplementation with GDM.
In randomized placebo-controlled trial which was conducted in Kashan, Iran discovered that Calcium plus vitamin D supplementation in women with GDM had beneficial effects on their metabolic profile [13]. In the large cohort of middle-aged women, found that calcium intake were inversely associated with the development of type 2 diabetes, and it’s intakes from supplements rather than from diet were significantly associated with a lower risk of type 2 diabetes [12].
Rob et al. [26] in a prospective cohort study including 41,186 participants of the Black Women's Health Study without a history of diabetes, who completed validated food frequency questionnaires, found that higher calcium intake was not independently associated with risk of type 2 diabetes.
Measurement error in the assessment of dietary intakes is inevitable. We only used dietary intake assessed at baseline, which may have contributed to imprecise results because of dietary changes during follow up. Further studies of calcium and dairy intakes in relation to gestational diabetes mellitus are needed to establish whether effects are independent of other dietary and lifestyle factors.
However, similar to our founding, in the study that analyzed the Calcium signaling proteins in skeletal muscle in women with gestational diabetes, GDM was associated with reduced skeletal muscle oxidative phosphorylation and disordered calcium homeostasis [9]. In the cross sectional study, serum ionized calcium of 46 insulin treated diabetic cases were less than 44 healthy control: mean 1.16 (SD 0.04) vs. 1.21(SD 0.03) mmol/L [27].
Guang et al. in the their study on 1,182 healthy subjects from the province of Newfoundland and Labrador, Canada, found that alteration of serum calcium homeostasis is significantly correlated with the abnormality of glucose level, insulin resistance, and -cell function [28].
The limitations of the present study should be mentioned. With any association study, the results of the present study require confirmation in other cohorts and populations. Furthermore, because of the design and large size of the current study, we used fasting urine calcium creatinine ratio measurements in just one specimen as an indication of body calcium status instead of serum calcium measurement, which is a more precise than fasting urine calcium creatinine ratio.
However, the findings of this study suggest that calcium supplementation in pregnancy decreased the development of GDM. Another result that is very considerable for predicting GDM is the less calcium creatinine ratio in women with GDM in comparing with normal women, before 24 weeks of gestation.
Acknowledgments
The research was financially supported by the Tarbiat Modares University. The authors would like to thank all the participants for their sincere cooperation in the study.
References
-
Metzger BE, Coustan DR (1998) Summary and recommendations of the Fourth International Workshop-Conference on Gestational Diabetes Mellitus. The Organizing Committee. Diabetes Care 21: B161-B167.
-
American Diabetes Association (2004) Diabetes Care. 27.
-
Tracy L. Setji, Ann J. Brown, Mark N. Feinglos (2005) Gestational Diabetes Mellitus. Clinical Diabetes 23: 17-24.
-
Milner RD, Hales CN (1967) The role of calcium and magnesium in insulin secretion from rabbit pancreas studied in vitro. Diabetologia 3: 47-49.
-
Ojuka EO (2004) Role of calcium and AMP kinase in the regulation of mitochondrial biogenesis and GLUT4 levels in muscle. Proc Nutr Soc 63: 275-278.
-
Wright DC, Hucker KA, Holloszy JO, Han DH (2004) Ca2+ and AMPK both mediate stimulation of glucose transport by muscle contractions. Diabetes 53: 330-335.
-
Williams PF, Caterson ID, Cooney GJ, Zilkens RR, Turtle JR (1990) High affinity insulin binding and insulin receptor-effector coupling: modulation by Ca2+. Cell Calcium 11: 547-556.
-
Zemel MB (2002) Regulation of adiposity and obesity risk by dietary calcium: mechanisms and implications. J Am Coll Nutr 21: 146S-151S.
-
Boyle KE, Hwang H, Janssen RC, DeVente JM, Barbour LA, et al. (2014) Gestational Diabetes Is Characterized by Reduced Mitochondrial Protein Expression and Altered Calcium Signalling Proteins in Skeletal Muscle. PLoS One 9: e106872.
-
Mitri J, Dawson-Hughes B, Hu FB, Pittas AG (2011) Effects of vitamin D and calcium supplementation on pancreatic β cell function, insulin sensitivity, and glycemia in adults at high risk of diabetes: the Calcium and Vitamin D for Diabetes Mellitus (CaDDM) randomized controlled trial. Am J Clin Nutr 94: 486-494.
-
Liu S, Song Y, Ford ES, Manson JE, Buring JE, et al. (2005) Dietary calcium, vitamin D, and the prevalence of metabolic syndrome in middle-aged and older U.S. women. Diabetes Care 28: 2926-2932.
-
Pittas AG, Dawson-Hughes B, Li T, Van Dam RM, Willett WC, et al. (2006) Vitamin D and calcium intake in relation to type 2 diabetes in women. Diabetes Care 29: 650-656.
-
Z Asemi, M Karamali, A Esmaillzadeh (2014) Effects of calcium-vitamin D co-supplementation on glycaemic control, inflammation and oxidative stress in gestational diabetes: a randomised placebo-controlled trial. Diabetologia 57: 1798-1806.
-
Malekshah AF, Kimiagar M, Saadatian-Elahi M, Pourshams A, Nouraie M, et al (2006) Validity and reliability of a new food frequency questionnaire compared to 24 h recalls and biochemical measurements: pilot phase of Golestan cohort study of esophageal cancer. Eur J Clin Nutr 60: 971-977.
-
Connerty HV, Briggs AR (1966) Am J. Clin Path 45: 290.
-
Moorehead WR, Biggs HG (1974) 2-Amino-2-methyl-1-propanol as the alkalizing agent in an improved continuous-flow cresolphthalein complexone procedure for calcium in serum. Clin Chem 20: 1458-1460.
-
Walmsley TA, Fowler RT (1981) Optimum use of 8-hydroxyquinoline in plasma calcium determinations. Clin Chem 27: 1782.
-
Kirtimaan Syal, Dibyajyoti Banerjee, Anand Srinivasan (2013) Creatinine Estimation and Interference. Indian J Clin Biochem 28: 210-211.
-
Caulfield LE, Zavaleta N, Shankar AH, Merialdi M (1998) Potential contribution of maternal zinc supplementation during pregnancy to maternal and child survival. Am J Clin Nutr 68: 499S-508S.
-
Munro HN (1981) Nutrient requirements during pregnancy--II. Am J Clin Nutr 34: 679-684.
-
Gandevani SB, Garshasbi A, Dibaj S (2011) Cut-off value of 1-h, 50-g glucose challenge test for screening of gestational diabetes mellitus in an Iranian population. J Obstet Gynaecol Res 37: 534-537.
-
Curry DL, Bennett LL, Grodsky GM (1968) Requirement for calcium ion in insulin secretion by the perfused rat pancreas. Am J Physiol 214: 174-178.
-
Henquin JC, Ravier MA, Nenquin M, Jonas JC, Gilon P (2003) Hierarchy of the beta-cell signals controlling insulin secretion. Eur J Clin Invest 33: 742-750.
-
Williams PF, Caterson ID, Cooney GJ, Zilkens RR, Turtle JR (1990) High affinity insulin binding and insulin receptor-effector coupling: modulation by Ca2+. Cell Calcium 11: 547-556.
-
Pereira MA, Jacobs DR Jr, Van Horn L, Slattery ML, Kartashov AI, et al. (2002) Dairy consumption, obesity, and the insulin resistance syndrome in young adults: the CARDIA Study. JAMA 287: 2081-2089.
-
van Dam RM, Hu FB, Rosenberg L, Krishnan S, Palmer JR (2006) Dietary calcium and magnesium, major food sources, and risk of type 2 diabetes in U.S. black women. Diabetes Care 29: 2238-2243.
-
Fogh-Andersen N, McNair P, Møller-Petersen J, Madsbad S (1982) Serum Calcium Fractions in Diabetes Mellitus. Clin Chem 28: 2073-2076.
-
Sun G, Vasdev S, Martin GR, Gadag V, Zhang H (2005) Altered Calcium Homeostasis Is Correlated With Abnormalities of Fasting Serum Glucose, Insulin Resistance, and beta-cell Function in the Newfoundland Population. Diabetes 54: 3336-3339.





