International Journal of Women's Health and Wellness
Understanding South Asian Immigrant Women's Food Choices in the Perinatal Period
G. M. A. Higginbottom1*, H. Vallianatos2, J. Shankar3, B Osswald4 and C. Davey4
1Mary Seacole Professor of Ethnicity and Community Health, School of Health Sciences, Queen's Medical Centre, Nottingham, UK
2Department of Anthropology, University of Alberta, Alberta, Canada
3Faculty of Social Work, University of Calgary, Alberta, Canada
4Faculty of Nursing, University of Alberta, Alberta, Canada
*Corresponding author:
Gina M. A. Higginbottom, Mary Seacole Professor of Ethnicity and Community Health, School of Health Sciences, Rm 1976, A Floor, South Block Link, Queen's Medical Centre, Nottingham NG7 2HA, UK, Tel: +44-0-115 82 30991, E-mail: gina.higginbottom@nottingham.ac.uk
Int J Womens Health Wellness, IJWHW-2-013, (Volume 2, Issue 1), Research Article; ISSN: 2474-1353
Received: January 13, 2016 | Accepted: February 22, 2016 | Published: February 24, 2016
Citation: Higginbottom GMA, Vallianatos H, Shankar J, Osswald B, Davey C (2016) Understanding South Asian Immigrant Women's Food Choices in the Perinatal Period. Int J Womens Health Wellness 2:013. 10.23937/2474-1353/1510013
Copyright: © 2016 Higginbottom GMA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Food practices throughout the perinatal period have a profound influence on the health and wellbeing of a mother and her child. Following migration, pregnant immigrant women bring with them culturally-situated beliefs about appropriate eating behaviors, while simultaneously encountering new socio-cultural environments that can negatively affect their food choices. Research is needed to inform and improve the provision of culturally appropriate maternal nutritional and healthcare.
Methods: We employed a focused ethnography, photo voice methods, and photo-assisted interviews to explore and understand South Asian immigrant women's food choices and practices during the perinatal period and to investigate the intersectionality of these factors in a social context of cultural adaptation and adjustment.
Findings: The key themes constructed from the data included (a) general health beliefs, (b) antenatal and postnatal food choices including Ayurvedic medical beliefs, (c) social advice and socio-economic factors.
Keywords
Food practices, Immigrant health, Women's health, Culturally appropriate, South Asian, Pregnancy, Perinatal, Canada
Introduction
Food choices and practices throughout the perinatal period have a profound influence on the health and wellbeing of a mother and her child [1,2]. During this vulnerable time period, immigrant women in Canada often encounter social, cultural, and economic challenges that can lead to underutilization of formal maternal health care and other community services, influence their eating behaviors and compromise health outcomes for them and their children [3,4]. Major challenges exist with respect to language fluency, and the provision of culturally safe and competent care, resulting in difficulties in navigating maternity care services by immigrant women. A lack of culturally appropriate health care delivery and negative interactions with the Canadian health care system may have serious consequences for women in the perinatal period [4-6]. Where migrants settle in Canada also affects their relative access to culturally appropriate health care; immigrant communities outside of the three major immigrant-receiving cities in Canada have fewer services available to them.
Negative maternal characteristics and birth outcomes of immigrants include significantly higher rates of gestational diabetes (predisposing the mothers to preeclampsia and type 2 diabetes and their offspring to obesity and type 2 diabetes) [7]; dieting with low maternal weight gain (compromising both newborn and maternal health) [8]; genetic anomalies such as neural tube defects due to lack of folic acid intake [9]; and maternal anemia (increasing the risk of preterm delivery) [10]. A Canadian study also found higher rates of low birth weight and full-term low birth weight (i.e. small for gestational age or SGA) for infants born to recent immigrant women (for this study, first-time registration with the provincial health insurance program within five years of the birth was used as a proxy for recent immigration) [11]. These outcomes are all related to maternal nutrition and food choices, highlighting the crucial importance of understanding immigrant women's food choices and eating behaviors.
The provision of culturally appropriate perinatal nutritional and diet education requires an understanding of women's traditional beliefs and eating practices [12] as well as an exploration of the factors that women encounter within the context of adaptation and adjustment. Immigrant women bring with them a set of culturally-situated beliefs about foods appropriate to eat during the perinatal period, which they often adhere to despite their new social environment [13,14]. Common to many humoral medical traditions, for example, is the belief that consuming foods that are too "hot" during pregnancy will result in miscarriage [15]. Women's food choices may be further shaped by social prescriptions and prohibitions, as well as social regulation (most notably by women's husbands and mothers-in-law) [15].
Evidence suggests an increasing prevalence of obesity post-migration because of the adoption of a Western diet [16]; in part due to "obesogenic" food environments in the vicinities of many immigrants' residences [17]. Conversely, immigrant women may internalize the dominant body norms of their new ethno cultural context and reduce their dietary intake, even during reproduction, to maintain or quickly return to these hegemonic body ideals [8].
The purpose of this research was to explore and understand immigrant South Asian women's ethno cultural food choices and practices as well as other health practices during the perinatal period, and specifically the intersection of these factors in a social context of cultural adaptation and adjustment. Our research question asks: How do the health beliefs and practices of immigrant women affect their food choices during the perinatal period?.
Research Setting
Canada is a multicultural society with a large immigrant population of diverse ethnic origin, first language, culture, religion, traditions, and socio-economic status. According to data from the National Household Survey, Canada had an immigrant population of 6,775,800 as of 2011 (20.6% of the total population) [18]. Immigrants from Asia (including the Middle East) make up the largest group, accounting for roughly 59.6% of all immigrants who arrived between 2006 and 2011 [18]. South Asians are the largest visible minority group in Canada, with a total of 1,567,400 individuals identifying themselves as South Asian [18]. This accounts for one-quarter of the total visible minority population and 4.8% of Canada's total population [18].
In the urban centre where this study took place, the arrival of immigrants in the past decade has been perceptible; South Asian immigrants currently constitute the majority of visible minorities. Visible minority is a term used in Canada that encompasses all populations with characteristics evident to others, which may in turn lead to different experiences than those in the dominant population group [12]. Although there are some health care services geared towards immigrant populations, such as our collaborating community organization, further improvements are still needed as immigrants' knowledge of accessing health services may be insufficient. Our community partner's services include assisting newcomers in applying for provincial health insurance.
Methodological Approach
We employed a focused ethnographic approach, characterized by (a) a conceptual orientation (provided by a single researcher or a team); (b) a focus on a discrete community or organization; (c) a focus on a problem within a specific context; (d) a limited number of participants; (e) the use of participants who may hold specific knowledge; and (f) the episodic or complete lack of observation of the participants [19]. This methodological approach enabled us to best answer our research question, as it is effective in exploring subcultures or groups of people within complex, pluralistic societies and for providing an "emic" (insider) view of a given phenomenon [20,21].
Participants
Purposive sampling [22] was used to select women in Alberta, Canada, who had relocated from a South Asian country (including Bangladesh, Bhutan, India, Nepal, Pakistan, and Sri Lanka) to Canada within the past ten years and who were in the perinatal period (from five months before to one month after parturition). We purposively sampled women from across South Asia to garner a snapshot of general issues these immigrant women faced; we recognize that food practices within South Asia are very heterogeneous and future work needs to further explore these regional food variations and its impacts on perinatal dietary practices. Participants were identified and recruited by collaborators at the Multicultural Health Brokers (MCHB) Co-operative, an award-winning agency serving immigrants in Alberta. Our MCHB collaborators introduced the study to women in their respective communities, obtained informed consent, assisted with interviews, and also acted as interpreters where necessary.
In total, thirteen South Asian women participated in this study. Eight women were from India (including Punjab, Kerala, Gujarat, and Tamil Nadu), two women were from Pakistan (Punjab), two were from Bhutan (Lhotshampa ethnicity), and one was from Nepal (Lamjung). The Indian women, one Pakistani woman, and the Nepali participant were all highly educated, having completed some form of post-secondary education. The Bhutanese women and one Pakistani participant had varying levels of education (grades 7, 10, and 12, respectively). Ages ranged from to 24 to 38, and all women were married. Eleven women were interviewed twice, the other two only once.
Data collection
Data was collected through photo-assisted semi-structured interviews, which incorporated photographs taken by the women and used as visual prompts in the interview process. Following informed consent, a short interview of about 30 minutes was undertaken by a trained research assistant (and translator where necessary) in the participant's home. Low-cost digital cameras were then provided to participants, who received training in their use. They were asked to take photographs of all their meals and snacks (including drinks) during a 3-day period (including one weekend day) and of other foods that they perceive to be healthy or unhealthy for consumption in the perinatal period (Supplementary File). The camera was then collected by the research assistant, who developed hard copies of the photos. This activity did not appear to influence women's views on appropriate foods to avoid/consume during the perinatal period. Instead, this approach allowed participants to capture food practices visually rather than having them verbally recalled, which provided enhanced accuracy and did not discriminate against women with little or limited English fluency. Furthermore, feedback from the participants suggests that the activity was enjoyable and gave them a sense of pride.
Next, a second semi-structured photo-assisted interview (approximately 90 minutes) was conducted in which women were asked to tell their story through the photos. Women were encouraged to discuss whether the food choices represented were typical or not, what factors influences their dietary choices, and what they would like to change. Interview questions also addressed culturally normative practices surrounding perinatal food choices and consumption, including how women negotiate normative practices within their own worldview and experiences.
Data analysis
Data analysis drew upon and adapted the principles expounded by Miles and Huberman [23] which include:
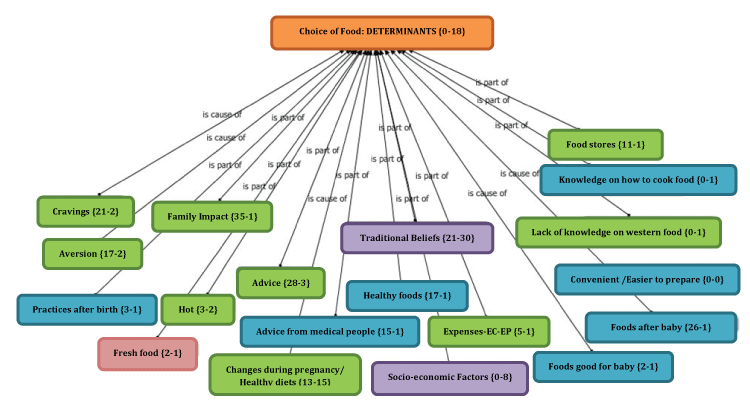
The data was organized into subsets defined by the ethno cultural orientation of the participant, enabling cross-cultural comparisons of the data such that important ethno cultural distinctions and similarities could be determined. Data was stored, managed, classified, and ordered with the aid of ATLAS.ti Scientific Software Development GmbH, a qualitative data analysis software package that facilitates the analysis of visual representations (Figure 1).
Results
The health beliefs and eating practices of the women in the South Asian cohort were variable and women's rich narratives uncovered both similarities and differences amongst the diverse cultures represented in this sample. Our interpretation of the data created three major themes related to South Asian women's food choices during pregnancy: (a) general health beliefs, (b) antenatal and postnatal food choices including Ayurvedic medical beliefs, (c) social advice and socio-economic factors.
General health beliefs
The food choices and practices of South Asian women were influenced by their conceptualizations of health in general, as well as what they believed to constitute a healthy pregnancy. Among all participants, health was defined in holistic terms and women believed that health included both physical and mental wellness: "Healthy body, healthy mind {EI07, I-1, 26, 2011}". [Brace brackets after each quotation provide data regarding the speaker and the quote: (E) number and ethnicity of participant (I-Indian, P-Pakistani, N-Nepali, B-Bhutanese), the interview (I) number, age, and year of speaker's arrival in Canada.] Women's health narratives also included the absence of disease or illness, being physically fit, being able to sleep, and being able to perform normal activities.
Most women exhibited a concentrated effort to be especially healthy during the perinatal period, although there were exceptions as others indicated that they did not change their lifestyle once they became pregnant. Women attained optimal health by eating healthy foods, exercising, and remaining calm and mentally balanced. The importance of balanced eating was also especially salient: "I think the way I'm eating is like I'm trying to include all the categories of the food {EN01, I-1, 27, 2011}". Women's "balanced meals" often consisted of a several foods such as rice or chapatti (an unleavened flatbread), protein such as meat or lentils, and vegetables. Many women referred to meals as healthy as long as they had a balance of these types of foods, and did not have an excess of any one food.
Another key finding across all participants that related to dietary beliefs was an emphasis on fresh foods and home-cooked meals. These types of foods were viewed as more nutritious, healthier, and safer: "If flour is fresh, then chapatti is healthy, you know, extra healthy. If it's a few days old, then the nutrients is gone. Yeah, fresh, definitely fresh is the good {EP01, I-2, 38, 2006}". Women avoided leftovers, preserved foods, and "outside" foods purchased from restaurants or fast food chains, as they were viewed as unhealthy and potentially dangerous to consume.
Finally, women's underlying health concepts were influenced by their concern for the ways in which their eating practices and behaviors would influence the health and development of their child. A common belief among South Asian mothers was that they needed to "eat for two", or considerably increase their overall food consumption, during the perinatal period. Women also shared the belief that their health choices and practices would have a direct influence on their fetus and baby. As such, they made a concentrated effort to make healthy choices: "So if the woman is healthy then the baby is going to be healthy {EP02, I-1, 28, 2011}".
Antenatal and postnatal food choices including Ayurvedic medical beliefs
During the perinatal period, women consumed and avoided certain foods based on the underlying health beliefs discussed above, as well as their individual knowledge. Vegetables, especially green leafy varieties, were mentioned by all South Asian participants to be especially healthy to consume during pregnancy: "The green vegetable, the green leafy vegetable, because when we are pregnant our blood level should be good. It's good and rich in iron {EI07, I-2, 26, 2011}". Fruits were also mentioned as healthy to consume. According to one Indian woman, fruit consumption is believed to result in a lighter-skinned baby, a trait which is highly desired in her culture: "And then if you eat more fruits, then the baby will get, you know, light color {EI05, I-1, 27, 2010}". Dairy products including yogurt and paneer (a fresh curd cheese) were viewed as healthy, and were consumed by some due to their belief that they are especially good for the development of the baby's bones. Indian women may also add saffron into their milk as it is traditionally believed to produce a light skinned baby.
Legumes and pulses (including beans, lentils, and chickpeas) were commonly consumed amongst Indian, Pakistani and Bhutanese women as part of a regular healthy diet, especially for vegetarians. Amongst non-vegetarians from Pakistan and India, chicken was viewed as healthy due to containing protein, energy, fat, and vitamins. Bhutanese women also consumed goat and lamb. Fish was not commonly mentioned, but was an important food for the Nepali participant and one woman from coastal India (Kerala). Soups made with meat and/or bones were consumed by Nepali, Bhutanese and Pakistani women during pregnancy for energy and to promote healthy bones: "...it's very healthy for the bones, and also it's on the whole, it's really good. It, you know, strengthens you, because she says as the pregnancy progresses, you get more and more tired and weaker, so you need that extra strength {EP02, I-2, 28, 2011}".
Grain products such as rice, chapatti, roti, and naan were important to be consumed as part of a regular diet by all women, and these foods accompanied most meals. Finally, Pakistani women consume butter, ghee, and oil in the final month of pregnancy in order to ensure a quicker and easier labor: "And more oil, butter during pregnancy. And at the end of your seven months or eight months, then they said that take more fats, more butter {EP01, I-1, 38, 2006}".
During pregnancy, women actively avoided foods that they believed were unhealthy in general, were particularly harmful to the health of their pregnant body or their baby, and would cause them discomfort or pain. Indian, Nepali and Bhutanese women chose to avoid spicy foods during pregnancy, as they believed that it would give them heartburn or cause the baby to have dark skin or an angry disposition. Fried, oily foods were avoided by some Indian women as they were viewed as unhealthy, and also avoided by Pakistani women who believed that they would cause the baby to slip out of the body. Sugar intake was reduced by some women who were concerned about managing or avoiding gestational diabetes.
Ayurvedic medicine had a significant influence on the food choices women make. In Ayurvedic medicine, foods are grouped based on their ability to heat or cool the body. During pregnancy, women's bodies are viewed as being in a 'hot' state and are thus in need of cooling. Conversely, following birth women's bodies are viewed as ‘cool' and in need of heating. Diet is one way that women can achieve balance throughout the perinatal period.
'Hot' foods are to be avoided during pregnancy, especially during the first trimester, as they can result in miscarriage: "...so the first trimester, not to have hot foods. So because of having hot foods, there's more chances of miscarriage {EP02, I-1, 28, 2011}". 'Hot' foods avoided by women during pregnancy included certain fruits and vegetables, such as papaya, mango, pineapple, eggplant, bitter gourd, and dried dates. Fish, chicken, eggs, nuts, jaggery, cloves, and black pepper were also all considered 'hot' foods that must be avoided.
Spices such as cloves and black pepper were to be avoided during pregnancy as they were considered 'hot' whereas spices such as methi (fenugreek), jwano (thyme), ajwain (carom), jeera (cumin) and fennel were consumed in the postpartum period due to their ability to increase lactation, contract the uterus, increase health, and avoid gas: "Yeah, so they rinse [fenugreek seed] in water. They soak it in water for overnight, and the next day they grind it and then cook it in a lot of ghee and nuts like cashew, almonds and raisins, different raisins, and it is believed that this thing, now it helps for the uterus to contract and go to the normal position, and it also helps to produce a lot of milk. (EN01, I- 2, 27, 2011)".
Women also avoided fried oily foods as they were unhealthy and spicy foods as they could cause heartburn. Caffeinated beverages including tea, coffee, and soda were avoided by Pakistani, Nepali, and Bhutanese women as their consumption was believed to result in lack of sleep and overall poor health.
Postnatally, women continued to consume vegetables for general health, and drink milk to increase lactation and help strengthen their baby's bones. Soups were also an important food for Indian, Pakistani, and Nepali women to consume postnatally. These soups could be prepared with or without meat".Light" foods were also mentioned by Indian and Pakistani participants as being important because they are nutritious and easy to digest. "Light" foods included porridge for Pakistani women and Indian women mentioned khichadi (a dish made from rice and lentils), batata poha (a dish made from pressed rice and potatoes), lentils, thin roti, porridge, seiwan (a dish made from vermicelli noodles, milk, sugar, and ghee) and overcooked rice. However, some Pakistani, Indian, and Nepali women also believed that they should be incorporating rich, heavy foods such as butter, ghee, and oil into their postnatal diet for health to support breastfeeding.
While hot foods were generally avoided during pregnancy, 'hot' foods may be consumed by women in the final month of pregnancy to encourage labor. 'Hot' foods are also encouraged in the postnatal period as they are believed to restore the body and help shed "bad blood": "...it cleanses the body...So if there's any, you know, left in the uterus, it cleans up, yeah {EI02, I-1, 24, 2012}". A 'hot' food commonly consumed by Punjabi Indian and Pakistani women after birth was panjiri, a food prepared with flour, ghee, gond/gondh, nuts, dried fruits, seeds, and spices (such as ginger, fennel, cardamom and carom).
Ayurveda views the body to be in a 'cold' state following birth and the body is believed to be weak and susceptible to illness. As such, it is important for women to avoid 'cold' natured foods: "The cold foods, what they would do is, you know, like the body is very fragile, the woman's after delivery, so those cold foods, you know, then you'd have a lot of back pains and all the pains and all that, yeah. And that's why the cold foods are avoided {EP02, I-1, 28, 2011}".
Women varied in their level of adherence to food restrictions based on Ayurveda, as well as the time frame in which they would avoid certain foods. Many women referred to food restrictions as being important only during the first trimester, while others avoided 'hot' foods for the entire perinatal period. In addition, some women chose to follow some restrictions while ignoring others suggesting generational changes with respect to Ayurvedic traditions.
Social advice and socioeconomic factors
Women received advice regarding healthy foods and practices from family members and Canadian health care workers, which impacted their own dietary choices. All women received health-related advice from family, but the degree to which this advice was followed varied considerably. The majority of advice given to women came from female family members, mostly importantly their mother and/or mother-in-law: "My mother, mother's sister and all. How to eat, "Don't do this, don't do that. Eat this, eat that {EI07, I-1, 26, 2011}". However, some women also received advice from their partners. Many Indian women who lived with their families also had their food choices and practices tightly monitored by others. In these cases, family members regulated or enforced certain health beliefs that may or may not have been believed by the woman herself: "Like often they put the pressure me, "Eat, eat, eat," always. Yeah, because it's the first time so I don't have any experience, right, so I have to listen {EI03, I-1, 25, 2010}". This was also the case for some women despite their family members living back in their home country, who would frequently speak with family members using voice or video calling.
However women varied in the extent to which they followed the advice of family members depending on their level of education and generational changes. "You know, like the old generation as my mom, she was not - she has no education. That's why she was just obeying their moms and their elders. But in our generation we have read from the books, that's good, that's bad, that's not an effect {EP01, I-1, 38, 2006}".
In addition to the information and advice received by relatives, many of the South Asian women received advice regarding healthy eating practices from Canadian health care workers. Pakistani and Indian women in particular placed value on the advice provided by Canadian health care workers, especially when they had been diagnosed with gestational diabetes or other health conditions. However, some women admitted to following only some of the advice provided to them, and one participant explained that the information provided was not suited to her cultural background and dietary restrictions.
A number of factors influenced women's adherence to the dietary advice that they received during pregnancy, including education, living arrangements, and reproductive history. Due to diversity in occupational status, income, education, and social support networks in Canada, there was considerable variation with respect to women's experiences during the perinatal periods. Social support emerged as the most influential socioeconomic factor on women's ability to consume healthy foods and eat what they wanted during the perinatal period. High levels of support from family and/or friends allowed many South Asian women in this study to adhere to their health beliefs and practices throughout the perinatal period.
One factor that influenced women's level of social support was their living situation in Canada. The Bhutanese and Nepali women in this study lived with extended family and perceived high levels of support, while the Pakistani women lived with their husbands and perceived low levels of support. The support systems of Indian women varied greatly, as some lived with extended family and others were socially isolated. Family was the most commonly reported source of support, and often focused on one's husband and in-laws. Women also received some support from friends.
Many South Asian cultures observe a tradition whereby women receive social support in the 40-day period immediately after having a baby. This tradition was specifically mentioned by Indian and Pakistani women, but not the Nepali or Bhutanese women. This postpartum period is characterized by mandated rest for the new mother. During this time, women are required or encouraged to stay in the home, rest, and avoid physical labor. Consequently, women are relieved of their domestic duties and are attended to by close female family relatives who take on the responsibilities of cooking, cleaning, and care of other children: "...I'm fully satisfied by what I'm getting. Yeah. Because like I'm not even like - except for feeding her, like they are taking care of everything, you know. I think I forgot cooking. [laughter] {EN01, I-1, 27, 2011}". This social support ensured that women were able to consume enough food, eat traditional postpartum foods, and had access to foods that they wanted to eat.
In contrast, women who had lower levels of perceived support found it difficult to adhere to traditional eating practices, cook, and consume healthy foods following birth:
"When we are pregnant, having a baby with ourself, by ourself, it really affects our pattern. If we have something with us, someone with us to help us to make something, and we have every - all the available stuff, what we want to eat, then that'll be good. Otherwise it plays a big part...Standing in the kitchen for more than one hour, it's better to stand in the kitchen for 30 minutes when we are by ourself, right? Easy. We used to cook the way which is easy for us". {EI07, I-2, 26, 2011}
As the above quote illustrates, women who are isolated in Canada and lack social support may be unable to consume the foods they desire, instead choosing more convenient, less healthy foods as a result of time constraints and issues with shopping for food.
In addition to social support, household income emerged as a factor influencing women's food choices. As the employment status of women and their husbands was variable, income level and cost of food was a concern for some women but not for others.
Women that did not find income to be an issue had at least two household incomes, were supported by their husband, and/or lived with extended family. These women had no constraints purchasing healthy foods, and also noted that they could purchase traditional foods despite their higher cost in Canada. In contrast, women who viewed income as a constraint had one household income in the perinatal period, lived with only their husbands, and had no family in Canada. These women discussed having difficulty affording healthy foods: "You know, no, there's not enough income...If we are going to a market and buying this salad things, then no, it's really expensive. You know, it's not easy to buy all the stuff and daily we can't have this one. Yeah, it's hard {EP01, I-2, 38, 2006}". In an effort to manage food costs, women would make food substitutions or limit their consumption of more expensive foods: "Here, a big cauliflower it's like five dollars or six dollars. The same time I can get a broccoli for one or two dollars, something. Then I'll go for the broccoli, right? It's like that {EI07, I- 2, 26, 2011}".
Conclusions
Each of the participants provided a snapshot on the range of issues facing immigrant mothers. For instance, some were highly educated and well-versed in biomedical models of nutrition while others relied on female kin to guide their food practices. Furthermore, these women had variable levels of social support as opposed to traditional extended family structures back home. Some participants had low household incomes while others were more financially secure. These variations highlight the challenges health practitioners face in caring for immigrants, in the wide variations affecting food practices within any ethno cultural group.
In general, participants were comfortable with customary food practices, and voiced little concern or desire to alter these practices; they were unconcerned about Canadian food guide recommendations unless they had a health issue such as gestational diabetes. The major issue affecting women's abilities to follow these customary practices was affordability of the required foods. Within this context, immigrant women's perinatal food choices are profoundly influenced by ethno-cultural determinants which may not correspond to Health Canada's current food guidelines food guidelines making it difficult for health care providers to classify and access nutritional value of ethno-cultural food (e.g. protein, fats, carbohydrates).
Socioeconomic factors were variable among the sample and were not overtly stated to be an issue affecting the ability to make healthy food choices, however, it is worth considering that lower socioeconomic status could affect one's ability to purchase nutritionally dense foods. The importance of social support in maintaining and enforcing healthy eating and healthy behaviors was highlighted by almost all immigrant women.
In summary, our study identifies important issues affecting the nutritional health of South Asian immigrant women, and highlights challenges in providing culturally appropriate health care: not only is the South Asian migrant community heterogeneous, but cultural variations within specific South Asian cultures are reflective of socioeconomic experiences and backgrounds. Future work needs to explore these variations in detail. These findings have important implications for Canadian health care providers, and potentially any health care context serving South Asian migrant populations. Knowledge about the food choices of South Asian women during the perinatal and postnatal periods, and the influence of indigenous systems of medicine like Ayurveda can be very useful for western educated service providers. This knowledge can help to provide culturally relevant advice that includes the best of both knowledge systems.
Acknowledgements
Support for this work was provided by the Canadian Institute of Health Research (CIHR) under Grant RES Pro00029147 and in part by GH as a CIHR Canada Research Chair (www.chairs-chaires.gc.ca). We would like to thank the Multicultural Health Brokers Cooperative for facilitating our access to participants in this study and also guiding our research practice in terms of cultural safety and competence.
Ethical Statement
Before commencing research, ethics approval was obtained from the University of Alberta Health Research Ethics Board.
References
-
Higginbottom GMA, Morgan M, Dassanayake J, Eyford H, Alexandre M, et al. (2012) Immigrant women's experiences of maternity care services in Canada: a protocol for systematic review using a narrative synthesis. Sys Rev 1: 27.
-
Higginbottom GMA, Mamede F, Barolia R, Vallianatos H, Chambers T (2014) Aboriginal and immigrant women's food choices and practices in pregnancy: a scoping review. CJMRP 13: 16-35.
-
Higginbottom GMA, Morgan M, Chiu Y, Forgeron J, Kocay D, et al. (2015) Immigrant women's experiences of maternity-care services in Canada: a systematic review using a narrative synthesis. Syst Rev 4.
-
Higginbottom GM, Hadziabdic E, Yohani S, Paton P (2014) Immigrant women's experience of maternity services in Canada: a meta-ethnography. Midwifery 30: 544-559.
-
Meddings F, Haith-Cooper M (2008) Culture and communication in ethically appropriate care. Nurs Ethics 15: 52-61.
-
Reitmanova S, Gustafson DL (2008) "They can't understand it": maternity health and care needs of immigrant Muslim women in St. John's, Newfoundland. Matern Child Health J 12: 101-111.
-
Renzaho A, Skouteris H, Oldroyd J (2010) Preventing gestational diabetes mellitus among migrant women and reducing obesity and type 2 diabetes in their offspring: a call for culturally competent lifestyle interventions in pregnancy. J Am Diet Assoc 110: 1814-1817.
-
Hyman I, Dussault G (2000) Negative consequences of acculturation on health behavior, social support and stress among pregnant Southeast Asian immigrant women in Montreal: an exploratory study. Can J Public Health 91: 357-360.
-
Grewal SK, Bhagat R, Balneaves LG (2008) Perinatal beliefs and practices of immigrant Punjabi women living in Canada. J Obstet Gynecol Neonatal Nurs 37: 290-300.
-
Nybo M, Friis-Hansen L, Felding P, Milman N (2007) Higher prevalence of anemia among pregnant immigrant women compared to pregnant ethnic Danish women. Ann Hematol 86: 647-651.
-
Urquia ML, Frank JW, Glazier RH, Moineddin R (2007) Birth outcomes by neighbourhood income and recent immigration in Toronto. Health Rep 18: 21-30.
-
Higginbottom GM, Vallianatos H, Forgeron J, Gibbons D, Mamede F, et al. (2014) Food choices and practices during pregnancy of immigrant women with high-risk pregnancies in Canada: a pilot study. BMC Pregnancy Childbirth 14: 370.
-
Matthey S, Panasetis P, Barnett B (2002) Adherence to cultural practices following childbirth in migrant Chinese women and relation to postpartum mood. Health Care Women Int 23: 567-575.
-
Essén B, Johnsdotter S, Hovelius B, Gudmundsson S, Sjöberg NO, et al. (2000) Qualitative study of pregnancy and childbirth experiences in Somalian women resident in Sweden. BJOG 107: 1507-1512.
-
Vallianatos H (2010) Poor and pregnant in New Delhi, India. Indian edn, Munshiram Manoharlal Publishers, New Delhi, India.
-
McDonald JT, Kennedy S (2005) Is migration to Canada associated with unhealthy weight gain? Overweight and obesity among Canada's immigrants. Soc Sci Med 61: 2469-2481.
-
Hemphill E, Raine K, Spence JC, Smoyer-Tomic KE (2008) Exploring obesogenic food environments in Edmonton, Canada: the association between socioeconomic factors and fast-food outlet access. Am J Health Promot 22: 426-432.
-
National household survey (2011) Immigration adn ethocultural diversity in Canada.
-
Mueke MA (1994) Critical issues in qualitative research methods. In: Morse JM, On the evaluation of ethnographies. Sage, Thousand Oaks, CA, 187-209.
-
Fetterman DM (1998) Ethnography: Step by step. Sage, Thousand Oaks, CA.
-
Spradley JP (1979) The ethnographic interview. Holt, Rinehart, and Winston, New York.
-
Higginbottom GM (2004) Sampling issues in qualitative research. Nurse Res 12: 7-19.
-
Miles MB, Huberman AM (1994) An expanded sourcebook: qualitative data analysis. (2nd edn), Sage, Thousand Oaks, CA.