International Journal of Women's Health and Wellness
Diffuse Adenomyosis Treated by Laparoscopic Conservative Surgery: A Case Report
Mauro Monteiro de Aguiar1*, Helena Juliana Nagy2, Marianna Fernandes Miranda3, Karina Sampaio Cavalcanti3 and Lorena Jackson3
1Head of Gynecologic Endoscopic Surgery Unit, Hospital das Clínicas of Federal University of Pernambuco, Brazil
2Professor of Gynecologic Endoscopic Surgery Unit, Hospital das Clínicas of Federal University of Pernambuco, Brazil
3Resident Doctor of Gynecology and Obstetrics Service, Hospital das Clínicas of Federal University of Pernambuco, Brazil
*Corresponding author:
Mauro Monteiro de Aguiar, Head of Gynecologic Endoscopic Surgery Unit, Hospital das Clínicas of Federal University of Pernambuco, Brazil, E-mail: mauro.aguiar2@gmail.com
Int J Womens Health Wellness, IJWHW-2-019, (Volume 2, Issue 2), Case Report; ISSN: 2474-1353
Received: April 12, 2016 | Accepted: May 16, 2016 | Published: May 18, 2016
Citation: de Aguiar MM, Nagy HJ, Miranda MF, Cavalcanti KS, Jackson L (2016) Diffuse Adenomyosis Treated by Laparoscopic Conservative Surgery: A Case Report. Int J Womens Health Wellness 2:019. 10.23937/2474-1353/1510019
Copyright: © 2016 de Aguiar MM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Adenomyosis consists in a benign gynecological condition that is characterized histologically by the presence of ectopic endometrial tissue in the myometrium. Clinically, it is characterized by dysmenorrhea and menorrhagia, dyspareunia, chronic pelvic pain and even infertility. The failure of clinical treatment requires hysterectomy. However, conservative surgery has been proposed as a feasible and safe option for treatment of adenomyosis, when dealing with young patients, in order to preserve the uterus. However, few data is available for laparoscopic approach in symptomatic diffuse form of the disease. We report a 22-year-old woman who underwent a conservative laparoscopic surgery for diffuse form of adenomyosis, confirmed by histology, with significant relief of pain and return to her usual activities.
Keywords
Adenomyosis, Laparoscopy, Dysmenorrhea, Hypermenorrhea
Introduction
Adenomyosis is a benign gynecological condition characterized by the presence of endometrial glands and stroma in the myometrium [1,2]. It may be found distributed within the whole uterine wall - in diffuse form - or in a limited area - as focal adenomyosis [3]. This ectopic tissue seems to induce hypertrophy and hyperplasia of the subjacent myometrium resulting in diffusely enlarged uterus [4]. Definitive diagnosis requires histopathological analysis of the uterus [5].
Clinical manifestations commonly includes dysmenorrhea and menorrhagia, but also dyspareunia, chronic pelvic pain and infertility have been reported [6]. Multiparous women in their forties or fifties are most affected [7]. Although, severe disease in younger women of reproductive age have been identified, mainly by improvement in imaging modalities [8].
Hysterectomy plays an important role in symptomatic patients who failed medical therapy. On the other hand, there is no consensus on the appropriate treatment for symptomatic adenomyosis in patients who want to preserve the uterus [9]. In this scenario, conservative surgical treatment has been performed in younger women [10] but, there are not many reports regarding the results of this management.
Since Hyams in 1952 [11] suggested the use of conservative surgery for the treatment of adenomyosis, some surgical techniques have been described [8]. These techniques propose resection of adenomyosis lesions and then the reconstruction of the uterine wall. The most effective treatment requires a more extensive resection of the affected tissues. However, this can lead to major defects in the uterine wall, posing a risk of uterine rupture during pregnancy as a complication of the procedure [12].
In case of focal adenomyosis, surgical procedure to preserve the uterus has been reported [7,10,11], but few surgical treatments have been described for diffuse adenomyosis, mostly, by open laparotomy.
Therefore, here we describe an uncommon case of a young patient with diffuse adenomyosis, presenting significant involvement of the anterior uterine wall and fundus, who underwent laparoscopic conservative surgery. The case report is followed by a review of the relevant literature.
Case Report
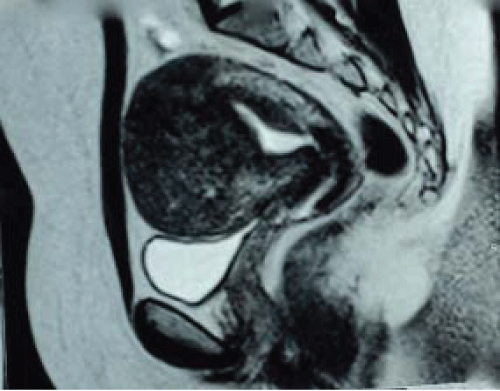
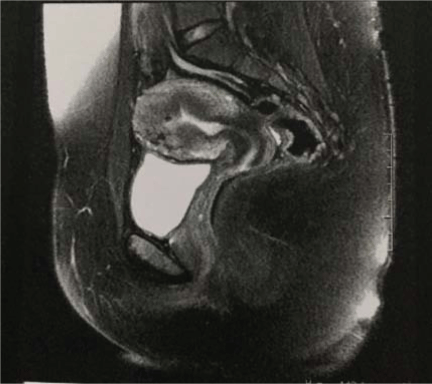
A 22 years old nulligravid female, without comorbidities or past pelvic surgery, presented incapacitating dysmenorrhea and menorrhagia for about a year. Pelvic magnetic resonance imaging (MRI) showed an overall increase in uterine volume (229 cm3) with diffuse thickening of the junctional zone in the anterior wall, measuring up to 53 mm. These findings were compatible with adenomyosis (Figure 1). The CA 125 level was 200.7 U/ml.
The initial clinical treatment included combined oral contraceptive (gestodene 75 mg and ethinylestradiol 30 mcg - Gestinol 28™) and non steroidal anti-inflammatory drugs (ketoprofen 100 mg - Profenid™). Then it was suggested using dienogest 2 mg (Allurene™), which was administered for 5 months, without improvement on the pelvic pain. After a year of clinical following, the patient came to our hospital.
Considering the patient's age and the clinical treatment failure, it was proposed a conservative laparoscopic surgery. The procedure was performed under general anesthesia in the Trendelenburg position with four-port laparoscopy. It was introduced one 10 mm port through the umbilicus for the zero-degree laparoscope, one 10 mm left lateral, and another 10 mm right lateral and one 5 mm infra-umbilical port were inserted. The surgeon used the central and the left-sided lateral port to perform most of the surgical procedures.
.
Figure 1: MRI before surgery showing an overall increase in uterine volume with thickening of the junctional zone.
View Figure 1
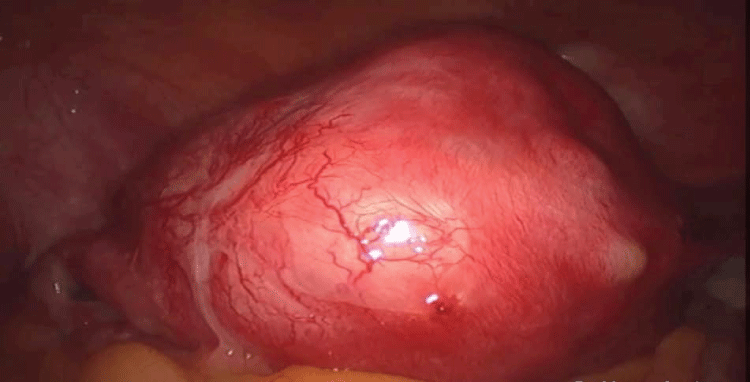
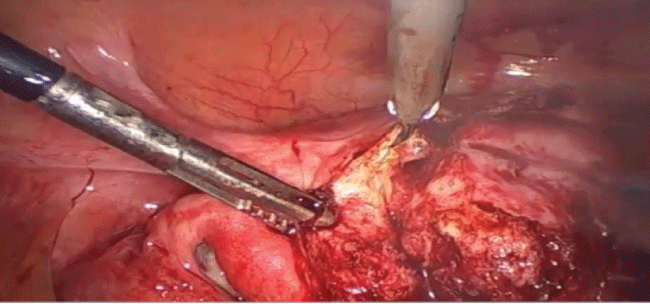
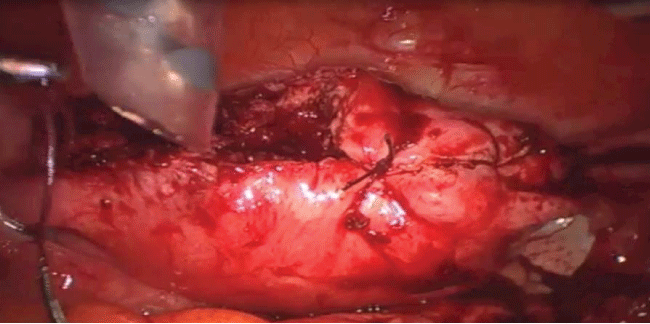
At first, it was injected into the uterine wall a vasoconstrictor agent diluted in saline solution in order to decrease bleeding during surgery. Using an ultrasonic scissor, a horizontal incision was made in the uterine fundus respecting the limits of the fallopian tubes. The incision continued along the coronal direction, however, the uterine cavity was never reached. A second incision was done, making a wide wedge-shaped resection of the anterior uterine wall and fundus. The incision was further continued along the anterior wall of the uterus. Afterward, the affected tissues were clamped with a forceps, identified and removed from the surrounding myometrium. If the myometrium appeared normal, it was spared as much as possible. The procedure was performed with caution to avoid damaging the endometrium (Figure 2 and Figure 3). The myorrhaphy was performed with interrupted sutures in two layers with polyglactin (Figure 4). The conservative procedure was concluded in 95 minutes.
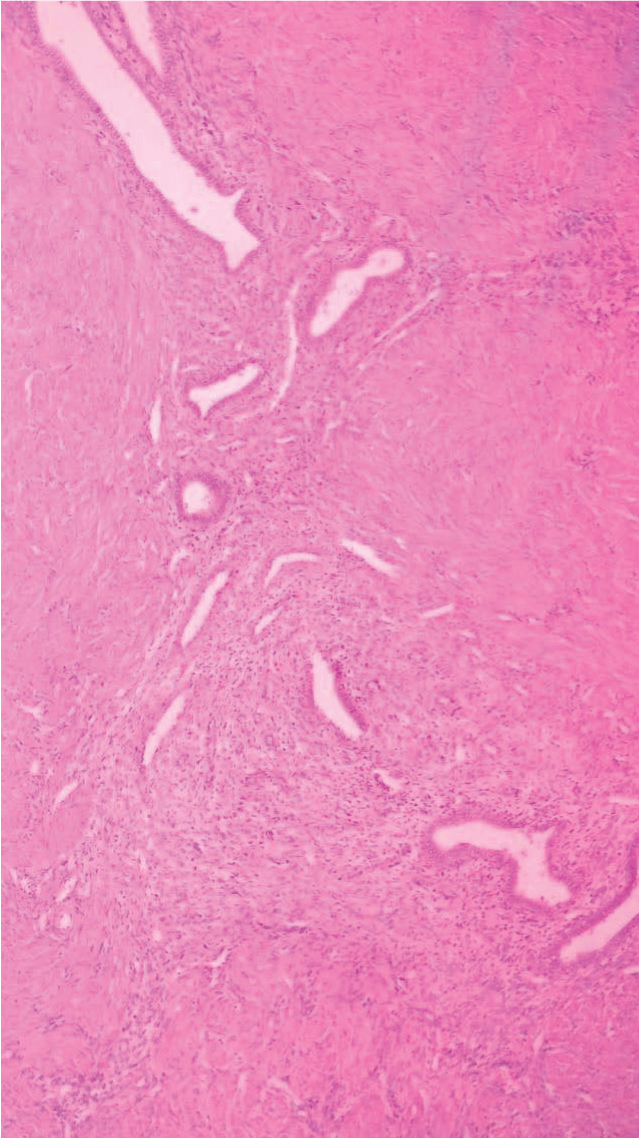
On the second postoperative day the patient was discharged without pain complaint and in good clinical condition. Histopathology analysis show presence of endometrial tissue in the myometrium, confirming adenomyosis (Figure 5 and Figure 6).
.
Figure 5: Histopathology analysis: presence of endometrial tissue in the myometrium.
View Figure 5
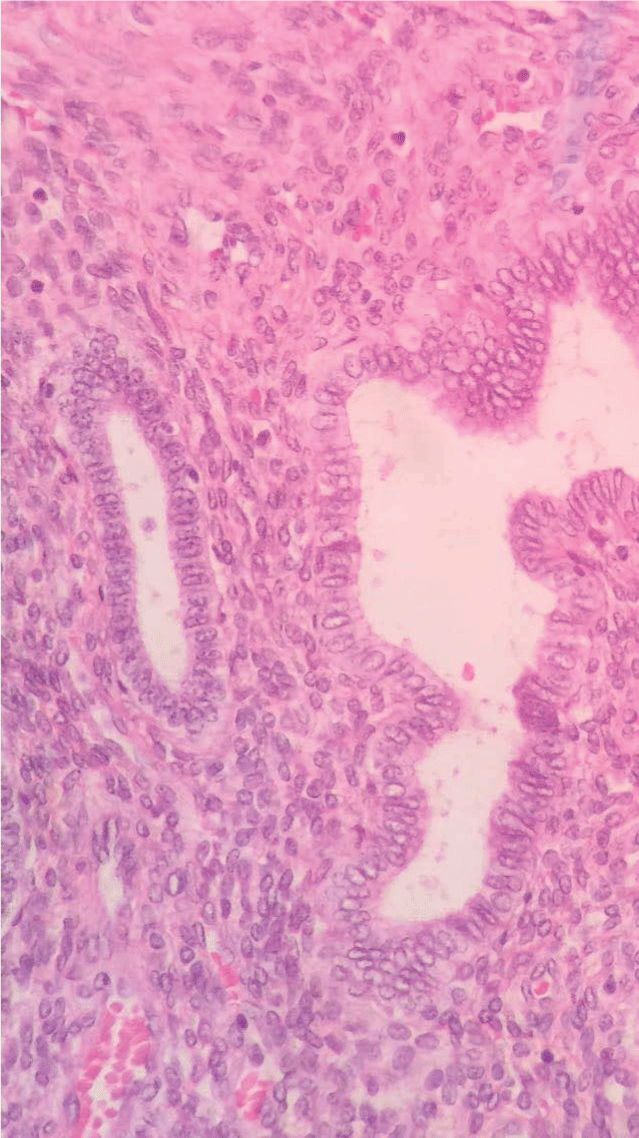
.
Figure 6: Histopathology analysis: presence of endometrial tissue in the myometrium.
View Figure 6
After surgical treatment, she related improvement in pain on the Visual Analog Scale (VAS). Her evaluation of the pre and post-operative pain received 10 and 02 points, respectively, after 1 year of follow-up. New pelvic MRI, 11 months after surgery, showed total uterine volume of 172 cm3, endometrium measuring 8 mm and junctional zone measuring 1.4 mm (Figure 7). Since the procedure, the patient has used continuous combined oral contraceptive pills (gestodene 75 mcg and ethinyl estradiol 30 mg - Gestinol 28™) and has returned to her work activities, which she was unable to perform before surgery.
.
Figure 7: MRI after surgery showing reduced uterine volume and thickening of the junctional zone.
View Figure 7
Discussion
Adenomyosis treatment in young patients is a challenging condition. Our patient, a 22-year-old woman, with no previous pregnancies had a presumed clinical diagnosis of adenomyosis, with disabling chronic pelvic pain and hypermenorrhea. Imaging study (MRI) revealed overall increase of total uterine volume, thickening of junctional zone with significant anterior uterine wall and fundus involvement, compatible with diffuse adenomyosis. Initially, the patient was treated with nonsteroidal anti-inflammatory drugs and an oral contraceptive. Another option, dienogest, has been attempted for five months.
The first line of treatment of adenomyosis includes symptomatic drugs such as the administration of nonsteroidal anti-inflammatory drugs and hormone therapy with a gonadotropin-releasing hormone (GnRH) agonist, danazol, and oral contraceptives [8]. Yet, the effects of the drug treatment are usually temporary, and symptoms often recur when patients stop taking medication [13]. Dienogest, an oral progestin, has been extensively researched in the treatment of endometriosis, but a pilot study has suggested that dienogest is an effective and well-tolerated therapy for symptomatic adenomyosis [14]. In addition, association between adenomyosis and pelvic endometriosis is occasionally reported [3]. After failure of medical treatment, hysterectomy is an option; however, it does not apply for cases of women who want to preserve fertility for the future [15].
Despite the medical treatment offered, she remained with hypermenorrhea and disabling dysmenorrhea. Then, she came to our hospital for evaluation of other possible treatments. Aiming at the uterus preservation, our team proposed a conservative laparoscopic surgery, a poorly described technique.
In our case, the patient underwent laparoscopic cytoreduction surgery. It was performed a horizontal incision in the uterine fundus with a wide wedge-shaped resection of the anterior uterine wall and fundus, without accessing the endometrial cavity. There was also the concern of preserving the tubes. Before the incision, it was infused a solution with vasoconstrictor agent. The procedure had an average duration of 95 minutes. The patient also had a short period of hospitalization after the procedure. After 1 year of follow-up, she also showed improvement in the dysmenorrhea complaints, downgrading from 10 (before) to 2 (after surgery) in assessment of Visual Analog Scale (VAS).
Takeuchi et al. conducted laparoscopic conservative surgery in 14 patients with adenomyosis, using a different way of reconstruction of uterine wall (double-flap method). The study presented similar results regarding duration of the procedure and period of hospitalization. The average operation time was 101.5 min and the average estimated blood loss was 225 cc. There were no cases of complications during the operations. Patients had a 3 days period of hospitalization after surgery without abnormalities. The medium-term monitoring of these patients showed a significant reduction in the average value of the analog pain scale before to after surgery. All 8 patients with hypermenorrhea showed improvement after the operation [8].
Osada et al. performed uterus preserving open surgery using triple-flap method in 104 patients suffering from massive adenomyosis. The study obtained similar results regarding pain relief. Moreover, of the 26 patients who wished to become pregnant, 14 succeeded with term pregnancies. No uterine rupture complication was reported [12].
Kim et al. reported 11 cases of laparoscopic-assisted adenomyomectomy using the double flap method is effective for uterine reduction and relief of dysmenorrhea and hypermenorrhea, evaluated by VAS [6].
The long-term follow-up can evaluate the possibility of term pregnancy for this patient. Pregnancy have been described after conservative treatments for adenomyosis, but the number of cases for each treatment is still small [7]. Tsui et al. suggests there was, in fact, an improvement in reproductive performance, compared with women treated with medical treatment only, observed by higher cumulative pregnancy rates, and higher cumulative final successful delivery rates. Taken together, conservative surgery might be an alternative if subfertile women with adenomyosis fail to become pregnant after an active treatment. Conversely, the author reminds that, conservative surgery might result in additional risk of adhesion, deformity of the uterus, occlusion of the Fallopian tubes and risk of total and/or subtotal hysterectomy, similar to any kind of uterine surgery, including myomectomy, which might compromise the ability to get pregnant. Therefore, more studies need to be performed in order to evaluate these outcomes [16].
Our study showed a case of laparoscopic conservative surgery for the treatment of diffuse adenomyosis in a young patient as a feasible and safe option for treatment, instead of classic hysterectomy. There are few descriptions in the literature for this approach and in this case, it results in clinical improvement of symptoms. The result stands out for the increased quality of life acquired after the treatment by the patient.
References
-
Bird CC, McElin TW, Manalo-Estrella P (1972) The elusive adenomyosis of the uterus--revisited. Am J Obstet Gynecol 112: 583-593.
-
Siegler AM, Camilien L (1994) Adenomyosis. J Reprod Med 39: 841-853.
-
Gordts S, Brosens JJ, Fusi L, Benagiano G, Brosens I (2008) Uterine adenomyosis: a need for uniform terminology and consensus classification. Reprod Biomed Online 17: 244-248.
-
Saremi A, Bahrami H, Salehian P, Hakak N, Pooladi A (2014) Treatment of adenomyomectomy in women with severe uterine adenomyosis using a novel technique. Reprod Biomed Online 28: 753-760.
-
McElin TW, Bird CC (1974) Adenomyosis of the uterus. Obstet Gynecol Annu 3: 425-441.
-
Kim JK, Shin CS, Ko YB, Nam SY, Yim HS, et al. (2014) Laparoscopic assisted adenomyomectomy using double flap method. Obstet Gynecol Sci 57: 128-135.
-
Nishida M, Takano K, Arai Y, Ozone H, Ichikawa R (2010) Conservative surgical management for diffuse uterine adenomyosis. Fertil Steril 94: 715-719.
-
Takeuchi H, Kitade M, Kikuchi I, Shimanuki H, Kumakiri J, et al. (2006) Laparoscopic adenomyomectomy and hysteroplasty: a novel method. J Minim Invasive Gynecol 13: 150-154.
-
Horng HC, Chen CH, Chen CY, Tsui KH, Liu WM, et al. (2014) Uterine-sparing surgery for adenomyosis and/or adenomyoma. Taiwan J Obstet Gynecol 53: 3-7.
-
Van Praagh I (1965) Conservative surgical treatment for adenomyosis uteri in young women: local excision and metroplasty. Canadian Medical Association Journal 93: 1174-1175.
-
HYAMS LL (1952) Adenomyosis; its conservative surgical treatment (hysteroplasty) in young women. N Y State J Med 52: 2778-2784.
-
Osada H, Silber S, Kakinuma T, Nagaishi M, Kato K, et al. (2011) Surgical procedure to conserve the uterus for future pregnancy in patients suffering from massive adenomyosis. Reprod Biomed Online 22: 94-99.
-
Wood C (1998) Surgical and medical treatment of adenomyosis. Hum Reprod Update 4: 323-336.
-
Hirata T, Izumi G, Takamura M, Saito A, Nakazawa A, et al. (2014) Efficacy of dienogest in the treatment of symptomatic adenomyosis: a pilot study. Gynecol Endocrinol 30: 726-729.
-
Huang X, Huang Q, Chen S, Zhang J, Lin K, et al. (2015) Efficacy of laparoscopic adenomyomectomy using double-flap method for diffuse uterine adenomyosis. BMC Women's Health 15: 24.
-
Tsui KH, Lee FK, Seow KM, Chang WC, Wang JW, et al. (2015) Conservative surgical treatment of adenomyosis to improve fertility: controversial values, indications, complications, and pregnancy outcomes. Taiwan J ObstetGynecol 54: 635-640.