International Journal of Women's Health and Wellness
Completion of Free Human Papillomavirus Vaccination Series at an Urban, Public Hospital
Sonia Guleria1, Alexandra Jones2, Lindsay Zimmerman1, Kelly Stempinski1 and Ashlesha Patel1,2*
1Department of Obstetrics and Gynecology, Division of Family Planning, USA
2Department of Obstetrics and Gynecology, Feinberg School of Medicine, Northwestern University, USA
*Corresponding author:
Ashlesha Patel, MD, MPH, Associate Professor, Department of Obstetrics and Gynecology, Northwestern University Feinberg School of Medicine, John H. Stroger Jr. Cook County Hospital 1901 W. Polk St 5th Floor, Chicago, IL 60622, USA, Tel: 312-864-5935, Fax: 312-864-9782, E-mail: apatel2@cookcountyhhs.org
Int J Womens Health Wellness, IJWHW-2-026, (Volume 2, Issue 3), Original Research; ISSN: 2474-1353
Received: April 13, 2016 | Accepted: July 08, 2016 | Published: July 11, 2016
Citation: Guleria S, Jones A, Zimmerman L, Stempinski K, Patel A (2016) Completion of Free Human Papillomavirus Vaccination Series at an Urban, Public Hospital Int J Womens Health Wellness 2:026. 10.23937/2474-1353/1510026
Copyright: © 2016 Guleria S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Completion of the three-dose human papillomavirus (HPV) vaccine series has been challenging and cost may play a role. The objectives of this study were 1) to evaluate vaccine completion rates after receipt of first dose and 2) to determine factors associated with vaccine completion among women presenting at an urban, public hospital, where the vaccine was provided free of charge.
Methods: A retrospective chart review was conducted of women age 14-26 years, who initiated the first HPV vaccine (Gardasil quadrivalent) dose during January 2010-December 2012, at Stroger Hospital's Family Planning Clinic in Chicago, IL. The outcome of interest was completion of all three vaccine doses. Log-binomial regression analysis was conducted to determine the socio-demographic and medical factors associated with completion.
Results: A total of 201 women initiated the first dose of the vaccine and were followed for an average time of 3.1 years. Over 68% of women self-identified as Non-Hispanic Black and 17% as Hispanic. Around 31% of women completed all three doses of the vaccine. The independent predictors of completion were Hispanic race/ethnicity (RR: 1.55; 95% CI: 1.00-2.41) and older age (RR: 2.45 (ages 25-26 vs. 14-19); 95% CI: 1.17-5.11).
Conclusion: HPV vaccine completion rates did not increase even when the vaccine was provided free of cost. This suggests that other incentives or measures must be adopted to increase participation among women who are younger and from ethnic minorities.
Keywords
HPV vaccine, Completion, Free, Women, Cost
Introduction
Human Papillomavirus (HPV) is a group of sexually transmitted viruses that poses significant public health issues, leading to both benign and malignant conditions, such as cervical, anogenital and oropharyngeal cancers [1]. Nearly 14 million Americans are newly diagnosed with HPV infection every year [2]. A majority of sexually active young people will acquire this virus at some point in their lives [1]. Although up to 90% of infections are cleared without any harm, its burden on the health care system is still enormous [3].
HPV vaccines introduced in 2006, represent a major advancement in preventive health for women. They can drastically lower risk for selective cancers in both women and men. In a study by Crowe et al., HPV vaccine was reported to decrease the risk for high grade cervical lesions (cervical intraepithelial neoplasia 2, adenocarcinoma in situ, or worse) by 46% [4]. However, HPV vaccination programs have faced challenges in access and uptake, leading to poor acceptance and less than impressive completion of its three part series, ultimately lowering its effectiveness. According to the National Immunization Survey (NIS), 40% of adolescent girls ages 13-17 years received all three doses of HPV vaccine in 2014 [5]. Compared with other vaccine programs, such as Hepatitis B, where penetration was up to 99% among adolescents, the uptake rates for HPV vaccine are exceptionally low [6].
Factors associated with vaccine completion have been cited in previous studies [7-12]. African-American and Hispanic race/ethnicity, having public insurance, lack of provider recommendation, distrust in vaccination programs and concerns regarding modification of sexual behavior among young women have been associated with lower initiation and completion of the vaccine schedule, while higher education has been associated with increased uptake [7-12]. Likewise, studies that have examined the associations with woman's age, have reported higher completion rates among younger as well as older women [7,10,12,13]. Furthermore, Widdice et al. reported that women who regularly visited health-care facility for administration of Depot medroxyprogesterone acetate (DMPA), an injectable hormonal contraceptive that is administered every three months, had 53% increased likelihood of vaccine completion during the study period [10]. However, in another study by Patel et al., repeated vaccine reminders to women were not successful in increasing completion rates [9]. Along with these barriers, most previous studies have cited financial restraint as a possible hindrance [14-16]. This barrier was reported to be important for uptake, as well as provision of the vaccine. High price of the vaccine, lack of insurance and inadequate insurance reimbursement were some of the concerns reported by low-income individuals and families [14], while health-care providers acknowledged financial burden to hinder them from recommending the vaccine to economically poor patients [15]. Although most of these studies have regarded cost as a perceived barrier for vaccine initiation and completion, few have assessed the effect of its removal.
The main objectives of our study were, to examine HPV vaccine completion after initiation in a setting where the vaccine was offered free of cost, and to determine socio-demographic (race/ethnicity, age and insurance status) and medical (contraceptive use, recent STIs, parity and visit type) factors associated with vaccine completion.
Methods
This retrospective study was conducted at Family Planning Clinic of John H. Stroger, Jr. Hospital in Chicago, Illinois, an urban, public training hospital, which serves Chicago's underserved and uninsured population, who primarily identify as low-income, Non-Hispanic Blacks. Women ages 14-26 years, who visited the clinic for symptomatic or preventive treatment, during January 2010-December 2012, were offered HPV vaccine (Gardasil quadrivalent) free of cost. In accordance with the Illinois law on minors seeking clinical management for sexually transmitted infections (STI), teenage women were exempt from parental approval for vaccination [17]. The Centers for Disease Control and Prevention's (CDC) HPV vaccine information statement outlines information pertaining to HPV infection and the importance of HPV vaccination, including details on the vaccination schedule and potential side effects [18]. A printed copy of this statement was provided to women at the time of vaccination. Those who received their first dose of HPV vaccine at the clinic, during January 2010-December 2012, were thus included in this study. Information related to socio-demographic and medical factors was extracted from electronic medical records of the women. This study was approved by the Cook County Health and Hospitals System Institutional Review Board.
The outcome of interest was receipt of all three doses of the vaccine series, after initiation of the first dose. Vaccination is recommended at zero, two, and six months, with one month leeway for the second and third doses. Apart from the CDC's vaccine information statement, which describes the vaccination schedule, no formal reminders were given to the women for subsequent vaccine doses. Women were thus followed until May 2014 for completion, given for potential completion time interval of 1.5 to 4.5 years. We examined several factors that have been associated with HPV vaccine uptake in previous studies, such as age, race/ethnicity, socio-economic status, contraceptive use, previous STIs or pregnancies and type of clinical services sought [7,10,12,19,20].
Patients' age at first visit was calculated from date of birth and the date of visit. Women were then grouped into four categories: 14-19 years, 20-22 years, 23-24 years and 25-26 years. Thus, teens were segregated from young women to assist in examining if there was a significant difference in vaccine uptake between teens and within narrow age ranges of young women. Women were categorized first by Hispanic and non-Hispanic, based on self-reported ethnicity, and then further categorized as Black, White or Others (Asian, Native Hawaiian, Pacific Islander, American Indian, Alaska Native), based on self-reported race. Data for our study was obtained from electronic medical records and hence we did not have information on income, which is considered a direct measure of socio-economic status [21]. However, since insurance type is correlated with an individual's income, we used women's insurance status (self-pay, private and public) as a proxy measure of socio-economic status [21]. Although insurance status may not fully capture the effect of socio-economic status of the women in our study, it has been considered as a valid measure in previous studies [10,12].
Women were stratified by method of contraception used according to World Health Organization recommended tiers: women using implants, intrauterine devices (IUDs) or permanent methods of sterilization were placed in tier 1; women using injectable, pills or patches in tier 2; women using barrier methods in tier 3. At each visit when the vaccine was administered, woman's primary reason to visit the clinic was recorded. In addition to vaccination, women visited the clinic for pregnancy tests, contraceptive management, STI screening etc. We thus analyzed primary intent to visit the clinic at first vaccination as 4 variables: ‘condition-oriented' if women sought medical help for pregnancy tests, procedures like colposcopy or post procedural follow-ups; ‘contraceptive' when intent of visit was any kind of contraceptive management; ‘preventive' when women sought STI, HIV or annual cervical cancer screenings; ‘immunization' when intent was only HPV vaccination. History of STI and number of pregnancies in the year prior to the first dose were also included in the analysis.
Statistical analysis was carried out using SAS v9.3 (SAS Institute, Cary, NC). Completion rates were expressed as percentage of the full sample, as it comprised all the women who had taken the first dose. Log-binomial models were fitted and all associations expressed as Relative Risks with significance level of 0.05.
Results
In this study, 201 women initiated HPV vaccination during the study period. Characteristics of the women are shown in table 1. Approximately 68% of women were Non-Hispanic Blacks, while 17% were Hispanics. The average age of women was 22 years (SD: 2.8 years). Most women had no insurance or were self-payers (64%), did not have a history of STI in the previous year (84%) and had never been pregnant (70%). For contraceptive use in the previous year, there were 61% women who used tier 2 methods, 24% who used tier 3 methods and 15% who used tier 1 methods. Around 41% of women sought clinical care for contraceptive management; 28% of women sought condition-oriented care; 19% women came for annual pap smears, HIV or STI screening; while 12% reported HPV vaccination to be the primary reason of visit.
![]()
Table 1: Descriptive characteristics of women ages 14-26 years who received human papillomavirus vaccine from 2010-2012 (n = 201).
View Table 1
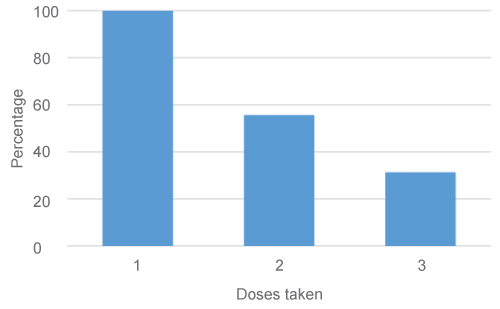
Of the 201 women, 31% successfully completed all three doses of HPV vaccine, while 56% took at least 2 doses during the study period (Figure 1). The median time interval between first and second or third vaccine doses was approximately 63 days (2 months) and 196 days (6.5 months), respectively (data not shown).
.
Figure 1: Incidence of completion of 3 doses of human papillomavirus vaccine in women ages 14-26 years from 2010-2012 (N = 201).
View Figure 1
In bivariate analysis, Hispanic women were 1.61 (95% CI: 1.03-2.53) times more likely to complete the vaccine series compared with Non-Hispanic Blacks (Table 2). Similarly, older women (25-26 years) had higher chances of completion compared with teens (14-19 years) (RR: 2.39; 95% CI: 1.14-5.01). None of the remaining variables proved significant predictors of vaccine completion in our study.
![]()
Table 2: Incidence and relative risk for vaccine completion for women ages 14-26 years who received human papillomavirus vaccine from 2010-2012 (n = 201).
View Table 2
In multivariable analysis, race/ethnicity and age remained significant factors for vaccine completion. After adjusting for age, Hispanic women were found to be 1.55 times more likely to be completers (95% CI: 1.00-2.41), compared with Non-Hispanic Black women. Similarly, when race/ethnicity was adjusted, older women (25-26 years) were more likely to be completers as compared with teens (14-19 years) (RR: 2.45; 95% CI: 1.17-5.11) (Table 3).
![]()
Table 3: Adjusted relative risk for vaccine completion for women ages 14-26 years who received human papillomavirus vaccine from 2010-2012, using log binomial model (n = 201).
View Table 3
Discussion
Previous studies have raised concerns about cost being an important predictor for successful HPV vaccine completion [11,14-16]. We tested the hypothesis that, without this cost barrier, completion rates would increase above those reported previously. However, in our setting, the findings did not demonstrate any increase. This review showed that half of the women in the study received up to two doses and one-third successfully completed the vaccine series. Similar completion rates have been reported previously, irrespective of the financial settings under which the vaccine was provided [7,10,13]. Although our results cannot be directly compared to those reported by NIS or other studies on vaccine completion, due to differences in study populations, yet our study demonstrated that even at low cost vaccine completion rates remained far from ideal. Women should however be made aware of Vaccine for Children program (VFC), whereby less than 19 year old, uninsured children are provided all vaccines, including HPV vaccine, free of cost, and the Affordable Care Act (ACA), whereby underinsured women can receive HPV vaccines for free (Henry et al., 2016; Walker et al., 2014). Further research is however needed, to determine reasons for lower completion and measures or incentives for increased participation, among young women.
Vaccine completion rates were reported to vary with health care departments, with higher completion rates in pediatrics and lower in family medicine and gynecology [7,20,22]. Health-care provider's attitudes towards vaccination and provider-patient comfort level were cited as the main reasons for these variations [7]. Thus, lower rates observed in our study may be a result of restrictive inclusion of women from a certain clinic. While some young women may not have established relationships with a health-care system, any time a young woman visits a health-care system should be considered as an opportunity to ensure vaccine initiation and completion. While reminders to patients have not been successful in increasing completion, reminders to the health-care provider may be more effective in preventing missed opportunities (Patel et al., 2014).
In multivariable model, only race/ethnicity and age remained significant, with Hispanic and older women being more likely candidates for completion. Age is a particular factor of interest in HPV studies: while some studies have reported higher completion rates among young adolescent women [7,13,19], others have reported higher rates among older women [10]. Our observation of older age being a significant predictor is thus consistent with other studies. This association could be possibly explained by increased vaccine awareness and initiation among older women, with higher initiation leading to higher completion [23]. Previous studies have also suggested that strong provider recommendation increases vaccine uptake at a particular age, and that providers were more likely to recommend vaccine to older individuals [7,24,25]. However, since we did not examine reasons for failure to complete the vaccine series, we could not determine if the age-related differences in vaccine uptake were due to factors related to woman's awareness/compliance (unaware of parental exemption for vaccine acceptance, limited knowledge about HPV and HPV vaccine, lower risk perception for STIs, cultural beliefs and distrust of health-care system or did not remember to take all three doses) or due to factors related to health-care system or provider (inability to completely address woman's concerns, preference for vaccinating older women or failure to provide vaccine doses at subsequent visits) [11].
In our study, Hispanic women were more likely than Non-Hispanic Blacks to have completed the series. Previous studies which examined the effect of race/ethnicity among urban or nationally representative sample of women have reported inconsistent results: some have reported completion to be lower among Hispanics [26,27], other reported almost no association with race/ethnicity [23], while one reported the association to vary with age among Hispanics [7]. However, these trends have been changing over time: recent studies on HPV vaccination have reported higher initiation (69%) and completion (47%) among Hispanic women, compared with women of any other race/ethnicity (for completion: Non-Hispanic black: 39%; Non-Hispanic White: 38%; Multi-racial: 37%) [5,28]. Hispanic women have high rates of cervical cancer incidence and mortality, however, previous studies have reported knowledge related to cervical cancer and HPV to be exceptionally low in this group [29,30]. Thus increased efforts were made to raise awareness regarding HPV infection and vaccines, in this ethnic minority group [30]. Increased awareness among Hispanic women may thus explain the association with race/ethnicity found in our study [31]. Furthermore, as compared with other races/ethnic groups, Hispanics were reported to have higher uptake for most childhood vaccines. Thus, increased willingness for vaccination, including HPV vaccine, increased social or familial support and increased trust in health-care providers and vaccination programs may further explain our results of increased vaccine completion in this group [28,32-34].
We hypothesized that certain conditions, which might warrant repeat clinic visits or follow-up, such as contraceptive replenishment, STI management, pre-natal visits and immunization requests, would increase the likelihood of vaccine completion. However, these factors did not change the completion rates. Chao et al. describe how history of recent STI is associated with increased willingness for vaccination, however, we found no difference, suggesting that the concern of acquiring HPV was not affected by recent STI [7]. Given that women who made more frequent visits to the hospital would have more opportunities of receiving the vaccine, we were surprised to find lack of difference between visit types, especially since we included both preventive and HPV vaccine focused visits [10]. We also observed that significantly small proportion of women visited the clinic for the purpose of vaccination, suggesting that primary prevention was not the focus among women in our study.
In order to circumvent some of the barriers associated with poor completion rates of HPV vaccine, such as number of doses and cost, suggestions for varying the dosing schedule or providing fewer than three doses have been recommended [35,36]. Kreimer et al. examined vaccine efficacy for reduced doses, in 18-25 year old women, nested in a phase 3 randomized clinical trial, in Costa Rica [37]. They reported that one and two doses of the vaccine were as protective as three doses, even after four years of vaccination [37]. However, in another randomized, phase 3 study conducted among Canadian women receiving quadrivalent HPV vaccine, immunogenicity was found to remain same for both three and two dose recipients one month after vaccination, but decreased for some HPV genotype 2-3 years after vaccination in the two dose recipients [35]. In addition, the immunogenicity was considerably better in adolescent girls than in young women [35]. The authors thus recommend that there is need for more evidence on immunogenicity and vaccine efficacy before presuming clinically significant difference and accepting reduced dose schedule [35].
A strength of our study is that the data was derived from electronic medical records and vaccine uptake was documented in the charts, and therefore our study was not prone to recall errors. We looked at urban minority women who are at increased risk of HPV infection and cervical cancers [1]. This study's results should be interpreted in context of its limitations. The foremost being that patients from a single clinic were recruited in this study. This could have led to a lower completion due to selection bias, as such women were more likely to be offered the vaccine while they were seeking care for STIs and contraception. No information on vaccine completion performed outside the study site was available, which may have lowered our estimates and biased our final findings.
Conclusion
Our study further delineates the lack of completion of the HPV vaccine series when initiated. While cost has often been perceived as a barrier to completion, our study demonstrates that even when cost is eliminated, vaccine completion rates do not improve. Given the completion rates of approximately 31%, seen in our study and across the country under different settings and scenarios, in order to reach 80% completion goal of Health People 2020 [38], more active interventions towards HPV vaccination must be adopted.
Conflict of Interest
All authors report no personal, political, commercial, financial, or academic conflicts of interest. All authors have approved the final article.
Funding Source
None.
References
-
http://www.cdc.gov/std/stats/sti-estimates-fact-sheet-feb-2013.pdf.
-
(2014) Genital HPV Infection - CDC Fact Sheet. CDC.
-
Molano M, Van den Brule A, Plummer M, Weiderpass E, Posso H, et al. (2003) Determinants of clearance of human papillomavirus infections in Colombian women with normal cytology: a population-based, 5-year follow-up study. Am J Epidemiol 158: 486-494.
-
Crowe E, Pandeya N, Brotherton JM, Dobson AJ, Kisely S, et al. (2014) Effectiveness of quadrivalent human papillomavirus vaccine for the prevention of cervical abnormalities: case-control study nested within a population based screening programme in Australia. BMJ 348: g1458.
-
Reagan-Steiner S, Yankey D, Jeyarajah J, Elam-Evans LD, Singleton JA, et al. (2015) National, Regional, State, and Selected Local Area Vaccination Coverage Among Adolescents Aged 13-17 Years--United States, 2014. Morbidity and mortality weekly report 64: 784-792.
-
Lu PJ, Yankey D, Jeyarajah J, O'Halloran A, Elam-Evans L, et al. (2015) Hepatitis B vaccination among adolescents 13-17 years, United States, 2006-2012. Vaccine 33: 1855-1864.
-
Chao C, Velicer C, Slezak JM, Jacobsen SJ (2009) Correlates for completion of 3-dose regimen of HPV vaccine in female members of a managed care organization. Mayo Clin Proc 84: 864-870.
-
Dempsey A, Cohn L, Dalton V, Ruffin M (2011) Worsening disparities in HPV vaccine utilization among 19-26 year old women. Vaccine 29: 528-534.
-
Patel A, Stern L, Unger Z, Debevec E, Roston A, et al. (2014) Staying on track: a cluster randomized controlled trial of automated reminders aimed at increasing human papillomavirus vaccine completion. Vaccine 32: 2428-2433.
-
Widdice LE, Bernstein DI, Leonard AC, Marsolo KA, Kahn JA (2011) Adherence to the HPV vaccine dosing intervals and factors associated with completion of 3 doses. Pediatrics 127: 77-84.
-
Holman DM, Benard V, Roland KB, Watson M, Liddon N, et al. (2014) Barriers to human papillomavirus vaccination among US adolescents: a systematic review of the literature. JAMA pediatrics 168: 76-82.
-
Schluterman NH, Terplan M, Lydecker AD, Tracy JK (2011) Human papillomavirus (HPV) vaccine uptake and completion at an urban hospital. Vaccine 29: 3767-3772.
-
Shen-Gunther J, Shank JJ, Ta V (2011) Gardasil HPV vaccination: surveillance of vaccine usage and adherence in a military population. Gynecol Oncol 123: 272-277.
-
Sanders Thompson VL, Arnold LD, Notaro SR (2012) African American parents' HPV vaccination intent and concerns. J Health Care Poor Underserved 23: 290-301.
-
Ferrer HB, Trotter C, Hickman M, Audrey S (2014) Barriers and facilitators to HPV vaccination of young women in high-income countries: a qualitative systematic review and evidence synthesis. BMC public health 14: 700.
-
Kester LM, Zimet GD, Fortenberry JD, Kahn JA, Shew ML (2013) A national study of HPV vaccination of adolescent girls: rates, predictors, and reasons for non-vaccination. Matern Child Health J 17: 879-885.
-
http://www.cico-il.org/legislation/childrens_health.html.
-
(2013) HPV vaccine- What you need to know. CDC.
-
Cook RL, Zhang J, Mullins J, Kauf T, Brumback B, et al. (2010) Factors associated with initiation and completion of human papillomavirus vaccine series among young women enrolled in Medicaid. J Adolesc Health 47: 596-599.
-
Rubin RF, Kuttab HM, Rihani RS, Reutzel TJ (2012) Patient adherence to three dose completion of the quadrivalent human papillomavirus (HPV) vaccine in a private practice. J Community Health 37: 1145-1150.
-
Shavers VL (2007) Measurement of socioeconomic status in health disparities research. J Natl Med Assoc 99: 1013-1023.
-
Vadaparampil ST, Staras SA, Malo TL, Eddleton KZ, Christie J, et al. (2013) Provider factors associated with disparities in human papillomavirus vaccination among low-income 9- to 17-year-old girls. Cancer 119: 621-628.
-
Dorell CG, Yankey D, Santibanez TA, Markowitz LE (2011) Human papillomavirus vaccination series initiation and completion, 2008-2009. Pediatrics 128: 830-839.
-
Vadaparampil ST, Kahn JA, Salmon D, Lee JH, Quinn GP, et al. (2011) Missed clinical opportunities: provider recommendations for HPV vaccination for 11-12 year old girls are limited. Vaccine 29: 8634-8641.
-
Pierre Joseph N, Clark JA, Mercilus G, Wilbur M, Figaro J, et al. (2014) Racial and ethnic differences in HPV knowledge, attitudes, and vaccination rates among low-income African-American, Haitian, Latina, and Caucasian young adult women. J Pediatr Adolesc Gynecol 27: 83-92.
-
Niccolai LM, Mehta NR, Hadler JL (2011) Racial/Ethnic and poverty disparities in human papillomavirus vaccination completion. Am J Prev Med 41: 428-433.
-
Schmidt S, Parsons HM (2014) Vaccination interest and trends in human papillomavirus vaccine uptake in young adult women aged 18 to 26 years in the United States: an analysis using the 2008-2012 National Health Interview Survey. Am J Public Health 104: 946-953.
-
Henry KA, Stroup AM, Warner EL, Kepka D (2016) Geographic Factors and Human Papillomavirus (HPV) Vaccination Initiation among Adolescent Girls in the United States. Cancer Epidemiol Biomarkers Prev 25: 309-317.
-
(2015) Cervical Cancer Rates by Race and Ethnicity. CDC.
-
Vanslyke JG, Baum J, Plaza V, Otero M, Wheeler C, et al. (2008) HPV and cervical cancer testing and prevention: knowledge, beliefs, and attitudes among Hispanic women. Qual Health Res 18: 584-596.
-
Kobetz E, Kornfeld J, Vanderpool RC, Finney Rutten LJ, Parekh N, et al. (2010) Knowledge of HPV among United States Hispanic women: opportunities and challenges for cancer prevention. J Health Commun 15: 22-29.
-
Kornfeld J, Byrne MM, Vanderpool R, Shin S, Kobetz E (2013) HPV knowledge and vaccine acceptability among Hispanic fathers. J Prim Prev 34: 59-69.
-
Elam-Evans LD, Yankey D, Singleton JA, Kolasa M (2014) National, state, and selected local area vaccination coverage among children aged 19-35 months - United States, 2013. Morbidity and mortality weekly report 63: 741-748.
-
Kepka DL, Coronado GD, Rodriguez HP, Thompson B (2012) Development of a radionovela to promote HPV vaccine awareness and knowledge among Latino parents. Public Health Rep 127: 130-138.
-
Dobson SR, McNeil S, Dionne M, Dawar M, Ogilvie G, et al. (2013) Immunogenicity of 2 doses of HPV vaccine in younger adolescents vs 3 doses in young women: a randomized clinical trial. Jama 309: 1793-1802.
-
Neuzil KM, Canh do G, Thiem VD, Janmohamed A, Huong VM, et al. (2011) Immunogenicity and reactogenicity of alternative schedules of HPV vaccine in Vietnam: a cluster randomized noninferiority trial. Jama 305: 1424-1431.
-
Kreimer AR, Rodriguez AC, Hildesheim A, Rolando H, Carolina P, et al. (2011) Proof-of-Principle Evaluation of the Efficacy of Fewer Than Three Doses of a Bivalent HPV16/18 Vaccine. Journal of the National Cancer Institute 103: 1444-1451.
-
http://www.cdc.gov/mmwr/preview/mmwrhtml/rr5602a1.htm.





