International Journal of Women's Health and Wellness
Breastfeeding at Hospital Discharge among High Risk Obstetrical Patients
Leandro Cordero1*, Amneet Bajwa2, Mona R Prasad3, Reena Oza-Frank2, Mark B Landon3 and Craig A Nankervis2
1Department of Pediatrics and Obstetrics, The Ohio State University, USA
2Department of Pediatrics, The Ohio State University, USA
3Department of Obstetrics and Gynecology, The Ohio State University, USA
*Corresponding author:
Leandro Cordero, Professor Emeritus, Department of Pediatrics and Obstetrics, The Ohio State University Medical Center, N118 Doan Hall 410 W. 10th Avenue Columbus, Ohio 43210-1228, USA, Tel: 614-293-8660, Fax: 614-293-7676, E-mail: Leandro.cordero@osumc.edu
Int J Womens Health Wellness, IJWHW-2-031, (Volume 2, Issue 3), Research Article; ISSN: 2474-1353
Received: July 08, 2016 | Accepted: August 20, 2016 | Published: August 23, 2016
Citation: Cordero L, Bajwa A, Prasad MR, Oza-Frank R, Landon MB, et al. (2016) Breastfeeding at Hospital Discharge among High Risk Obstetrical Patients. Int J Womens Health Wellness 2:031. 10.23937/2474-1353/1510031
Copyright: © 2016 Cordero L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: In the United States, at the time of discharge from the hospital, approximately 79% of the general maternal population started breastfeeding their infants. Less is known about breastfeeding among women with diverse high risk obstetrical (HROB) conditions, a group at high risk for low breastfeeding rates.
Objective: To determine infant feeding preference and breastfeeding at the time of hospital discharge among HROB women who attended prenatal subspecialty clinics and delivered during 2012-2014.
Design/Methods: A total of 308 HROB women included 112 with diabetes (DM), 80 who were treated for substance abuse (SA), 75 with miscellaneous (MISC) high risk conditions (i.e., chronic hypertension, extreme non-diabetic obesity, etc.) and 41 with a history of preterm labor or preterm delivery (PTL). Infant feeding preference was ascertained prenatally. At the time of discharge, breastfeeding was considered started if feedings were exclusive (100%), partial (50%-74%) or predominantly (≥ 75%) of maternal milk.
Results: Preference to breastfeed by HROB group was 79% DM, 71% SA, 71% MISC, and 78% PTL. Breastfeeding was observed in 42% DM, 50% SA, 44% MISC, and 44% PTL. There were 228 multiparous, of them 116 (51%) had prior breastfeeding experience, however, only 67 (57%) started breastfeeding.
Conclusions: In spite of the heterogeneity of their morbidities women with HROB conditions intended to breastfeed at a rate similar to that of the general population. However, breastfeeding rates among women with diverse HROB conditions including those with prior experience are low and may require specific educational strategies in order to improve outcomes.
Background
Breastfeeding is beneficial to the health and well-being of mothers and their infants [1,2]. In 2011, approximately 79% of the general maternal population in the U.S. started breastfeeding by the time of discharge from the hospital [3]. Breastfeeding in these low risk obstetrical women has been extensively reviewed in the literature [3-5]. In addition to traditionally recognized barriers to breastfeeding, maternal morbidities such as diabetes, substance abuse, pre-term labor and other high risk obstetrical (HROB) conditions may also interfere with or delay breastfeeding [1-5]. Recently, we reported breastfeeding rates by the time of hospital discharge of 76% in women with severe preeclampsia [6], 54% in women with gestational diabetes mellitus (GDM) [7], 55% in women with pre-gestational diabetes mellitus (PGDM) [8] and 56% in extremely obese non-diabetic women [9]. Breastfeeding rates at the time of discharge ranging from 24% to 50% have been reported among women whose infants developed neonatal abstinence syndrome (NAS) [10,11]. In spite of supportive hospital practices, exclusive breastfeeding at one week postpartum was lower among women with medically complex pregnancies who intended to breastfeed [12] Intention to breastfeed is a strong predictor of breastfeeding initiation even among women with HROB conditions [6-9]. However, there is a significant discordance between intention to breastfeed and breastfeeding during the postpartum period [6-9,13]. Hundalani, et al. [13] characterized the discordance between intention and actual breastfeeding as a missed opportunity for targeted intervention. In spite of the above, scarce and conflictive information is available on breastfeeding by the time of hospital discharge among women with HROB conditions.
Objective
To examine breastfeeding intention and actual breastfeeding at the time of hospital discharge in women with diverse HROB conditions.
Subject and methods
Our study population consisted of 308 women with HROB conditions who were consecutively enrolled in prenatal subspecialty clinics and delivered infants during 2012-2014. In our institution, prenatal care to HROB women is provided at subspecialty clinics: diabetes mellitus (DM), antepartum treatment for substance abuse (SA), miscellaneous (MISC) high risk conditions and women with a history of preterm labor or preterm delivery (PTL).
This retrospective chart review was approved by the Institutional Review Board of the Wexner Medical Center at The Ohio State University. Hard copies and electronic medical records were reviewed and in compliance with our guidelines, all information was coded and de-identified. Pregnancies delivered at ≥ 34 weeks of gestation and not affected by major fetal malformations were included. Pre-pregnant body mass index (BMI, Kg/m2) was defined as normal (18.5-24.9), overweight (25-29.9), obese (30-34.9), very obese (35-39.9) and extremely obese (≥ 40). Upon arrival to the subspecialty clinics, all women declare their infant feeding preference and received verbal and written information about the benefits of breastfeeding for them and their infants from the perinatal team (doctors, nurses, nutritionist and social worker). Lactation consultations prenatally were by referral, while postpartum consultations were universally offered. For the purpose of this study, infant feeding preference declared on arrival to labor and delivery was used. Women with a history of opioid dependence currently enrolled in a treatment program (buprenorphine/naloxone or methadone) and free of human immunodeficiency virus were encouraged to breastfeed if they also complied with the Academy of Breastfeeding Medicine (ABM) guidelines [14].
In our institution, supportive hospital practices which encourage breastfeeding are similar to those described by Kozhimannil, et al. [12] and include antenatal, labor and delivery, and post-partum nursing care and interaction with lactation consultants. Depending on the condition of the mother and her infant at the time of delivery, maternal-infant interactions (holding, skin to skin contact, breastfeeding) were encouraged. Per our institutional guidelines, asymptomatic infants born to HROB mothers were transferred to the well baby nursery (WBN). Symptomatic infants (i.e., respiratory distress (RDS), hypoglycemia, birth asphyxia) were transferred directly from the delivery room to the NICU.
Infants at risk of hypoglycemia (blood glucose < 40 mg/dl) were screened via serial point of care testing (Accu-Chek®) starting at the first hour of life and prior to the first feeding [6-9]. Infants in the WBN with hypoglycemia were breastfed or given formula. Those with repeated low blood glucose values were treated with IV dextrose (4-6 mg/Kg/min).
After delivery, at risk neonates were evaluated for NAS by a trained neonatal nursing staff using a modified Finnegan scale [11]. Pharmacologic treatment with methadone was initiated if three scores ≥ 8 or 2 scores ≥ 12 were observed over a 24-hour period [11].
As documented in the medical record, breastfeeding was defined as started if at the time of discharge, the infant was exclusively (100%), partially (50-74%) or predominantly (≥ 75%) breastfed [15]. Due to the retrospective study design, no follow-up information was available on infant feeding practices beyond hospital discharge.
Statistical Analysis
Comparisons between groups and subgroups of patients were made with one way ANOVA or Kruskal-Wallis tests for continuous variables and chi-square or Fisher's exact tests for categorical variables. Multivariable logistic regression was used to ascertain the strength of association of maternal variables (race, parity, BMI, smoking, mode of delivery, breastfeeding preference and prior experience) and neonatal variables (gestational age, birth weight and admission to the NICU) with breastfeeding by the time of discharge; variable selection for final multivariable models was based on backward stepwise selection with an entry criterion of p < 0.1 and an exit criterion of p > 0.1. Significance was established at a two-sided p value < 0.05.
Results
Diabetes mellitus
There were 66 women diagnosed with GDM; 34 were treated with diet modification and 32 were treated with Glyburide® (28) or insulin (4). There were 46 women diagnosed with PGDM (22 class B, 5 type 2 DM and 19 classes C-F). Four of the 46 women with PGDM were treated with diet modifications, 4 with Glyburide®, 3 with Metformin® and 35 with insulin. Eighty-five of the 112 (76%) women with DM had hemoglobin A1C drawn prior to delivery (median 5.9%, range 4.6-12.5%). Besides DM, these patients had additional comorbidities including chronic hypertension (23), preeclampsia (7), obesity (22) and extreme obesity (36). Three patients had hepatitis B, one hepatitis C and four had herpes simplex virus (HSV).
Substance abuse treatment
This group was composed of women who initiated and maintained antepartum treatment for opiate abuse. Seventy-one of the 80 (89%) were treated with Suboxone®, 6 with Buprenorphine® and 3 with methadone. All women had urine toxicology done at the time of delivery; all samples were positive for the prescribed substance, while 4 (5%) were also positive for opiates. Besides the history of substance abuse, 29 of the 80 (36%) had hepatitis C. Six (8%) women had HSV infections and one (1%) had a history of syphilis. Other comorbidities included psychiatric diagnosis (16), gestational or chronic hypertension (8) and obesity (4) or extreme obesity (5).
Miscellaneous HROB conditions
Twenty-nine (39%) of the 75 women cared for at this clinic were teenagers (14 ≤ 16 years and 15 ≥ 17 years). Age alone was the HROB factor for 8 (31%) of the 29 teenagers, whereas 21 teenagers had comorbidities that included scoliosis (1), psoriasis (1), fractured pelvis (1), cerebral palsy (1), urinary tract infections (2), preeclampsia (2), asthma (4), STD (6) and miscellaneous (3). The remaining 46 women attending the MISC clinic had a variety of HROB conditions including pancreatitis (1), spina bifida (1), hydrocephalus (1), astrocytoma (1), non-Hodgkin's lymphoma (1), fibrosarcoma (1), developmental delay (1), scoliosis (2), epilepsy (3), preeclampsia (2), hyperthyroidism (3), cardiomyopathy (5) psychiatric illnesses (5), STD (7), chronic hypertension (8), obesity (6), extreme obesity (13) and miscellaneous (7).
History of preterm labor or preterm delivery
The admission criterion for this subspecialty clinic for these 41 multiparous patients was a history of preterm labor or preterm delivery. Their reproductive history comprised of 174 pregnancies that resulted in 43 (24%) term, 62 (36%) preterm deliveries, 69 (40%) abortions and 105 (60%) live children. In addition to the history of preterm labor or preterm delivery, this group of 41 patients presented with other comorbidities that included cardiomyopathy (1), uterine malformations (3), scoliosis (3), preeclampsia (4), asthma (4), sexually transmitted disease (4), obesity (4), extreme obesity (7) and various psychiatric illnesses (14).
Demographic and clinical information for all HROB women are presented in table 1. Most variables, except intention to breastfeed, differed significantly among HROB groups. Women in the MISC group were younger on average than those in the other groups. Women in the SA group were mainly white, while those in the PTL and DM group were mostly African American. Obesity was more common among women with DM and less common among those in the SA group. Approximately 75% of the women in the DM, SA and MISC groups and all women in the PTL (by definition) were multiparous. Smoking and history of perinatal infections was significantly higher among women in the SA group. Mode of delivery was also different between the groups as cesarean deliveries ranged from 55% among women with DM to 28% for those in the MISC group. Indications for primary cesarean deliveries were similar across the groups and included failure of labor to progress, breech presentation, suspected macrosomia, and fetal distress. First mother-infant contact occurred significantly earlier following vaginal delivery (median 1, range 0.3-87 hrs) than following cesarean delivery (median 6, range 0.3-96 hrs, p < 0.01). Women with a history of PTL were more likely to have contact with their infants during the first 90 minutes than women with DM (71% vs. 46% respectively, p 0.006).
![]()
Table 1: Maternal demographic and clinical information for women with high risk obstetrical conditions.
View Table 1
Neonatal outcomes
Clinical data for the 308 infants born during the study period according to their mothers HROB conditions are presented in table 2. Of the 308 infants, 271 (87%) were born at term while the remaining 37 (13%) infants were born at 34 weeks (4), 35 weeks (13), or 36 weeks (20) GA. One minute Apgar score ≤ 5 affected 24 of 308 (8%) infants and persistent low APGAR scores at 5 minutes was observed in only 2 infants. Low and normal Apgar scores were evenly distributed among all HROB groups. Two hundred and fifty-four of 308 infants (82%) were transferred from the delivery room to the WBN, while 54 (18%) were admitted directly to the NICU. Of the 112 infants born to women with DM, 28 (25%) were admitted directly to the NICU. The most common admission diagnosis was hypoglycemia (11) followed by RDS (10). Fourteen of the 80 SA (18%), 10 of the 75 MISC (13%) and 2 of the 41 PTL (5%) were also admitted to the NICU with various diagnoses.
![]()
Table 2: Neonatal outcomes of infants born to women with high risk obstetrical conditions.
View Table 2
Thirty (38%) of the 80 infants from the SA group developed NAS. Twenty-three (77%) of the 30 infants who developed NAS were treated at the WBN, while the remaining 7 (33%) required admission to the NICU. The percentage of mothers and infants discharged home together were: 86% of the DM, 14% of the SA, 90% of the MISC and 90% of the PTL group. All mothers and infants were discharged home in good health.
Intention to breastfeed
Intention to breastfeed was similar among the groups and was declared by 79% of the women in the DM group (74% for GDM and 87% for PGDM), 71% in the SA group, 71% in the MISC group and 78% in the PTL group (Table 1 and Figure 1). Among women in the MISC group, 32 of the 46 (70%) non-teenagers and 22 of the 29 (76%) teenagers declared intention to breastfeed.
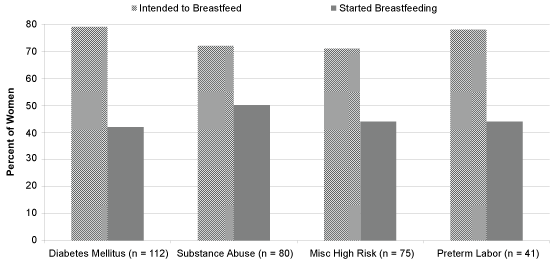
.
Figure 1: Percent of women in each High Risk Obstetrical group who intended to breastfed and those within each group who breastfeed by the time of discharge from the hospital.
View Figure 1
Before the current pregnancy, 116 of the 228 (51%) multiparous women had breastfed at least one of their 258 live infants (Table 3). On arrival to labor and delivery, 103 of these 116 (89%) women intended to breastfeed at a rate similar to the 80 (84%) primiparous women from all HROB groups. In contrast, 112 multiparous women without breastfeeding experience had the lowest rate of intention to breastfeed (54%). Regression analysis controlling for living children, race, and use of a lactation consultant confirmed that multiparous women with prior experience were more likely to intend to breastfeed than multiparous women without prior experience (Table 3).
![]()
Table 3: Adjusted effects on intention to breastfeed for all high risk obstetrical patients.
View Table 3
Breastfeeding at the time of discharge
At the time of discharge from the hospital, 138 of the 308 (45%) infants were breastfeeding. Fifty-one of them (37%) were exclusively breastfeeding, while the remaining 87 (63%) were partially or predominantly breastfeeding. As shown in table 2 and figure 1, breastfeeding was similar among all groups: 42% in the DM group, 50% in the SA group, and 44% in the MISC and PTL groups. Sixteen of the 29 (55%) teenagers and 17 of the 46 (37%) non-teenagers in the MISC group were breastfeeding.
Combining all 308 infants from the four HROB groups by GA there were 271 term and 37 late preterm infants. One hundred twenty-seven of 271 term (47%) and 11 of 37 (30%) late preterm infants were breastfeeding at discharge (p 0.05, data not shown). Women with infants in the WBN were more likely to breastfeed than those whose infants were admitted to the NICU (OR 2.8, CI 1.3-6.0, p 0.007). Furthermore, the odds of breastfeeding were higher for those women who received lactation consultation (Table 4).
![]()
Table 4: Predictors of breastfeeding at discharge for all high risk obstetrical patients.
View Table 4
Breastfeeding by parity, previous experience and intention
One hundred sixteen (51%) of the 228 multiparous women had prior experience and of them, 103 (89%) intended to breastfeed. Only 67 (65%) of the 103 were breastfeeding at the time of discharge.
One hundred twelve of the 228 (49%) multiparous women had no previous experience with breastfeeding. Sixty-one of the 112 (54%) intended to breastfeed, however, only 31 (51%) of them breastfed by discharge. Sixty-six of the 80 (83%) primiparous women intended to breastfeed, while only 39 (59%) of them were breastfeeding at discharge. Regression analysis showed that the odds of breastfeeding were higher for women with prior experience (Table 4).
Discussion
In spite of the heterogeneity of morbidities and co-morbidities associated with HROB pregnancies, intention to breastfeed was similar to that of the general population. Breastfeeding rates at the time of discharge, however, remain disappointingly low [6-9].
Traditionally recognized barriers to breastfeeding such as lack of supportive hospital practices, lack of intention, maternal complications of labor and delivery, mode of delivery, prolonged mother-infant separation and infant morbidities may affect all HROB groups [5,12]. Recognition of the unique barriers to breastfeeding affecting each of the HROB groups during the postpartum period may lead to specific educational strategies to improve outcomes.
Breastfeeding rates among women with GDM lags behind that of the general population [7,16]. Women with PGDM have even lower rates compared to women with GDM and the non-diabetic population [8,16]. Possible explanations for the low rates observed among women with PGDM include the high incidence of obesity [8], cesarean delivery, complications of labor and delivery, need for specialized care of their infants, as well as delayed lactogenesis II [16-18]. It is also conceivable that women with PGDM may have concerns for their own health and may be more sensitive to life disruptions, such as the birth of a healthy or ill newborn [19,20].
Pregnant women undergoing opioid treatment for substance abuse who wish to breastfeed may present a risk not only to themselves, but also to their infants due to possible exposure to drugs, tobacco, alcohol and perinatal infections (i.e., hepatitis B and C, HIV and other sexually transmitted diseases). Despite these risks, their infants stand to benefit significantly from lactation [11,21-23]. A pregnant HIV negative woman in a comprehensive substance abuse treatment program who intends to breastfeed should be encouraged to do so [14]. Compliance should be monitored with serial urine toxicology screens during the antepartum period and at the time of delivery [14,21-23].
The high incidence of NAS often requiring longer hospitalization for the infants and unavoidable mother infant separations presents another major challenge for breastfeeding in this unique group. In our antepartum opioid treatment program, the majority of women received Suboxone®. While the incidence of NAS may not be affected by treatment choice, there is evidence that its severity among infants exposed to Buprenorphine® or Suboxone® is less than those exposed to methadone and that the need for pharmacological treatment may be shorter [11,21-23]. Awareness of these observations may have encouraged women in the SA group to intend to breastfeed. The 50% breastfeeding rate observed among women undergoing substance abuse treatment is comparable to that reported by other investigators [11,21-23].
In the present investigation, 29 of 78 (37%) opioid dependent women in the SA group were hepatitis C virus (HCV) positive. Vertical transmission of HCV occurs in 3-5% of the cases and may be related to mode of delivery or other obstetrical practices [24]. Breastfeeding does not appear to increase the risk of transmission because the amount of HCV in maternal milk and colostrum is very low and is likely inactivated in the infant digestive tract [24,25]. Breastfeeding is not contraindicated in most cases of hepatitis B, however it is not recommended by drug manufacturers during maternal antiviral therapy [25].
In the present study, intention to breastfeed was 70% for 46 older women and 76% for the 29 teenagers who composed the MISC group. A recent publication also from Ohio showed no differences in intention to breastfeed between inner city (mostly African American) teenagers (63%) and their non-teenage (60%) counterparts [26]. The breastfeeding rates at discharge of 55% for teenagers and 37% for older women with HROB conditions are lower than the rates reported for adolescents and for non-adolescents from the general population [27].
It has been reported that breastfeeding ranged from 59-70% in late preterm infants and that breastfeeding is more challenging in late preterm infants than in term infants [28]. Difficulties associated with breastfeeding observed in late preterm infants may be due to developmental immaturities, as well as maternal morbidities directly or indirectly associated with premature birth [28,29].
Regardless of HROB conditions, primiparous and multiparous women without prior experience will intend and start breastfeeding less often than multiparous women with previous experience. This observation characterizes a group of women that deserve special attention and a different educational strategy in order to improve breastfeeding [30]. Of note, approximately one-third of primiparous and multiparous with and without experience who intended to breastfeed failed to start breastfeeding. This discordance between intention to breastfeed and breastfeeding merits further investigation.
Previously we reported that diabetic women and those with preeclampsia were as likely to intend to breastfeed as the general maternal population, but not necessarily more likely to start breastfeeding [6-9]. Our data suggests that the discordance between intention and breastfeeding may also be found among women with other HROB conditions. Of concern is that low breastfeeding rates may also lead to early discontinuation or shorter duration of breastfeeding [9,31-33].
Traditionally, pre and postnatal breastfeeding counseling focused on the benefit to the infant without major emphasis on potential maternal benefits. For example, breastfeeding may prevent long term sequelae of metabolic syndrome, which may be of significant importance to the diabetic population [1,2]. Additionally, breastfeeding can potentially limit postpartum depression and relapse in substance abuse patients due to the impact of oxytocin [34].
It is important to recognize that meaningful comparisons of data between studies is often precluded by vague and inconsistent definitions of breastfeeding initiation [12,13]. Following 1991 WHO recommendations, some investigators use “one feeding of breast milk daily or any attempt to breastfeed before discharge” to categorize an infant as breastfed [9,14]. Others use data collected from birth certificates during the first or second day after delivery [15], from postpartum questionnaires in person, or by mail/phone, often weeks or even months following delivery [35-37]. In order to provide some consistency, for many years we have used a semi-quantitative definition based on feeding behaviors documented in hospital records [6-9].
Limitations of our study are those inherent to retrospective investigations as well as the lack of follow-up information on infant feeding practices beyond hospital discharge and the heterogeneity and size of the different HROB groups. One of the strengths of the investigation is the definition of breastfeeding utilized and the fact that the data was obtained directly from hospital records and not from post-delivery maternal recall. More importantly, regardless of HROB group, parity, prior breastfeeding experience and a variety of morbidities, all women were cared for and delivered at a single institution and had similar infant feeding preferences.
Conclusion
While intention to breastfeed is similar to that of the general maternal population, breastfeeding at discharge from the hospital for women with diverse HROB conditions is disappointingly low. Primiparous and multiparous women without previous breastfeeding experience may require targeted educational effort to improve breastfeeding behavior. Discussion of the benefits of breastfeeding for mothers and infants and lactation support may improve breastfeeding in these and other HROB groups of women.
References
-
Stuebe AM, Schwarz EB (2010) The risks and benefits of infant feeding practices for women and their children. J Perinatol 30: 155-162.
-
Gunderson EP, Hurston SR, Ning X, Lo JC, Crites Y, et al. (2015) Lactation and progression to type 2 diabetes mellitus after gestational diabetes mellitus: A Prospective Cohort Study. Ann Intern Med 163: 889-898.
-
Centers for Disease Control and Prevention. Breast feeding Report Card 2014.
-
(2007) Evidence on the long-term effects of breastfeeding: systematic reviews and meta-analysis. World Health Organization, Geneva, Switzerland, USA.
-
(2011) The Surgeon General's Call to Action to Support Breastfeeding. U.S. Department of Health and Human Services, Office of the Surgeon General, Washington, DC, USA.
-
Cordero L, Valentine C, Samuels P, Giannone PJ, Nankervis CA (2012) Breastfeeding in women with severe preeclampsia. Breastfeed Med 7: 457-463.
-
Cordero L, Gabbe S, Landon MB, Nankervis CA (2013) Breastfeeding initiation in women with gestational diabetes mellitus (GDM). J Matern Fetal Neonat Med 1: 303-310.
-
Cordero L, Thung S, Landon MB, Nankervis CA (2014) Breast-feeding initiation in women with pregestational diabetes mellitus. Clin Pediatr (Phila) 53: 18-25.
-
Cordero L, Oza-Frank R, Landon MB, Nankervis CA (2015) Breastfeeding initiation among macrosomic infants born to obese non-diabetic mothers. Breastfeed Med 10: 239-245.
-
Wachman EM, Byun J, Philipp BL (2010) Breastfeeding rates among mothers of infants with neonatal abstinence syndrome. Breastfeed Med 5: 159-164.
-
Gawronski KM, Prasad MR, Backes DR, Lehman KJ, Gardner DK, et al. (2014) Neonatal Outcomes Following In Utero Exposure to Buprenorphine/Naloxone or Methadone. SAGE Open Medicine 2.
-
Kozhimannil KB, Jou J, Attanasio LB, Joarnt LK, McGovern P (2014) Medically complex pregnancies and early breastfeeding behaviors: a retrospective analysis. PLOS One 9.
-
Hundalani SG, Irigoyen M, Braitman LE, Matam R, Mandakovic-Falconi S (2013) Breastfeeding among inner-city women: from intention before delivery to breastfeeding at hospital discharge. Breastfeed Med 8: 68-72.
-
Reece-Stremtan S, Marinelli KA (2015) ABM Clinical Protocol #21: guidelines for breastfeeding and substance use or substance use disorder, revised 2015. Breastfeed Med 10: 135-141.
-
Labbok MH, Starling A (2012) Definitions of breastfeeding: call for the development and use of consistent definitions in research and peer-reviewed literature. Breastfeed Med 7: 397-402.
-
Oza-Frank R, Chertok I, Bartley A (2014) Differences in breast-feeding initiation and continuation by maternal diabetes status. Public Health Nutr 18: 727-735.
-
Sparud-Lundin C, Wennergren M, Elfvin A, Berg M (2011) Breastfeeding in women with type 1 diabetes. Diabetes Care 34: 296-301.
-
Matias SL, Dewey KG, Quesenberry Jr CP, Gunderson EP (2014) Maternal prepregnancy obesity and insulin treatment during pregnancy are independently associated with delayed lactogenesis in women with recent gestational diabetes mellitus. Am J Clin Nutri 99: 115-121.
-
Berg M, Erlandsson LK, Sparud-Lundin C (2012) Breastfeeding and its impact on daily life in women with type 1 diabetes during the first six months after childbirth: a prospective cohort study. Int Breastfeed J 7: 20.
-
Kachoria R, Oza-Frank R (2014) Factors associated with breastfeeding at discharge differ by maternal diabetes type. Diabet Med 31: 1222-1229.
-
O'Connor AB, Collett A, Alto WA, O'Brien LM (2013) Breastfeeding rates and the relationship between breastfeeding and neonatal abstinence syndrome in women maintained on buprenorphine during pregnancy. J Midwifery Womens Health 58: 383-388.
-
Jones HE, Dengler E, Garrison A, O'Grady KE, Seashore C, et al. (2014) Neonatal outcomes and their relationship to maternal buprenorphine dose during pregnancy. Drug Alcohol Depend 134: 414-417.
-
Mozurkewich EL, Rayburn WF (2014) Buprenorphine and methadone for opioid addiction during pregnancy. Obstet Gynecol Clin North Am 41: 241-253.
-
Tosone G, Maraolo AE, Mascolo S, Palmiero G, Tambaro O, et al. (2014) Vertical hepatitis C virus transmission: Main questions and answers. World J Hepatol 6: 538-548.
-
Dunkelberg JC, Berkley EM, Thiel KW, Leslie KK (2014) Hepatitis B and C in pregnancy: a review and recommendations for care. J Perinatol 34: 882-891.
-
Alexander A, O'Riordan MA, Furman L (2010) Do breastfeeding intentions of pregnant inner-city teens and adult women differ? Breastfeed Med 5: 289-296.
-
Apostolakis-Kyrus K, Valentine C, DeFranco E (2013) Factors associated with breastfeeding initiation in adolescent mothers. J Pediatr 163: 1489-1494.
-
(2011) Academy of Breastfeeding Medicine. ABM Clinical Protocol #10: breastfeeding the late preterm infant (34(0/7) to 36(6/7) weeks gestation) (first revision June 2011). Breastfeed Med 6: 151-157.
-
Radtke JV (2011) The paradox of breastfeeding-associated morbidity among late preterm infants. J Obstet Gynecol Neonatal Nurs 40: 9-24.
-
Hackman NM, Schaefer EW, Beiler JS, Rose CM, Paul IM (2015) Breastfeeding outcome comparison by parity. Breastfeed Med 10: 156-162.
-
Donath SM, Amir LH; ALSPAC Study Team (2003) Relationship between prenatal infant feeding intention and initiation and duration of breastfeeding: A cohort study. Acta Pediatr 92: 352-356.
-
DiGirolamo A, Thompson N, Martorell R, Fein S, Grummer-Strawn L (2005) Intention or Experience? Predictors of continued breastfeeding. Health Educ Behav 32: 208-226.
-
Gross SM, Resnik AK, Nanda JP, Cross-Barnet C, Augustyn M, et al. (2011) Early postpartum: A critical period in setting the path for breastfeeding success. Breastfeed Med 6: 407-412.
-
Stuebe AM, Grewen K, Meltzer-Brody S (2013) Association between maternal mood and oxytocin response to breastfeeding. J Womens Health (Larchmt) 22: 352-361.
-
Andrade SE, Scott PE, Davis RL, Li DK, Getahun D, et al. (2013)Validity of health plan and birth certificate data for pregnancy research. Pharmacoepidemiol Drug Saf 22: 7-15.
-
Tenfelde S, Finnegan L, Hill PD (2011) Predictors of breastfeeding exclusivity in a WIC sample. J Obstet Gynecol Neonatal Nurs 40: 179-189.
-
Brown A, Jordan S (2014) Active management of the third stage of labor may reduce breastfeeding duration due to pain and physical complications. Breastfeed Med 9: 494-502.





