International Journal of Women's Health and Wellness
"Cold Uterus" and Other Beliefs about Fertility on the US-Mexico Border
Allison M Gilbert1*, Jill A McDonald1, Rebecca L Palacios1, Ivan de la Rosa2 and Elynor Wilson3
1Department of Public Health Sciences, College of Health and Social Services, New Mexico State University, USA
2School of Social Work, College of Health and Social Services, New Mexico State University, USA
3Chapel Hill, North Carolina, USA
*Corresponding author:
Allison M Gilbert, Department of Public Health Sciences, College of Health and Social Services, New Mexico State University Las Cruces, New Mexico 88003, USA, E-mail: am.gilbert14@gmail.com
Int J Womens Health Wellness, IJWHW-2-032, (Volume 2, Issue 3), Original Research; ISSN: 2474-1353
Received: June 04, 2016 | Accepted: September 02, 2016 | Published: September 05, 2016
Citation: Gilbert AM, McDonald JA, Palacios RL, de la Rosa I Wilson E (2016) "Cold Uterus" and Other Beliefs about Fertility on the US-Mexico Border. Int J Womens Health Wellness 2:032. 10.23937/2474-1353/1510032
Copyright: © 2016 Gilbert AM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
In the United States and Mexico, birth rates are higher along the US-Mexico border than in non-border areas. Socioeconomic and cultural factors have been studied in relation to fertility among US Hispanics, but study in the border region is limited. To better understand the complexity of fertility behavior along the border, we analyzed transcripts from previously conducted discussion groups that were broadly focused on reproductive health in the region. A total of 61 pregnant or recently pregnant women in one pair of US and Mexican border cities participated. Analysis revealed four themes, including trusted sources of reproductive health information, pregnancy prevention, gender roles, and family planning and abortion. A number of women expressed the belief that a "cold uterus" or a "young uterus" could prevent conception. These ideas might express a popular belief that could affect choices surrounding pregnancy. Results suggest that family members and healthcare providers are trusted sources, but information they share may not be evidence-based; contraceptive decision-making takes place in a context of strong social norms and gender roles; and family planning is a familiar concept, but may not be practiced until after a first pregnancy. This qualitative analysis suggests new explanations for birth disparities and a need for new measures of reproductive health in behavioral survey instruments.
Keywords
Hispanic, Women's health, Family planning, Reproductive health
Introduction
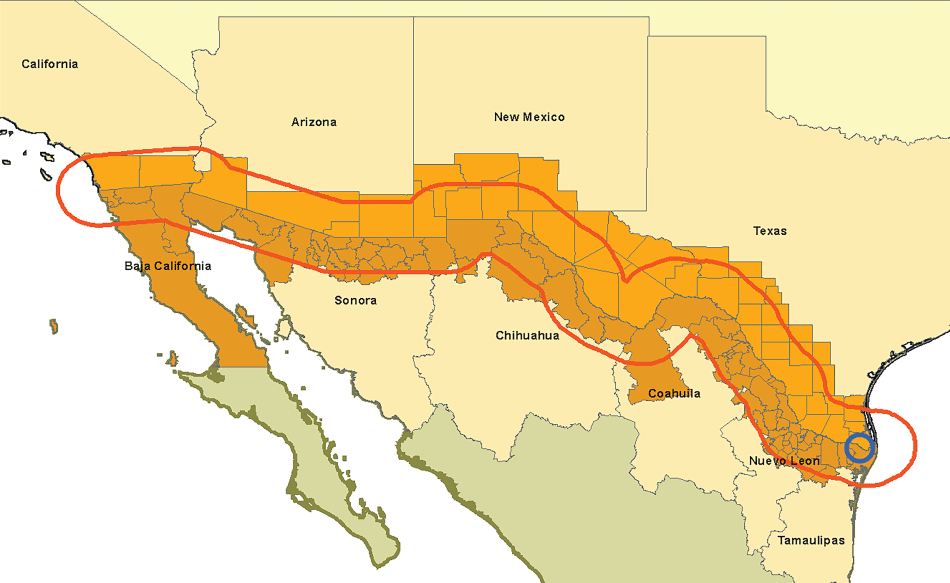
The United States-Mexico border region includes 44 United States [US] counties and 80 Mexican municipios [1] (see Figure 1). Birth rates in US counties and Mexican municipios are higher than rates elsewhere in the US and Mexico, respectively [2]. Hispanic adolescents in US border counties have especially high birth rates compared to their peers in the US. Among every 1000 US Hispanic girls aged 15-19 years, 73.8 gave birth per year in border counties in 2009 compared to 63.6 in the US overall. Similarly, in Mexican border municipios, 86.7 per 1000 girls age 15-19 years in 2009 gave birth compared to 72.5 in Mexico overall [2]. Despite steady declines in birth rates among all racial/ethnic groups in the US [3] and in Mexico [2], and national and regional goals to reduce adolescent fertility [4-6], disparities in birth rates between young US Hispanic and Mexican women on the border and their non-border peers persist [7].
US and Mexican state-based surveys that monitor trends in reproductive health [8,9] can provide information about factors associated with fertility in the region. For example, the Texas Pregnancy Risk Assessment Monitoring System [PRAMS] included an oversample of border county births in 2010 which showed lower rates of postpartum contraception use and higher rates of unwanted birth, mistimed birth, and intimate partner violence among border county women [10]. In a special analysis of data from Mexico's 2006 National Health and Nutrition Survey [ENSANut], investigators found that adolescents in border municipios were more likely than other Mexican adolescents to not use a condom at first sex [11]. A review of literature and recent national survey data from the US Hispanic population found that access to healthcare likely impacts many aspects of health, including fertility behavior [12]. While these surveys gather useful information on fertility practices and related behavior, they are not designed to help explain the reasons behind these behaviors and how they might impact fertility rates in the region.
We took advantage of previously collected qualitative data to examine sociocultural influences that may be operating on fertility behavior in one area of the US-Mexico border. We expect results to enhance our understanding of contraception and birth practices in this population and suggest approaches to address the birth disparity among adolescents and youth.
1Figure 1: Southwest Institute for Health Disparities Research [6].
http://swihdr.research.nmsu.edu/
Methods
Study sample
Study data derive from discussion groups conducted in Brownsville, Texas, USA and Matamoros, Tamaulipas, Mexico in 2004 as part of an effort to develop a model for binational reproductive health surveillance in the region [13]. The discussion groups targeted low-income women living in low-resource colonias2 who are not easily reached by health surveillance techniques that rely on fixed home addresses and good telephone coverage. The purpose of the discussion groups was to determine how standard reproductive health surveillance questions would be interpreted and whether women would be willing to respond to such questions. Project staff worked with community partners who served the target population, including promotoras, physicians, and community health center staff, and used convenience sampling to identify the sample. In Brownsville, study women were recruited through two community organizations and a Women, Infants and Children [WIC] clinic, a US government-funded program to assist pregnant and recently pregnant women, infants, and children with nutrition and healthcare. In Matamoros, a community organization and the adolescent health clinic at the public community hospital recruited study women. Women eligible for study were at least fifteen years old, currently or recently pregnant (had given birth in the last twelve months), and resided in Brownsville or Matamoros. Community partners in Brownsville and in Matamoros were asked to recruit up to 20 eligible participants ≤ 19 years of age (referred to as the young women, or YW) and up to 20 eligible participants ≥ 20 years of age (referred to as the adult women, or AW). A total of sixty-one eligible women participated in eight discussion groups, including two among YW and two among AW in each community (Table 1).
![]()
Table 1: Characteristics of discussion groups.
View Table 1
Discussion groups were held at the same locations from which women were recruited. Each discussion lasted approximately two hours. The moderator guide included ten prompts on a broad range of reproductive health surveillance topics, including pregnancy, infant health and family life. The discussions were conducted in Spanish, recorded, and transcribed. Spanish language transcripts were then translated by a professional interpreter and dictated into an audio voice recorder for transcription into English. Spanish and English transcripts were then reviewed by the original study investigators and perceived discrepancies were discussed and resolved. The de-identified, translated transcripts of the discussion group interviews were used in the current study.
Data analysis
We used MAXQDA 11 qualitative data software to conduct a thematic, secondary analysis of the group transcripts. Following standard methods for qualitative data analysis [15], the transcripts were reviewed to identify themes and sub themes regarding fertility behavior using inductive techniques [16]. One investigator had primary responsibility for transcript review, theme identification and coding. The codes and text were organized into clusters supported by themes and subthemes [15]. The coding process was concluded after six reviews of the transcripts produced no new themes or codes [17]. These were then reviewed by a second investigator and discrepancies were resolved through discussion. The two investigators agreed on the final set of codes and themes.
2A colonia is a residential area along the US-MX border that lacks some basic services, such as potable water and electricity [14].
Results
Four major themes emerged from the data that were gathered from the 61 study women: trusted reproductive health information sources, pregnancy prevention, gender roles, and family planning and abortion. Several subthemes emerged from these themes and are documented under each theme heading and in table 2.
![]()
Table 2: Discussion group themes and subthemes.
View Table 2
Trusted sources of information
Throughout the discussion groups, women talked about where they received reproductive and pregnancy health information. Prominent sources of information included family members, friends and, to a lesser extent, health care professionals. For example, one Brownsville AW described the sources of reproductive health information this way: "Your mother, female family, doctor, or people you can trust". Another Brownsville YW talked about her knowledge of the rhythm method of contraception: "I know a little about this because I speak with my sisters". Women also acknowledged that institutions like a clinic or school are sources of information. Brownsville women mentioned clinics and gynecologists as information sources more frequently than the Matamoros women. However, in all groups women spoke mostly about family and close friends in this context. As one Brownsville AW stated: "You pass it on from person to person and the information is learned". When asked about regular doctor visits as a source of information, one Matamoros AW commented: "I always ask my mother and my grandmother".
Some women, especially those in the Matamoros discussion groups, suggested that they had an unmet need for accurate information. Matamoros women noted that it was often difficult to talk about their reproductive health with family, partners, or other knowledgeable sources. One Matamoros AW explained, "We are not comfortable telling our mothers: I'm 18 years old and I had sex with my boyfriend. She will get hysterical and... We should have someone that could guide us or tell us what to do".
Pregnancy prevention
The women mentioned many methods of contraception and discussed their own use as well as their perception of other women's contraceptive use. In addition, they expressed beliefs about contraception in relation to fertility. These beliefs seemed to guide when, why, and which contraceptive methods they used.
Contraceptive methods and use: Women in each discussion group mentioned methods of contraception initiated by men and others by women. One AW from Matamoros addressed the abstinence method of contraception stating bluntly that "Nobody does that".
Some women were familiar with the idea of using a condom with a second contraceptive method, but others expressed it was uncommon to use two methods of contraception at once. One Brownsville YW explained that condoms are a convenient form of contraception:
"Because it is the fastest way; to get pills or shots you have to go to the doctor, but not with a condom. You could go to any store to buy it. Some stores even have them in the bathrooms so you could do it secretly".
Intrauterine devices [IUDs], pills, shots, condoms, rhythm, withdrawal, abstinence, home remedies, emergency contraception, and male and female sterilization were each mentioned in at least one discussion group. The home remedy, ruda tea, or rue, is commonly used for abortion [18,19] but was referred to by one Matamoros AW as a method of contraception. Condoms were talked about most often, but pills, rhythm, IUDs, shots, tubal ligation, and vasectomy were also frequently discussed in all groups.
Timing of initial contraceptive use: Delaying the initiation of contraception until after the first baby was discussed in every group. Several women gave their personal accounts: (Brownsville AW) "I started taking medicine after I had my first daughter" and (Matamoros AW) "I started to take care of myself when I was 22 years old. I had my first baby at 14 and the other one at 18, but I didn't take care". However, remarks made by young women in Brownsville and Matamoros more often acknowledged using contraceptives at menarche or sexual debut than remarks made by adult women in either community.
Cold uterus: Adult women on both sides of the border and the young women in Mexico talked about the possibility of a "cold uterus" in the context of hormonal contraceptives. Women said that if contraception was started too early, the uterus could become cold or infertile, and result in a woman's inability to become pregnant later in life. As one Matamoros AW stated:
"They say that if you use contraceptives when you are too young it is bad for you. They say you will not be able to have a baby. That is why some women don't want to take it before...They say your uterus will get cold".
Other statements that illustrate this belief include: (Matamoros YW) "Some say your uterus is cold and you need to warm it", suggesting that a cold uterus is not compatible with pregnancy and must be warmed before a pregnancy is viable, and (Brownsville AW) "Some people say that if you get married and start to take care, your uterus will get cold and you will not be able to get pregnant. So normally, you first have a child and then you take care". In response to another woman who spoke about the uterus becoming cold, a Matamoros AW stated: "I have a friend that was taking the pills since she was 12 years old. She is now 25 years old and she can't get pregnant. She is sterile because she took care of herself from a young age".
Young uterus: A "young uterus", different from a cold uterus, was used to describe young women who cannot conceive or sustain a pregnancy. One Matamoros YW said, "If they are too young they could have a weak uterus". Another Matamoros YW shared, "My mother said I had a young uterus. I didn't think I was going to get pregnant".
Gender roles
Throughout each discussion group, the women mentioned several societal expectations regarding contraception, pregnancy, and motherhood.
Female gender roles: Several women shared their beliefs about a woman's inevitable motherhood. However, several women also demonstrated resistance to this traditional role and felt they had some control over becoming a mother. One Brownsville AW expressed both beliefs, "I think that women are the ones that have to deal with the kids because the man has to go to work ... It is up to us to take care if our partner won't take care of us".
One Matamoros AW stated, "If you are pregnant and married, it's your husband's and you should want to have it". From this statement and others, it seemed that a married woman's attitude towards giving birth was expected to be positive. Another Matamoros YW described her acceptance of her pregnancy after learning that she was pregnant: "They told me I could abort it. I didn't want to get pregnant, but I decided to have it".
Similarly, one Brownsville AW shared her belief about who has responsibility for contraceptive care, and ultimately whether or not a woman becomes pregnant, "The woman should take care of herself. Today, it is always the woman". Another Matamoros AW voiced a similar attitude: "It is our responsibility to take care".
Women seldom mentioned religion as playing a part in their role as a woman and mother. God or religion was mentioned just four times and only in the Brownsville AW discussion groups in reference to one's ability to have a child. For example, an AW in Brownsville said, "This is my second one because I lost the first one. Thank God, He gave me another one". Women in other discussion groups spoke freely about contraception and abortion but did not mention God or religious beliefs.
Male gender roles: In six of the eight discussion groups, male gender roles were discussed extensively. Some women shared that their decision to become pregnant was mutual, but numerous women stated that men's preferences in relationships often dominated. Two Matamoros AW described that men can "Demand a baby", and "You could be taking care or have been married two or three years and they will demand a baby. You don't want to contradict them so you get pregnant". Another Matamoros AW described the difficulty of using condoms because condom use can depend on: "If he wants it; if not, no". In regards to consensual sex and trying to protect oneself, a YW from Brownsville stated, "If it's your boyfriend or your partner that is not abuse. If it's your husband and he wants to have sex, you should". Some women also mentioned that going to a male doctor was difficult because their partner did not want them seen by another man.
Family planning and abortion
Many women seemed aware of the concept of family planning but did not seem to engage in family planning behavior. Some women held strong beliefs about family planning as indicated by this quote from a Matamoros AW, "People get pregnant because they want to. There is lots of information on birth control out there. When you are 15 or over, you should know that if you have sex you will get pregnant".
Family planning: Occasional comments from the discussion groups indicated that some women had planned their pregnancies. One Brownsville AW shared, "I was taking pills to avoid getting pregnant, but I wanted to get pregnant, so I started taking vitamins". Another Brownsville YW described her planned pregnancy:
"I planned it. Well, my husband and I planned it. We took care of ourselves before and after. We used condoms. After I had my baby I started using the shot. I don't know why, but I started to use it. (Laughing) It was planned, we had been together for some time and I became pregnant".
Several women expressed surprise about their pregnancy or said it was unexpected. (Matamoros AW) "You don't think about it. I'm pregnant and I didn't plan it. This is not the best time in my life to be having a baby". These women did not indicate that they were ready to be pregnant or had planned their pregnancy. Their comments had a slightly negative tone, suggesting that these unintended pregnancies may have also been unwanted at the time they occurred. For example, one Brownsville YW reflected on her pregnancy: "I was frustrated because I had not finished high school".
Abortion: Women in all groups mentioned several methods of intentional and unintentional termination of a pregnancy, including a medical or surgical abortion. Some methods stated by the women include: (Matamoros AW) "Some will carry something heavy on purpose so that the baby will come", (Matamoros AW) "Or you could run". (Brownsville AW) "She was taking Aruga to lose the baby", and (Brownsville AW) "In Mexico they take Tajua... It is a beer. You boil it with pills and Desenfrioles3 and drink it". One Matamoros AW stated that "If you go to a doctor they could report you to the authorities, but the midwife will not". Women also mentioned that abortions occur as a result of intimate partner violence. For example, when referring to women's male partners or husbands, one Matamoros AW said, "They hit them. Probably because they didn't want to have sex so they hit them... I have a friend that lost her baby because of that".
3Desenfrioles likely refers to Desenfriol D, a common cold medicine sold in Mexico [20].
Discussion
Our study utilized existing discussion group transcripts to explore factors influencing fertility behavior in two communities along the US-Mexico border. We identified four themes and several subthemes within each theme (Table 2). The analysis of these themes and subthemes indicated that prevalent societal norms, such as women's trusted sources of reproductive health information and traditional gender roles, and beliefs about infertility in relation to age and the timing of contraceptive use may impact a woman's reproductive health behavior in important ways. These observations are consistent with the framework of sociocultural theory, which asserts that behavior stems from and is shaped by interactions with others, society, and culture [21].
In this study, women's trusted sources for information about reproductive health were primarily the women with whom they shared close relationships and included health authority figures like gynecologists. These trusted relationships, particularly family, likely trump other sources of information or are a woman's only source of information. This observation is consistent with other studies of child-bearing women in the US-Mexico border region [22] and elsewhere [23].
Also, consistent with other research [24], our results suggest that communication about sexual and reproductive health between women and their trusted family members is lacking due to a variety of factors. Literature supports that Hispanic women have less access to quality sources of health information and affordable health care than other women [12]. Another possible contributor to lack of accurate information is the shortage of healthcare providers and workers in the border region. In some areas, the region is nearly 50% more likely to have medical service shortages [25].
Despite lower access to reproductive health information, numerous methods of contraception were discussed by study women, suggesting that women who are or have been pregnant are informed about a variety of contraceptive methods. However, the exact source of this information and whether or not women learned about these methods before they became sexually active cannot be determined from our study.
The trusted sources of information reported by women in this study may be perpetuating attitudes and beliefs that contribute to higher fertility at younger ages [24]. One such belief is that early hormonal contraceptive use, such as the pill, causes a uterus to become cold and resistant to later child-bearing. A belief that certain contraceptive methods have adverse effects on future fertility could lead to the delay of initial contraceptive use until a woman is certain she will have at least one child. This finding is consistent with a belief held by Hispanic women in Houston, Texas [26] that the birth control pill has significant adverse outcomes.
The concept of a cold uterus resulting from early use of hormonal contraceptives may have its roots in ancient humoral medicine beliefs still prevalent in Latino and other cultures [27-30]. Humoral theory suggests the body is a balanced combination of four humors, unique to each individual, and that an imbalance of these humors causes illness [27]. There is evidence that some Mexican heritage women prefer to eat hot foods at conception and during pregnancy to prepare a warm and loving environment for the fetus [30]. Perhaps the cold uterus phenomenon described by our study women stems from these traditional beliefs.
Another misperception about one's ability to conceive that might be perpetuated by women's trusted sources of information is the protection against pregnancy offered by a young uterus. As described in these discussion groups, a young uterus cannot carry a child when the would-be mother is too young. The definition of "too young", or the age before which pregnancy will not occur, was not specified by the discussion group women. Believing that a young uterus will prevent pregnancy could lead adolescents to incorrectly think that they can be sexually active and avoid pregnancy simply because of their young age.
Abortion was discussed among the women as a way to avoid having a child, and the women discussed different methods of abortion. Several women talked about self-induced abortions, such as home remedies, lifting heavy objects, or running while pregnant. A few women also mentioned intimate partner violence as a cause of abortion; though, it is unclear from the transcripts if these abortions were the intent of the partner perpetrating the violence or an unintended consequence of an abusive relationship. We do know that intimate partner violence is more prevalent among women who abort their pregnancy than among women who do not [31]. The Matamoros women reported that midwives or clandestine services were safer than doctors because of the potential legal repercussions; abortion remains illegal in the state of Tamaulipas, Mexico except when the mother's life is in danger [32]. This finding is consistent with a study by Juarez and Singh [33] which found high rates of unsafe abortion among Mexican adolescents and young women. Literature supports that many women, particularly in developing countries where abortion is illegal, seek clandestine abortions to avoid social stigma associated with terminating a pregnancy [34].
Study women infrequently mentioned religion in the discussion groups, despite the strong majority of both Mexicans and Mexican Americans identifying as Catholic [35]. Only the Brownsville AW mentioned a religious figure. In contrast, existing literature indicates that women commonly reference their religious beliefs when discussing sexual health and behavior [36]. A study of abortion attitudes among Mexican, Puerto Rican and Cuban women, found that women who identified with strong Christian religious beliefs had sharply negative views regarding abortion [36].
There is evidence in the discussion group transcripts that societal norms and gender roles impact fertility decisions among study women. Some women stated that their fertility decisions reflected their partner's preferences. For example, using a male condom might require partner assent and action, and seeing a doctor for contraception may depend on the gender of the doctor and permission from the woman's partner. This is consistent with other findings that Mexican men tend to dominate household and family decision making in their relationships [37]. Sterling and Sadler [24] identified male dominance and female submissiveness as factors influencing contraceptive use among Hispanic adolescents and young adults. Women in our study acknowledged a strong male influence and expressed a need for women to take contraception into their own hands so as to avoid a difference of opinion with their partner. This is consistent with previous observations that Hispanic women consider contraception to be a women's issue and opt not to include men in decisions about contraception if possible [26].
Except for differences in the discussion around abortion and occasional references to God by the adult women in Brownsville, US and Mexican women in this study shared common concerns and discussed the themes uncovered in this analysis nearly equally. This commonality is likely due to a shared Mexican culture and a fluid border, that is, the movement of many families back and forth across the border for work, school, shopping and social reasons [25,38].
Adolescent birth rates are high in the US-Mexico border region compared to the US and the US Hispanic population, but the reasons why rates are high are not known. Poverty and lack of access to care have been implicated [25], but cultural norms operating in this population likely play an important role and are relatively unexplored [39]. This study adds to our understanding of how cultural norms and beliefs could play a key role in fertility patterns in this population. An additional strength of our study is that it includes women living on both sides of the border. This is important because US and Mexican adolescents who live along the border have fertility rates that are higher than rates elsewhere in the US and Mexico, respectively. To the extent they also share behavioral and cultural characteristics [25] that impact fertility, binational approaches to adolescent pregnancy prevention that are sensitive to shared sociocultural norms and consistent with regional goals to reduce adolescent pregnancy [5] might have greater likelihood of success.
This study also has a number of limitations. First, the data were collected in 2004 and may not reflect the situation of women who are currently pregnant in Brownsville and Matamoros study communities. However, cultural influences and themes like those uncovered in this analysis are unlikely to change quickly [40,41], and more recent data continue to show disparities among teenage and unplanned pregnancies in this population [7,42,43]. Second, potentially important demographic characteristics, such as parity and marital status, were not collected during the discussion groups and could not be analyzed. Third, as is typical in qualitative research, the sample was not designed to be representative of all women living in the study communities and thus results cannot be generalized beyond the study population.
Recommendations
We have several recommendations. First, our findings point to a need for improved, culturally relevant health education among study women, their family members, and others who provide support. As women's beliefs, attitudes, and sexual choices develop within the context of their relationships, culturally relevant educational interventions that consider restructuring women's sociocultural environment, similar to what some family-centered comprehensive sexual education programs have done for Hispanic communities [44], are needed. Future educational interventions could be tailored to address the knowledge gaps and gender roles that complicate fertility decision-making in border communities. Second, efforts to reduce the barriers to access of family planning resources may be worthwhile. Interventions leading to an increase in knowledge will likely also increase motivation to seek resources [45]. Interventions could include allowing oral contraception to be sold over-the-counter in the US, or making long acting reversible contraceptives and education more available to women [46]. Third, collecting qualitative information from nulliparous women would provide valuable information about pregnancy intention, knowledge about sexual health, and societal pressures that influence fertility behavior. Fourth, national and state surveillance systems that serve the US-Mexico border population should be revised to include questions and response options that capture important characteristics of this population, such as unique barriers to early initiation of hormonal contraception and key sources of fertility information. Lastly, whatever approaches are taken to eliminate the fertility disparity shared by border communities, a binational effort that could maximize the potential of available resources in the region and take advantage of the interconnectedness of this trans-border population makes sense [38].
Conclusion
Our qualitative study of US Hispanic and Mexican women in two communities along the Texas-Mexico border found evidence of previously unreported cultural factors that may explain high fertility in this population. The prevalent belief that early use of hormonal contraception prevents pregnancy later (a cold uterus) and that very young women are protected against pregnancy because their uteri are too young for conception could cause women to delay use of contraception until after a first pregnancy. Additional findings support previous literature regarding the importance of male and female gender roles in fertility behavior and decision-making, inaccurate information or lack of quality information from trusted sources, and the frequent use of clandestine abortion methods. These results call for culturally relevant health education strategies and improvements in reproductive health surveillance instruments that will enhance the public health programs and policies that serve the US-Mexico border population and work toward the goals of both nations.
Acknowledgements
The authors thank the original study participants and the Division of Reproductive Health at the Centers for Disease Control and Prevention for use of the data.
Ethics Statement
The protocol for the original study was reviewed for human subjects concerns by the Centers for Disease Control and Prevention and found to be in compliance. Use of the data for this analysis of the translated transcripts was approved by the primary investigator's Institutional Review Board.
References
-
http://www.borderhealth.org/border_region.php
-
Mc Donald JA, Mojarro O, Sutton PD, Ventura SJ (2013) A binational overview of reproductive health outcomes among US Hispanic and Mexican women in the border region. Preventing Chronic Disease 10.
-
Martin JA, Hamilton BE, Osterman MJK, Curtin SC, Mathews TJ (2013) Births: Final data for 2012. National Vital Statistics Report 62.
-
https://www.healthypeople.gov/2020/topics-objectives/topic/family-planning.
-
http://www.borderhealth.org/files/res_2805.pdf.
-
http://omm.org.mx/images/stories/Documentos%20grandes/Programa%20Sectorial%20de%20Salud%202013-2018.pdf.
-
McDonald JA, Mojarro O, Sutton PD, Ventura SJ (2015) Adolescent births in the border region: A descriptive analysis based on US Hispanic and Mexican birth certificates. Matern Child Health J 19: 128-135.
-
http://www.cdc.gov/prams.
-
http://ensanut.insp.mx/.
-
Pregnancy Risk Assessment Monitoring System [PRAMS]. Texas.
-
Instituto Nacional de Salud Pública Encuesta Nacional de Salud y Nutrición 2006 (2008) Resultados en las Fronteras, Instituto Nacional de Salud Pública-Secretaría de Salud, Cuernavaca, México.
-
Escarse JJ, Kapur K (2006) Access to and quality of health care. In: Tienda M, Mitchell F, Hispanics and the future of America. The National Academies Press, Washington DC, 410-446.
-
McDonald JA, Johnson CH, Smith R, Folger SG, Chavez,AL, et al. (2008) Reproductive health surveillance in the US-Mexico border region, 2003-2006: The Brownsville-Matamoros sister city project for women's health. Prev Chronic Dis 5: 1-17.
-
http://www.sos.state.tx.us/border/colonias/what_colonia.shtml.
-
Pope C, Ziebland S, Mays N (2000) Qualitative research in health care: Analyzing qualitative data. BMJ 320: 114-116.
-
Guest G, MacQueen KM, Namey EE (2012) Introduction to applied thematic analysis. Sage Publications, Thousand Oaks, CA.
-
http://dx.doi.org/10.4135/9781412963909.
-
http://www.webmd.com/vitamins-supplements/ingredientmono-885-rue.aspx?activeingredientid=885&activeingredientname=rue.
-
Polgar S, Fried ES (1976) The bad old days: Clandestine abortions among the poor in New York City before liberalization of the abortion law. Fam Plann Perspect 8: 125-127.
-
http://www.farmaciasdelnino.mx/eng/index/item/375/desenfriol-d-24tab.
-
Vygotsky L, Michael Cole (1978) Mind in society: The development of higher psychological processes. Harvard University Press, Cambridge, MA.
-
DeSisto CL, McDonald,JA, Rochat R, Diaz-Apodaca BA, Declercq E (2016) Decision-making about method of delivery U.S.-Mexico Border. Health Care for Women Int 37: 426-443.
-
Declercq ER, Sakala C, Corry MP, Applebaum S (2006). Listening to mothers II: Report of the second national U.S. survey of women's childbearing experiences. Childbirth Connection.
-
Sterling SP, Sadler LS (2009) Contraceptive use among adolescent Latinas living in the United States: The impact of culture and acculturation. J Pediatr Health Care 23: 19-28.
-
http://www.borderhealth.org/files/res_2213.pdf.
-
Sangi-Haghpeykar H, Ali N, Posner S, Poindexter AN (2006) Disparities in contraceptive knowledge, attitude and use between Hispanic and non-Hispanic whites. Contraception 74: 125-132.
-
http://ocp.hul.harvard.edu/contagion/humoraltheory.html.
-
http://patch.com/georgia/peachtreecorners/cold-uterus-and-infertility.
-
http://www.traditionalqi.com/2011/04/20/1639/.
-
Zoucha R, Zamarripa CA (2013) People of Mexican heritage. In: Purnell LD, Paulanka BJ, Transcultural Health Care: A Culturally Competent Approach. (2nd edn), F.A. Davis, Philadelphia, PA, 264-278.
-
Williams GB, Brackley MH (2009) Intimate partner violence, pregnancy and the decision for abortion. Issues Ment Health Nurs 30: 272- 278.
-
http://informe2015.gire.org.mx/#/ampliacion-causales-aborto
-
Juarez F, Singh S (2012) Incidence of induced abortion by age and state, Mexico, 2009: New estimates using a modified methodology. International Perspectives on Sexual and Reproductive Health 38: 58-67.
-
Grimes DA, Benson J, Singh S, Romero M, Ganatra B, et al. (2006) Unsafe abortion: The preventable pandemic. The Lancet 386: 1908-1919.
-
Donoso JC (2014) On religion, Mexicans are more Catholic and often more traditional than Mexican Americans. Pew Research Center.
-
Ellison CG, Echevarria S, Smith B (2005) Religion and abortion attitudes among U.S. Hispanics: Findings from the 1990 Latino national political survey. Social Science Quarterly 86.
-
Knapp J, Muller B, Quiros A (2009) Women, men, and the changing role of gender in immigration. Institute for Latino Studies University of Notre Dame 3: 1-14.
-
Marquez RR, Romo HD (2008) Transformations of la Familia on the U.S.-Mexico Border. University of Notre Dame Press, Notre Dame, IN.
-
Pittman SA, Feldman JB, Ramirez N, Arrendondo S (2009) Best practices for working with pregnant Latina adolescents along the Texas-Mexico border. Professional Development: The International Journal of Continuing Social Work Education 12: 17.
-
Landale NS, Oropesa RS (2007) Hispanic families: Stability and change. Annual Review of Sociology 33: 381-405.
-
http://www.tlacc.org/assets/hispanic-acculturation.pdf.
-
http://www.cdc.gov/pcd/issues/2008/oct/08_0057.htm.
-
Vasquez D, McDonald JA, Homedes N, Brown LD (2014) Unintended birth among Hispanic women in Texas: A descriptive analysis. Maternal and Child Health Journal 19: 1220-1229.
-
Fish H, Manlove J, Moore KA, Mass E (2014) What works for adolescent sexual and reproductive health: Lessons from experimental evaluations of programs and interventions. Child Trends.
-
http://healthaffairs.org/blog/2016/05/25/knowledge-is-power-improving-health-care-information-for-the-most-vulnerable/.
-
Potter JE, White K, Hopkins K, Amastae J, Grossman D (2010) Clinic versus over-the-counter access to oral contraception: Choices women make along the US-Mexico border. Am J Public Health 100: 1130-1136.