International Journal of Women's Health and Wellness
A Pilot Study of Patient Motivation for Postpartum Contraception Planning During Prenatal Care
Lindsay M Goad1, Heather R Williams2, Mackenzie S Treloar3, Colleen K Stockdale2 and Abbey Hardy-Fairbanks2*
1University of Iowa Carver College of Medicine, USA
2Department of Obstetrics and Gynecology, University of Iowa Hospitals and Clinics, USA
3Department of Obstetrics and Gynecology, The Ohio State University Medical Center, USA
*Corresponding author:
Abbey Hardy-Fairbanks, MD, Department of Obstetrics and Gynecology, University of Iowa Hospitals and Clinics, 200 Hawkins Drive, Iowa City, IA 52242, USA, E-mail: abbey-hardy-fairbanks@uiowa.edu
Int J Womens Health Wellness, IJWHW-3-048, (Volume 3, Issue 1), Research Article; ISSN: 2474-1353
Received: October 25, 2016 | Accepted: March 27, 2017 | Published: March 29, 2017
Citation: Goad LM, Williams HR, Treloar MS, Stockdale CK, Hardy-Fairbanks A (2017) A Pilot Study of Patient Motivation for Postpartum Contraception Planning During Prenatal Care. Int J Womens Health Wellness 3:048. 10.23937/2474-1353/1510048
Copyright: © 2017 Goad LM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Short interpregnancy interval increases maternal and infant morbidity. Improved postpartum contraceptive education and planning may reduce these risks by allowing adequate birth spacing. However, the readiness and acceptance of women to discuss contraception plans during pregnancy is unknown.
Methods: A cross-sectional study was conducted of pregnant women between 25-35 6/7 weeks' gestation at the University of Iowa Hospitals and Clinics from February 2015 to July 2015. Patients were given a survey that assessed readiness, capability and confidence about discussing and choosing a postpartum contraception plan at a prenatal visit. Secondary outcomes examined previous contraception choices, breastfeeding goals and overall knowledge regarding postpartum contraception.
Results: 238 subjects completed the survey prenatally at an average gestational age of 32 completed weeks (SD 2.9). While 73.4% planned to start contraception after delivery, 34.5% were unsure as to what method they would use. 65.5% of subjects were ready or very ready to discuss a contraception plan at their visit, 76.4% felt capable or very capable of choosing a postpartum contraception plan and 88.7% felt confident or very confident they would be able to use an effective method of birth control after having their baby. When asked if they felt ready to choose a postpartum contraception plan, 60.4% of women felt ready or very ready.
Conclusion: While the majority of pregnant women plan to start postpartum contraception, most of these women have not identified a method. Therefore, the prenatal period is an optimal time to educate and discuss available contraception options as women are receiving regular healthcare.
Introduction
Over half of pregnancies in the United States are unintended-an outcome that can be prevented by effective contraception use [1]. Women's ability to effectively use contraceptives is crucial to their education and workforce participation, income, mental health and happiness, relationship stability and children's well-being [2]. Family planning has many health benefits for mothers, newborns and families. Pregnancies that are spaced less than 18 months from the previous birth comprise one third of pregnancies in the US and have an increased risk of maternal and infant morbidity including the risk of prematurity and low birth weight as well as child health and development issues [3,4]. Although typical recommendations are to abstain from sexual activity until the six week postpartum visit, multiple studies have shown that many women engage in unprotected intercourse while postpartum [5].
Behavioral change models and motivational interviewing have been used to address several health related behaviors, including weight loss, smoking cessation and contraception use. Specifically, these techniques have influenced behavior change and have increased the likelihood of effective contraception use [6]. The antepartum period provides an important window of opportunity to discuss highly effective contraception, such as long-acting reversible contraception (LARC) methods, as women are receiving regular healthcare and have been historically thought to be motivated to engage in planning of postpartum contraception. However, the readiness and acceptance of women to discuss and choose a postpartum contraception plan prenatally is unknown.
The purpose of this study is to preliminarily assess women's readiness, capability and confidence in discussing and choosing a postpartum contraception plan prenatally. We also examined women's contraceptive history prior to conception, future conception and contraception plans, women's breastfeeding goals and general postpartum contraception knowledge.
Material and Methods
A 30 question survey (Appendix 1) was given to pregnant women between 25 and 35 6/7 weeks' gestation receiving prenatal care at the University of Iowa Hospitals and Clinics Obstetrics and Gynecology Department between February 2015 and July 2015. The survey was administered by a member of the healthcare team also certified to participate in research studies, which included a medical student, midwife, medical assistant or physician. It took approximately 5-10 minutes to complete. The survey contained a statement with the elements of consent, was self-explanatory and subjects completed it without assistance. The survey assessed readiness, capability and confidence in discussing and choosing a postpartum contraception plan. Questions were answered on a five point Likert scale. The survey also assessed previous contraception history and behavior, future conception and contraception plans, breastfeeding goals and overall knowledge regarding postpartum contraception. RED Cap (Research Electronic Data Capture), a secure web-based application was used for data collection and analysis. Women were excluded if they were under 18 years of age (due to IRB requirements) at the time of conception, non-English speaking or if they conceived through in vitro fertilization.
Routine prenatal care contraception counseling is highly variable between providers, which is why this variable was collected. Residents and generalist typically use efficacy based contraception counseling, but midwifery and high risk contraceptive counseling is variable.
We calculated the percentage of women who were ready and capable to discuss and choose a postpartum contraception plan prenatally according to gestational age and their Likert scale response. We examined women's past contraception history and behavior as well as future conception and contraception plans after delivery. Women were also asked their opinions on postpartum contraception including whose opinion they valued, how well it was discussed with their obstetrical provider and if LARC options (including the intrauterine device and implant) were specifically discussed. We also assessed if the pregnancy was planned.
As a final step, we surveyed women's breastfeeding goals and general postpartum contraception knowledge in true and false format such as "You cannot get pregnant until 6 weeks after having a baby" and "You cannot get pregnant before you have a normal period after delivery". We also assessed how breastfeeding effects conception and milk supply and the ability of women to have highly effective contraception before leaving the hospital after delivery.
Results
A total of 236 women were recruited for the study at an average of 32 weeks gestation completed. 41% reported that the pregnancy was unplanned by reporting they had not anticipated pregnancy any sooner than 6month to a year from the time they discovered their conception. Prior to this pregnancy, the five most commonly used contraceptive methods were oral contraceptive pills (83.2%), barrier methods such as condoms (64.8%), withdrawal (24.6%), depo medroxyprogesterone acetate (23.4%) and the IUD (20.9%). Only 2.5% of women reported no history of contraception use in the past. The methods used most recently prior to becoming pregnant include: oral contraceptives (35.9%), barrier methods such as condoms (23.3%), and the IUD (13.4%).
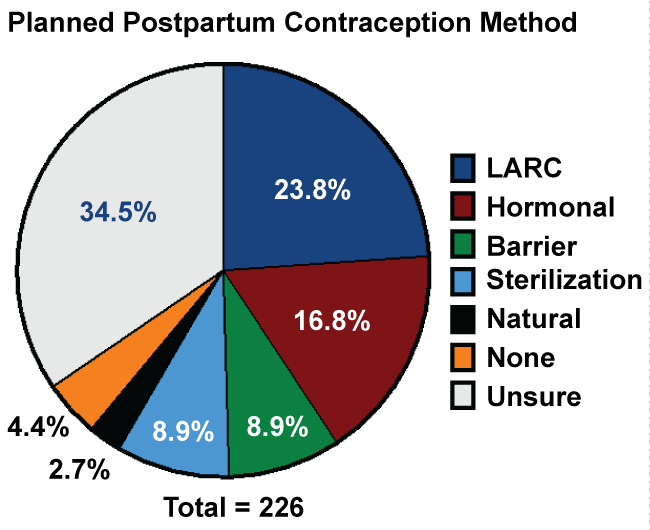
The majority of women (73.4%) planned to use postpartum contraception with close to 90% of those women planning to initiate contraception in the first 60 days after delivery. The most common contraceptive methods that women planned to use include: IUD (18.5%), oral contraceptive pills (14.5%), and barrier methods such as condoms (8.8%). However, 34.3% of women were still unsure of what method they were going to use postpartum (Figure 1).
.
Figure 1: Contraception plans and anticipated methods postpartum. Women were asked what contraception method they were planning to use. The majority of pregnant women are unsure of what method they will use postpartum. Almost 25% of women plan to use the most efficacious method, a long acting reversible contraceptive (LARC). The next most common method is a hormonal method, followed by a barrier method or sterilization with 10% each. Less than 5% plan to use no contraception method postpartum.
View Figure 1
When asked about their past contraception behavior compared to their anticipated contraception behavior after delivery, there was a 30.6% increase in the number of women who plan to "always" use contraception following delivery and a 9.5% decrease in the number of women who plan to "never" use contraception after delivery (Table 1). About half of women (50.4%) were planning on conception as soon as possible in the month before becoming pregnant, indicating a planned pregnancy. Over one third of women (37.6%) reported a plan to never become pregnant after delivery and over one third of women (37.2%) did not plan to conceive for at least another 2 years after delivery.
![]()
Table 1: Anticipated contraception behavior change after pregnancy. The survey asked two questions regarding contraception behavior with the same five answer choices, listed above: "Before you became pregnant with this pregnancy, did you use an effective method of birth control?" and "After my delivery, I plan to use an effective method of birth control?" comparing results, there is a 30.6% increase in the number of women who plan to always use contraception following delivery. There is a 9.5% decrease in the number of women who plan to never use contraception after delivery.
View Table 1
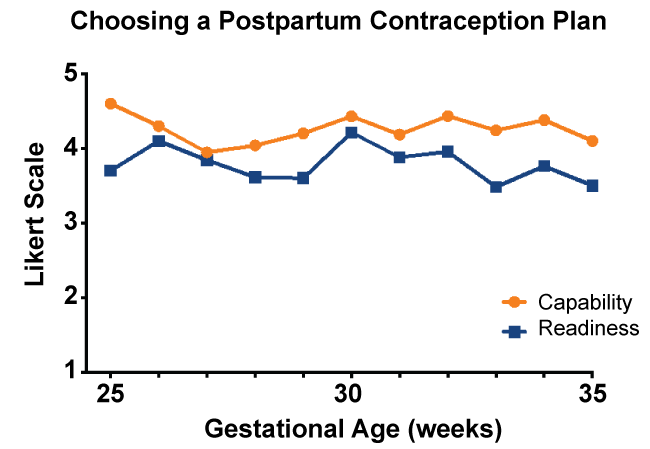
Women were asked about their readiness to discuss and choose a postpartum contraception method prenatally. Over half of women (55.6%) felt ready to discuss a postpartum contraception plan prenatally, two thirds of women felt capable of having a conversation about postpartum contraception while pregnant, 57.7% felt capable of choosing a postpartum contraception plan prenatally and 44% felt ready to choose a postpartum contraception plan during a prenatal visit. Of the women who did not feel ready to choose a contraception plan prenatally, the majority felt the timing was not right for them (28.6%) followed closely by not having enough information to make a decision (27.3%). According to gestational age, women felt more capable than ready to choose a postpartum contraception plan at every gestational age. Readiness to choose a postpartum contraception plan peaked at 30 weeks' gestation and tapered as pregnancy progressed (Figure 2).
.
Figure 2: Capability and readiness to choose a postpartum contraception plan by gestational age. Women were asked to assess how capable and ready they felt to choose a postpartum contraception plan using a Likert scale. On average, women felt capable and ready to choose a postpartum contraception plan at their prenatal visit. Overall, women felt more capable than ready to choose a postpartum contraception plan at each gestational age. Readiness to choose a postpartum contraception plan peaked at 30 weeks gestation and tapered as pregnancy progressed. Women felt most capable to choose a postpartum contraception plan early in pregnancy at 25 weeks. Capability remained stable from 29 to 35 weeks gestation.
View Figure 2
Women were then asked about their experience with contraception discussion, half (51%) of women stated their obstetrical provider talked to them about a contraception plan at a prenatal visit and of those women, 82.7% felt the topic was talked about for the "correct amount" of time. Less than 1% felt it was talked about "too much." Over half of women (58.9%) stated long acting reversible contraception options had not been discussed with them at a prenatal visit. Most women (67.9%) felt postpartum contraception should be discussed during pregnancy, with over half of women (50.6%) stating the third trimester is best. Some women (16.8%) thought the topic should not be discussed until the 6-week postpartum visit. Importantly, 80% of women valued their obstetrical provider's advice the most regarding contraception choices followed by their partner's advice (12%).
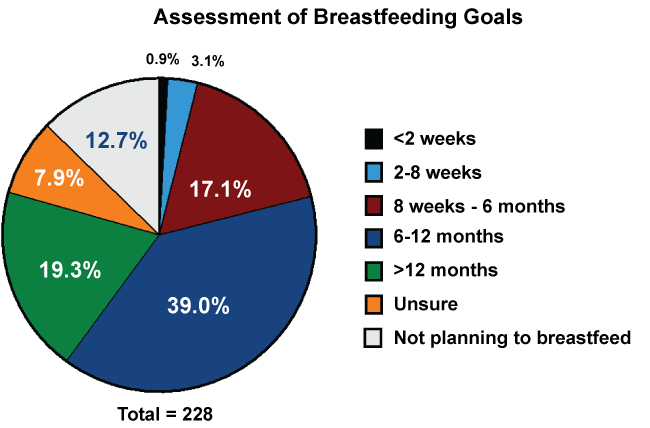
Secondary outcomes included breastfeeding goals as well as general contraception knowledge. Almost all women (87.3%) planned to breastfeed, with the most common goal being between 6-12 months (39%) followed by 19.3% of women hoping to breastfeed for 12 months or more (Figure 3). Most women understood that the first time you can get pregnant after having a baby is after the first ovulation (58.8%) and another 25.5% of women thought they were at risk for pregnancy immediately after delivery. Over 90% of women understood that you can get pregnant before 6 weeks postpartum and before having a normal period. Furthermore, about 98% of women understood that breastfeeding is not 100% protective against pregnancy.
.
Figure 3: Breastfeeding goals postpartum. Women were surveyed on what their goal length of time to breastfeed postpartum was almost 40% of women plan to breastfeed for 6-12 months postpartum, while about 20% plan to breastfeed for more than 12 months. 29% of women plan to breastfeed for 6 months or less. About 13% plan not to breastfeed postpartum.
View Figure 3
Discussion
It has been suggested that waiting until the routine six week postpartum visit to discuss and plan postpartum contraception is woefully inadequate and leaves women unprotected from unplanned short interval pregnancies and the increased morbidity that follows [7-10]. Unplanned pregnancies have serious consequences for infant, child and parental health including increased rates of abortions, negative effects on antenatal care, breastfeeding behavior and child nutrition. Studies have also found an association of unintended pregnancy with increased maternal rates of depression, anxiety and abuse as well as poor neonatal relationships and poor long-term mother-child relationships for all children in the family [11-13]. Additionally, discussing contraception options prenatally gives patients an opportunity to think about family planning-before she is occupied with a new baby and recovering from childbirth-ask questions and learn about postpartum contraception including the possibility of fertility shortly after delivery despite breastfeeding and the contraception options available and the evidence concerning breast feeding and contraceptive options.
Studies have shown that women who receive prenatal contraceptive counseling are more likely to use contraception postpartum [14,15]. Specifically, prenatal contraceptive counseling has been shown to improve the use of modern, more effective methods of contraception over traditional methods such as withdrawal, lactational amenorrhea and cycle counting [14]. The prenatal period is a unique window of opportunity to educate women on highly effective methods of contraception as women are often motivated to prevent a subsequent unplanned pregnancy soon after delivery. Prenatal counseling also allows women to have ample time to think about family planning options and continue the discussion with their provider as they have regular healthcare during pregnancy. One study found that the addition of contraceptive counseling at the 6 week postpartum visit did not improve contraceptive use compared to women that only had contraceptive counseling prenatally [16]. This suggests that women may be overwhelmed after the delivery of a new baby and are less motivated and interested in discussing and implementing contraception at this time and are at an increased risk of a short interpregnancy interval.
Close to 90% of women planned to breastfeed with two thirds planning to breastfeed for at least 6 months, the recommended length of exclusive breast feeding by the American Academy of Pediatrics [17]. Breastfeeding rates continue to rise in the United States with over a 10% increased rate of women that are breastfeeding at 6 and 12 months postpartum [18]. It is important to educate women prenatally that breastfeeding is not an effective method of contraception and another option should be used to prevent unintended pregnancy during this time period as one study showed that at least 70% of unintended pregnancies occurred within the first year after a delivery [9].
This analysis shows that most women plan to use contraception after delivery; however, many have not identified a method and thus may benefit from discussing contraception prenatally. The majority of women in this study reported feeling capable/ready and very capable/ready to discuss and choose a postpartum contraception plan while pregnant, and the majority of women themselves reported that the prenatal period is the best time for this discussion.
Most women did not intend to get pregnant for at least another two years after delivery and can benefit from highly effective reversible contraception options. There has been a significant increase in IUD use in the United States in the past 15 years, growing from 1.8% in 2002 to 9.5% in 2012 [19]. These results are consistent with the growing popularity of IUD's among both parous and nulliparous women and the continuing trend for women to use them postpartum [20]. A recent study in Colorado showed that 43% of women chose to initiate a LARC method after delivery while a recent study in North Carolina showed that more than one third of women planned to use a LARC method after delivery [21,22]. Although many providers had not yet discussed LARC methods specifically during the prenatal period, it was the most common method that women planned to use postpartum proving that the IUD's success in reducing unintended pregnancy is becoming well known either from the media or word of mouth among reproductive aged women despite any formal education prenatally. This sample of women's past contraception history mirrors national contraception trends in that the most common methods used are the pill, barrier and lastly the LARC options [23]. Importantly, this study did not take into account access to contraception resources and healthcare. Healthcare barriers have been shown to impact contraception behaviors and be a significant public health challenge for women of reproductive age [24,25]. The administration of the study survey itself may have sparked conversations about contraceptive options and that possibility is under investigation currently.
This study has shown that the obstetrical provider also serves a unique role in women's care as the person whose advice is valued most in regards to future contraception choices. Therefore, the provider has an obligation to educate women on all the contraception options available including the advantages and disadvantages of each. It is imperative that providers discuss LARC methods as they are the most efficacious reversible option available and sterilization as over a third of women were not planning to become pregnant in the future in this study. Permanent contraception is a highly desired option for women who plan to never become pregnant again and can be completed at the time of delivery or shortly after if it is discussed ahead of time [26].
Conclusion
Most women plan to "always" use contraception after delivery; however, many have not identified a method. The majority of women are ready and capable to discuss and choose a postpartum contraception plan while pregnant, thus the prenatal period is an optimal time to discuss available options and formulate a plan. Close to 90% of women plan to breastfeed with two thirds planning to breastfeed for 6 months or more.
References
-
Finer LB, Zolna MR (2014) Shifts in intended and unintended pregnancies in the United States, 2001-2008. Am J Public Health 104: S43-S48.
-
Sonfield A, Hasstedt K, Kavanaugh ML, Anderson R (2013) The Social and Economic Benefits of Women's Ability to Determine Whether and When to Have Children. Guttmacher Institute, New York.
-
Grisaru-Granovskya S, Gordon ES, Haklai Z, Samueloff A, Schimmel MM (2009) Effect of interpregnancy interval on adverse perinatal outcomes-a national study. Contraception 80: 512-518.
-
DeFranco EA, Stamilio DM, Boslaugh SE, Gross GA, Muglia LJ (2007) A short interpregnancy interval is risk factor for preterm birth and its recurrence. Am J Obstet Gynecol 197: e1-e6.
-
Bloch JR, Webb DA, Mathew L, Culhane JF (2012) Pregnancy intention and contraceptive use at six months postpartum among women with recent preterm delivery. J Obstet Gynecol Neonatal Nurs 41: 389-397.
-
Whitaker AK, Quinn MT, Martins SL, Tomlinson AN, Woodhams EJ, et al. (2015) Motivational interviewing to improve postabortion contraceptive uptake by young women: development and feasibility of a counseling intervention. Contraception 92: 323-329.
-
Madden T, Mullersman JL, Omvig KJ, Secura GM, Peipert JF (2013) Structures contraceptive counseling provided by the contraceptive CHOICE project. Contraception 88: 243-249.
-
Speroff L, Mishell DR Jr (2008) The Postpartum visit: it's time for a change in order to optimally initiate contraception. Contraception 78: 90-98.
-
White K, Teal SB, Potter JE (2015) Contraception after delivery and short interpregnancy intervals among women in the United States. Obstet Gynecol 125: 1471-1477.
-
Sok C, Sanders JN, Saltzman HM, Turok DK (2016) Sexual Behavior, Satisfaction, and Contraceptive Use Among Postpartum Women. J Midwifery Womens Health 61: 158-165.
-
Gipson JD, Koenig MA, Hindin MJ (2008) The effects of unintended pregnancy on infant, child, and parental health: a review of the literature. Stud Fam Plann 39: 18-38.
-
Singh S, Sedgh G, Hussain R (2010) Unintended pregnancy: worldwide levels, trends, and outcomes. Stud Fam Plann 41: 241-250.
-
Barber JS, Axinn WG, Thornton A (1999) Unwanted childbearing, health, and mother-child relationships. J Health Soc Behav 40: 231-257.
-
Patil E, Jensen JT (2016) Permanent Contraception for Women. Semin Reprod Med 34: 139-144.
-
Adanikin AI, Onwudiegwu U, Loto OM (2013) Influence of multiple antenatal counselling sessions on modern contraceptive uptake in Nigeria. Eur J Contracept Reprod Health Care 18: 381-387.
-
Barber SL (2007) Family Planning advice and postpartum contraceptive use among low-income women in Mexico. Int Fam Plann Perspect 33: 6-12.
-
http://pediatrics.aappublications.org/content/pediatrics/129/3/e827.full.pdf.
-
http://www.cdc.gov/breastfeeding/pdf/2013BreastfeedingReportCard.pdf.
-
Mosher WD, Moreau C, Lantos H (2016) Trends and determinants of IUD use in the USA, 2002-2012. Hum Reprod 31: 1696-1702.
-
Branum AM, Jones J (2015) Trends in long-acting reversible contraception use among U.S. women aged 15-44. NCHS Data Brief 188: 1-8.
-
Tang JH, Dominik R, Re S, Brody S, Stuart GS (2013) Characteristics associated with interest in long-acting reversible contraception in a postpartum population. Contraception 88: 52-57.
-
Tocce KM, Sheeder JL, Teal SB (2012) Rapid repeat pregnancy in adolescents: do immediate postpartum contraceptive implants make a difference? Am J Obstet Gynecol 206: 481-487.
-
Daniels K, Daugherty J, Jones J, Mosher W (2015) Current Contraceptive Use and Variation by selected Characteristics Among Women aged 14-55: United States, 2011-2013. National health statistics reports, no 86, National Center for Health Statistics, Hyattsville, MD.
-
Kennedy S, Grewal M, Roberts EM, Steinauer J, Dehlendorf C (2014) A qualitative study of pregnancy intention and the use of contraception among homeless women with children. J Health Care Poor Underserved 25: 757-770.
-
http://www.guttmacher.org/pubs/win/contraceptive-needs-2014.pdf.
-
Vural F, Vural B, Cakiroglu Y (2016) The Effect of Combined Antenatal and Postnatal Counselling on Postpartum Modern Contraceptive Use: Prospective Case-Control Study in Kocaeli, Turkey. J Clin Diagn Res 10: 04-07.





