Journal of Geriatric Medicine and Gerontology
Coronary Stenting in the Elderly: Current Status and Future Developments
SR Gnanenthiran, A Yong and HC Lowe*
Concord Repatriation General Hospital, University of Sydney, Australia
*Corresponding author:
HC Lowe, Head, Cardiac Catheterization Laboratories, Cardiology Department, Concord Repatriation General Hospital, Hospital Rd, Concord, NSW, 2139,Tel: 02 9767 500, E-mail: h.lowe@bigpond.net.au
J Geriatr Med Gerontol, JGMG-2-013, (Volume 2, Issue 1), Brief Review; ISSN: 2469-5858
Received: February 24, 2016 | Accepted: June 18, 2016 | Published: June 21, 2016
Citation: Gnanenthiran SR, Yong A, Lowe HC (2016) Coronary Stenting in the Elderly: Current Status and Future Developments. J Geriatr Med Gerontol 2:013. 10.23937/2469-5858/1510013
Copyright: © 2016 Gnanenthiran SR, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
A case is presented to first illustrate some contemporary and likely future developments in coronary stenting in the elderly, followed by a discussion of such issues.
An 86-year-old independent but frail woman living at home, presented with recurrent chest pain and pulmonary oedema. Her past history included recurrent medically managed non ST elevation myocardial infarction, heart failure and steroid responsive idiopathic thrombocytopenia (ITP). The electrocardiogram demonstrated lateral ST depression and T wave inversion. High sensitivity troponin T rose from 39 ng/L to 65 ng/L. Echocardiogram demonstrated normal left ventricular ejection fraction and hypokinesis of the basal inferior wall. The platelet count was initially 11 × 10˄9/L, rising to 200 × 10˄9/L post prednisone. She was commenced on dual antiplatelet therapy (aspirin and clopidogrel), intravenous heparin, diuretics and underwent coronary angiography.
Angiography revealed an ostial left main coronary artery (LMCA) 90% stenosis, mid left anterior descending (LAD) 70% stenosis and a first diagonal 80% stenosis (Figure 1). She was deemed to be unsuitable for coronary artery bypass grafting due to frailty and co morbidities. Haematology consulted suggested if coronary intervention were to be contemplated ideally bare metal stenting (BMS) should be considered to lessen the time on dual antiplatelet therapy, with increased prednisone dose and close monitoring of platelet count. She underwent coronary stenting to both LMCA and LAD stenosis. A 6F XB3.0 guide catheter was used with a 0.014 Run-through Floppy wire (Terumo Corp, Tokyo, Japan, via the femoral approach. A novel drug eluting stent (DES) (Synergy 3.5 × 12 mm, Boston Scientific, Natick, MA, USA) was used for the LMCA, and a BMS (2.75 × 12 mm integrity, Boston Scientific) to the LAD. The diagonal branch was not treated on this occasion given a small myocardial territory subtended. The Synergy stent has a novel design with a bioabsorbable polymer that elutes everolimus placed only on the abluminal stent surface, and is further discussed below. The patient remains well at 3 months post discharge, with a plan to continue aspirin, taper her prednisone, and stop her clopidogrel at 6 months or earlier, if there was any evidence of intolerance or bleeding secondary to the combination, with this duration determined by the Synergy drug eluting stent rather than the bare metal stent.
.
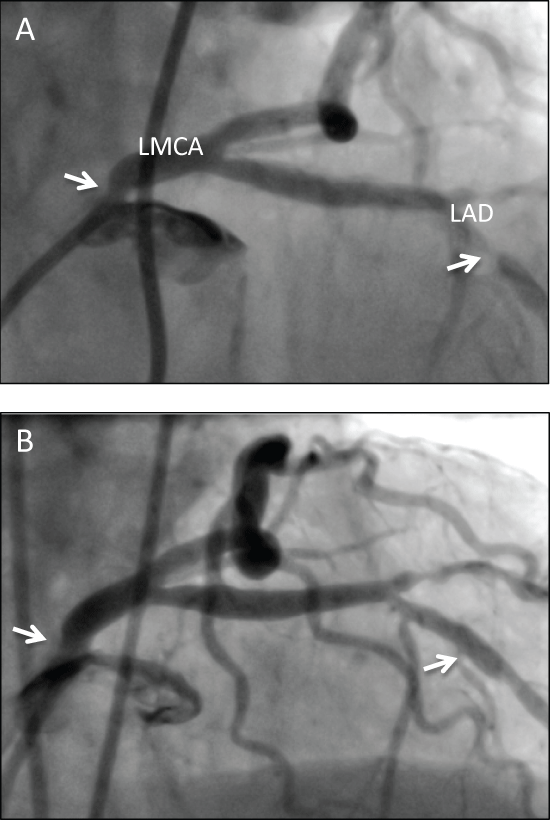
Figure 1 A) Angiography prior to coronary stenting: RAO 38, Cranial 23 angiography revealing ostial left main coronary artery stenosis (LMCA) (estimated at 90% in RAO 28, caud 19 view not shown) indicated by white arrow, and left anterior descending coronary stenosis (LAD) indicated by white arrow; B) Angiography post coronary stenting: RAO 38, Cranial 23 view. Stents marked by white arrows at prior points of stenosis in LMCA and LAD with excellent angiographic result.
View Figure 1
Coronary disease remains a leading cause of death in elderly patients, who have an increased risk of coronary events, mortality, cardiogenic shock, recurrent ischemia and re-hospitalization [1]. There is a general perception that the elderly have worse outcomes and suffer higher complication rates including bleeding, compared to younger cohorts such that older people have generally been less likely to undergo revascularisation. Historically, selected patients have been shown to receive benefit from revascularisation from coronary bypass surgery (CABG) or percutaneous coronary intervention (PCI), though this has often been underutilised [2,3]. However, perhaps as a result of improving stent and other technologies, PCI is now increasingly being utilised such that currently approximately 12% of PCI is performed in patients aged ≥ 80 years [4,5]. Many contemporary studies demonstrate similar or only slightly lower rates of successful reperfusion with PCI compared to younger age groups in the setting of PCI for acute myocardial infarction (TIMI 3 flow = 97.3% in > 80 year old v 98.3% in < 80 year old sp = 0.24) [6]. Moreover, meta-analyses confirm that PCI can offer good clinical outcomes for octogenarians, with a 30-day mortality of 5.4% and 1 year survival of 87% [7]. Some of the developments that have contributed to these improved outcomes, and some likely future developments, are now discussed.
Bare Metal vs. Drug Eluting Stents in the Elderly
The use of DES has been less in older populations [8], likely due to the perceived bleeding risks associated with prolonged dual antiplatelet therapy. A number of recent studies suggest any such bleeding risks may be less than previously estimated.
The XIMA (Xience or Vision Stents for the Management of Angina in the Elderly) multicentre randomized control trial compared the use of DES to BMS in patients > 80 years with ACS (68%) or stable angina (32%) at one year [9]. Dual antiplatelet therapy at 1 year was 32.2% for patients in the BMS group and 94.0% in the DES group. Myocardial infarction (4.3% vs. 8.7%, p = 0.01) and target vessel revascularization (2.0% vs. 7.0%, p = 0.001) were less frequent in the DES group. There was no difference in major haemorrhage (2.3% vs. 1.7%, p = 0.61), death (8.5% vs. 7.2%, p = 0.50), or cerebrovascular accident (1.5% vs. 1.2%, p = 0.77).
Similarly, observational studies also support the use of DES in older patients, even in the very elderly > 85 years old [8,10,11]. The use of DES was associated with reduced mortality compared to bare metal stents (BMS): age > 85 years (28.4% vs. 38.3%, p < 0.001); age 75 to 84 years (16.8% vs. 24.8%, p < 0.001) (median follow-up 640.8 ± 423.5 days). DES was associated with lower re hospitalization for myocardial infarction: age > 85 years (9.2% vs. 11.6%, p < 0.001); age 75 to 84 years (7.4% vs. 9.4%, p < 0.001) (median follow-up 640.8 ± 423.5 days) [8]. The benefits of DES appear to persist even over long term follow up, with another study demonstrating reductions in myocardial infarction (8.6% vs. 16.6%, p = 0.038) and target vessel revascularization rates (7.9% vs. 21.9%; p = 0.003) at 5 years in patients aged > 75 years compared to BMS [12]. Furthermore, there was no significant increase in bleeding events in those with DES (13.8% vs. 12.2%, p = 0.882) [12].
Access Route Choice in the Elderly
Following a number of studies suggesting improved outcomes for radial vs. femoral access in elective PCI (RIVAL), the MATRIX trial suggested superiority for radial PCI in reducing bleeding complications and mortality in the general ACS population compared to those randomised to femoral access [12,13].
This preference for radial access PCI has been examined also in the elderly, with acceptable failure rates of the radial approach of 7.5-9.8%, requiring crossover to alternate access [14-17]. Left radial access is a valid alternative, with reduced subclavian tortuosity (6% versus 32%, p = 0.002) observed [18]. While some studies suggest a longer cannulation and/or procedural time [15,17], other trials suggest that there is no significant difference with experienced operators [17].
There is indeed increasing evidence that transradial access may provide benefit in the elderly. A randomized trial demonstrated that in patients aged over seventy-five, there was reduced major complications (bleeding requiring surgery or transfusion or stroke, 0% vs. 3.2%, p < 0.001) compared to femoral access. Additionally, there were reduced rates of access site bleeding (2.7% vs. 9.6%, p = 0.004), hematoma (4.5% vs. 10.9%, p = 0.006), or any vascular complication (7.1% vs. 23.7%, p < 0.001) with the radial approach as opposed to femoral [15]. Additionally, radial access is associated with reduced ambulation time, shorter CCU stays (3.6 ± 1.5 vs. 5.0 ± 3.2 days, p = 0.001), and even reduced duration of hospitalization (13.3 ± 7.4 days vs. 19.2 ± 11.1 days, p = 0.001) compared to femoral access in AMI patients > 80 years old [17,19].
Novel Stent Technologies
While novel stent technologies have not been specifically targeted to the elderly, there has been a rapid evolution of stent technology, with the emergence of bio-absorbable scaffolds, bio-absorbable polymers and even novel polymer-free stents that deliver anti-proliferative agents. Such stent technology may eventually be less dependent on prolonged dual antiplatelet therapy, which would be ideal for those at high risk for bleeding including the elderly.
Bio-absorbable scaffolds comprise a fully bioresorbable Poly-L-Lactic Acid (PLLA) mechanical scaffold incorporating drug delivery similar to a DES, reviewed in detail elsewhere [20]. This mechanical scaffold provides support for approximately one year, and is completely resorbed by 4 years in a pig model [21]. A randomised trial comparing everolimus eluting bio-absorbable scaffolds (Absorb) compared to the second generation Xience DES (everolimus) demonstrated that there was no difference in cardiac death (0.6% vs. 0.1%), target vessel revascularisation (3.0% vs. 2.5%) or myocardial infraction (6.0% vs. 4.6%) from target lesion failure in the Absorb scaffold compared to DES at one year [22], though there was a small increase in stent thrombosis (1.4% vs. 0.7%, P = 0.21) associated with the Absorb scaffold, particularly sub acutely between 24 hours and 30 days (0.9% vs. 0.1%, p = 0.04). At present the potential for such scaffolds to offer shorter duration antiplatelet agent use, has therefore not been met, but is a field of active investigation. These bioresorbable stents have similarly not been trialled specifically for LMCA stenting, nor particularly in the elderly, though again is likely to be an area of future investigation.
Bio-absorbable polymers involve the short-term delivery to the vessel wall of anti-proliferative polymers, often abluminally coated on the stent surface. The EVOLVE II randomised trial compared the second generation DES Promus element plus (everolimus) to the novel Synergy stent. This is a bio absorbable abluminal polymer eluting everolimus, used in the case discussed above [23]. The attraction of such a design is locally-delivered anti proliferative drug from a bio absorbable polymer - to potentially lessen restenosis - with a luminal stent surface of thin strut cobalt chromium alloy - to potentially lessen stent thrombosis and lessen the duration of antiplatelet use. To date, non-inferiority has been likely demonstrated, with no difference in cardiac death (0.5% vs. 0.9%, p = 0.34), myocardial infarction (5.4% vs. 5.0%, p = 0.68), target vessel revascularisation (2.6% vs. 1.7%, p = 0.21) and definite/probable stent thrombosis (0.4% vs. 0.6%, p = 0.5) at one year, but the question as to whether this technology will translate to reduced antiplatelet use remains under investigation.
Conclusions
PCI is becoming increasingly utilised in older populations, with several new approaches impacting upon decision-making. Drug eluting stents and radial access appear to provide robust benefits in the elderly. Advances in stent technologies are being actively evaluated, which may ultimately reduce the need for prolonged dual antiplatelet agents in the elderly.
References
-
Popitean L, Barthez O, Rioufol G, Zeller M, Arveux I, et al. (2005) Factors affecting the management of outcome in elderly patients with acute myocardial infarction particularly with regard to reperfusion. Data from the French regional RICO survey. Gerontology 51: 409-415.
-
Sheridan BC, Steams SC, Rossi JS, D'Arcy AP, Federspeil JJ, et al. (2010) Three-year outcomes of multivessel revascularisation in very elderly acute coronary syndrome patients. Ann Thorac Surg 89: 1889-1895.
-
Alexander KP, Newby LK, Cannon CP, Armstrong PW, Gibler WB, et al. (2007) Acute coronary care in the elderly, part 1: Non-ST-segment-elevation acute coronary syndromes: a scientific statement for healthcare professionals from the American Heart Association Council on Clinical Cardiology: in collaboration with the Society of Geriatic Cardiology. Circ 115: 2549-2569.
-
Singh M, Peterson ED, Roe MT, Ou FS, Spertus JA, Rusfeld JS, et al. (2009) Trends in the association between age and in-hospital mortality after percutaneous coronary intervention: National Cardiovascular Data Registry experience. Circ 2: 20-26.
-
Bauer T, Mollmann H, Weidinger F, Zeymer U, Seabra-Gomes R, et al. (2011) Predictors of hospital mortality in the elderly undergoing percutaneous coronary intervention for acute coronary syndromes and stable angina. Int J Cardiol 151: 164-169.
-
Murphy JC, Kozor RA, Figtree G, Hansen PS, Rasmussen HH, et al. (2012) Procedural and in-patient outcomes in patients aged 80 years or older undergoing contemporary primary percutaneous coronary intervention. EuroIntervention 8: 912-919.
-
McKellar SH, Brown ML, Frye RL, Schaff HV, Sundt TM 3rd (2008) Comparison of coronary revascularization procedures in octogenarians: a systematic review and meta-analysis. Nat Clin Pract Cardiovasc Med 5: 738-746.
-
Wang TY, Masoudi FA, Messenger JC, Shunk KA, Boyle A, et al. (2012) Percutaneous coronary intervention and drug-eluting stent use among patients >85 years of age in the United States. J Am Coll Cardiol 59: 105-112.
-
de Belder A, de la Torre Hernandez JM, Lopez-Palop R, O'Kane P, Hernandez Hernandez F, et al. (2014) A prospective randomized trial of everolimus-eluting stents versus bare-metal stents in octogenarians: the XIMA Trial (Xience or Vision Stents for the Management of Angina in the Elderly). J Am Coll Cardiol 63: 1371-1375.
-
Puymirat E, Mangiacapra F, Peace A, Ntarladimas Y, Conte M, et al. (2013) Safety and effectiveness of drug-eluting stents versus bare-metal stents in elderly patients with small coronary vessel disease. Arch Cardiovasc Dis 106: 554-561.
-
Badheka AO, Arora S, Panaich SS, Patel NJ, Patel N, et al. (2014) Impact on in-hospital outcomes with drug-eluting stents versus bare-metal stents (from 665,804 procedures). Am J Cardiol 114: 1629-1637.
-
Mangiacapra F, Ricottini E, Di Gioia G, Peace A, Patti G, et al. (2015) Comparison among patients ≥75 years having percutaneous coronary angioplasty using drug-eluting stents versus bare metal stents. Am J Cardiol 115: 1179-1184.
-
Jolly SS YS, Cairns J, Niemelä K, Xavier D, Widimsky P, et al. (2011) Radial versus femoral access for coronary angiography and intervention in patients with acute coronary syndromes (RIVAL): a randomised, parallel group, multicentre trial. Lancet 377: 1409-1420.
-
Ziakas A, Gomma A, McDonald J, Klinke P, Hilton D (2007) A comparison of the radial and the femoral approaches in primary or rescue percutaneous coronary intervention for acute myocardial infarction in the elderly. Acute Card Care 9: 93-96.
-
Achenbach S, Ropers D, Kallert L, Turan N, Krahner R, et al. (2008) Transradial versus transfemoral approach for coronary angiography and intervention in patients above 75 years of age. Catheter Cardiovasc Interv 72: 629-635.
-
Rodriguez-Leor O, Fernandez-Nofrerias E, Carrillo X, Mauri J, Labata C, et al. (2014) Results of primary percutaneous coronary intervention in patients >75 years treated by the transradial approach. Am J Cardiol 113: 452-456.
-
Hu F, Yang Y, Qiao S, Xu B, Liu H, et al. (2012) Comparison between radial and femoral approach for percutaneous coronary intervention in patients aged 80 years or older. J Interv Cardiol 25: 513-517.
-
Freixa X, Trilla M, Feldman M, Jimenez M, Betriu A, et al. (2012) Right versus left transradial approach for coronary catheterization in octogenarian patients. Catheter Cardiovasc Interv 80: 267-272.
-
Jinnouchi H, Sakakura K, Wada H, Kubo N, Sugawara Y, et al. (2012) Transradial percutaneous coronary intervention for acute myocardial infarction reduces CCU stay in patients 80 or older. Int Heart J 53: 79-84.
-
Foin N, Lee RD, Mario C, Virmani R, Wong P, et al. (2014) Impact of stent strut design in metallic stents and biodegradable scaffolds. Int J Cardiol 177: 800-808.
-
Onuma Y SP, Perkins LE, Okamura T, Gonzalo N, García-García HM, et al. (2010) Intracoronary optical coherence tomography and histology at 1 month and 2, 3, and 4 years after implantation of everolimus-eluting bioresorbable vascular scaffolds in a porcine coronary artery model: an attempt to decipher the human optical coherence tomography images in the ABSORB trial. Circulation 122: 2288-2300.
-
Ellis SG KD, Metzger DC, Caputo RP, Rizik DG, Teirstein PS, et al. (2015) Everolimus-Eluting Bioresorbable Scaffolds for Coronary Artery Disease. N Engl J Med 373:1905-1915.
-
Kereiakes DJ, Windecker S, Lee Jobe R, Mehta SR, Sarembock IJ, et al. (2015) Efficacy and safety of a novel bioabsorbable polymer-coated, everolimus-eluting coronary stent: the EVOLVE II Randomized Trial. Circ Cardiovasc Interv 8: 1-8.





