Journal of Obesity and Weight-loss Medication
Physical Exercise versus Natural Estrogen Supplement in Treatment of Metabolic Syndrome in Aged Postmenopausal Wistar Rats
Bahgat NM1, Saad RA2, Lasheen NN3* and Sabry YG2
1Professor of Physiology, Faculty of Medicine, Ain Shams University, Egypt
2Associate Professor of Physiology, Faculty of Medicine, Ain Shams University, Egypt
3Lecturer of Physiology, Faculty of Medicine, Ain Shams University, Egypt
4Demonstrator of Physiology, Faculty of Medicine, Ain Shams University, Egypt
*Corresponding author:
Noha N Lasheen, Lecturer of Physiology, Faculty of Medicine, Ain Shams University, Egypt, Email: nohalasheen@med.asu.edu.eg, nlashen@yahoo.com
J Obes Weight-Loss Medic, JOWM-2-011, (Volume 2, Issue 1), Research Article
Received: January 26, 2016: Accepted: February 23, 2016: Published: February 26, 2016
Citation: Bahgat NM, Saad RA, Lasheen NN, Sabry YG (2016) Physical Exercise versus Natural Estrogen Supplement in Treatment of Metabolic Syndrome in Aged Postmenopausal
Wistar Rats. J Obes Weight-Loss Medic 2:011.
Copyright: © 2016 Bahgat NM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The present study was performed to evaluate the effects of either a low intensity swim- exercise program or low soybean flour supplementation on the different components of metabolic syndrome in aged postmenopausal rats. Fifty five rats, weighing 260-350 gm, were randomly allocated into: Control group (C), Metabolic Syndrome group(MS), Metabolic syndrome 6-week - swim exercised group (MSE), and Metabolic syndrome 6 week -soybean flour supplemented group (MSS). All rats were followed weekly for assessment of body weight and arterial blood pressure which was found to be significantly increased in all metabolic syndrome groups (MS,MSE and MSS) compared to C group. At the end of the experimental period, all rats were subjected to measurement of arterial blood pressure. Biochemical analysis including plasma insulin and fibrinogen levels, and lipid profile was performed, then HOMA-IR and atherogenic index (AI) were calculated.
MS rats exhibited significant increase in their body weight gain (BWG), visceral fat (VF), visceral fat/ body weight ratio (VF/BW Ratio), arterial blood pressure values (ABP), as well as, plasma triglyceride level (TG) and AI compared to their controls. MSE group exhibited significant decrease in their BWG, VF, VF/BW Ratio and AI compared to MS group. The MSS had significantly decreased BMI, VF and VF/BW Ratio, ABP values, plasma TG and AI compared to MS group. Plasma levels of insulin and total cholesterol were significantly higher in MSS group compared to the MS group. MSE group showed normalization of the values of their BWG, VF, VF/BW Ratio. MSS group showed normalization of their BMI, VF and VF/BW Ratio. When the (MSS) group was compared to the MSE group, a significant increase in plasma insulin level was observed in addition to significant decrease in ABP values.
Conclusion:
Low dietary intake of soybean flour or low intensity swim- exercise program for 6 weeks were equally effective in normalizing visceral adiposity, but were partially effective as regards hypertriglyceridemia and hypertension in metabolic syndrome aged rats.
Keywords
Metabolic syndrome, Exercise, Soy bean, Aging, Adiposity
List of Abbreviations
AI: Atherogenic index, BW: Body weight, BWG: Body weight gain, Ch: Total cholesterol, CVD: Cardio-vascular diseases, DBP: Diastolic blood pressure, FB: Fibrinogen, FBG: Fasting blood glucose, BMI: Body mass index, FBW: Final body weight, HOMA-IR: Homeostasis model assessment of insulin resistance, MS: Metabolic syndrome- untreated group, MSE: Metabolic syndrome swim-exercised group, MSS: Metabolic syndrome soybean-supplemented group, SBP: Systolic blood pressure; TG: Triglycerides, VF: Visceral fat, WC: Waist circumference
Introduction
Metabolic syndrome (MS) is defined as a collection of risk factors including elevated blood levels of fasting glucose, total cholesterol, LDL- cholesterol, triglycerides as well as increased arterial blood pressure and central adiposity. It could be associated with increased risk for cardiovascular disease (CVD) and type 2 diabetes [1].
The prevalence of the metabolic syndrome was found to be higher in aged population particularly in females [2]. Moreover, the state of estrogen deficiency was reported to be associated with an increased risk for the development of MS [3] in addition to a higher androgen to estrogen ratio in postmenopausal women than premenopausal ones [4]. In addition, adipose tissue could produce several cytokines including leptin, adiponectin and IL-6 [5].
Soybean was reported by Barnes [6] to be the principal plant that produces the natural estrogens (phytoestrogens and isoflavones) and might be considered as a natural alternative to estrogen replacement therapy [6,7]. However, reports in literature about its health benefits were conflicting with some authors reporting favorable anti diabetic effect, body weight gain reduction, body composition improvement and amelioration of hypertension [8-10] and it was reported that, in a raw unprocessed form, soybeans contain a variety of enzymes and other biomolecules that could interfere with digestion and absorption of other nutrients [11]. Isoflavone molecules in soy could inhibit an enzyme involved in thyroid hormone synthesis [12].
On the other hand, life style intervention by increasing physical activity had become an important aspect of a non-pharmacological strategy to control obesity, weight gain, insulin resistance, glucose intolerance and dyslipidemia, independent of the changes in body fat content [13,14]. This was further confirmed by Seo et al. [15] who reported that exercise was a good method for preventing MS as it increased muscle mass, decreased percent body fat and body weight, controlled diabetes, reduced blood pressure, and reduced overall cardiovascular risk factors.
However, some authors reported that the harmful effects of overeating, smoking and other physical abuses cannot be corrected by exercise alone [16], and that although exercise training might increase cardio-respiratory fitness, yet it had no independent effect on insulin sensitivity [17]. This was explained by Sostaric et al. [18] that the highly aerobic muscle stimulation under anaerobic conditions might generate a large amount of reactive oxygen species that could disrupt mitochondrial and cellular functions.
Therefore, it was intriguing to investigate and compare the effects of natural estrogen supplementation and life style intervention in the form of physical exercise program on the different components of metabolic syndrome in aged postmenopausal female rats.
Aim of the Work
The present study aimed at evaluating the long term effects of implementing a swim- exercise program and soybean flour supplementation in diet on the various components of the metabolic syndrome in aged female rats.
Materials and Methods
Experimental animals
This study was carried out on 55 aged female Wistar rats, initially weighing 250-280 gm (age of rats was between 15-21 months). Rats were purchased from Ophthalmic Diseases Research Institute (Giza) and were housed in the Physiology Department Animal House, Faculty of Medicine, Ain Shams University under standard conditions of boarding at room temperature 22 ± 1°C. Rats were kept in plastic cages (3-4 rats /cage) for one week for acclimatization. Regular meals were introduced daily at 8:00h. Rats were fed water ad libitum and standard rat chow diet (every Kg rat chow consisted of 400ml milk, 600g balady bread and vegetables). This study was approved by the Ethics Committee of Faculty of Medicine, Ain Shams University.
Age of rats was calculated according to the following equation:
Age in months = {Body weight in grams X 0.0675} -1.9 [19].
Experimental protocol
All rats were checked for estrous cycle activity by vaginal swabs and all rats showing estrous cycle activity were excluded. The included menopausal rats were randomly allocated into the following experimental groups:
Group I: Control group (n = 13): Rats in this group were fed standard rat diet throughout the study.
Group II: Metabolic Syndrome group (n = 42): They were allowed to drink10% fructose solution (10 gm fructose dissolved in 100 ml distilled water) for 8 weeks to induce metabolic syndrome [20].
At the end of the 8th week, rats were subdivided into
A. Metabolic syndrome- untreated rat group (n = 13). They continued drinking the 10% fructose solution till the end of the study. On the 9th week of the study, those rats were subjected to 5 minute water immersion before each swimming session of the swim-exercised (MSE) rat group.
B. Metabolic syndrome swim-exercised rat group (n = 15). Rats in this group continued drinking the 10% fructose solution till the end of the study and were subjected to swim exercise program, 2 hours daily, 5 days a week, for 6 weeks. The 2-hour swimming session was considered a low intensity long term exercise program according to Koshinaka et al. [21].
C. Metabolic syndrome soybean-supplemented rat group (n = 14).They continued drinking the 10% fructose solution till the end of the study and were fed standard rat chow supplemented with 10% soybean flour for 8 weeks [22]. Soybean flour (consisted of 48% soybean protein and 6% fat) was purchased from Soybean product factory, Food Technology Research Institute, Agricultural Research Center, Giza, Egypt. Wang and Murphy [23] reported that commercially available soy products, such as soy flour and textured protein, contain 0.1-5 mg isoflavones/gm protein.
Throughout the experimental period, both water intake and food intake were evaluated daily to each cage and divided by the rat number in the cage to ensure that all rats received adequate water and food per day. Also, all rats were subjected to weekly assessment of:
1. Body weight and body mass index (BMI)
2. Arterial blood pressure (ABP)
At the end of the induction period of metabolic syndrome (8th week), all rats were subjected to measurement of arterial blood pressure and waist circumference. On the day before the sacrifice day, intraperitoneal glucose tolerance test was performed.
On the day of sacrifice, overnight fasted rats were weighed and anaesthetized by intra-peritoneal injection of Pentobarbitone (40 mg/kr BW). All anthropometry measures (nasoanal length, waist circumference and final BMI) were determined. Then, a midline abdominal incision was made, and blood samples were collected from the abdominal aorta into flouride containing tube and heparinized tube. The abdominal fat (retroperitoneal, perirenal and mesenteric) was excised and weighed in 5-digit Metler balance (Sartorius AG, BL-210S).
Blood samples were centrifuged at 4000 rpm for 15 minutes to obtain plasma samples. The fluoride containing plasma was used to determine fasting blood glucose (FBG) on the same day of sacrifice. The heparinized plasma was stored at -80°C for later determination of plasma insulin, lipid profile and fibrinogen level. Then, the homeostasis model assessment of insulin resistance (HOMA-IR) and the atherogenic index (AI) were calculated.
Experimental procedures
Because female sex hormones confer protection against metabolic syndrome [24] all rats were checked for estrous cycle activity by vaginal swabs and all rats showing estrous cycle activity were excluded.
Vaginal swab: Vaginal smears were carried out to monitor cellular differentiation and to evaluate the presence of leucocytes, nucleated epithelial cells, or cornified cells. Aged female rodents exhibit periods of persistent estrous associated with low levels of progesterone and tonic blood titres of estrogen which stimulates cornification of the vaginal epithelium and acyclic state [25].
In menopausal rats, the vaginal smear showed an atrophic pattern consisting of leucocytes, mucus and scarce nucleated epithelial cells (Figure 1a), while fertile rat's vaginal smears consisted mainly of exfoliated cornified cells (Figure 1b) [26]. Thus, the fertile rats were excluded and the menopausal rats were included in the study.
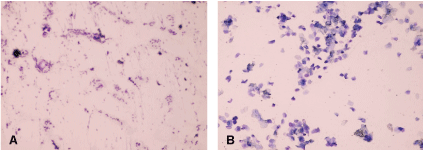
.
Figure 1: (a) Microscopic examination of vaginal swab in aged premenopausal rat showing large number of vaginal epithelial cells and few leukocytes (400x); (b) Microscopic examination of vaginal swab in aged postmenopausal rat showing scarcity of cells due to vaginal desquamation and many leukocytes (400x).
View Figure 1
Swimming training protocol: The protocol of swim - training was 2 hours swimming a day between 10-12 AM, 5 days/week for 6 weeks. At the beginning of every swimming session, sedentary control rats were immersed in water for 5 minutes, then the metabolic syndrome swim-exercised rats were put in water and were urged to swim actively all the time. In the first week of the swimming program, the duration of the swimming session was prolonged gradually from 20 minutes in the first day to 120 minutes by the fifth day for accommodation modified from Liu et al. [27]. Water was maintained at a thermoneutral temperature 30 ± 2°C. Water was emptied from the tank after each swimming session and the tank was thoroughly cleaned.
Determination of Body Mass Index (BMI): It was calculated according to the following equation:
BMI = Body weight (gm)/ length (cm2) [28].
Measurement of arterial blood pressure: The rat arterial blood pressure was measured using non-invasive small animal tail blood pressure system (NIBP200A, Biopac systems Inc; USA).
Intraperitoneal glucose tolerance test: It was performed according to Kennaway et al. [29] by using Uni-Check blood glucose test strips. The apparatus was calibrated using the bar code film strip. Rats were fasted for six hours by moving to a clean cage without food at the end of their dark cycle, then they were weighed. Fasting blood glucose level was estimated. A glucose challenge dose (1 gm glucose/Kg BW) dissolved in distilled water, was injected intraperitoneally. Blood glucose values were estimated using the rat tail blood at 30, 60 minutes.
Measurement of fasting blood glucose level: It was assayed by enzymatic oxidation according to Tietz [30] using liquizyme glucose reagent kits (Spectrum Diagnostics) supplied by Egyptian Company for Biotechnology.
Measurement of plasma insulin level: It was determined by enzyme-linked-immunosorbent assay (ELISA) method according to Bowsher et al. [31] using insulin kit supplied by Abnova, Egypt.
HOMA-IR was calculated according to Bonora et al. [32] as follows:
HOMA-IR = [fasting plasma insulin (μU/mL) x fasting plasma glucose (mmol/L)/22.5].
(Blood glucose was converted from mg/dl unit to mmol/L by dividing on 18).
Determination of plasma fibrinogen level: It was performed by ELISA according to a method describedby Bach-Gansmo et al. [33], using kit supplied by Assaypro.
Determination of plasma triglycerides level: This was performed according to the method described by Vassault et al. [34] using kits supplied by Greiner Diagnostic, Germany.
Determination of plasma total cholesterol: This was performed according to the method described by Rifai et al. [35] using kits (CHOD-PAP) supplied by Greiner Diagnostic, Germany.
Determination of plasma LDL-cholesterol: This was performed using a method described by (Rifai et al. [35] using kits supplied by Greiner Diagnostic, Germany.
Determination of plasma HDL-cholesterol: This was performed according to the method described by Fruchart [36], using kits supplied by Greiner Diagnostic, Germany.
Determination of plasma IL-6: Using Rat IL-6 ELISA kit (Immuno-Biological Laboratories, Inc.) (IBL-America).
Calculation of Atherogenic index: The atherogenic index was calculated according to Grundy et al. (1987) as follows: Atherogenic index = Total cholesterol / HDL-C [37].
Statistical Analysis
All results in the present study were expressed as mean ± SE of the mean. Statistical Package for the Social Sciences (SPSS, Inc., Chicago, IL, USA) program, version 16.0 was used. Differences were considered significant when P ≤ 0.05.
Correlations and Lines of Regression were calculated by linear regression analysis using the Least Square Method. A probability of (P < 0.05; 2tailed) was considered statistically significant.
Ethics Committee
This study was approved by the Ethics Committee of Faculty of Medicine, Ain Shams University.
Results
Throughout the 14 week-study period, no deaths were observed in control group, one rat died from the metabolic syndrome (MS) and metabolic syndrome soybean flour- supplemented (MSS) rat groups (death ratio; 7%). On the other hand, 5 rats died from the metabolic syndrome swim- exercised (MSE) rat group with a death ratio 30% due to drowning. The final number (n) of rats in the four studied rat groups was control group (n = 13), MS (n = 12), MSE (n = 10) and MSs (n = 13).
On the 8th week of the study before starting the intervention programs (swim-exercise program and the soybean flour supplementation in diet)
All rats with metabolic syndrome (MS, MSE and MSS) showed insignificant changes in their body weight, body mass index and waist circumference when compared to the control (C) rat group. However, they showed significantly higher systolic, diastolic and mean arterial blood pressure values when compared to the control group (153.11 ± 1.19 versus 132.07 ± 1.04; 86.57 ± 0.84 versus 80.3 ± 0.83; 108.75 ± 0.72 versus 97.56 ± 0.76, P < 0.001, P < 0.002, P < 0.001, respectively) (Table 1).
![]()
Table 1: Changes in systolic blood pressure (SBP, mmHg), diastolic blood pressure (DBP, mmHg) and mean arterial blood pressure (MAP, mmHg), body weight (BW, gm), body mass index (BMI) and waist circumference (WC7w) in the 8th week in control group (C) and all metabolic syndrome (MS, MSE and MSS) groups.
View Table 1
Anthropometry measures at the end of experimental period
Final body weights and body mass indices were not significantly different in metabolic syndrome (MS) group compared to control group. However, MS rats showed significant increase in their body weight gain, visceral fat weight and visceral fat / body weight ratio compared to the control group (57.5 ± 12.3 versus 30 ± 6.9; 29.29 ± 3.19 versus 21.85 ± 2.9 and 0.09 ± 0.008 versus 0.07 ± 0.008; P < 0.05) (Figure 2).
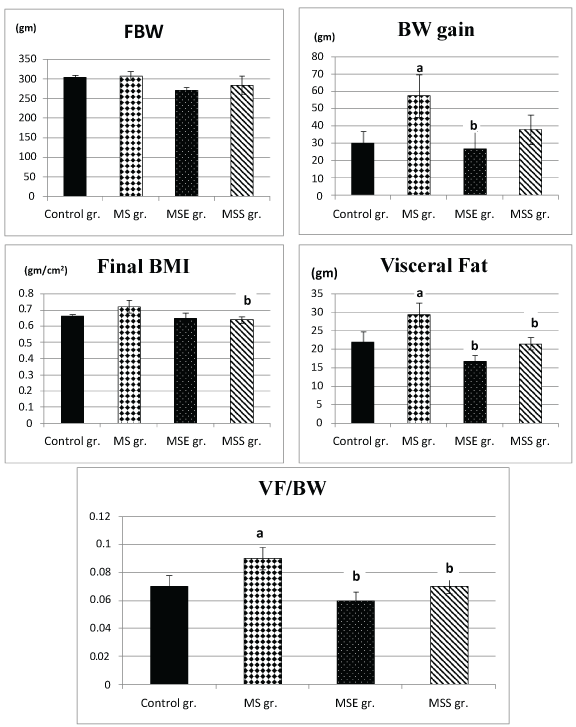
.
Figure 2: Anthropometry changes in the different studied groups. (a) Significance by LSD at P < 0.05 from control group; (b) Significance by LSD at P < 0.05 from metabolic syndrome group.
View Figure 2
Metabolic syndrome swim-exercised (MSE) group exhibited insignificant changes in their final body weight and body mass index compared to metabolic syndrome (MS) group, however, their body weight gain, visceral fat weight and visceral fat /body weight ratio were significantly decreased compared to MS group becoming insignificantly different from control group (27 ± 10.01 versus 57.5 ± 12.3; 16.7 ± 1.59 versus 29.29 ± 3.19 and 0.06 ± 0.006 versus 0.09 ± 0.008; P < 0.05, P < 0.001, P < 0.01, respectively) (Figure 2).
On the other hand, metabolic syndrome soybean flour-supplemented group (MSS) had insignificant changes in their final body weight and body weight gain compared to metabolic syndrome (MS) rat group. However, their body mass index, visceral fat and visceral fat/ body weight ratio were significantly decreased compared to MS rat group becoming insignificantly different from control group (0.64 ± 0.02 versus 0.72 ± 0.04; 21.5 ± 1.59 versus 29.29 ± 3.19 and 0.07 ± 0.005 versus 0.09 ± 0.008; P < 0.05). Body weight, body weight gain, body mass index, visceral fat and visceral fat/body weight ratio were not significantly different between MSS and MSE groups (Figure 2).
Changes in arterial blood pressure
Systolic, diastolic and mean arterial blood pressure values showed significant increase in metabolic syndrome (MS) group compared to control group (153.58 ± 0.95 versus 133.76 ± 0.32; 91.92 ± 1.2 versus 80.5 ± 0.84 and 112.47 ± 0.98 versus 98.28 ± 0.51; P < 0.001). Metabolic syndrome swim-exercised (MSE) group exhibited insignificant change in their systolic, diastolic and mean arterial blood pressure values compared to metabolic syndrome (MS) group, remaining significantly higher than control group values (154.1 ± 1.42 versus 133.76 ± 0.32; 89.4 ± 1.3 versus 80.5 ± 0.84 and 110.9 ± 1.16 versus 98.28 ± 0.51; P < 0.001) (Figure 3).
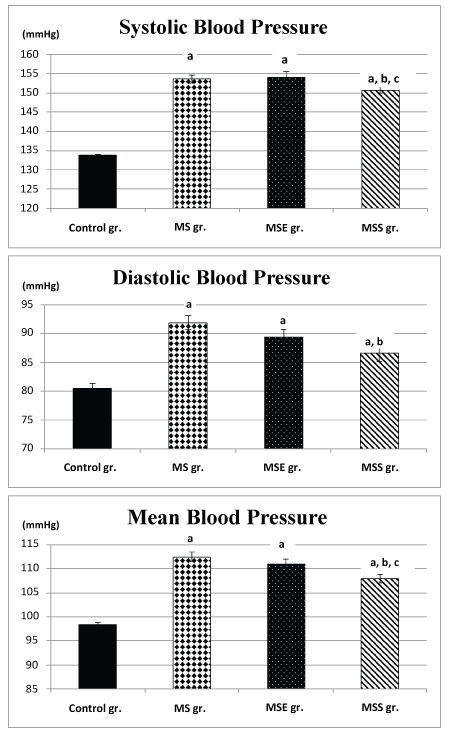
.
Figure 3: Changes in systolic, diastolic and mean pressure values in the different studied groups. (a) Significance by LSD at P < 0.05 from control group; (b) Significance by LSD at P < 0.05 from metabolic syndrome group; (c) Significance by LSD at P < 0.05 from metabolic syndrome swim- exercised group.
View Figure 3
On the other hand, metabolic syndrome soybean flour-supplemented group (MSS) showed significant decrease in their systolic, diastolic and mean arterial blood pressure values compared to metabolic syndrome (MS) group (150.7 ± 0.84 versus 153.58 ± 0.95; 86.6 ± 1.4 versus 91.92 ± 1.2 and 107.97 ± 0.95 versus 112.47 ± 0.98; P < 0.05, P < 0.005, P < 0.001, respectively). However their systolic, diastolic and mean arterial blood pressure values remained significantly higher than control group values (150.7 ± 0.843 versus 133.76 ± 0.32; 86.6 ± 1.4 versus 80.5 ± 0.84 and 107.97 ± 0.95 versus 98.28 ± 0.51; P < 0.001, P < 0.001, P < 0.0001, respectively).When MSS rat group was compared to MSE rat group, systolic blood pressure and mean arterial blood pressure values were found to be significantly decreased (150.7 ± 0.84 versus 154.1 ± 1.42; 86.6 ± 1.4 versus 89.4 ± 1.3 and 107.97 ± 0.95 versus 110.96 ± 1.16; P < 0.01, P < 0.02, P < 0.0001, respectively), although, the diastolic blood pressure value was not significantly changed (Figure 3).
Fasting blood glucose level, plasma insulin level and the homeostasis model assessment of insulin resistance (HOMA-IR)
Fasting blood glucose levels and HOMA-IR were not significantly different in metabolic syndrome (MS) group compared to control (C) group and were not significantly changed in either metabolic syndrome swim- exercised (MSE) group or metabolic syndrome soybean flour-supplemented (MSS)group when compared to MS group and when compared to each other (Table 2). Similarly, plasma insulin levels were not significantly different in metabolic syndrome (MS) group when compared to control (C) group and were not significantly changed in metabolic syndrome swim-exercised (MSE) group when compared to MS group. However, metabolic syndrome soybean-flour (MSs) group showed highly significant increase in their plasma insulin levels when compared to MS, MSE and the control (Table 2).
![]()
Table 2: Changes in fasting blood glucose (BGf, mg/dl), plasma insulin level (µU/ml), HOMA-IR, fibrinogen level (FB, μgm/ml) and interleukin6 (IL6) (pg/ml)in the different studied groups.
View Table 2
Also, as shown in table 3, intraperitoneal glucose tolerance test showed that significantly higher fasting blood glucose level only in metabolic syndrome compared to the control group while insignificant changes were observed in metabolic syndrome swim- exercised (MSE) group and metabolic syndrome soybean flour-supplemented group when either compared to control group or metabolic syndrome group or to each other (Table 2).
![]()
Table 3: Intraperitoneal glucose tolerance test in all studied groups.
View Table 3
Blood glucose after 30 min was significantly reduced in metabolic syndrome swim- exercised (MSE) group compared to metabolic syndrome group, while non-significant changes were present when comparing treated or untreated metabolic syndrome groups to control group or to each other (Table 2).
Blood glucose after 60 min was significantly reduced in metabolic syndrome swim- exercised (MSE) group and in metabolic syndrome soybean flour-supplemented group compared to metabolic syndrome group. Non-significant changes were obtained when comparing the blood glucose after 60 min in MSE and MSS groups and when comparing all metabolic syndrome groups with the control group (Table 2).
Changes in plasma fibrinogen level
Plasma fibrinogen levels were not significantly different in metabolic syndrome (MS) group compared to control group and were not significantly changed in either metabolic syndrome swim- exercised (MSE) group or metabolic syndrome soybean-flour supplemented group (MSS) when compared to MS or control groups and when compared to each other (Table 2).
Changes in plasma IL6 level
Plasma IL6 level was significantly increased in metabolic syndrome (MS) group, metabolic syndrome swim- exercised (MSE) group and metabolic syndrome soybean-flour supplemented group (MSS) compared to control group. It was significantly lowered in MSE group and in MSS when compared to MS. However, non-significant changes were observed in MSS compared to MSE (Table 2).
Changes in plasma lipid profile and atherogenic index (AI)
Metabolic syndrome (MS) group showed significantly higher values of plasma triglyceride level and atherogenic index compared to control group (120.9 ± 13.68 versus 47.1 ± 4.8; P < 0.001) and (6.69 ± 2.15 versus 2.28 ± 0.41; P < 0.5), respectively. However, their plasma levels of total cholesterol, HDL-cholesterol and LDL-cholesterol were not significantly different from their control group values (Figure 4).
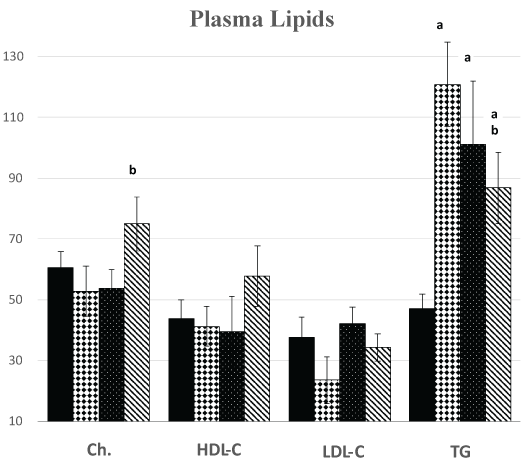
.
Figure 4: Changes in plasma lipid profile [total cholesterol (Ch., mg/dl), high density lipoprotein cholesterol (HDL-C, mg/dl), low density lipoprotein cholesterol (LDL-C, mg/dl)] in the different studied groups. (a) Significance by LSD at P < 0.05 from control group (C); (b) Significance by LSD at P < 0.05 from metabolic syndrome group (MS).
View Figure 4
Although metabolic syndrome swim-exercised (MSE) group didn’t show significant changes in their plasma levels of total cholesterol, HDL-cholesterol, and LDL-cholesterol from MS group values, MSE group exhibited significant decrease in their atherogenic index (1.4 ± 0.15 versus 6.69 ± 2.15, P < 0.01) becoming not significantly different from control group values. On the other hand, plasma triglyceride level of MSE group showed insignificant decrease from MS group value, remaining significantly higher than control group values (101.1 ± 20.82 versus 47.1 ± 4.8, P < 0.01) (Figure 4).
Despite metabolic syndrome soybean flour- supplemented group (MSS) had non-significant changes in plasma levels of HDL-cholesterol and LDL-cholesterol compared to MS group, their plasma total cholesterol level was significantly higher than the MS group (75.08 ± 8.91 versus 52.9 ± 8.25, P < 0.05), being not significantly different from control group values. Atherogenic index in MSS group exhibited significant decrease compared to MS group (2.64 ± 0.60 versus 6.69 ± 2.15, P < 0.05), and being not significantly different from control group. Plasma triglyceride level showed significant decrease in MSS group than MS group (86.85 ± 11.72 versus 120.9 ± 13.86, P < 0.05), although still significantly higher than control group level (86.85 ± 11.72 versus 47.1 ± 4.8, P < 0.05). However, when MSS group was compared to MSE group, no significant difference was found in any parameter of plasma lipid profile (Figure 4).
Correlations
Correlation study in the different studied groups revealed a significant positive correlation between absolute and relative weights of visceral fat (VF and VF/BW ratio) and fasting blood glucose level in both MS and MSS groups. Also, there was a significant positive correlation between absolute and relative weights of visceral fat (VF and VF/BW ratio) and HOMA-IR only in MS group (Table 4 and Table 5).
![]()
Table 4: Correlations of visceral fat (VF) weight to fasting blood glucose (FBG) and HOMA-IR in the different studied groups.
View Table 4
![]()
Table 5: Correlations of visceral fat /body weight (VF/BW) ratio to fasting blood sugar and HOMA-IR in the different studied groups.
View Table 5
Discussion
In the present study, metabolic syndrome rats showed significant hypertension on the 8th week of the study, but no significant changes were observed as regards their body weight, body mass index and waist circumference from control values. Similarly, Bahgat and Soliman [38] found insignificant changes in body weight, BMI in fructose induced metabolic syndrome in aged Wistar rats. This might be attributed to the fact that both metabolic syndrome (MS) and control rats in the present study were aged and menopausal. Both aging and menopause independently induce some features of the metabolic syndrome as reported by Ghezzi et al. [39], who stated that aging in Wistar rats triggered metabolic syndrome, as well as, Guerra et al. [40], who demonstrated that metabolic syndrome could be produced in young rats by induction of menopause by ovariectomy. Also, studies of animal models develop a complete case of metabolic syndrome, including all risk factors, are rare. Aging process could lead to the manifestation of metabolic syndrome symptoms in rodents; however, manifestation differs between rat strains [39]. In addition, fat distribution could be more closely linked to metabolic disorders than total body weight, and fat distribution was found to be even more significant in older individuals [41].
However, by the end of the study, metabolic syndrome rats exhibited significant body weight gain, visceral obesity, hypertension and hypertriglyceridemia compared to the controls, although their food consumption was not comparable throughout the study. Stabilized food intake was observed in the current study after 8 weeks similar to the studies of Morley [42], Takano et al. [43] and Ghezzi et al. [39]. Rats ate more during accelerated body growth similar to human beings, with subsequent stabilization. Thus, the increased weight gain and mesenteric fat in animals could not be related to the increased food intake [39].
Lifestyle intervention by the swim-exercise program or soybean flour supplementation in diet caused MSE and MSS rats to show significant decrease in their visceral adiposity, plasma triglycerides and atherogenic index compared to MS group. Blood pressure values showed significant decrease in MSS group, but remained insignificantly different from MS group values in the MSE group. Therefore, lifestyle intervention, implemented in the present study, could normalize some features of the metabolic syndrome like visceral adiposity but couldn’t completely normalize hypertension or hypertriglyceridemia.
Lewis et al. [44] reported that dietary fructose increases triglyceride production by enterocytes in the form of chylomicrons. Fructose disposal by hepatocytes is mainly in the form of lactate, glucose and fatty acids which become incorporated into very-low-density lipoprotein (VLDL)-palmitate [45]. Fructose, by providing large amounts of hepatic triose-phosphate as precursors for fatty acid synthesis, is highly lipogenic together with fructose contribution to the synthesis of both the glycerol- and the fatty-acyl parts of VLDL-triglycerides [45].
Moreover, hepatic insulin resistance and disturbed lipid metabolism could contribute to insulin resistance and impaired glucose tolerance because hepatic insulin resistance causes glucose production by the liver to be less suppressed by insulin leading to hyperinsulinemia and hyperglycemia which are primary events in the development of metabolic syndrome in animal models [46]. Hyperinsulinemia contributes to hypertension by increasing sympathetic nervous system activity, enhancing renal sodium reabsorption and accumulating intracellular aldehydes, thereby, impairing the function of L-type calcium channels leading to an increased intracellular calcium concentration in vascular smooth muscle, and increased vascular resistance [47-49].
In the present study, metabolic syndrome (MS) rats didn’t exhibit significant fasting hyperglycemia or insulin resistance when compared to control rats. Wistar rats at age of twenty-four months were found to have similar blood insulin and blood glucose levels as three-month-old adult rats [50], despite increased body weight and adipocyte hypertrophy [51]. However, intraperitoneal glucose tolerance test revealed significant fasting hyperglycemia only in metabolic syndrome group compared to the control group, despite non-significant changes in 30 min and 60 min readings. This could be attributed at least partially to the already high fasting blood glucose levels in the control rats because of aging and menopause [52].
Nevertheless, a significant positive correlation between absolute and relative weights of visceral fat and fasting blood glucose levels, as well as, the HOMA-IR were observed in the metabolic syndrome (MS) rat group. This finding was in line with the report of The Third Report of The National Cholesterol Education Program [53] that visceral adiposity is the cornerstone of the pathogenesis of metabolic syndrome resulting in insulin resistance. In addition, Tappy and Lê [54] reported that fructose could be linked to insulin resistance through altered lipid metabolism and lipotoxicity secondary to stimulation of de novo lipogenesis, or by fructose induced oxidative stress.
Also, the intraperitoneal glucose tolerance test showed significant lower 30 min and 60 min readings in swim-exercised trained metabolic syndrome compared to metabolic syndrome group. However, metabolic syndrome soybean-supplemented (MSS) group had only significantly lowered 60 min reading compared to metabolic syndrome group. This could be attributed to the positive correlation between absolute and relative weights of visceral fat and fasting blood glucose persisted in the metabolic syndrome soybean-supplemented (MSS) rat group, while the positive correlation between absolute and relative weights of visceral fat and HOMA-IR was abolished, possibly because MSS rats exhibited significant decrease in their visceral fat weights and significant hyperinsulinemia. Neither the controlnor the swim-exercised rat (MSE) groups showed significant positive correlations between visceral fat weights and fasting blood glucose or HOMA-IR, the index of insulin resistance.
The relationship between high fructose intake and visceral obesity was reported by Pollock et al. [55] and was attributed by Khitan and Kim [56] to be due to postprandial hypertriglyceridemia, and by Bursac et al. [57] to be due to alterations of glucocorticoid signalling in both hypothalamus and adipose tissue resulting in enhanced adipogenesis, possibly serving as an adaptation to energy excess in order to limit deposition of fat in non-adipose tissues.
In the present study, MS rats had significant hypertriglyceridemia when compared to control group although non- significant changes in fasting blood glucose were observed in MS rats. Similarly, Botezelli et al. [58,59] reported that fructose induced metabolic syndrome in rats was found to be manifested as altered lipid metabolism more than glucose alterations.
Also, visceral fat was reported to be hyperlipolytic and more resistant to the antilipolytic effect of insulin than subcutaneous fat [60], being an important source of free fatty acids and inflammatory mediators, such as TNF-α, interleukins (IL) and adipokines, which were directly delivered to the liver via the portal vein, affecting hepatic glucose and fat metabolism, and possibly contributing to the development of hepatic insulin resistance [61].
The metabolic features observed in MS, MSE and MSS groups could be attributed to the significant higher plasma IL6 level according to the study of Brunner et al. [62].
Both TNF-α and IL-6, released from visceral fat, were considered to cause insulin resistance. TNF-α could cause it directly by down-regulating insulin receptor substrate 1 (IRS-1), inducing serine phosphorylation of IRS-1 and by decreasing glucose transporting protein-1 (GLUT-1), while IL-6 could cause insulin resistance by decreasing the activation of IRS-1 [63]. In the present study, although hepatic insulin resistance was not assessed, yet its manifestations like hypertriglyceridemia as reported by Sparks et al. (2012) was evident in all groups with metabolic syndrome (MS, MSE and MSS) [64].
It is worth noting that aging process might be overwhelming the metabolic syndrome features in this study. Spencer et al. [65] reported that at or after the menopause, there could be increased total cholesterol and triglycerides; lowered HDL and HDL subfraction 2; increased LDL and lipoprotein A; increased insulin resistance; decreased insulin secretion; decreased insulin elimination; increased android fat distribution; impaired vascular function; increased factor VII and fibrinogen, and reduced sex-hormone binding globulin. Therefore, the non-significant changes observed in MS group compared to control group could be due to the metabolic features developed in postmenopausal period. Imperatore et al. [66] suggested that hyperfibrinogenemia could be a component of the metabolic syndrome, thus it was evaluated in the current study.
Therefore, the rats of MS developed 3 criteria of metabolic syndrome by the end of experimental period which were hypertension, increased triglycerides, significant weight gain and visceral fat increase compared to control rats. However, the MSE and MSS groups developed hypertension and hypertriglyceridemia with decreased visceral adiposity and less weight gain when each group compared to control group.
The physical exercise program implemented in the present study normalized visceral obesity in MSE rats and improved dyslipidemia as evidenced by normalization of the atherogenic index and amelioration of hypertriglyceridemia. This was in agreement with the results of Damirchi et al. [67] and Mostarda et al. [68], although they used higher exercise- intensity programs. These favourable effects might be attributed to increased utilization of fructose as an energy source during exercise, thus decreasing fructose load in the blood [69]. Also, it might be suggested that by targeting the visceral adiposity in MSE rats, accompanied by significantly reduced IL6, the physical exercise program could reverse or alleviate the events that ensued from visceral obesity and led to hepatic insulin resistance. Irving et al. [70] reported that there is a preferential loss of visceral fat with aerobic exercise possibly by inducing secretion of lipolytic hormones, facilitating greater post-exercise energy expenditure and fat oxidation, and by favouring a greater negative energy balance [71].
Soy bean flour is one of the less processed soybean products that are less likely to induce soybean side effects. The present study, also, demonstrated that diet supplementation with soybean flour was effective in improving almost all the criteria of the metabolic syndrome that were observed in the non-supplemented metabolic syndrome (MS) group (namely body mass index, visceral obesity, arterial blood pressure, plasma triglycerides and atherogenic index), which agreed with the findings of Hamed et al. [72] and Barrios-Ramos et al. [73]. The improving of these features could be partially due to decreased plasma IL6.
The favourable effects of soybean flour on the metabolic syndrome markers in MSS group might be because it targeted the main pathogenic mechanism of metabolic syndrome (visceral adiposity), thus reversing or alleviating the deleterious consequences ensuing from visceral obesity which are increased free fatty acid flux to the liver and increased hepatic synthesis of triglycerides, hepatic and peripheral insulin resistance and hypertension.
The anti adipogenic effect of soybean particularly on the visceral fat was consistent with the findings of Hamed et al. [72], possibly by down regulating the adipogenesis -related genes [74].
Soybean flour is a raw product of soybeans that contain many ingredients like proteins (~ 50%) , fibers, polyunsaturated fatty acids, phytoestrogens like isoflavones (an estrogen- like molecule), genistein, daidzein and glycitein lignin, saponins and sterols with some of them having antioxidant capacity [75]. These components could contribute to the favorable effects of soybean flour on triglyceride and arterial blood pressure.
The significantly high plasma insulin level in soybean flour-supplemented group than MS, MSE and control groups might contribute to the significant decrease in plasma triglyceride level. This insulinotropic effect of soybean was consistent with the findings of Feres et al. [76] and Yang et al. [77]. The soybean constituent involved in this insulinotropic effect was suggested to be its isoflavonoid aglycones and small peptides [78]. Moreover, soybean feeding might affect insulin sensitivity and lipid homeostasis via altered signalling in the liver through promiscuous nuclear receptors, including peroxisome proliferator-activated receptors [PPAR] either PPARα and/or PPARγ [79] or through other transcription factors, such as the sterol regulatory element binding protein [8].
The triglyceride - lowering effect of soybean flour in MSS rats was consistent with the findings of Andrade et al. (2013), who explained it to be due to decreased liver fat content and increased intestinal peristalsis [80]. Soybean protein and isoflavones might be involved in the triglyceride lowering effect of soybean flour as reported by Cederroth and Nef [81]. Isoflavones, which are the main phytoestrogens in soybean bind with its receptors, could exert an estrogen-like effect on plasma lipids in the form of decreasing total cholesterol, particularly in the LDL fraction, VLDL and triglycerides, as well as, elevating HDL-C [82]. However, in the current study, HDL-C was insignificantly increased when compared to control group.
The blood pressure lowering effect of soybean flour supplementation in diet was also explained by Yang et al. [83] to be caused by its protein component which has inhibitory effect on angiotensin II-converting enzyme. In addition, Genistein treatment, a soy derived isoflavone, caused decrease in SBP, plasma lipids and insulin resistance together with increased HDL cholesterol in postmenopausal metabolic syndrome in rat. This could be through affecting PPAR involved in regulation of insulin sensitivity, adipogenesis, lipid metabolism, inflammation, and blood pressure [84]. Bragt and Popeijus [85] mentioned that synthetic PPARs agonists, such as fibrates and thiazolidinediones could treat metabolic disturbances such as hyperlipidemia and diabetes mellitus, both typical features of metabolic syndrome. Moreover, genistein could act as an estrogen receptor (ER) agonist in a low estrogenic state and as antagonistin an estrogenic excess, in which it could be ligand for PPAR determining antiestrogenic effects leading to adipogenesis [86]. The balance between the activation of ERs and PPARγ could be related to the genistein concentration and this might account for the different obtained results in significant higher total cholesterol in MSS compared to MS. Also, this higher cholesterol level in MSS group compared to MS group could be due to either insignificant increase in HDL-C fraction [82] or due to excessive soy-protein intake which was mentioned to do more harm than good [87]. In addition, Soy-protein feeding in mini pigs caused increase in the total, free thyronine and postprandial growth hormone [88], partly affecting cholesterol concentrations by soy protein.
In contrast to rodents, humans need very high fructose consumption to develop metabolic syndrome. However, bad dietary habits in the form of consumption of sweetened beverages, containing either sucrose or a mixture of glucose and fructose, were associated with increased food intake because fructose causes less satiation than glucose [89]. This might result in increased body weight, visceral obesity, increased intrahepatic lipids, dyslipidemia, insulin resistance and hypertension [54]. This, together, with an abnormal life style in the form of high caloric diet and low physical activity would result in development of the metabolic syndrome.
The present study showed that either low dietary intake of soybean flour or low intensity physical exercise program was effective in normalizing visceral adiposity and atherogenic index as an aspect of dyslipidemia. Also, they alleviated the other features of the metabolic syndrome like hypertriglyceridemia, possibly by targeting visceral adiposity as the initiating pathology of metabolic syndrome. The results, also, showed that the soybean flour intake was more effective in decreasing the metabolic syndrome-associated hypertension than the physical exercise program.
Conclusion
The present study showed that low dietary intake of soybean flour or low intensity swim- exercise program were completely and equally effective in normalizing visceral adiposity, the main pathogenic event of metabolic syndrome, but were partially effective as regards hypertriglyceridemia and variably effective as regards the hypertension with no significant effect of the swim-exercise program and partial improvement by the soybean flour dietary intake, possibly by decreasing plasma IL6. The results of the current study demonstrate two natural lifestyle interventions that can be used to manage the metabolic syndrome according to its features in every patient.
Further studies are recommended to evaluate the effects of the physical exercise program and soybean flour dietary intake on the different features of the metabolic syndrome, particularly other grades of exercise intensity and various soybean ingredients and/or their combination.
Conflict of Interest
The authors declared no conflict of interest in this study.
Funding
This study was funded only by the authors, without any source of funding from any institute.
References
-
Alberti KG, Eckel RH, Grundy SM, Zimmet PZ, Cleeman JI, et al. (2009) Harmonizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 120: 1640-1645.
-
Ogbera AO (2010) Prevalence and gender distribution of the metabolic syndrome. Diabetol Metab Syndr 2:1.
-
Gohlke-Bärwolf C (2000) Coronary artery disease--is menopause a risk factor? Basic Res Cardiol 95 Suppl 1: 77-83.
-
Janssen I, Powell LH, Crawford S, Lasley B, Sutton-Tyrrell K (2008) Menopause and the metabolic syndrome: the Study of Women's Health Across the Nation. Arch Intern Med 168: 1568-1575.
-
Kolovou GD, Kolovou V, Kostakou PM, Mavrogeni S (2014) Body mass index, lipid metabolism and estrogens: their impact on coronary heart disease. Curr Med Chem 21: 3455-3465.
-
Barnes S (2010) The biochemistry, chemistry and physiology of the isoflavones in soybeans and their food products. Lymphat Res Biol 8: 89-98.
-
Patisaul HB, Jefferson W (2010) The pros and cons of phytoestrogens. Front Neuro endocrinol 31: 400-419.
-
Badger TM, Ronis MJ, Wolff G, Stanley S, Ferguson M, et al. (2008) Soy protein isolate reduces hepatosteatosis in yellow Avy/a mice without altering coat color phenotype. Exp Biol Med (Maywood) 233: 1242-1254.
-
Charles C, Yuskavage J, Carlson O, John M, Tagalicud AS, et al. (2009) Effects of high-dose isoflavones on metabolic and inflammatory markers in healthy postmenopausal women. Menopause 16: 395-400.
-
Furumoto T, Fujii S, and Tsutsui H (2010) Daidzein, soy phytoestrogen, selectively ameliorates obesity-related hypertension in mice and humans without affecting other metabolic derangements: Pp. 23.441. Journal of Hypertension 28: e377.
-
Gilani GS, Cockell KA, Sepehr E (2005) Effects of antinutritional factors on protein digestibility and amino acid availability in foods. J AOAC Int 88: 967-987.
-
Doerge DR, Chang HC (2002) Inactivation of thyroid peroxidase by soy isoflavones, in vitro and in vivo. J Chromatogr B Analyt Technol Biomed Life Sci 777: 269-279.
-
Ekelund U, Franks PW, Sharp S, Brage S, Wareham NJ (2007) Increase in physical activity energy expenditure is associated with reduced metabolic risk independent of change in fatness and fitness. Diabetes Care 30: 2101-2106.
-
Ciolac EG, Greve JM (2011) Exercise-induced improvements in cardiorespiratory fitness and heart rate response to exercise are impaired in overweight/obese postmenopausal women. Clinics (Sao Paulo) 66: 583-589.
-
Seo DI, Jun TW, Park KS, Chang H, So WY, et al. (2010) 12 weeks of combined exercise is better than aerobic exercise for increasing growth hormone in middle-aged women. Int J Sport Nutr Exerc Metab 20: 21-26.
-
Eriksson J, Taimela S, Koivisto VA (1997) Exercise and the metabolic syndrome. Diabetologia 40: 125-135.
-
Segal KR, Edano A, Abalos A, Albu J, Blando L, et al. (1991) Effect of exercise training on insulin sensitivity and glucose metabolism in lean, obese, and diabetic men. J Appl Physiol 71: 2402-2411.
-
Sostaric SM, Skinner SL, Brown MJ, Sangkabutra T, Medved I, et al. (2006) Alkalosis increases muscle K+ release, but lowers plasma [K+] and delays fatigue during dynamic forearm exercise. J Physiol 570: 185-205.
-
Abood AMM, Ayobe MH, Wakeim SA, and Abou-Shanab SA (1993) Comparison of cardiovascular functions in old and young rats. M.Sc Thesis, Physiology department, Faculty of Medicine, Ain shams University.
-
Sánchez-Lozada LG, Tapia E, Jiménez A, Bautista P, Cristóbal M, et al. (2007) Fructose-induced metabolic syndrome is associated with glomerular hypertension and renal micro vascular damage in rats. Am J Physiol Renal Physiol 292: F423-429.
-
Koshinaka K, Sano A, Howlett KF, Yamazaki T, Sasaki M, et al. (2008) Effect of high-intensity intermittent swimming on postexercise insulin sensitivity in rat epitrochlearis muscle. Metabolism 57: 749-756.
-
Adesanya OA (2012) Hormonal and histoarchitectural changes in the prostate and testis of Wistar Rats Fed with Soy-Flour Enriched Diet. WMC 3: 002659.
-
Wang HJ, Murphy PA (1994) Isoflavone content in commercial soybean foods. J Agic Food Chem 42: 1666-1673.
-
Weinberg ME, Manson JE, Buring JE, Cook NR, Seely EW, et al. (2006) Low sex hormone-binding globulin is associated with the metabolic syndrome in postmenopausal women. Metabolism 55: 1473-1480.
-
Sengupta P (2012) A Scientific Review of Age Determination for a Laboratory Rat: How old is it in comparison with Human age? Biomed Int 2:81-89.
-
Parhizkar S, Abd Latiff L, Abdul Rahman S, Ibrahim R, and Dollah MA (2011): In vivo estrogenic activity of Nigella sativa different extracts using vaginal cornification assay JMPR 5: 6939-6945.
-
Liu J, Yeo HC, Overvik-Douki E, Hagen T, Doniger SJ, et al. (2000) Chronically and acutely exercised rats: biomarkers of oxidative stress and endogenous antioxidants. J Appl Physiol 89: 21-28.
-
Bernardis LL (1970) Prediction of carcass fat, water and lean body mass from Lee's "nutritive ratio" in rats with hypothalamic obesity. Experientia 26: 789-790.
-
Kennaway DJ, Owens JA, Voultsios A, Boden MJ, Varcoe TJ (2007) Metabolic homeostasis in mice with disrupted Clock gene expression in peripheral tissues. Am J Physiol Regul Integr Comp Physiol 293: R1528-1537.
-
Tietz NW (1995) Clinical guide to laboratory tests. (3rd edn) WB saunders, Philadelphia, 268-273.
-
Bonora E, Targher G, Alberiche M, Bonadonna RC, Saggiani F, et al. (2000) Homeostasis model assessment closely mirrors the glucose clamp technique in the assessment of insulin sensitivity : studies in subjects with various degrees of glucose tolerance and insulin sensitivity. Diabetes Care 23: 57-63.
-
Bach-Gansmo ET, Godal HC, and Skjonsberg OH (1998) Degradation of Fibrinogen and Cross-Linked Fibrin by Human Neutrophil Elastase Generates D-Like Fragments Detected by ELISA but Not Latex D-Dimer Test. Thromb Res 92: 125-134.
-
Vassault A, Grafmeyer D, Naudin C, Dumont GR, and Bailly M (1986) Protocole de validation de techniques. Ann Bio Clin 44: 679-685.
-
Rifai N, Bachorik PS, and Albers JJ (1999) Lipids, lipoproteins and apolipoproteins. In: Burtis CA, Ashwood ER, Tietz (3rd edn). W.B Saundes, Philadelphia, 809-861.
-
Fruchart JC (1982) Separation of low density lipoproteins and determination of cholesterol and phospholipids bound to this fraction. Rev. Fr. Des laboratories 103: 7-17.
-
Grundy SM, Greenland P, Herd A, Huebsch JA, Jones RJ, et al. (1987) Cardiovascular and risk factor evaluation of healthy American adults. A statement for physicians by an Ad Hoc Committee appointed by the Steering Committee, American Heart Association. Circulation 75: 1340A-1362A.
-
Bahgat NM, Soliman GZA (2011) Effect of Nigella Sativa Supplementation in Diet on Metabolic Syndrome in Aged Rats. Journal of American Science 7:7.
-
Ghezzi AC, Cambri LT, Botezelli JD, Ribeiro C, Dalia RA, et al. (2012) Metabolic syndrome markers in wistar rats of different ages. Diabetol Metab Syndr 4: 16.
-
Guerra RC, Zuñiga-Muñoz A, Lans VG, Díaz-Díaz E, Betancourt CAT, and Pérez-Torres I (2014) Modulation of the Activities of Catalase, Cu-Zn, Mn Superoxide Dismutase, and Glutathione Peroxidase in Adipocyte from Ovariectomised Female Rats with Metabolic Syndrome. Int J Endocrinol 2014: 175080
-
Forouhi NG, Sattar N, McKeigue PM (2001) Relation of C-reactive protein to body fat distribution and features of the metabolic syndrome in Europeans and South Asians. Int J Obes Relat Metab Disord 25: 1327-1331.
-
Morley JE (2001) Decreased food intake with aging. J Gerontol A Biol Sci Med Sci 2: 81-88.
-
Takano S, Kanai S, Hosoya H, Ohta M, Uematsu H, et al. (2004) Orexin-A does not stimulate food intake in old rats. Am J Physiol Gastrointest Liver Physiol 287: G1182-1187.
-
Lewis GF, Uffelman K, Naples M, Szeto L, Haidari M, et al. (2005) Intestinal lipoprotein overproduction, a newly recognized component of insulin resistance, is ameliorated by the insulin sensitizer rosiglitazone: studies in the fructose-fed Syrian golden hamster. Endocrinology 146: 247-255.
-
Parks EJ, Skokan LE, Timlin MT, Dingfelder CS (2008) Dietary sugars stimulate fatty acid synthesis in adults. J Nutr 138: 1039-1046.
-
Kim SP, Ellmerer M, Van Citters GW, Bergman RN (2003) Primacy of hepatic insulin resistance in the development of the metabolic syndrome induced by an isocaloric moderate-fat diet in the dog. Diabetes 52: 2453-2460.
-
Reaven GM, Lithell H, Landsberg L (1996) Hypertension and associated metabolic abnormalities--the role of insulin resistance and the sympathoadrenal system. N Engl J Med 334: 374-381.
-
Rocchini AP, Katch V, Kveselis D, Moorehead C, Martin M, et al. (1989) Insulin and renal sodium retention in obese adolescents. Hypertension 14: 367-374.
-
Vasdev S, Longerich L, Gill V (2004) Prevention of fructose-induced hypertension by dietary vitamins. Clin Biochem 37: 1-9.
-
Carrascosa JM, Ruíz P, Martínez C, Pulido JA, Satrústegui J, et al. (1989) Insulin receptor kinase activity in rat adipocytes is decreased during aging. Biochem Biophys Res Commun 160: 303-309.
-
Newby FD, DiGirolamo M, Cotsonis GA, Kutner MH (1990) Model of spontaneous obesity in aging male Wistar rats. Am J Physiol 259: R1117-1125.
-
Carr MC (2003) The emergence of the metabolic syndrome with menopause. J Clin Endocrinol Metab 88: 2404-2411.
-
Royer M, Castelo-Branco C, Blumel JE, Chedraui PA, Danckers L, et al. (2007) The US National Cholesterol Education Programme Adult Treatment Panel III (NCEP ATP III): Prevalence of the metabolic syndrome in postmenopausal Latin American women. Climacteric 10: 164-170.
-
Tappy L, Lê KA (2010) Metabolic effects of fructose and the worldwide increase in obesity. Physiol Rev 90: 23-46.
-
Pollock NK, Bundy V, Kanto W, Davis CL, Bernard PJ, et al. (2012) Greater fructose consumption is associated with cardiometabolic risk markers and visceral adiposity in adolescents. J Nutr 142: 251-257.
-
Khitan Z, Kim DH (2013) Fructose: a key factor in the development of metabolic syndrome and hypertension. J Nutr Metab 682673.
-
Bursac BN, Vasiljevic AD, Nestorovic NM, Velickovic NA, Vojnovic Milutinovic DD, et al. (2014) High-fructose diet leads to visceral adiposity and hypothalamic leptin resistance in male rats--do glucocorticoids play a role? J Nutr Biochem 25: 446-455.
-
Botezelli JD, Dalia RA, Reis IM, Barbieri RA, Rezende TM, et al. (2010) Chronic consumption of fructose rich soft drinks alters tissue lipids of rats. Diabetol Metab Syndr 2: 43.
-
Botezelli JD, Mora RF, Dalia RA, Moura LP, Cambri LT, et al. (2010) Exercise counteracts fatty liver disease in rats fed on fructose-rich diet. Lipids Health Dis 9: 116.
-
Mittelman SD, Van Citters GW, Kirkman EL, Bergman RN (2002) Extreme insulin resistance of the central adipose depot in vivo. Diabetes 51: 755-761.
-
Wajchenberg BL (2000) Subcutaneous and visceral adipose tissue: their relation to the metabolic syndrome. Endocr Rev 21: 697-738.
-
Brunner EJ, Hemingway H, Walker BR, Page M, Clarke P, et al. (2002) Adrenocortical, autonomic, and inflammatory causes of the metabolic syndrome: nested case-control study. Circulation 106: 2659-2665.
-
Arner P (2005) Insulin resistance in type 2 diabetes -- role of the adipokines. Curr Mol Med 5: 333-339.
-
Sparks JD, Sparks CE, Adeli K (2012) Selective hepatic insulin resistance, VLDL overproduction, and hypertriglyceridemia. Arterioscler Thromb Vasc Biol 32: 2104-2112.
-
Spencer CP, Godsland IF, Stevenson JC (1997) Is there a menopausal metabolic syndrome? Gynecol Endocrinol 11: 341-355.
-
Imperatore G, Riccardi G, Iovine C, Rivellese AA, Vaccaro O (1998) Plasma fibrinogen: a new factor of the metabolic syndrome. A population-based study. Diabetes Care 21: 649-654.
-
Damirchi A, Mehdizade R, Ansar MM, Soltani B, Babaei P (2010) Effects of aerobic exercise training on visceral fat and serum adiponectin concentration in ovariectomized rats. Climacteric 13: 171-178.
-
Mostarda C, Moraes-Silva IC, Salemi VM, Machi JF, Rodrigues B, et al. (2012) Exercise training prevents diastolic dysfunction induced by metabolic syndrome in rats. Clinics (Sao Paulo) 67: 815-820.
-
Ahlborg G, Björkman O (1990) Splanchnic and muscle fructose metabolism during and after exercise. J Appl Physiol 69: 1244-1251.
-
Irving BA, Davis CK, Brock DW, Weltman JY, Swift D, et al. (2008) Effect of exercise training intensity on abdominal visceral fat and body composition. Med Sci Sports Exerc 40: 1863-1872.
-
Pritzlaff CJ, Wideman L, Blumer J, Jensen M, Abbott RD, et al. (2000) Catecholamine release, growth hormone secretion, and energy expenditure during exercise vs. recovery in men. J Appl Physiol 89: 937-946.
-
Hamed GM, Bahgat NM, El-Agaty SM, Soliman GZA, and Emara MM (2010) Effects of a soybean protein diet protein diet on ovariectomised female albino rats subjected to myocardial infarction. Singapore Med J 51: 781-789.
-
Barrios-Ramos JP, Garduño-Siciliano L, Loredo M, Chamorro-Cevallos G, Jaramillo-Flores ME (2012) The effect of cocoa, soy, oats and fish oil on metabolic syndrome in rats. J Sci Food Agric 92: 2349-2357.
-
Shin D, Choi I, Yokoyama WH, Kim M and Kim Y (2014) Decreased fat accumulation in 3T3-L1 pre-adipocytes treated with extracts of heat-processed soy flour and breads. Int J food sci & tech 49: 759-767.
-
Mikstacka R, Rimado AM, Ignatowicz E (2010) Antioxidant effect of Trans-Resveratrol, pterostilbene, quercetin and their combinations in human erythrocytes in vitro. Plant Food Hum Nutr 65: 57-63.
-
Feres NH, Reis SR, Veloso RV, Arantes VC, Souza LM, et al. (2010) Soybean diet alters the insulin-signaling pathway in the liver of rats recovering from early-life malnutrition. Nutrition 26: 441-448.
-
Yang HJ, Kwon DY, Kim MJ, Kang S, Park S (2012) Meju, unsalted soybeans fermented with Bacillus subtilis and Aspergilusoryzae, potentiates insulinotropic actions and improves hepatic insulin sensitivity in diabetic rats. Nutr Metab 9: 37.
-
Kwon DY, Hong SM, Ahn IS, Kim MJ, Yang HJ, et al. (2011) Isoflavonoids and peptides from meju, long-term fermented soybeans, increase insulin sensitivity and exert insulinotropic effects in vitro. Nutrition 27: 244-252.
-
Ricketts ML, Moore DD, Banz WJ, Mezei O, Shay NF (2005) Molecular mechanisms of action of the soy isoflavones includes activation of promiscuous nuclear receptors. A review. J Nutr Biochem 16: 321-330.
-
Andrade GF, de Almeida Cd, Espeschit AC, Dantas MI, Benjamin Ldos A, et al. (2013) The addition of whole soy flour to cafeteria diet reduces metabolic risk markers in wistar rats. Lipids Health Dis 12: 145.
-
Cederroth CR, Nef S (2009) Soy, phytoestrogens and metabolism: A review. Mol Cell Endocrinol 304: 30-42.
-
Clarkson TB, Anthony MS, Morgan TM (2001) Inhibition of postmenopausal atherosclerosis progression: a comparison of the effects of conjugated equine estrogens and soy phytoestrogens. J Clin Endocrinol Metab 86: 41-47.
-
Yang HY, Yang SC, Chen JR, Tzeng YH, Han BC (2004) Soyabean protein hydrolysate prevents the development of hypertension in spontaneously hypertensive rats. Br J Nutr 92: 507-512.
-
Bitto A, Altavilla D, Bonaiuto A, Polito F, Minutoli L, et al. (2009) Effects of aglycone genistein in a rat experimental model of postmenopausal metabolic syndrome. J Endocrinol 200: 367-376.
-
Bragt MC, Popeijus HE (2008) Peroxisome proliferator-activated receptors and the metabolic syndrome. Physiol Behav 94: 187-197.
-
Dang ZC, Audinot V, Papapoulos SE, Boutin JA, Lowik CW (2003) Peroxisome proliferator-activated receptor gamma (PPARgamma) as a molecular target for the soy phytoestrogen genistein. Journal of Biological Chemistry 278: 962-967.
-
Azadbakht L, Kimiagar M, Mehrabi Y, Esmaillzadeh A, Padyab M, et al. (2007) Soy inclusion in the diet improves features of the metabolic syndrome: a randomized crossover study in postmenopausal women. Am J Clin Nutr 85: 735-741.
-
Scholz-Ahrens KE, Hagemeister H, Unshelm J, Agergaard N, Barth CA (1990) Response of hormones modulating plasma cholesterol to dietary casein or soy protein in minipigs. J Nutr 120: 1387-1392.
-
Rodin J (1991) Effects of pure sugar vs. mixed starch fructose loads on food intake. Appetite 17: 213-219.
Bowsher RR, Wolny JD, Frank BH (1992) A rapid and sensitive radioimmunoassay for the measurement of proinsulin in human serum. Diabetes 41: 1084-1090.





