Trauma Cases and Reviews
Segmental Bone Muscle and Skin Cross Leg Flap for the Treatment of Posttraumatic Infected Segmental Bone Defect in a Child- A Case Report
Piotr Pedzisz*, Ireneusz Babiak, Jakub Janowicz and Mateusz Kulig
Department of Orthopaedics and Traumatology, Medical University of Warsaw, Poland
*Corresponding author: Piotr Pedzisz, Department of Orthopaedics and Traumatology, Medical University of Warsaw, Lindleya 4, Warsaw, Poland, E-mail: piotrek.pedzisz@yahoo.com
Trauma Cases Rev, TCR-1-011, (Volume 1, Issue 2), Case Report; ISSN: 2469-5777
Received: August 07, 2015 | Accepted: September 18, 2015 | Published: September 21, 2015
Citation: Pedzisz P, Babiak I, Janowicz J, Kulig M (2015) Segmental Bone Muscle and Skin Cross Leg Flap for the Treatment of Posttraumatic Infected Segmental Bone Defect in a Child- A Case Report. Trauma Cases Rev 1:011. 10.23937/2469-5777/1510011
Copyright: © 2015 Pedzisz P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A mangled limb in a pediatric patient produces therapeutic dilemma whether to amputate or salvage greater than in adult. We herein present a case of a 10 year old child with high energy injury to both lower limbs. The bone muscle and skin segment of the limb planned for amputation has been used as a "spare part" for the contralateral shin defect in order to save at least one weight bearing limb. The cross leg flap has been successful. The patient walks without limp using PTB prosthesis. No recurrence of infection was observed within 10 years post-op. We conclude that the limb salvage attempt in a child should be based more on surgeon decision rather than strict guidelines and is always worth trying.
Keywords
Mangled limb, Osteomyelitis, Cross leg flap, Amputation
Introduction
Posttraumatic segmental osteomyelitis of distal tibia accompanied by extensive soft tissue loss with mangled opposite lower extremity is a rare and challenging condition. In most cases bilateral amputation seems to be the treatment of choice. In a pediatric patient, however, the decision making process is more complex, since the proposed solution may not be acceptable for both the child and the parents [1,2].
Case Report
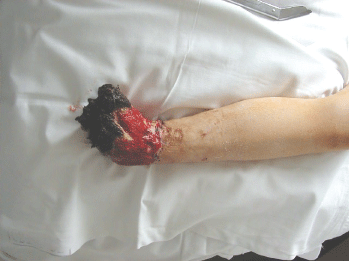
A 10-year old girl had been admitted to our Department after having been run over by a tram. She had a crush injury of the left foot (8 MESS score) and a Gustillo-Anderson IIIB open tibial fracture on the right side (6 MESS score) (Figure 1). The plantar sensation and pulse on the right foot were present. Despite multiple debridements, local and parenteral antibiotics and vacuum therapy of the left foot, the deep infection with osteomyelitis ensued that required the amputation of left foot on the level of ankle joint (Figure 2).
.
Figure 1: Crush injury of the left foot and an Gustillo-Anderson IIIB open tibial fracture on the right side
View Figure 1
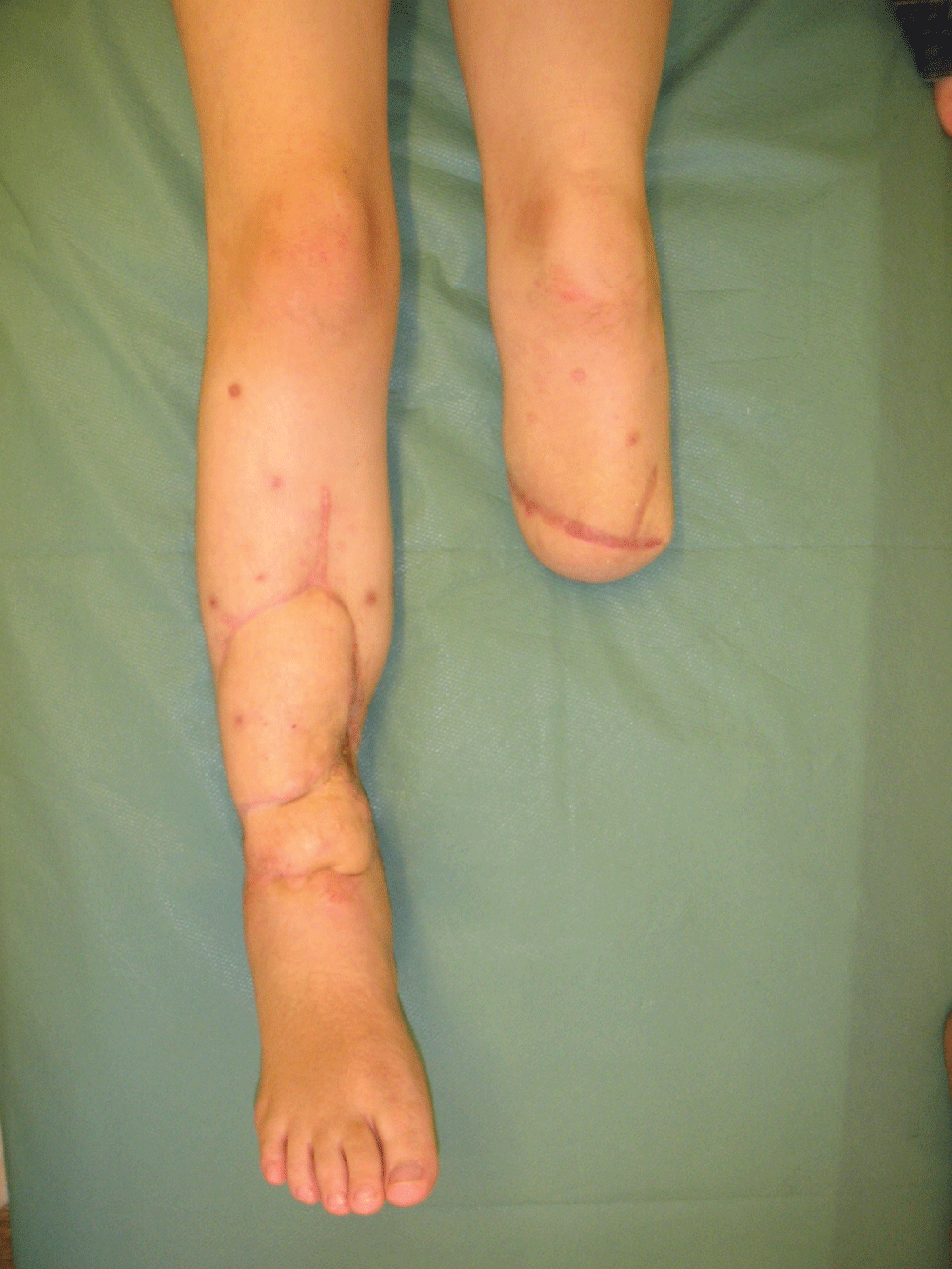
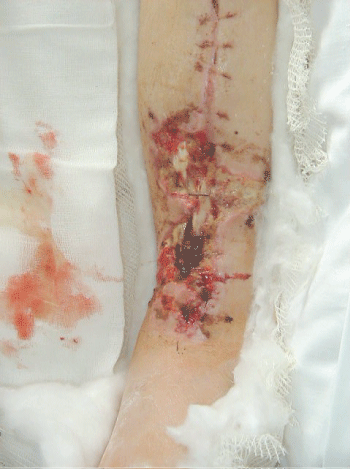
The deep infection on the right side required several surgical procedures with debridement of infected tissues and resulted in 10 cm segmental diaphyseal bone defect of distal tibia with accompanying muscle and skin loss on the same level (Figure 3). The remaining stump of the left shin was not suitable for the use of prosthesis and was finally planned for a below knee amputation on selected level. However the remaining distal part of left leg was intended to be used as a donor complex tissue for reconstruction of segmental defect on right tibia.
.
Figure 3: Segmental diaphyseal bone defect of distal tibia with accompanying muscle and skin loss
View Figure 3
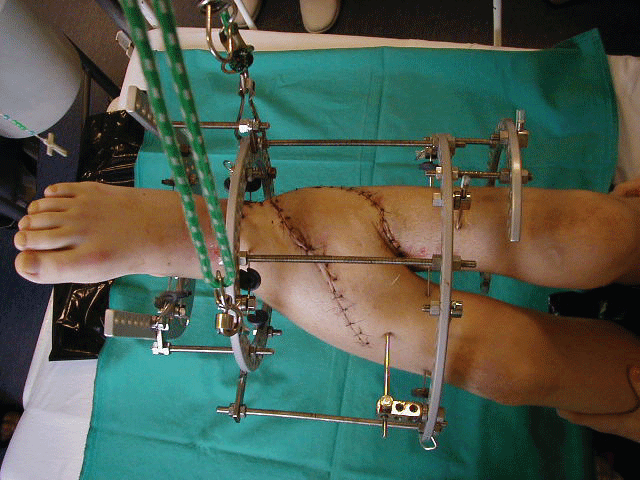
After determining the level of amputation the first stage of the reconstruction procedure was performed. It included dissection of pedicled bone muscle and skin segment on left leg and placing it into the defect on right side (Figure 4, Figure 5).
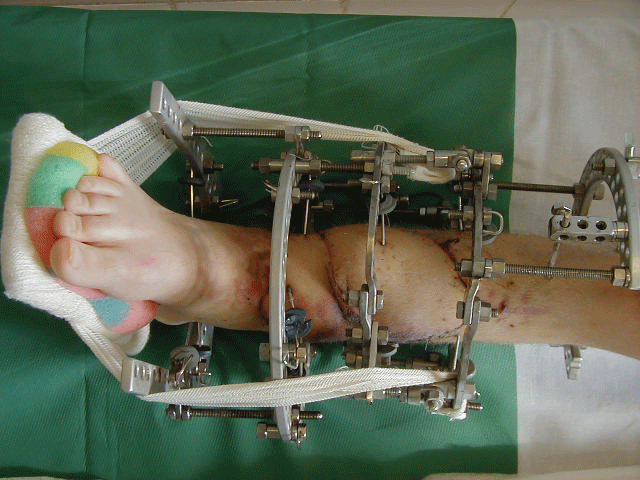
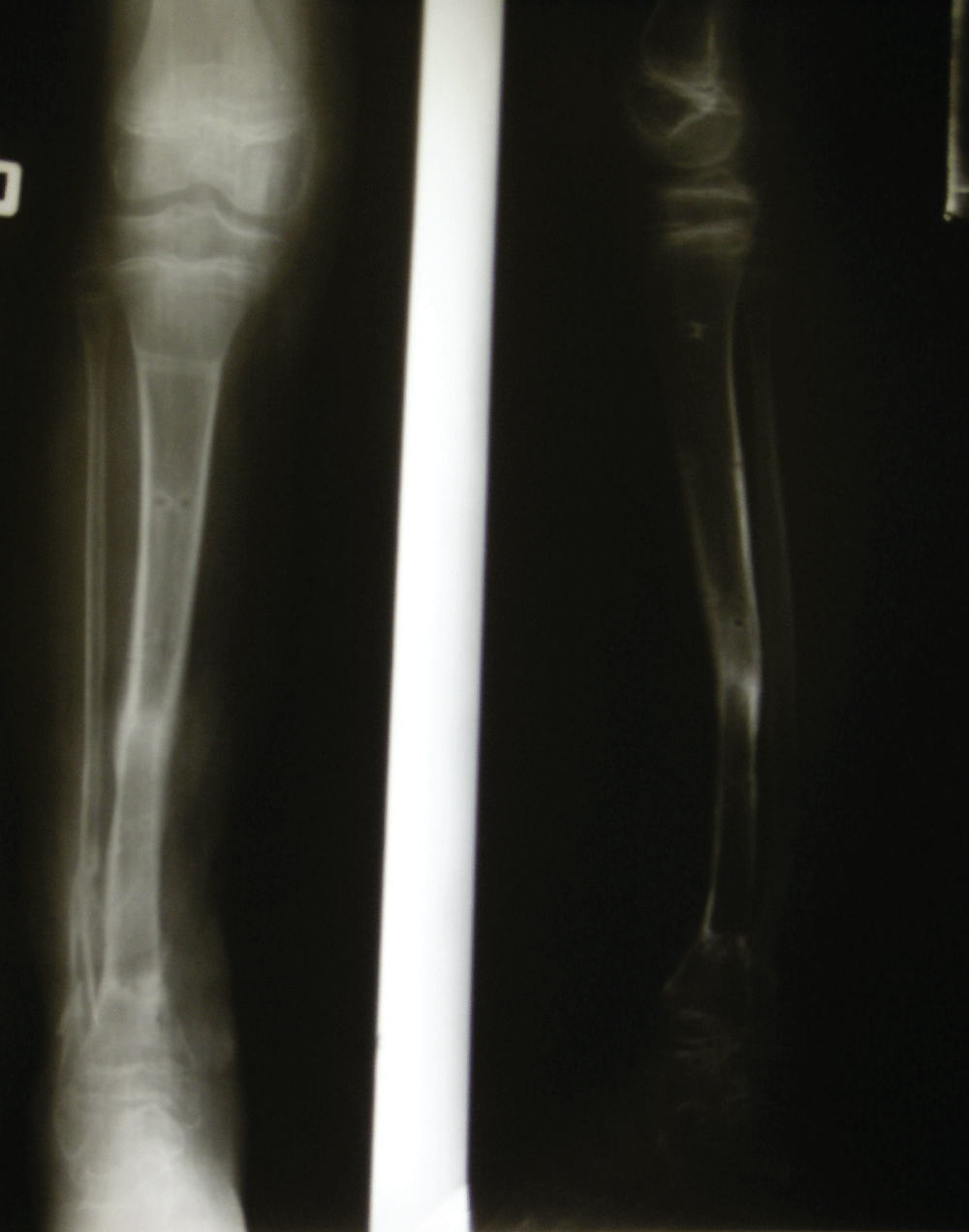
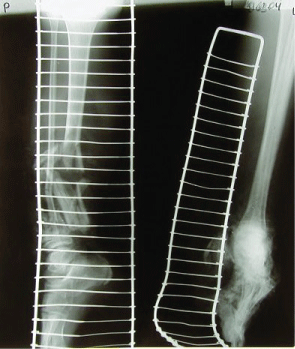
The temporary stabilisation with modified Ilizarov fixator was performed. After 4 weeks a second stage of reconstruction was done with final formation of below knee stump on left side and change of configuration of Ilizarov fixator on right side (Figure 6). After consecutive 3 months the soft tissue flap healed and union between the transported bone segment and the defect on right tibia was observed on X-ray that allowed the removal of the external fixator (Figure 7).
Summary and Conclusion
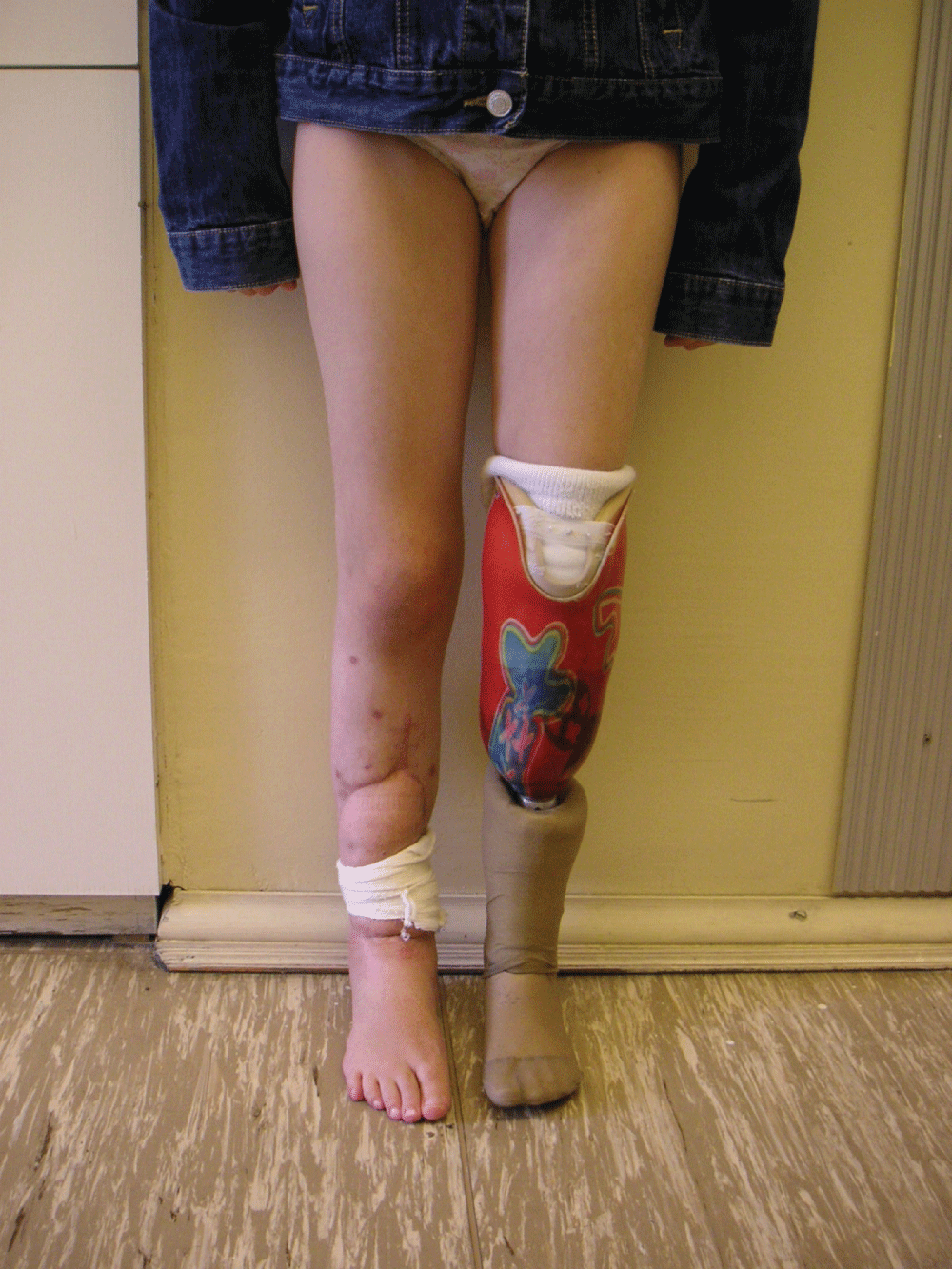
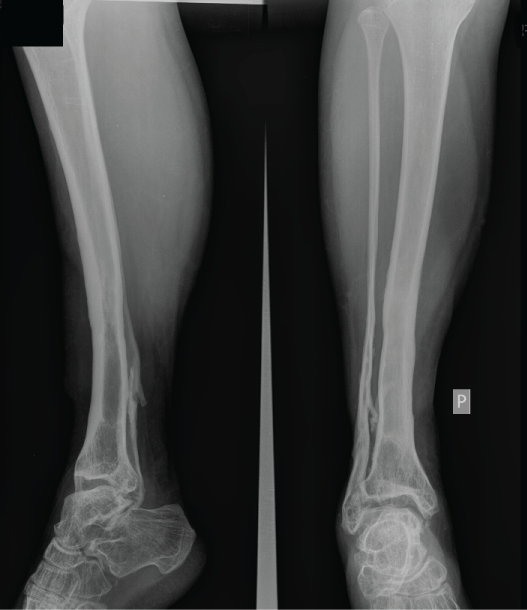
Complete healing of primarily infected complex segmental tissue defect on right tibia and sound healing of below knee stump on the left side was achieved. The patient was able to walk using PTB prosthesis with no visible limp (Figure 8, Figure 9). The ankle joint was stable with ROM of 0 degrees dorsiflexion and 45 degrees plantarflexion with no sensory deficit in the foot. The growth plates were not damaged during the procedure and no growth disturbances were observed, still, the comparison with the contralateral shin was not possible No recurrence of infection was observed within 10 years after the surgery (Figure 10).
The guidelines for treatment of pediatric patient with bilateral mangled limb are scarce. The injury scoring systems are helpful in the decision making. They should not however be treated indiscriminately as in the adult group [1-3]. The development of surgical techniques and the healing potential of a child make the reconstruction and salvage possible even in more severe cases [4-6]. The implication of bilateral amputation in a child forces these rare situations to be treated aggressively in order to save at least one weight bearing limb. In this particular case the first plan was a vascularized iliac bone graft with a gastrocnemius flap and split thickness skin grafting [3,7]. However, further compromise of the shin muscles was not desirable and the shape and mechanical strength of the iliac bone graft was considered inferior to contralateral tibia. Taking advantage of the shin stump as a source of a "spare parts" seems a reasonable choice when its amputation is inevitable [8].
The discussed case demonstrates that: a crossover pedicled composite tissue transfer from one leg planned for amputation on selected level can salvage the opposite leg in case of high-grade bilateral open fracture of distal part of lower extremity resulting in segmental osteomyelitis of one tibia.
References
-
Stewart DA, Coombs CJ, Graham HK (2012) Application of lower extremity injury severity scores in children. J Child Orthop 6: 427-431.
-
Johansen K, Daines M, Howey T, Helfet D, Hansen ST Jr (1990) Objective criteria accurately predict amputation following lower extremity trauma. J Trauma 30: 568-572.
-
Patzakis MJ, Zalavras CG (2005) Chronic posttraumatic osteomyelitis and infected nonunion of the tibia: current management concepts. J Am Acad Orthop Surg 13: 417-427.
-
Bartlett CS 3rd, Weiner LS, Yang EC (1997) Treatment of type II and type III open tibia fractures in children. J Orthop Trauma 11: 357-362.
-
Weinberg A, Mosheiff R, Liebergall M, Berlatzky Y, Aner H, et al. (1999) Amputated lower limbs as a bank of organs for other organ salvage. Injury 30 Suppl 2: B34-38.
-
Keating JF, Simpson AH, Robinson CM (2005) The management of fractures with bone loss. J Bone Joint Surg Br 87: 142-150.
-
MacKenzie EJ, Bosse MJ, Kellam JF, Burgess AR, Webb LX, et al. (2002) Factors influencing the decision to amputate or reconstruct after high-energy lower extremity trauma. J Trauma 52: 641-649.
-
Prasarn ML, Helfet DL, Kloen P (2012) Management of the mangled extremity. Strategies Trauma Limb Reconstr 7: 57-66.