Trauma Cases and Reviews
Is That Only a Spinous Process Fracture? Report of a Case of a C6 Spinous Process Fracture with Accompanying Complex Ligamentous Injury Resulting in a Delayed Unilateral Facet Dislocation at the C6-7 Level
Gergely Bodon1*, Juergen Degreif1, Harald Seifarth2 and Tobias Pitzen3
1Department of Orthopaedic Surgery and Traumatology, Klinikum Esslingen, Germany
2Department of Diagnostic and Interventional Radiology, Klinikum Esslingen, Germany
3SRH Clinic Karlsbad-Langensteinbach, Spine Centre, Germany
*Corresponding author: Gergely Bodon, Department of Orthopaedic Surgery and Traumatology, Klinikum Esslingen, Hirschlandstrasse 97, 73730 Esslingen a.N., Germany, E-mail: gbodon@gmail.com
Trauma Cases Rev, TCR-1-014, (Volume 1, Issue 3), Case Report; ISSN: 2469-5777
Received: October 14, 2015 | Accepted: November 07, 2015 | Published: November 10, 2015
Citation: Bodon G, Degreif J, Seifarth H, Pitzen T (2015) Is That Only a Spinous Process Fracture? Report of a Case of a C6 Spinous Process Fracture with Accompanying Complex Ligamentous Injury Resulting in a Delayed Unilateral Facet Dislocation at the C6-7 Level. Trauma Cases Rev 1:014. 10.23937/2469-5777/1510014
Copyright: © 2015 Bodon G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Spinous process fractures of the cervical spine are considered harmless. We report a case of a C6 spinous process fracture with accompanying ligamentous injury at the C6-7 level which led to secondary unilateral facet dislocation at C6-7.
A 76 years old patient suffered a motor vehicle accident and was brought to our hospital with neck pain and an occipital wound. On the initial polytrauma computed tomography (CT) an isolated spinous process fracture of C6 with hematoma among the posterior soft tissues was diagnosed as well as fracture of the right L1 transverse process. CT of the cervical spine showed no signs of segmental instability. Conservative treatment was introduced and the patient was provided with a soft cervical collar. On the third day of admission, he developed a left sided radiculopathy. Subsequent magnetic resonance imaging (MRI) showed a left sided unilateral facet dislocation at C6-7 with accompanying disco-ligamentous injury of the same level. The patient underwent posterior reduction and instrumentation followed by anterior discectomy and fusion of C6-7. The combined approach led to anatomic reduction and resolution of the radiculopathy.
While computed tomography (CT) screening detects almost all of the fractures of the cervical spine, screening for potentially unstable accompanying ligamentous injuries of the cervical spine is still challenging. Since discoligamentous injuries are difficult to diagnose using CT only, a careful clinical examination together with adequate imaging including MRI must be done to rule out ligamentous injuries in case of a traumatic spinous process fracture to avoid secondary dislocation with the risk of neurologic injury. Spinous process fractures caused by direct or indirect trauma and those of due to ligamentous stress ("clay-shoveler's fracture") must be sharply separated in the clinical practice.
Introduction
Isolated spinous process fractures are considered as benign injuries of the cervical spine [1,2], although their role as "sentinel" in complex spinal injuries was already recognized about thirty years ago [3]. Isolated spinous process fractures are treated conservatively with analgesics, restriction of physical activity and wearing of a soft cervical collar for 4-6 weeks [4-6]. Surgical treatment was reported in patients with chronic pain, consisting of resection of the free bony fragment [7,8]. The pathomechanism of spinous process fracture shows great variations. Direct blow to the neck, hyperflexion, hyperextension, flexion-extension injury and immense stress during different sport activities or manual work ("clay-shoveler's fracture") has been reported [4,7].
Screening of trauma patients for a potentially unstable discoligamentous injury of the cervical spine in the absence of unstable fracture or signs of segmental instability is challenging [9]. Although nonskeletal cervical spine injuries are believed to occur rarely [10,11], Demetriades reported that subluxations of the cervical spine without a fracture could make up as much as 10,65% of cervical spine injuries [12]. The real number of occult ligamentous injuries is probably underreported, this was also verified by the study of Mayer [9].
We report a case of a C6 spinous process fracture with initially undetected ligamentous injury at the C6-7 level which led to secondary unilateral facet dislocation at C6-7. This case shows the importance of repeated clinical examinations together with adequate imaging studies to avoid secondary dislocation with the risk of neurologic injury.
Case Report
History and examination
A 76 years old male suffered a motor vehicle accident (rollover with 100 km/h) traveling in a sports car as a passenger. The patient arrived at the emergency unit of the hospital wearing a stifneck collar; he was hemodynamically stable and alert (GCS 15). He complained of neck pain with tenderness over the lower cervical spine without radiating pain into the upper extremities and had an occipital wound. Neurologic examination showed no sensory or motor deficits, he had no signs of myelopathy or any pathological reflexes. The polytrauma CT revealed fracture of the right L1 transverse process and fracture of the C6 spinous process.
At this time, our main diagnosis regarding the cervical spine was a fracture of the spinous process of C6 which did not extend to the lamina. Spinous process fractures of this kind are considered as stable injuries [1] therefore conservative treatment was initialized; the patient was admitted for observation and was provided with a soft cervical collar for pain reduction. A cervical MRI was ordered to rule out ligamentous injury and dynamic films (flexion-extension) were planned after the acute phase to check for segmental instability.
Three days after the accident, the patient developed a left sided radiculopathy. Neurologic examination showed irritation of the left C7 nerve root with palsy of the triceps and finger extensor muscles (Grade 4/5 strength in both muscle groups) without clinical signs of cervical myelopathy. An MRI was done on the same day, which showed a left sided unilateral facet dislocation at C6-7. The patient was treated surgically with open posterior reduction and anterior discectomy and fusion of C6-7. Details of the imaging studies are discussed below.
Imaging
The polytrauma CT on the day of admission (with sagittal and coronal reformations) showed fracture of the L1 right transverse process. CT of the cervical spine (Figure 1) showed fracture of the C6 spinous process and degenerative changes of the C6-7 segment. It showed no prevertebral hematoma (normal width of retrotracheal space) but significant hematoma among the posterior soft tissues between C1-6 was visible. Alignment of the cervical spine was correct, there was no segmental kyphosis, widening of the disc space, ventro- or retrolisthesis and there was no sign of dislocation of the facet joints (the zygapophyseal joints showed normal articular apposition, there was no "fanning" of the interlaminar and interspinous spaces). There was no suspicion of ligamentous injury. The changes seen at the C6-7 level were due to degenerative changes, there was no sign of abnormal alignment.
.
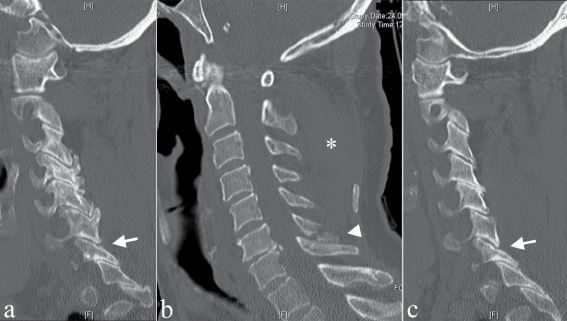
Figure 1: First CT of the patient. Image a and c shows sagittal view at the level of the lateral masses on the right (a) and left (c) side. Arrow points at C6-7 facet joint. Image b shows medial plane. Arrowhead points at the broken spinous process of C6. Asterisk marks the hematoma among the posterior soft tissues.
View Figure 1
The MRI three days after admission showed a left sided unilateral facet dislocation at C6-7 (Figure 2). The "jumped facet" resulted in foraminal stenosis at the C6-7 level compressing the exiting left C7 nerve root. The C6 vertebral body was anteriorly displaced on C7 about 25% of the anteroposterior diameter of the vertebral body resulting in central spinal canal stenosis without radiologic signs of myelopathy. According to the MRI, the facet capsules on both sides, yellow ligament, anterior longitudinal ligament and the disc was also disrupted at the C6-7 level. The posterior longitudinal ligament was not torn and also there was no traumatic disc herniation seen at the C6-7 level. MRI showed degenerative spinal canal stenosis at C4-5 with posttraumatic facet joint effusion without disruption of the facet capsules or the yellow ligament.
.
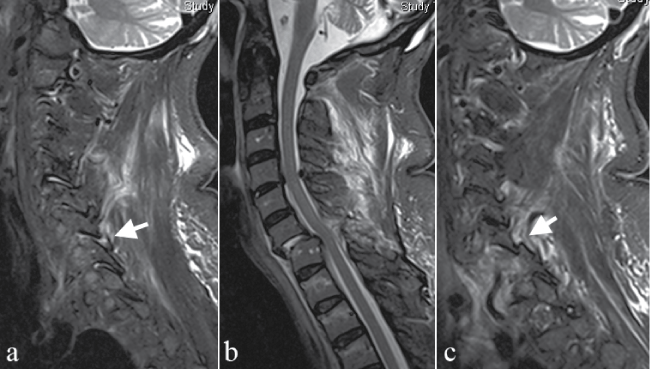
Figure 2: MRI of the patient made on the 3rd day of admission showing unilateral facet dislocation at C6-7. Image a shows the level of the lateral masses on the right side. Arrow points at the ruptured C6-7 facet joint. Image b shows the medial plane ventrolisthesis of C6 on C7 is visible with minimal prevertebral hematoma, complete disruption of the disc and yellow ligament. Pic c shows the level of the lateral masses on the left side. Arrow points at the jumped facet of C6-7.
View Figure 2
Operation
The patient was operated by the senior author, T.P. using a combined P-A approach consisting of posterior reduction and instrumentation and anterior cervical discectomy and fusion. The patient was intubated bronchoscopically and positioned prone. A classical midline posterior approach was used to reach the posterior surface of the C6-7 vertebras. The spinous process of C6 was broken, the yellow ligament was disrupted on both sides and also the joint capsule on the left side was disrupted. The inferior articular process of C6 was dislocated anteriorly (jumped facet) leaving the left superior articular facet of C7 "naked".
Reduction was done by resection of the left superior articular process of C7 using a high speed drill with a 3mm diamond burr. A few minutes later, the C6 vertebra returned to its anatomic position.
The fractured spinous process of C6 was resected and also the remaining yellow ligament was removed at the C6-7 level. Posterior fusion was done using lateral mass screws in C6 and C7 (according to the preoperative CT, the anatomy of the C7 lateral mass allowed the placement of lateral mass screws in this case). A rod was placed between the C6 and C7 lateral mass screws and slight additional reposition was done. After placement of a drainage and wound closure, the patient was turned and positioned for the anterior approach. An ACDF was performed using a classical ventral approach from the left side. At the C6-7 level a small prevertebral hematoma was found. The anterior longitudinal ligament was partly disrupted while the C6-7 disc was completely disrupted. There was no herniated disc material in the spinal canal. After removal of the disc and preparation of the endplates, a cage was placed and anterior fusion was done using a dynamic plate at the C6-7 level. After placement of drainage, the wound was closed. The postoperative X-ray and CT are shown on Figure 3.
.
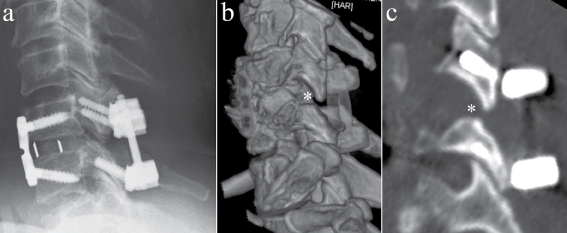
Figure 3: Image a shows postoperative lateral x-ray showing anatomic reposition of the segment C6-7. Picture b shows 3D reconstruction, c the postoperativ CT in the sagittal. Asterisk marks the removed tip of the left superior facet of C7.
View Figure 3
Postoperative course
The postoperative course was uneventful. The radicular pain disappeared postoperatively and the neurologic deficits improved to Grade 5/5 at the time of discharge. Postoperative X-rays revealed an anatomic reduction and the 3 months follow up showed fusion of the C6-7 segment.
Discussion
Fracture of the cervical spinous process is a rare injury, Stiell found only 12 of these fractures, examining 8924 stable and alert trauma patients with blunt trauma to the head and/or neck during their prospective cohort study resulting in the Canadian C-Spine Rule [1]. Beside direct or indirect trauma, the most common cause of an isolated spinous process fracture is ligamentous stress on the spinous process due to excessive contraction of the trapezius and rhomboid muscles while lifting heavy weights [6,7]. This is the "clay-shoveler's fracture", an avulsion fracture of the spinous process of C7, C6 or Th1 (in that order of frequency) usually not extending to the lamina [2]. It occurs mainly in manual workers, but was also reported in sportsmen during different sports activities [5,6]. In case of the "clay-shoveler's fracture", the posterior ligamentous complex remains intact, therefore this injury is considered stable and can be treated conservatively [2,4-6]. We believe that spinous process fracture caused by direct or indirect trauma and those of due to ligamentous stress ("clay-shoveler's fracture") must be sharply separated.
In our institution the Canadian C-Spine Rule is used to assess alert and stable trauma patients [1]. According to the Canadian C-Spine Rule this peculiar patient needed radiographic check up because of the associated high-risk factors and his clinical symptoms. These are as follows: age above 65 years, dangerous mechanism (rollover mechanism, high speed > 100 km/h), neck pain and midline tenderness over the cervical-spine on physical examination. We use three-view radiography (anteroposterior, lateral and open-mouth odontoid view) to clear our patients and add CT-scanning in cases with abnormal x-rays or when the area in question is not well visualized using radiography or by high suspect on clinical examination. In our department patients requiring CT of the head will have their cervical spine scanned at the time of the head CT. This protocol is similar to that of Barba [13]. Computed tomography is reported to be superior to plain radiographs evaluating the cervical spine for bony injuries [14-20]. Although CT is the most sensitive, specific, and also cost effective modality to screen the cervical spine for bony injuries, it is not an effective modality to screen for ligamentous injuries of the cervical spine [14], and also not appropriate to predict instability [21]. CT is the best modality to diagnose and define the anatomy of a fracture, a possible ligamentous injury or disc herniation is best demonstrated by MRI [2,21]. Vanguri et al. found 52 ligamentous injuries examining 5676 patients in their retrospective review. Of the 52 patients with ligamentous injury, 32 patients had at least one fracture of the cervical spine identified by the CT scan, 20 ligamentous injuries were suspected by CT and of these 10 had no fracture [22]. Dickason examined the spectrum of injuries associated with cervical spinous process fractures on 17 patients. They concluded that spinous process fractures may represent serious injuries while isolated fracture of the spinous process is rare [23].
In this case, fracture of the spinous process was detected by CT but the extent of ligamentous injury could not be perceived. Based on the CT our main diagnosis was a fracture of the spinous process of C6 which did not extend to the lamina. Spinous process fractures of this kind are considered as stable injuries [1]. However, retrospectively reviewing our first CT there are two signs that cannot be interpreted as degenerative changes. First, the disc C6-7 showed marked narrowing. Posterior disc space was narrower (endplate on endplate) than the anterior disc space but still narrower as the other disc spaces. This finding could be explained by the traumatic disruption of the anulus seen later on the MRI. Second, there is a break in the posterior spinolaminar line considering the C6-C7-Th1 laminas; the C7 lamina is slightly ventrally displaced. The disruption of the spinolaminar line in case of a spinous process fracture as a sign of associated posterior ligamentous injury was described by Matar [24]. These two findings could have forewarned the disruption of the disc and posterior ligamentous structures which made this motion segment unstable.
We have two possible theories to explain the secondary dislocation at C6-7. According to the first theory, beside the spinous process fracture of C6, our patient suffered a ligamentous injury of the posterior ligamentous complex and disruption of the C6-7 disc, resulting in instability of the C6-7 level. This instability led to the unilateral facet dislocation at C6-7 three days later.
The second possibility is that the primary injury was an unilateral facet dislocation with spontaneous reposition immediately after the injury. The accompanying soft tissue injuries caused the instability of the segment and led to the secondary dislocation. It was reported that unilateral and bilateral facet dislocations have a tendency to spontaneous reposition after the initial trauma, making primary diagnosis difficult [9,25].
Unilateral facet dislocation is a flexion-distraction injury of the subaxial cervical spine [26]. There are a few studies examining the extent of soft tissue disruption after unilateral facet dislocation. Vaccaro examined 25 patients with unilateral dislocations using MRI after closed traction reduction and found that unilateral facet dislocation was associated with disruption of most soft tissue structures (posterior ligamentous complex, yellow ligament, joint capsule and disc), with the exception of the posterior longitudinal ligament (disrupted only in 12%) [27]. According to Sim's in vitro study, unilateral facet dislocation will not occur as long as the anulus fibrosus and the ipsilateral yellow ligament is intact [28]. The study of Nadeau showed similar results, they concluded that the main stabilizers of the subaxial cervical spine are the anulus fibrosus, nucleus pulposus and the yellow ligaments [29]. Halliday et al. tried to predict clinical instability using MRI in patients with unilateral lateral mass/facet fractures. They found that the degree of ligamentous injury at the level of the fracture correlates with instability and found that patients with an injury of at least three of the following four structures - facet capsule, interspinous ligament, anterior longitudinal ligament and posterior longitudinal ligament - may require operative stabilization [21].
Conclusion
Spinous process fracture caused by direct or indirect trauma and those of due to ligamentous stress ("clay-shoveler's fracture") must be sharply separated in the clinical practice. Clinical and radiologic re-evaluation of a patient is needed in case of persistent neck pain or if there is a change in the clinical picture to diagnose a possible ligamentous injury or a secondary dislocation.
In case of a spinous process fracture caused by direct or indirect trauma an MRI is needed to rule out associated ligamentous injuries. We suggest a surgical therapy if disruption of the facet joint capsule, disc (or the posterior anulus fibrosus) and the yellow ligament is seen on the MRI to avoid secondary dislocation with the risk of neurologic injury.
Disclosure
The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
References
-
Stiell IG, Wells GA, Vandemheen KL, Clement CM, Lesiuk H, et al. (2001) The Canadian C-spine rule for radiography in alert and stable trauma patients. JAMA 286: 1841-1848.
-
Harris JHJ, Edeiken-Monroe BS (1987) The radiology of acute cervical spine trauma (2nd edn). Williams & Wilkins, USA.
-
Meyer PG, Hartman JT, Leo JS (1982) Sentinel spinous process fractures. Surg Neurol 18: 174-178.
-
Victor B Feldman, Frank Astri (2001) An atypical clay shoveler's fracture: a case report. J Can Chiropr Assoc 45: 213-220.
-
Hetsroni I, Mann G, Dolev E, Morgenstern D, Nyska M (2005) Clay shoveler's fracture in a volleyball player. Phys Sportsmed 33: 38-42.
-
Kim SY, Chung SK, Kim DY (2012) Multiple cervical spinous process fractures in a novice golf player. J Korean Neurosurg Soc 52: 570-573.
-
Hirsh LF, Duarte LE, Wolfson EH, Gerhard W (1991) Isolated symptomatic cervical spinous process fracture requiring surgery. Case report. J Neurosurg 75: 131-133.
-
Brown CN, McKenna P (2009) A Wii-related clay-shoveler's fracture. Scientific World Journal 9: 1190-1191.
-
Mayer M, Zenner J, Auffarth A, Blocher M, Figl M, et al. (2013) Hidden discoligamentous instability in cervical spine injuries: can quantitative motion analysis improve detection? Eur Spine J 22: 2219-2227.
-
Lekovic GP, Harrington TR (2007) Litigation of missed cervical spine injuries in patients presenting with blunt traumatic injury. Neurosurgery 60: 516-522.
-
Seijas R, Ares O, Casamitjana J (2005) Occult ligamentous injury of the cervical spine associated with cervical spine fracture. Acta Orthop Belg 71: 746-749.
-
Demetriades D, Charalambides K, Chahwan S, Hanpeter D, Alo K, et al. (2000) Nonskeletal cervical spine injuries: epidemiology and diagnostic pitfalls. J Trauma 48: 724-727.
-
Barba CA, Taggert J, Morgan AS, Guerra J, Bernstein B, et al. (2001) A new cervical spine clearance protocol using computed tomography. J Trauma 51: 652-656.
-
Diaz JJ Jr, Aulino JM, Collier B, Roman C, May AK, et al. (2005) The early work-up for isolated ligamentous injury of the cervical spine: does computed tomography scan have a role? J Trauma 59: 897-903.
-
Griffen MM, Frykberg ER, Kerwin AJ, Schinco MA, Tepas JJ, et al. (2003) Radiographic clearance of blunt cervical spine injury: plain radiograph or computed tomography scan? J Trauma 55: 222-226.
-
Kligman M, Vasili C, Roffman M (2001) The role of computed tomography in cervical spinal injury due to diving. Arch Orthop Trauma Surg 121: 139-141.
-
Schenarts PJ, Diaz J, Kaiser C, Carrillo Y, Eddy V, et al. (2001) Prospective Comparison of Admission Computed Tomographic Scan and Plain Films of the Upper Cervical Spine in Trauma Patients with Altered Mental Status. J Trauma 51: 663-668.
-
Blackmore CC, Ramsey SD, Mann FA, Deyo RA (1999) Cervical spine screening with CT in trauma patients: a cost-effectiveness analysis. Radiology 212: 117-125.
-
Blackmore CC, Mann FA, Wilson AJ (2000) Helical CT in the primary trauma evaluation of the cervical spine: an evidence-based approach. Skeletal Radiol 29: 632-639.
-
Katz MA, Beredjiklian PK, Vresilovic EJ, Tahernia AD, Gabriel JP, et al. (1999) Computed tomographic scanning of cervical spine fractures: does it influence treatment? J Orthop Trauma 13: 338-343.
-
Halliday AL, Henderson BR, Hart BL, Benzel EC (1997) The management of unilateral lateral mass/facet fractures of the subaxial cervical spine: the use of magnetic resonance imaging to predict instability. Spine (Phila Pa 1976) 22: 2614-2621.
-
Vanguri P, Young AJ, Weber WF, Katzen J, Han J, et al. (2014) Computed tomographic scan: it's not just about the fracture. J Trauma Acute Care Surg 77: 604-607.
-
Dickason GN, Motsitsi NS (2007) Cervical spinous process fractures: The spectrum of injuries. The Internet Journal of Spine Surgery.
-
Matar LD, Helms CA, Richardson WJ (2000) "Spinolaminar breach": an important sign in cervical spinous process fractures. Skeletal Radiol 29: 75-80.
-
Mueller E-J, Muhr G (1997) Wirbelsaulenverletzungen. Thieme 74.
-
Allen BL Jr, Ferguson RL, Lehmann TR, O'Brien RP (1982) A mechanistic classification of closed, indirect fractures and dislocations of the lower cervical spine. Spine (Phila Pa 1976) 7: 1-27.
-
Vaccaro AR, Madigan L, Schweitzer ME, Flanders AE, Hilibrand AS, et al. (2001) Magnetic resonance imaging analysis of soft tissue disruption after flexion-distraction injuries of the subaxial cervical spine. Spine 26: 1866-1872.
-
Sim E, Vaccaro AR, Berzlanovich A, Schwarz N, Sim B (2001) In vitro genesis of subaxial cervical unilateral facet dislocations through sequential soft tissue ablation. Spine (Phila Pa 1976) 26: 1317-1323.
-
Nadeau M, McLachlin SD, Bailey SI, Gurr KR, Dunning CE, et al. (2012) A biomechanical assessment of soft-tissue damage in the cervical spine following a unilateral facet injury. J Bone Joint Surg Am 94: e156.





