Trauma Cases and Reviews
Missed Spinal Lesions in Traumatized Patients
Ana M Cerván de la Haba*, Miguel Rodríguez Solera J, Miguel S Hirschfeld León and Enrique Guerado Parra
Department of Orthopaedic Surgery, Traumatology and Rehabilitation, Hospital Universitario Costa del Sol. University of Malaga, Spain
*Corresponding author: Ana M Cerván de la Haba, Hospital Universitario Costa del Sol, Autovía A7 km 187 C.P. 29603, Marbella, Spain, Tel: 951976224, E-mail: anacervan@me.com
Trauma Cases Rev, TCR-2-027, (Volume 2, Issue 1), Case series; ISSN: 2469-5777
Received: October 31, 2015 | Accepted: January 13, 2016 | Published: January 15, 2016
Citation: de la Haba AMC, Miguel RSJ, León MSH, Parra EG (2016) Missed Spinal Lesions in Traumatized Patients. Trauma Cases Rev 2:027. 10.23937/2469-5777/1510027
Copyright: © 2016 de la Haba AMC, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Overlooked spinal injuries and delayed diagnosis are still common in traumatized patients. The management of trauma patients is one of the most important challenges for the specialist in trauma. Proper training and early suspicion of this lesion are of overwhelming importance.
The damage control orthopaedics, diagnosis and treatment algorithm applied to multitrauma patients reduces both morbidity and mortality in polytrauma patients due to missed lesions. Algorithm on its diagnosis and after on its treatment is necessary in order to decrease complications. Despite application of care protocols for trauma patients still exist missed spinal injuries.
We report four cases of missed spinal lesion in trauma patients. We propose perform a very exhaustive clinical and imaging study thorough all polytraumatized patient in order to minimize missed spinal injuries.
Keywords
Spinal lesions, Polytrauma patients, Missed lesions
Introduction
Diagnosis of spinal fractures in traumatized patients is one of the most important challenges for trauma specialist surgeons. Proper training and early suspicion of spinal lesions are of overwhelming importance, mainly in apparent asymptomatic patients including those having a fall with no apparent symptoms of lesions.
A missed injury can be defined as any not discovered nor suspected upon admission to either the intensive care unit or a hospitalization ward. Some authors, after reviewing the records of 567 patients (all trauma patients assessed by St Michael's Hospital trauma service from 1995 to 1997) found that 46 out of them (8.1%) had missed injuries diagnosed after hospital discharge, this patients were in most more severely injured and the majority of missed injuries were potentially avoidable with repeat clinical assessments and a high index of suspicion [1].
There are many guidelines for the management of multiple trauma patients, as outlined by the Advanced Trauma Life Support Course (ATLS) [2] by giving a very clear algorithm for the initial management of these patients. According to this, a second survey will help in decreasing the number of missed spinal injuries, being claim that standardized tertiary trauma survey is vitally important in the detection of clinically significant missed injuries and should be included in trauma care, our misdiagnosis occurs at first or later examinations [3]. However despite even a third survey still many injuries are overlooked [4,5].
In this paper based on the case method, we discuss the diagnosis of missable spinal fractures within several traumatic settings.
Case Studies
Case 1
A 72-year-old male with the diagnosis of ankylosing spondylitis and diabetes, presented to the emergency department of our Institution with lumbar pain after having a severe staircases fall. Physical examination at that time revealed thoracolumbar pain without neurological symptoms and signs. Two plain, anterior and lateral x-ray projections of the thoracolumbar spine were taken and interpreted as with no traumatic signs, so no further studies were obtained and the patient was discharged home. Two weeks later, because he was still on pain and began to feel some weakness on both legs together with urinary retention, came again to the emergency department.
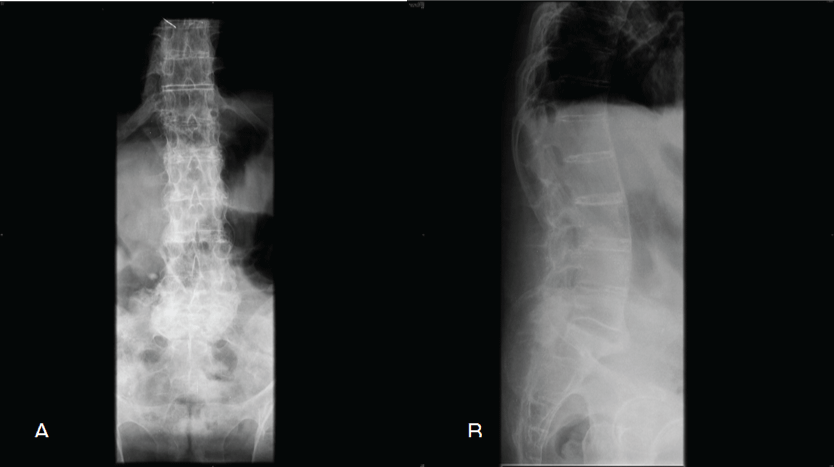
.
Figure 1: Anteroposterior (A) and lateral; (B) spine radiograph on admission, the first time the patient came to Hospital.
View Figure 1
He underwent two new x-rays and a magnetic resonance images (MRI) which revealed a T12-L1 fracture. He was duly operated on with a posterior thoracolumbar fusion with pedicle screw instrumentation. In a retrospective review of the initial x-rays a subtle rupture of the anterior intervertebral ligament between T12-L1 could be seen, together with lung shadows making difficult the diagnosis of his vertebral lesion (Figure 1, Figure 2 and Figure 3).
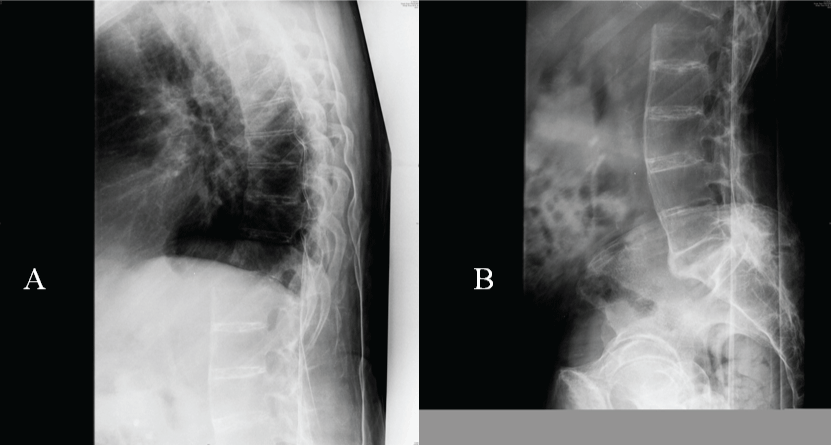
.
Figure 2: Lateral spine radiographs two weeks later, imaging studies at injury revealed an important unstable thoracolumbar fracture at T12.
View Figure 2
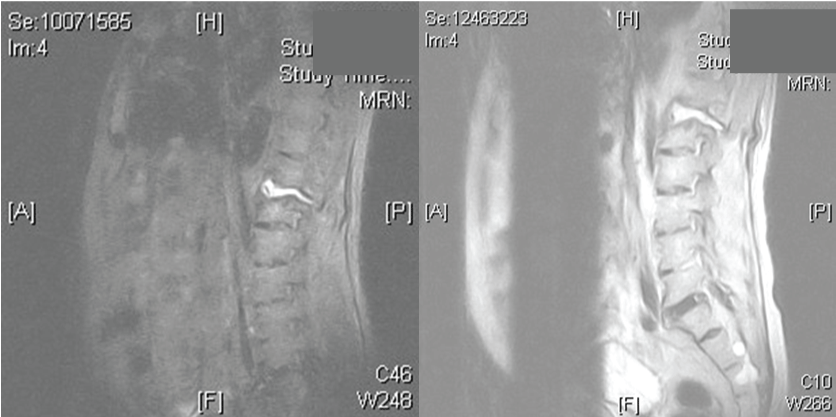
.
Figure 3: MRI of the spine, sagittal images of MRI, illustrated a T12-L1 fracture, with damage in the posterior aspect of T12 and the posterior longitudinal ligament is avulsed.
View Figure 3
Case 2
A 26-year-old male presented to the emergency department after having a high speed motor vehicle accident. He complained of cervical pain, but since physical examination and cervical plain radiographs were reported as normal, he was discharged home. He returned 4 days later with progressive weakness of both hands and still on cervical pain. CT scan showed a left facet dislocation at C6-C7 level. He underwent emergent closed posterior reduction and anterior cervical discectomy together with C6-C7 fusion by means of plating and tricortical allograft. He dramatically improved few hours after surgery (Figure 4 and Figure 5).
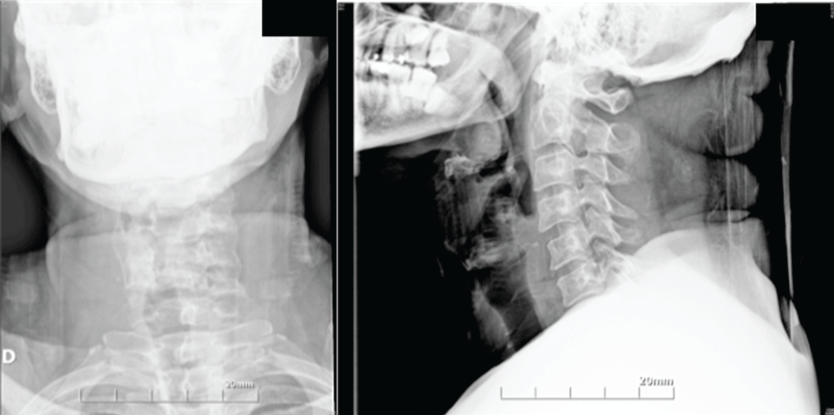
.
Figure 4: Radiographs on admission, anteroposterior (A) and lateral (B) views does not illustrated the whole cervical spine.
View Figure 4
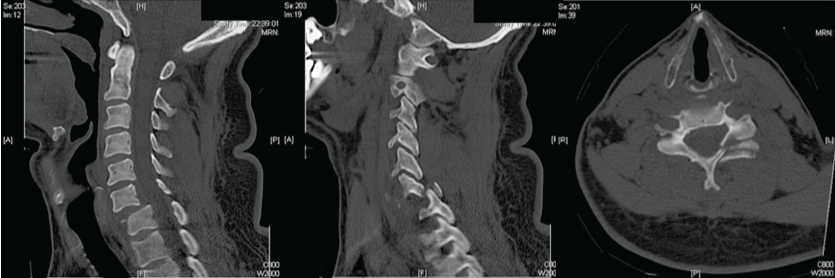
.
Figure 5: Sagittal (A, B) and axial (C) images of CT scan clearly shows the fracture facet dislocation at C6C7.
View Figure 5
Case 3
A 37-year-old male came to our hospital after a blow onto his head jumping into the sea. On neurological examination he presented some weakness and numbness on both hands together with neck pain. An anteroposterior and lateral radiograph projections, and a CT scan of the neck were performed and interpreted to be normal. During his stay at emergency upper limb weakness and pain, particularly in his left hand, worsened. A MRI was performed displaying a C4-C5 disc hernia with cord compression (Figure 6 and Figure 7).
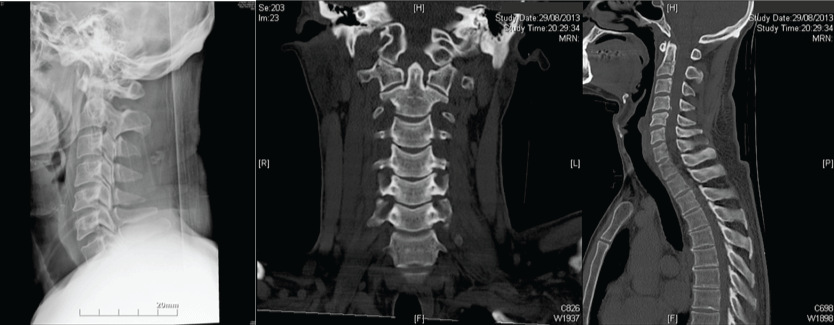
.
Figure 6: Simple radiograph (A) and CT coronal and sagittal views (B,C) does not show the injury.
View Figure 6
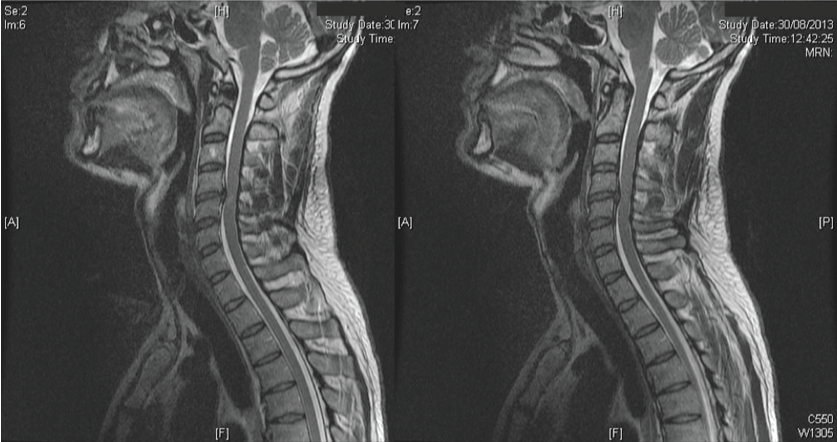
.
Figure 7: Cervical spine magnetic resonance imaging (MRI) scanning show the C5 hernia disc and cord compression at this level.
View Figure 7
Case 4
A 41-year-old male presented to the emergency department after a high-speed motorcycle accident. He was evaluated and treated for multiple leg injuries and a wrist fracture. He underwent a posteroanterior and a lateral thoracic radiograph; both projections were reported to be normal. He was discharge home. Four weeks later he developed progressive legs weakness and also thoracic spine pain. A CT-scan and a MRI were performed, becoming evident a T5 fracture. He underwent a combined anterior and posterior surgical stabilization procedures. He also fully improved after surgery (Figure 8 and Figure 9).
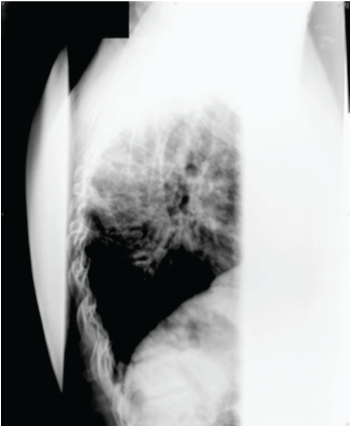
.
Figure 8: Lateral spine radiograph on admission included shoulders obstructing the view of the thoracic spine.
View Figure 8
.
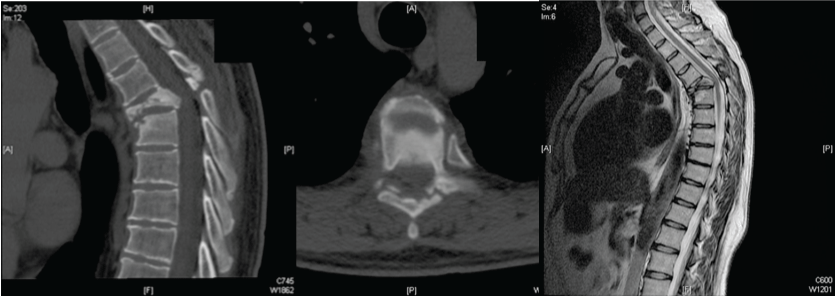
Figure 9: Axial and sagittal CT scan views (A,B) and MR sagittal image (C) show a thoracic injury at the T5 level.
View Figure 9
Discussion
There are several reports in literature about missed spinal fractures in traumatized patients. It is well known the importance of CT in identifying fractures which otherwise may be missed on plain radiographs, particularly at the upper cervical and cervicothoracic spine junction.
There are some recognized useful guides for the evaluation and diagnosis of cervical spine injuries such as The National Emergency X-Radiography Utilization Study (NEXUS) [6] or the Canadian C-Spine Clearance Rule Study [7,8]. They provide guidelines when collars neck should be left in place for patients with normal examinations but with neck pain and the impossibility of carrying out adequate dynamics radiograph examinations in flexion and extension or MRI. Since patients conditions may change, a reevaluation should be performed by an experienced doctor with the intention of trying to avoid overlooked lesions [9]. Some authors [9,10-13], propose tertiary examinations (repeated head-to-toe examination and review of all laboratory and radiologic studies).
In cases of patients who are in a coma or have low levels of consciousness the reevaluation is critical and CT scan must be done in these cases [14,15] if there is a possibility at all of a cervical spinal injury. Special care must be taken in patients with traumatic brain injury [16] as they cannot cooperate during clinical examination, ranging the prevalence of cervical spine injury in these patients between 1.8 to 26% [17].
Another possibility which must be thought is the coexistence of multilevel spinal lesions. Once the diagnosis of a spinal injury is made, a thorough search for some other level lesions must be performed [18]. Hence in case of severe trauma patients (patients who have suffered a fall from height or a traffic accident) an early whole-body CT-scan must be taken [19,20], and should this diagnosis test fail in displaying spinal lesions under the suspicion that a spinal, particularly ligamentous, lesion exists, a MRI will be necessary to complete the study [21], because one of the most common reason for missed injuries is the insufficient imaging studies.
Patients with the diagnosis of ankylosing spondylitis are under an extremely high risk of fracture. Delaying the diagnosis may entail an unexpected catastrophic injury [22], consequently special attention must be paid in these patients as to undergo CT-scan. Cervical spine fractures and dislocations may be very difficult to be diagnosed under x-rays or even by CT-scan, especially at the cervicothoracic junction. Only 52% of cervical fractures will be detected in simple radiographs and under CT scan diagnosis increases up to 98% of the cases. However diagnosis of soft tissues injuries, such as ligamentous injuries, disc hernia, or cord injury, may become a problem in the cervical spine even under CT-scan. In these cases a MRI becomes essential. In any case, physical examination, if at all possible, may be the key in the case that all diagnosis tests are negative. For all patients suspected to have a spinal injury CT scans should be obtained as the initial imaging study [23,24]. Further imaging studies are required if CT-scan is negative and the patient still has spine pain. The Eastern Association for the Surgery of Trauma Practice Management Guidelines Committee (EAST) recommends in patients still on neck pain, leaving the collar in place until a MRI or dynamics flexo-extension radiographs are obtained, once a CT- scan study was normal [25]. Spine MRI has become routine for patients with neurological deficits or inability to cooperate with neurological examination due to coma or intubation.
The damage control orthopaedics, diagnosis algorithms applied to multitrauma patients reduces both morbidity and mortality, particularly those due to missed lesions [26].
References
-
Buduhan G, McRitchie DI (2000) Missed injuries in patients with multiple trauma. J Trauma 49: 600-605.
-
(1994) American College of Surgeons Committee on Trauma. Initial assessment and management. In: Advanced Trauma Life Support Reference Manual. American College of Surgeons, Chicago, 17-37.
-
Pfeifer R, Pape HC (2008) Missed injuries in trauma patients: A literature review. Patient Saf Surg 2: 20.
-
Enderson BL, Reath DB, Meadors J, Dallas W, DeBoo JM, et al. (1990) The tertiary trauma survey: a prospective study of missed injury. J Trauma 30: 666-669.
-
Enderson BL, Maull KI (1991) Missed injuries. The trauma surgeon's nemesis. Surg Clin North Am 71: 399-418.
-
Hoffman JR, Wolfson AB, Todd K, Mower WR (1998) Selective cervical spine radiography in blunt trauma: methodology of the National Emergency X-Radiography Utilization Study (NEXUS) Ann Emerg Med 32: 461-468.
-
Stiell IG, Clement CM, Mc Knight RD, Brison R, Schull MJ, et al. (2003) The Canadian C-Spine Rule versus the NEXUS low-risk criteria in patients with trauma. N Englan J Med 349: 2510-2518.
-
Stiell IG, Wells GA, Vandemheen KL, Clement CM, Lesiuk H, et al. (2001) The Canadian C-spine rule for radiography in alert and stable trauma patients. JAMA 286: 1841-1848.
-
Wei CJ, Tsai WC, Tiu CM, Wu HT, Chiou HJ, et al. (2006) Systematic analysis of missed extremity fractures in emergency radiology. Acta Radiol 47: 710-717.
-
Yang F, Bai XJ, Li ZF (2011) Analysis of misdiagnosis in patients with multiple trauma. Chin J Traumatol 14: 20-24.
-
Howard J, Sundararajan R, Thomas SG, Walsh M, Sundararajan M (2006) Reducing missed injuries at a level II trauma center. J Trauma Nurs 13: 89-95.
-
Thomson CB, Greaves I (2008) Missed injury and the tertiary trauma survey. Injury 39: 107-114.
-
Janjua KJ, Sugrue M, Deane SA (1998) Prospective evaluation of early missed injuries and the role of tertiary trauma survey. J Trauma 44: 1000-1006.
-
Platzer P, Hauswirth N, Jaindl M, Chatwani S, Vecsei V, et al. (2006) Delayed or missed diagnosis of cervical spine injuries. J Trauma 61: 150-155.
-
Saltzherr TP, Beenen LF, Reitsma JB, Luitse JS, Vandertop WP, et al. (2010) Frequent computed tomography scanning due to incomplete three-view X-ray imaging of the cervical spine. J Trauma 68: 1213-1217.
-
Piatt JH Jr (2005) Detected and overlooked cervical spine injury among comatose trauma patients: from the Pennsylvania Trauma Outcomes Study. Neurosurg Focus 19: E6.
-
Chiu WC, Haan JM, Cushing BM, Kramer ME, Scalea TM (2001) Ligamentous injuries of the cervical spine in unreliable blunt trauma patients: incidence, evaluation, and outcome. J Trauma 50: 457-463.
-
Nelson DW, Martin MJ, Martin ND, Beekley A (2013) Evaluation of the risk of noncontiguous fractures of the spine in blunt trauma. J Trauma Acute Care Surg 75: 135-139.
-
Huber-Wagner S, Lefering R, Qvick LM, Korner M, Kay MV, et al. (2009) Effect of whole-body CT during trauma resuscitation on survival: a retrospective, multicentre study. Lancet 373: 1455-1461.
-
Takami M, Nohda K, Sakanaka J, Nakamura M, Yoshida M (2014) Usefulness of full spine computed tomography in cases of high-energy trauma: a prospective study. Eur J Orthop Surg Traumatol 24 Suppl 1: S167-171.
-
Gebauer G, Osterman M, Harrop J, Vaccaro A (2012) Spinal cord injury resulting from injury missed on CT scan: the danger of relying on CT alone for collar removal. Clin Orthop Relat Res 470: 1652-1657.
-
Finkelstein JA, Chapman JR, Mirza S (1999) Occult vertebral fractures in ankylosing spondylitis. Spinal Cord 37: 444-447.
-
Bailitz J, Starr F, Beecroft M, Bankoff J, Roberts R, et al. (2009) CT should replace three-view radiographs as the initial screening test in patients at high, moderate, and low risk for blunt cervical spine injury: a prospective comparison. J Trauma 66: 1605-1609.
-
Hashem R, Evans CC, Farrokhyar F, Kahnamoui K (2009) Plain radiography does not add any clinically significant advantage to multidetector row computed tomography in diagnosing cervical spine injuries in blunt trauma patients. J Trauma 66: 423-428.
-
Como JJ, Díaz JJ, Dunham CM, Chiu WC, Duane TM, et al. (2009) Practice management guidelines for identification of cervical spine injuries following trauma: update from the Eastern Association for the Surgery of Trauma Practice Management Guidelines Committee. J Trauma 67: 651-659.
-
Cerván AM, Cruz E, Cano JR, Jimenez M, Guerado E (2014) Outcome of combined pelvic and spinal lesion in polytrauma patients. Scientific Exhibition AAOS New Orleans Marzo.





