Trauma Cases and Reviews
A Case Report of a Rare Complication of an Intrapelvic Migration of the Lag Screw of a Gamma Nail: Review of the Literature
Dimitrios Georgiannos1,2*, Vasilios Lampridis1 and Ilias Bisbinas1
1424 Military General Training Hospital, Thessaloniki, Hellas, Greece
2Royal Bournemouth Hospital, Bournemouth, UK
*Corresponding author: D. Georgiannos, MD, Consultant Orthopaedic Surgeon, Royal Bournemouth Hospital, Castle Lane East, Bournemouth, BH7 7DW, UK, E-mail: EVI_DIM45@hotmail.com
Trauma Cases Rev, TCR-2-031, (Volume 2, Issue 1), Case Report; ISSN: 2469-5777
Received: January 17, 2016 | Accepted: February 04, 2016 | Published: February 06, 2016
Citation: Georgiannos D, Lampridis V, Bisbinas I (2016) A Case Report of a Rare Complication of an Intrapelvic Migration of the Lag Screw of a Gamma Nail: Review of the Literature. Trauma Cases Rev 2:031. 10.23937/2469-5777/1510031
Copyright: © 2016 Georgiannos D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Gamma nail is a safe internal fixation device widely used for treatment of pertrochanteric fractures. Cut out of lag screw has been reported to be the most frequent mechanical complication. Penetration of acetabulum and intrapelvic migration of the lag screw of the gamma nail is an extremely rare complication. We report two cases of medial migration and penetration of the medial wall of acetabulum by the lag screw of a gamma nail and a comprehensive review of the literature.
We conclude that the careful reaming of femoral head, the achievement of optimal anatomic reduction, the accurate placement of the lag screw, and the regular radiographic follow-up of patients with unstable fracture pattern or imperfect reduction, should be taken in consideration to avoid this rare but devastating complication of the use of gamma nail.
Introduction
The gamma nail has been widely used for the treatment of trochanteric fractures. It was introduced in 1988 and after three modifications of its design it has successfully been in use till today, considered as a first choice option of internal fixation of pertrochanteric fractures. It combines the biomechanical advantages of a sliding hip screw with those of an intramedullary nail. The sliding hip screw provides a controlled impaction of the fracture, thus increasing the stability of fracture and decreasing the bone healing time. The intramedullary nail sits nearer to the weight bearing axis, reducing the bending stresses up to 30% [1].
One of the most common complications associated with the use of the gamma nail and the other intramedullary devices is the cut out of the lag screw. As a consequence to cut out is the medial migration of the screw into pelvis, which is considered as a rare complication [2]. This article presents two cases of medial intrapelvic migration of the lag screw of the gamma nail and a comprehensive review of the literature regarding this very rare but devastating complication.
Case 1
A 69-year-old female with known history of metastatic breast Ca and pathological intertrochanteric fracture of right hip which was treated with a short gamma nail five months ago in another institution, admitted after a fall from standing position. She was complaining of pain of right hip and was unable to walk. Radiographs revealed a fixation failure with intrapelvic lag screw migration, screw disengagement from the nail, proximal migration of the nail and distal screws breakage (Figure 1). Also, X-rays revealed metastatic lesions of left hip trochanteric area with no actual fracture. She underwent revision fixation of right hip with insertion of a long gamma nail locked distally with two screws. It was notable that the lag screw had penetrated the acetabular fossa posteriorly. The metalwork was removed without any subsequent complications although due to extreme medial migration of the lag screw a vascular surgeon was available to get involved. She additionally underwent prophylactic nailing of left hip with a long gamma nail (Figure 2). She mobilized partially weight bearing for two months and then fully weight bearing as tolerated. She was followed up for five months and she had an uneventful rehabilitation postoperatively. Unfortunately she died seven months later due to metastatic disease.
.
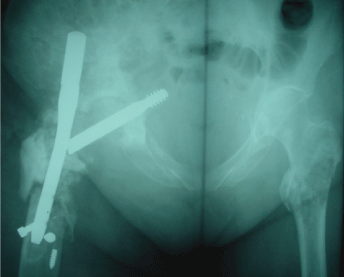
Figure 1: Anteroposterior radiograph of pelvis shows disengagement of lag screw from a short gamma nail, medial migration into pelvis and breakage of the distal screws.
Note: The metastatic lesions in the trochanteric area of the opposite hip.
View Figure 1
.
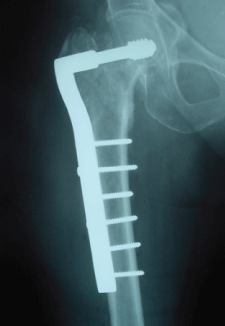
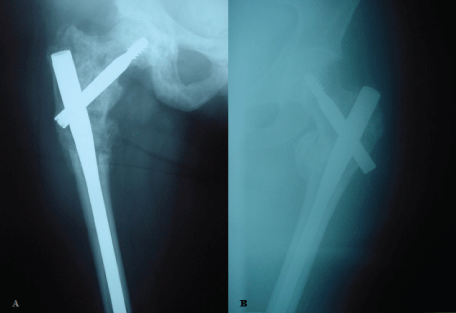
Figure 2: Radiographs showing revision intramedullary fixation of the right hip (A) and the primary prophylactic fixation of the left one (B).
View Figure 2
Case 2
An 82-year-old female admitted with painful right hip after a fall and inability to walk. Radiographs revealed a reverse oblique fracture of right hip with subtrochanteric extension (AO 31-A3). The fracture was fixed with a long gamma nail locked distally with two screws (Figure 3). She mobilized fully weight bearing and discharged home. At six weeks, the follow-up radiographs revealed penetration of the acetabulum and migration of the lag screw into pelvis (Figure 4). After removal of the gamma nail the fracture fixed with a dynamic condylar screw (DCS) plate (Figure 5). Four months post revision operation the patient was discharged from the clinic with confirmed clinical and radiological union of the fracture.
.
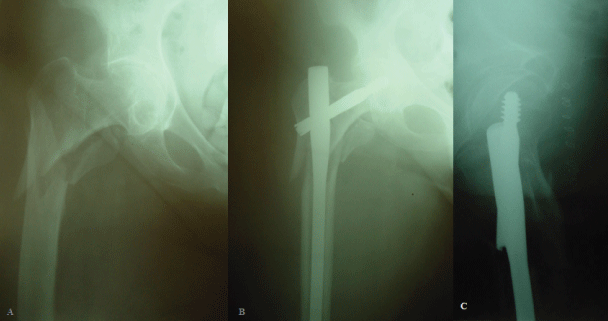
Figure 3: Radiographs showing an unstable reverse oblique intertrochanteric fracture of right hip (A) and intramedullary fixation with a long gamma nail (B,C).
View Figure 3
.
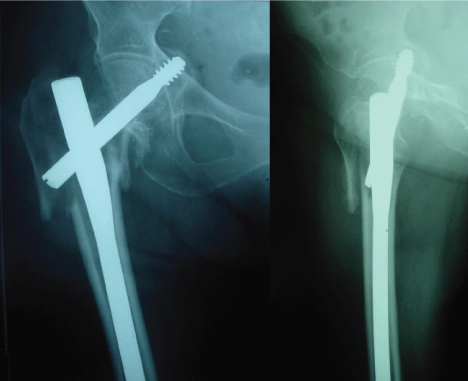
Figure 4: AP and lateral radiograph showing penetration of the acetabulum and migration of the lag screw into pelvis six weeks postoperatively.
View Figure 4
Discussion
The cut out of the lag screw has been reported to be the most frequent mechanical mode of failure for internal fixation devices for treatment of trochanteric hip fractures with an incidence up to 7.2% [3]. Although cut out of the lag screw or penetration of the femoral head is the key element for intrapelvic migration of gamma nail lag screw [2], the latter complication is considered to be extremely rare. Only 3 cases (Table 1) of medial intrapelvic migration of the lag screw of a gamma nail have been reported in the English literature [2,4].
![]()
Table 1: Literature review.
View Table 1
Migration of lag screw in a double cervical screw device has been explained by the so-called “Z-effect” phenomenon, where the proximal lag screw migrates medially and the distal one migrates laterally [5]. So far, there is only one biomechanical study which gives an explanation about the mechanism that could cause medial migration. Weil et al. reported a study where gamma nail lag screw (among others) began to “walk” medially while rotation and axial loading with weight bearing occurred [6]. The authors were able to prove medial migration of the lag screw in all five examined implants (TFN, PFN, PFNA, Gamma3, IMHS) without any statistical difference between these implants. It should be stressed out that this complication was not observed with the sliding hip screw.
Specific conditions had to be fulfilled to achieve medial migration of the femoral neck element. These included deficiency of the lateral buttress, an unstable medial cortex, constant controlled friction within the femoral head, an axial load loading in varus. The authors concluded that there might be a small increased risk of medial migration in unstable fractures with or without a great trochanter fracture.
Lag screw cutout has also been shown to be dependent on the position of the screw within the femoral head. Optimizing tip-apex distance is critical in preventing fixation failure when using an extramedullary sliding hip screw to fix pertrochanteric fractures. A recent study suggests that placement of the lag screw of the gamma nail inferiorly in the AP plane and centrally in the lateral plane maximizes biomechanical stiffness and load-to-failure of the fixation [7].
In the first case of our study, there was an intertrochanteric fracture in a bed of metastatic lesion of pertrochanteric area with deficient lateral buttress, unstable medial cortex and a delayed union due to carcinomatosis. In the second case the fracture was a reverse oblique intertrochanteric with subtrochanteric extension. By definition it was an unstable fracture which was suboptimally reduced and fixed in varus position with the lag screw in retroverted position in the femoral head. We hypothesized that in both cases the locking mechanism of lag screw had failed and the lag screw advanced medially rather cut out of the femoral head.
Flint et al. summarized the proposed risk factors for femoral head and acetabulum penetration and medial migration of lag screws in five categories; i) intraoperative surgeon-related factors: damage of femoral head by over-reaming, malposition of lag screw, ii) intraoperative fracture-related factors: lateral buttress deficiency, unstable medial cortex, malreduction in varus position, osteoporotic bone, distraction of fracture site due to non weight bearing restrictions, iii) implant-related factors: nail/lag screw dysfunction, set screw dysfunction, nail toggling, iv) technical mistakes: too great tip-apex distance, superior/anterior placement of lag screw in the femoral head, inadequate lag screw length, v) postoperative factors: fall, additional trauma, abnormal forces to hip articulation [2].
Conclusion
Gamma nail is a safe internal fixation device indicated for complex and unstable intertrochanteric and subtrochanteric fracture patterns. It has got very low complication rates with cut out of lag screw the most frequently reported. Medial intrapelvic migration of the lag screw is an extremely rare complication. To further avoid this rare but devastating complication, we recommend surgeons should:
1. Avoid damage to femoral head and over-reaming
2. Achieve optimal and anatomic reduction of fracture
3. Accurately place the lag screw (with a tip-to-apex distance less than 25mm and placement of the lag screw inferiorly in the AP plane and centrally in the lateral plane)
4. Use appropriate length lag screw
5. Secure the set screw locking mechanism
6. Radiographic follow-up of patients with unstable fracture patterns and imperfect fracture reduction
References
-
Valverde JA, Alonso MG, Porro JG, Rueda D, Larrauri PM, et al. (1998) Use of the Gamma nail in the treatment of fractures of the proximal femur. Clin Orthop Relat Res: 56-61.
-
Flint JH, Sanchez-Navarro CF, Buckwalter JA, Marsh JL (2010) Intrapelvic migration of a gamma nail lag screw: review of the possible mechanisms. Orthopedics 33.
-
Bojan AJ, Beimel C, Speitling A, Taglang G, Ekholm C, et al. (2010) 3066 consecutive Gamma Nails. 12 years experience at a single centre. BMC Musculoskelet Disord 11: 133.
-
Lucke M, Burghardt RD, Siebenlist S, Ganslmeier A, Stöckle U (2010) Medial migration of lag screw with intrapelvic dislocation in gamma nailing--a unique problem? A report of 2 cases. J Orthop Trauma 24: e6-e11.
-
Strauss EJ, Kummer FJ, Koval KJ, Egol KA (2007) The "Z-effect" phenomenon defined: a laboratory study. J Orthop Res 25: 1568-1573.
-
Weil YA, Gardner MJ, Mikhail G, Pierson G, Helfet DL, et al. (2008) Medial migration of intramedullary hip fixation devices: a biomechanical analysis. Arch Orthop Trauma Surg 128: 227-234.
-
Kuzyk PR, Zdero R, Shah S, Olsen M, Waddell JP, et al. (2012) Femoral head lag screw position for cephalomedullary nails: a biomechanical analysis. J Orthop Trauma 26: 414-421.
-
Heineman DJ, van Buijtenen JM, Heuff G, Derksen EJ, Pöll RG (2010) Intra-abdominal migration of a lag screw in gamma nailing: report of a case. J Orthop Trauma 24: e119-122.