Trauma Cases and Reviews
Tibial Plateau in Combination with Diaphyseal Fracture: A Case Study
Ran Atzmon, Dror Lindner, Zachary T. Sharfman*, Oded Rabau, Yiftah Beer and Gabriel Agar
Department of Orthopaedic Surgery, Arthroscopic Surgery and Sports Medicine units, Assaf Harofeh Medical Center, Zerifin, Israel
*Corresponding author: Zachary Sharfman T, Department of Orthopaedic Surgery, Arthroscopic Surgery and Sports Medicine units, Assaf Harofeh Medical Center, Zerifin, Israel, E-mail: zachsharfman@gmail.com
Trauma Cases Rev, TCR-2-032, (Volume 2, Issue 1), Case Report; ISSN: 2469-5777
Received: November 14, 2015 | Accepted: February 06, 2016 | Published: February 09, 2016
Citation: Atzmon R, Lindner D, Sharfman ZT, Rabau O, Beer Y, et al. (2016) Tibial Plateau in Combination with Diaphyseal Fracture: A Case Study. Trauma Cases Rev 2:032. 10.23937/2469-5777/1510032
Copyright: © 2016 Atzmon R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Simultaneous tibial plateau and diaphyseal tibial fractures are a rare occurrence and have seldom been reported in the literature. Each fracture requires a different surgical approach, which creates challenges for the operating physician. Tibial plateau fractures require anatomical reduction and restoration of the joint line in order to achieve rigid fixation and immediate mobilization of the joint. Conversely, diaphysis tibial fractures can be treated with relative stability and do not require anatomical reduction and fixation. The unique combination of tibial plateau and diaphysis tibial fractures is challenging, as the two pathologies require vastly different interventions performed in the same location. This case presents a single operation composed of two stages, starting with fixation of the diaphyseal fracture using an intra-medullary nail (IMN), and arthroscopic assisted closed reduction and internal fixation using cannulated screws for co-contaminant tibial plateau and diapheseal tibial fracture.
Introduction
Tibial plateau fractures present a disturbance in the joint congruency, occurring in the articular part of the proximal tibia, and affecting the stability and motion of the knee. Tibial plateau fractures comprise only 1% of all fractures [1]. The characteristics of tibial plateau fractures depend on the interplay between anatomy of the tibia, and the direction of force and the energy applied to the limb. A high-energy fracture might increase comminution and distinct fracture patterns compared to low energy fracture patterns. In addition, high-energy fractures are frequently associated with significant soft tissue injury, as well as meniscal and ligamentous injuries to the knee, which necessitate further treatment and consideration [2].
In cases involving both tibial plateau and diaphyseal fractures, the goals of treatment include anatomic restoration of the joint line to achieve rigid fixation allowing for immediate mobilization of the joint in addition to addressing soft tissue injuries [3]. As opposed to tibial plateau fractures, diaphyseal tibial fractures can be treated with relative stability and do not require anatomical reduction and fixation. Both fracture types are usually caused by a high-energy trauma associated with motor vehicle accidents or a fall from height. The incidence of co-contaminant tibial plateau fracture and diaphyseal tibial fracture is rare and has rarely been reported in the literature. This may be due to the different mechanistic patterns of fracture and associated force transfer unique to each fracture type [2-4].
Case Presentation
A 40-year-old male with presented to the emergency department after a motorcycle accident wearing a full head helmet without additional protective gear. He was examined on site and complained of pain in his right lower leg. His Glasgow Coma Scale was 15' and vital signs were normal. On his admission to the emergency room he was rushed to the trauma room and was further examined by both general and orthopaedic surgeons. The patient described a direct blow to the right lower leg.
Examination revealed deformity and swelling of the distal third of the right shin. Palpation of the area revealed tenderness. Manual muscle testing of the foot and neurovascular screening of the left lower extremity were normal. Peripheral pulses where checked in addition to sensory innervation in the entire limb and distal motor function of the ankle and foot. While examining the patients shin, the knee appeared swollen, palpation of the lateral knee joint line elicited pain. No further evaluation of knee was possible due to pain. The laboratory tests were normal.
.
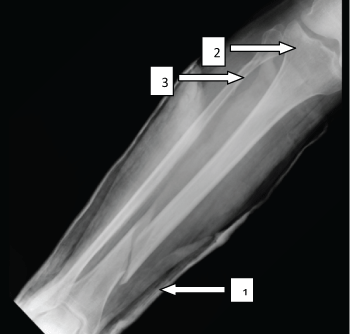
Figure 1: Coronal X-ray demonstrating a spiral distal tibial fracture with less than 50% translation (1), anon-compression tibial plateau fracture (2) and a high fibular fracture (3).
View Figure 1
.
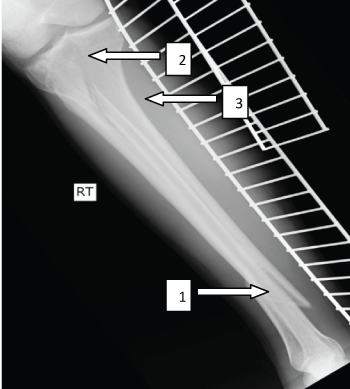
Figure 2: Sagital X-ray demonstrating the translation of the distal tibialfracture (1), atibial plateau fracture (2) and a fibular fracture with translation (3).
View Figure 2
X-ray of the right lower leg revealed a high spiral fibular fracture and a diaphyseal fracture of the tibia in the transition zone between the middle and distal thirds (Figure 1 and Figure 2). Due to high index of suspicion based on the clinical examination further X-rays of the entire leg were taken and revealed a lateral tibial plateau fracture with depression. CT scan confirmed the lateral tibial plateau fracture with a depression of 5 millimeters and a split component (Schatzker II) with no loose bodies inside the joint, as well as an oblique comminuted fracture in the proximal fibula, knee effusion and diaphyseal fracture (Figure 2, Figure 3 and Figure 4). The patient was treated with a temporary long posterior splint applied to the leg, analgesic medication, and a toxoid vaccine.
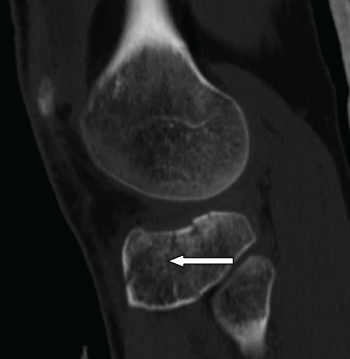
.
Figure 3: Sagittal CT demonstrating a splitting tibial plateau fracture (Schatzker type II).
View Figure 3
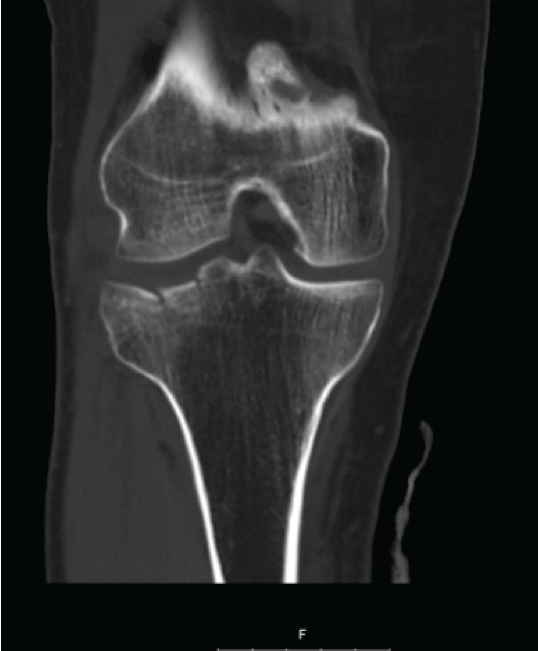
.
Figure 4: Coronal CT view demonstrating the lateral splitting tibial plateau fracture (Schatzker type II).
View Figure 4
Surgical Procedure/Follow-up
Less than 24 hours after admission the patient underwent a two stages surgery with general anesthesia.
First stage - Treating the diaphyseal tibial fracture - A midline incision above the patellar tendon was executed, splitting of the tendon. A guide wire was inserted and remained in the medullary canal. Under guided fluoroscopy an intra-medullary nail was introduced using a medial Polar Screw to maintain leg axis, and two proximal locking screws as well as three distal locking screws were placed.
Second stage - Upon achieving reduction and fixation of the diaphysael fracture, two arthroscopic portals were established in the knee (antero-lateral and antero-medial). The pump used was a FMS duo system (DePuy Synthes, Warsaw, Indiana) and the pump was set to maintain a pressure of 40 mmHg throughout the surgery. The arthroscope was introduced and thorough examination demonstrated comminution and depression of the lateral tibial plateau as well as a gap between the lateral meniscus and the plateau. Using a standard anterior cruciate ligament (ACL) tibial drill guide (Smith & Nephew, Andover, MA), which was set on 60°, a guide was inserted through the intra medullary nail entrance point to the center of the depressed fragment. Verification of the guides’ position was confirmed with fluoroscopy and arthroscopic visualization.
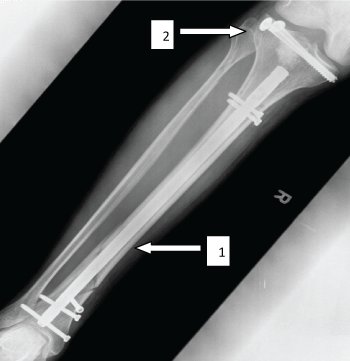
.
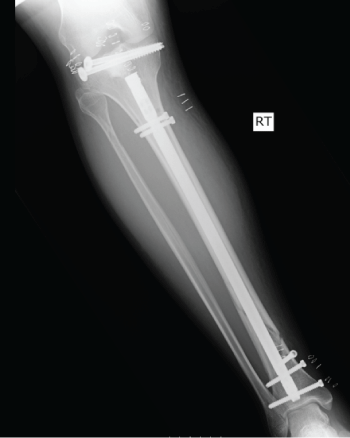
Figure 5: Post-operative X-ray, demonstrating intra medullary nail in the tibial diaphysis (1) and two cannulated screws in the tibial plateau after elevating and restoring the joint line (2).
View Figure 5
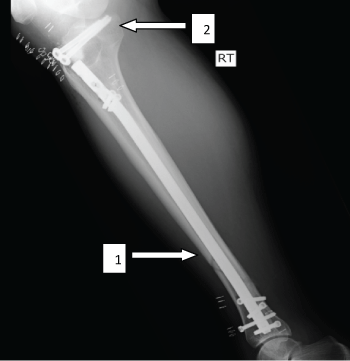
.
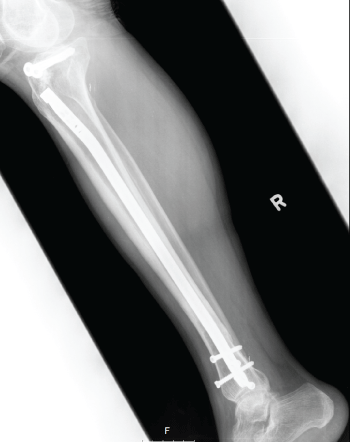
Figure 6: Post-operative X-ray, demonstrating intra medullary nail in the tibial diaphysis (1) and two cannulated screws in the tibial plateau after elevating and restoring the joint line (2).
View Figure 6
A specially angulated cannulated tamp, was used to elevate the fracture site under direct arthroscopic visualization. The area of maximum depression of the tibial plateau was identified and a 2 mm K-wire was inserted from the metaphyseal region to the articular surface through the ACL ligamentoplasty tibial guide (Smith & Nephew) at a sixty degrees angle. This served as a guide for medial corticotomy of the tibia, which can be performed using an 8-10 mm cannulated drill, with a cylindrical beater (Arthrex, Inc., Naples, FL). The depressed fragments are then gently elevated altogether with the cancellous bone underneath, visualizing the restoration of the articular surface. Bone reduction forceps were used to reduce the split fracture. The bony defect was filled with 15 cc of tri-calcium sulfate (TCP) (Science and Bio materials, France) and two cannulated screws (7 mm diameter) (DePuy Synthes, Warsaw, Indiana) were inserted parallel to the joint line under the subchondral bone. Postoperative X-rays demonstrate the final fixation in figure 5, figure 6, figure 7 and figure 8.
Non-weight bearing was instructed for 6 weeks after the procedure in a hinged knee brace locked in the 0-30 position (post op lite knee brace, Breg). Non-weight bearing was followed by 4 weeks of partial weight bearing in the brace. Range of motion was gradually increased until full range of motion was achieved at 3 month post-surgery. The patient was released from the hospital two days after surgery and immediately began physical therapy to improve range of motion activities and muscle strengthening. The hinged knee brace was used for 12 weeks. At the three month follow-up both fractures had healed with good alignment. Full weight bearing and knee range of motion from 0-120° was achieved by three months.
At 6 month follow-up the patient remains in physiotherapy 3 times a week at an outpatient physical therapy center. He complained of minor pain and limitation of motion in the ankle joint without pain or limitation in the knee joint. On physical examination the patient walks with a minor antalgic gate. The scars are well healed, without effusion or redness. The patient has full range of motion in the knee joint, extension 0 flexion 135, without pain. The ankle joint has full planter flexion 20 degrees (equal with contralateral side), 10 degrees dorsiflexion in knee extension and 20 degrees in knee flexion. There are neurovascular deficits. On X-ray the bony structures showed good fracture healing with acceptable alignment.
At one year 1-year follow-up the patient participates in physical therapy twice weekly. The only complaint is pain related to hardware protrusion into soft tissue specifically related to the distal IMN screws, which can be palpated. The patient returned to work walks without a cane, has a moderate antalgic gate. His range of motion is equal bilaterally with significant improvement in the ankle since the 6 month follow-up. The patient is awaiting surgery to remove hardware and had a Tenger Lysholm knee score of 81 (good to fair 65-83).
Discussion
Intra-articular fractures pose challenges for orthopedic surgeons due to high severity of trauma, associated soft tissue injuries and the necessity for anatomic reduction. The advantages of surgical intervention include early mobilization, stable reduction and anatomic restoration of knee joint alignment. This helps to avoid sequaela of intra articular fractures, which include pain, osteoarthritis, limited mobility and many others.
Arthroscopy assisted minimally invasive surgery has become a popular method to treat tibial plateau fractures because it allows direct visualization of the intra-articular fractures and accurate fracture reduction as well as diagnosis and treatment of meniscal, ligamentous, and soft tissue injuries. Additionally, the technique allows for thorough-joint lavage, and removal of loose fragments. The advantages arthroscopy assisted minimally invasive surgery included a reduced rate of infection and compartment syndrome, with increased preservation of blood vessels, nerves and soft tissues in comparison to open surgery [1,3,5,6]. Arthroscopy assisted tibial plateau fracture fixation has potential complications including compartment syndrome [7,8]. Pump irrigation should be maintained at less than 50 mmHg and the calf should be inspected throughout the operation to avoid compartment syndrome [7,8].
The combination of tibial plateau and diaphysis fracture is rarely described in the literature. Usually the diaphyseal fracture will be the most prominent component in physical exam and thus attracts the treating physician’s attention. This might mask a concurrent tibial plateau fracture. In all multiple trauma patients a thorough physical exam should conducted with systemic approach to ensure that all joints are evaluated.
In this case the tibial plateau fracture was Schatzker type II and presented with mild finding on X-ray. Even in an isolated setting these fractures require a high index of suspicion for additional fractures. In the setting of additional injuries in the ipsilateral limb, the likelihood of missing additional injuries is increased. It is therefore recommended that the physician thoroughly evaluates injuries to assess the need for further imaging.
In this case the operation first focused on fixation of the diaphyseal tibial fracture using IMN inserted through the patellar tendon. By first achieving fixation of the tibial diaphysis stability was restored to the limb and the articular joint line. This created a better working platform for tibial plateau fixation. After surveying the knee for lavage arthroscopically, the IMN entry point (used for diaphaseal fixation) was used for reduction and elevation of the tibial plateau. Using this portal eliminated an accessory incision and another entry point for infection as well as additional soft tissue damage. This technique is safe, reproducible and employs minimal invasive techniques, causing minimal soft tissue disturbance while allowing for anatomic reduction and fixation of both fractures.
In conclusion, the combination of tibial diaphyseal and tibial plateau fractures is a rare entity, which might be missed. A high index of suspicion, thorough physical exam, with radiographic imaging is necessary to avoid misdiagnosis. In more complicated cases advanced imaging such as CT or MRI can be employed for better visualization. Once diagnosed surgical intervention fixating the diaphyseal fracture with an IMN, and the tibial plateau with and arthroscopic assisted technique, using the IMN entry point to elevate the depressed fragment provided good outcomes in this case. Fixation of the tibial plateau fracture can be achieved with cannulated screws and plate or screws alone.
References
-
Atesok K, Doral MN, Whipple T, Mann G, Mei-Dan O, et al. (2011) Arthroscopy-assisted fracture fixation. Knee Surg Sports Traumatol Arthrosc 19: 320-329.
-
Berkson EM, Virkus WW (2006) High-energy tibial plateau fractures. J Am Acad Orthop Surg 14: 20-31.
-
Chan YS (2011) Arthroscopy- assisted surgery for tibial plateau fractures. Chang Gung med J 34: 239-247.
-
Kwok CS, Crossman PT, Loizou CL (2014) Plate versus nail for distal tibial fractures: a systematic review and meta-analysis. J Orthop Trauma 28: 542-548.
-
Rademakers MV, Kerkhoffs GM, Sierevelt IN, Raaymakers EL, Marti RK (2007) Operative treatment of 109 tibial plateau fractures: five- to 27-year follow-up results. J Orthop Trauma 21: 5-10.
-
Marsh JL, Smith ST, Do TT (1995) External fixation and limited internal fixation for complex fractures of the tibial plateau. J Bone Joint Surg Am 77: 661-673.
-
Burdin G (2013) Arthroscopic management of tibial plateau fractures: Surgical technique. Orthop Traumatol Surg Res 99: S208-S218.
-
Scheerlinck T, Ng CS, Handelberg F, Casteleyn PP (1998) Medium-term results of percutaneous, arthroscopically-assisted osteosynthesis of fractures of the tibial plateau. J Bone Joint Surg [Br] 80: 959-964.