Trauma Cases and Reviews
The Trauma Associated with TMJA and Surgical Methods of Temporomandibular Joint Ankylosis
Jin Qiu and Ming Zhang*
Department of Oral and Maxillofacial Surgery, Chinese People's Liberation Army General Hospital Hainan Branch, China
*Corresponding author: Ming Zhang, Department of Oral and Maxillofacial Surgery, Chinese People's Liberation Army General Hospital Hainan Branch, Hai tang Bay, Sanya, Hainan province, China, Tel: 15692538791, E-mail: doctorzm@163.com
Trauma Cases Rev, TCR-2-033, (Volume 2, Issue 1), Case Report; ISSN: 2469-5777
Received: November 16, 2015 | Accepted: February 22, 2016 | Published: February 25, 2016
Citation: Qiu J, Zhang M (2016) The Trauma Associated with TMJA and Surgical Methods of Temporomandibular Joint Ankylosis. Trauma Cases Rev 2:033. 10.23937/2469-5777/1510033
Copyright: © 2016 Qiu J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Temporomandibular Joint Ankylosis (TMJA) is a severe disease which affects the function of oral and maxillofacial system. It leads to mouth opening limitation, facial deformity and OSAHS in the severe cases. The most common cause of ankylosis involves trauma, most frequently associated with condylar fractures [1]. The surgical treatment following the functional training is the best option. Its surgical treatment involves three aspects:to remove the anatomic factors of ankylosis, to restore or rebuilt the structure of TMJ,and to remedy secondary deformities [2,3]. This case presents the progress of TMJ ankylosis, clinical features and surgical management.
Keywords
Ankylosis, Temporomandibular joint, Trauma, Arthroplasty
Introduction
Temporomandibular joint ankylosis is defined as bony or fibrous adhesion of the anatomic joint components. The causes of TMJ ankylosis includes trauma, local or systemic infection and etc. Retrospective studies of TMJ ankylosis showed trauma was the most common etiology. Most of the traumatic temporomandibular joint ankylosis was caused by condylar fracture. And the sagittal and comminuted fracture of the mandibular condyle were the main type of condylar fracture causing temporomandibular joint ankylosis [2,3]. The TMJ ankylosis usually cause a limitation in opening the mouth, causing difficulties with mastication, speaking and oral hygiene as well as influencing mandibular growth. When TMJ ankylosis occurs in childhood, it can retard mandibular development, and will lead to maxillofacial deformity such as facial asymmetry, micrognathia, bird face deformity, create malocclusion and aggravate psychological disorders. It is very difficult to treat TMJ ankylosis in clinical condition. Although various techniques have been described, the treatment results remain unsatisfied. Re-ankylosis is one of the most frequently seen complications [4,5]. Here is a case about the patient who had condylar fracture in his childhood and developed into temporomandibular joint ankylosis that makes him unable to open his mouth, to chew food, to have developed facal deformity.
Case Report
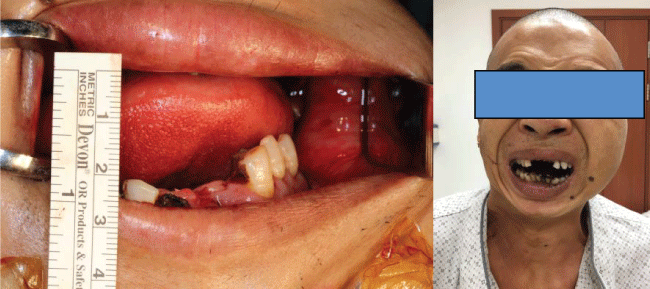
Man 35 years old. He fell from tree with the chin hitting on the ground at the age of nine, leading to the condylar fracture. In the rural area, people lack of conscious of doctor, so we have no idea about the treatment that he took at that time. After the trauma, he begun to unable to open his mouth, from 2 mm to complete limited mouth opening during 2 years. Now he came to doctor because he cannot open his mouth for 24 years. He is diagnosed as temporomandiblular joint ankylosis, with maxillofacial deformity, facial asymmetry, micrognathia, malocclusion, complete restriction of opening, bad oral hygiene (Figure 1). The CT scan shows the left TMJ is completely obliterated by bony ankylotic mass growing between the mandibular ramus and cranial base (Figure 2). The right side the head of the condylar process is visible but significantly deformed, with the fibrous adhesions making TMJ movement impossible (Figure 2). We designed a preauricular incision in order to expose the ankylosis compeletly with hidden beauty and advoid facial nerve damage, our operative protocol for the left TMJ ankylosis entailed resection of ankylotic mass, arthroplasty, interpositional tissue transfer to the TMJ with temporalis fascial flap, the right TMJ was dealed with fibrous tissue release and partly condylar head resection (Figure 3). After the surgery he can open his mouth to 25 mm.
.
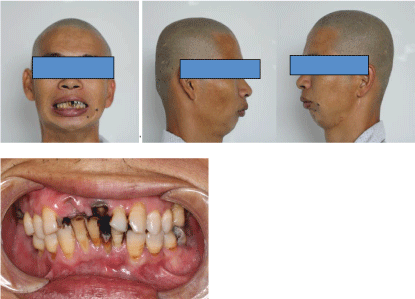
Figure 1: The patient have no movement of his mandibular, completely restriction in opening mouth, bird face, malocclusion, bad oral hygiene.
View Figure 1
.
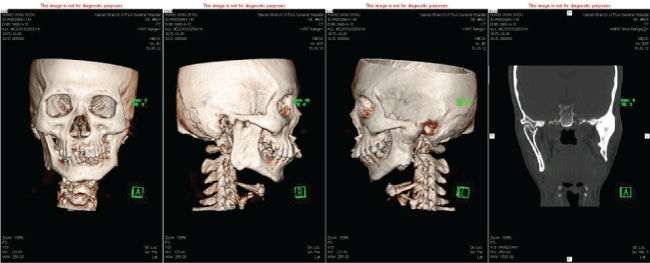
Figure 2: CT Scan show the left TMJ bony ankylotic mass, the right condylar head dislocation and maxillofacial deformity.
View Figure 2
.
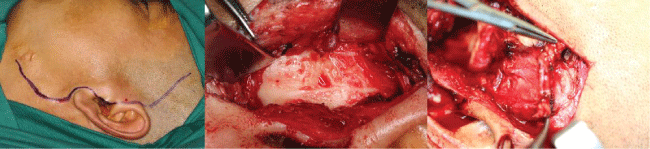
Figure 3: The left side preauricular incision to show the bony ankylotic mass, recontruction the condylar and interpositional tissue with the temporalis superficial fascial flap.
View Figure 3
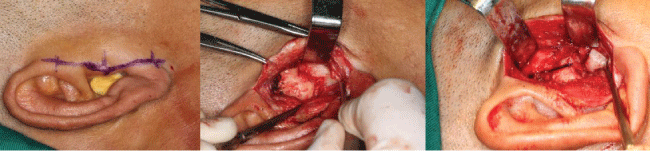
The right side preauricular incision, the fibrous adhsion in articular disc and glenoid fossa,arthroplasty of the joint cavity (Figure 4). The interincisal opening of 25 mm (Figure 5).
.
Figure 4: The right side preauricular incision, the fibrous adhsion in articular disc and glenoid fossa,arthroplasty of the joint cavity.
View Figure 4
Summary and Conclusion
Temporomandubular joint ankylosis is an intracapsular union of the condyle and the temporal articular surface that restricts mandibular movements, including fibrous adhesions or bony fusion between the condyle, disc, glenoid fossa, and articular eminence. The leading causes include trauma and infection. In this case, the man surffered from a trauma that makes mandibular fracture and was not treated properly, thus developed to temporomandibular joint ankylosis. It can be a serious and disabling condition that leads to difficulties in mastication, swallowing, chewing, esthetics and oral hygiene. The treament of TMJ ankylosis poses a significant challenge because of technical difficulties and a high incidence of recurrence. Its treatment includes the orthodontist, oral and maxillofacial surgeon [6]. Sawhney (1986) divided TMJ ankylosis into 4 types: Type I: The head of the condylar process is visible but significantly deformed, with the fibroadhesions making TMJ movement impossible; Type II: Consolidation of the deformed head of the condylar process and articular surface occurs mostly at the edges and in the anterior and posterior parts of the structures, and the medial part of the surface of the condylar head remain undamaged; Type III: The ankylotic mass involves the mandibular ramus and zygomatic arch; an atrophic and displaced fragment of the anterior part of the condylar head is in a medial location; Type IV: TMJ is completely obliterated by bony ankylotic mass growing between the mandibular ramus and cranial base. According to the classification of the TMJ ankylosis proposed by Sawhney, the treatment protocol for Type I ankylosis was fibrous tissue release or condylar head resection with costochondral graft (CCG) and temporalis myofascial flap (TMF). For Type II ankylosis, the lateral bony fusion was resected while the intact residual condylar fragment displaced medially was remained. The operation was named "lateral arthroplasty" (LAP). TMF or masseter muscle flap (MMF) was used as a barrier in the lateral gap between temporomandibular joint fossa and stump of the mandibular ramus. If the medial condylar fragment was too small to bear the load, it was resected with the bony mass. The joint was reconstructed with CCG and TMF or MMF [7-10]. For Type III and IV ankylosis, the bony fusion was completely removed and the joint was reconstructed with CCG and TMF or MMF. Autogenous bone grafts includes non-vascular and vascular grafts, various non-vascularised free autogenous bone grafts from the tibial or clavicular bone, sternoclavicular joint, iliac crest, metatarsal bone or metatarsophalangeal articulation are used, autogenous vascular grafts harvested from rib, iliac crest or tibial bones. Another resource to reconstruct the TMJ is the use of alloplastic prosthesis joint replacement. Thanks to the development of the technology and materials, detailed imaging such as computed 3D tomography and the preparation of stereolithographic models has allowed the construction of an individual prosthesis for each patient [11,12]. According to a classic approach, autogenous tissues should be used in the treatment of developmental and functional disorders accompanying TMJ ankylosis in children. Theoretically, autogenous grafts should grow together with the patient. In practice, however, post-surgical performance of grafts involves undesirable phenomena such as resorption, unpredictable overgrowth, secondary asymmetry and even re-ankylosis. A treatment by means of TMJ prosthesis should be considered in the cases of serious anatomical and functional disorders of TMJ, failure of the previous therapy carried out using a free bone graft, recurrent ankylosis, or unpredictable overgrowth, Although a customized individual CAD/CAM TMJ reconstruction seems very expensive, its overall long-term cost is often equal to or less than that of autogenous TMJ reconstruction. After all, the long-termed treatment effect continued to be observed.
References
-
Yang Chi, He Dong-mei, Chen Min-jie, Zhang Xiao-hu, Qiu Ya-ting, et al. (2011) Classification and treatment of traumatic temporomandibular joint ankylosis: An analysis of 84 consecutive patients. China J Oral Maxillofac Surg 9: 45-50.
-
Akama MK, Guthua S, Chindia ML, Kahuho SK (2009) Management of bilateral temporomandibular joint ankylosis in children: case report. East Afr Med J 86: 45-48.
-
Jiang Yangmei (2015) Two-stage treatment protocol for the management of temporomandibular joint ankylosis with secondary deformities in adults. J Pract Stomatol 31.
-
Jain G, Kumar S, Rana AS, Bansal V, Sharma P, et al. (2008) Temporomandibular joint ankylosis: a review of 44 cases. Oral Maxillofac Surg 12: 61-66.
-
Movahed R, Mercuri LG (2015) Management of temporomandibular joint ankylosis. Oral Maxillofac Surg Clin North Am 27: 27-35.
-
Maki MH, Al-Assaf DA (2008) Surgical management of temporomandibular joint ankylosis. J Craniofac Surg 19: 1583-1588.
-
Xue Guo-chu, Xu Ping-ping, Ai Wei-jian, Zhou Hui-xi, Liu Shu-guang, et al. (2006) Application of temporalis myofascial flap combined with coronoid process graft in the treatment of temporomandibular joint ankylosis. China J Oral Maxillofac Surg 4: 189-193.
-
Mercuri LG (2008) Temporomandibular Joint Reconstruction. In: Fonseca R Oral and Maxillofacial Surgery. Elsevier, Philadelphia 945-960.
-
Zhou Qing (2013) Classification and treatment of temporomandibular joint. Chinese Journal of Practical Stomatology 6.
-
Smith JA, Sandler NA, Ozaki WH, Braun TW (1999) Subjective and objective assessment of the temporalis myofascial flap in previously operated temporomandibular joints. J Oral Maxillofac Surg 57: 1058-1065.
-
Sawhney CP (1986) Bony ankylosis of the temporomandibular joint: follow-up of 70 patients treated with arthroplasty and acrylic spacer interposition. Plast Reconstr Surg 77: 29-40.
-
Xie Geng - yun, Nan Xin -rong (2008) Clinical research into operation in true ankylosis of temporomandibular joint. Chinese Journal of Practical Stomatology.