Trauma Cases and Reviews
Pigmented Villonodular Synovitis: Unusual Locations in Two Young Soccer Players
Yanguas Javier*, Domí nguez David, Florit Daniel, Terricabras Joaquim, Puigdellí vol Jordi, Brau Juan José , Lizárraga Marí a Antonia and Pruna Ricard
Futbol Club Barcelona Medical Department, Barcelona, Spain
*Corresponding author: Javier Yanguas, Futbol Club Barcelona Medical Department, Barcelona, Spain, E-mail: xavier.yanguas@fcbarcelona.cat
Trauma Cases Rev, TCR-2-036, (Volume 2, Issue 2), Clinical Cases; ISSN: 2469-5777
Received: January 12, 2016 | Accepted: March 25, 2016 | Published: May 01, 2016
Citation: Yanguas J, David D, Daniel F, Joaquim T, Jordi P, et al. (2016) Pigmented Villonodular Synovitis: Unusual Locations in Two Young Soccer Players. Trauma Cases Rev 2:036. 10.23937/2469-5777/1510036
Copyright: © 2016 Yanguas J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Pigmented villonodular synovitis is a relatively rare idiopathic proliferative disorder affecting the synovium of joints, bursae and tendon sheaths. Knee and hip are the most affected joints. We report two cases of unusual locations in two young male soccer players (17 and 13 years old): distal tibiofibular joint and pes anserine bursa. Diagnoses were confirmed by magnetic resonance imaging (MRI). In the first case the treatment was conservative, followed-up by MRI and computed tomographic several times during the season once pain disappeared and the player could return to play normally. In the second case, due to the importance of doing an exact differential diagnose with a synovialosarcome, biopsy and subsequent excision was the only considered option. Clinical, radiological and histologic exams are needed for the diagnosis of PVNS and the treatment, particularly in sports (soccer), should be selected according to each particular case.
Keywords
Villonodular pigmented synovitis, Soccer player, Young athlete, Syndesmotic joint, Pes anserine bursa
Introduction
Pigmented villonodular synovitis (PVNS) is a relatively rare, benign, idiopathic proliferative disorder affecting the synovial-lined joints [1,2]. Jaffe and colleagues [3] described it as a “benign inflammatory state of the synovium of unclear aetiology and as a tumor-like aggression of synovial tissue involving joints” and repetitive intra-articular effusion, pain and loss of function may result. Diagnosis is more common between ages 20 and 50 years, with a median age of 30 years [4].The most common location is the knee (up to 80%). Hip, flexor tendon sheaths of the hand, ankle and shoulder joints can be also affected and the sternoclavicular and distal tibiofibular joints are rare locations [5-8]. Two different types of behaviour of PVNS have been described: diffuse PVNS that involves the entire joint synovium and localized PVNS that involves a discrete nodular, lobulated mass [9]. Diffuse PVNS has nearly equal incidence in male and female patients, while the localized form demonstrates a female-to-male predominance ratio of 1.5-2:1 [4]. Magnetic resonance imaging (MRI) is useful to delineate the soft tissue extent and bony involvement. In presence of PVNS, synovial abnormalities can be identified because of their low signal intensity on both T1 and T2-weighted images [1,9,10]. The recurrence rate for the diffuse type may be as high as 50% whereas the rate for the localized type is considered low [11-13]. In addition malignant transformation is considered rare [14] but to avoid tumor spread, complete surgical excision and careful tissue handling are essential [1]. To date, we don’t have found in medical literature differences in terms of incidence between physically active people and their sedentary counterparts.
.
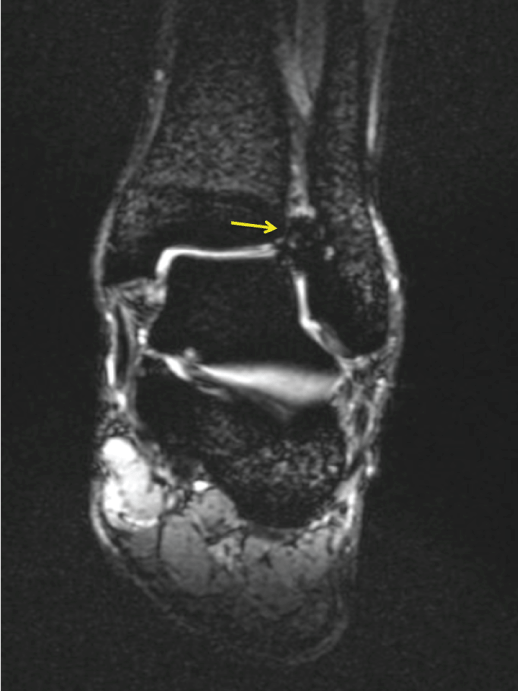
Figure 1: Coronal MRI image showing hemosiderin deposition (arrows) suggesting focal pigmented villonodular synovitis in distal tibiofibular joint.
View Figure 1
.
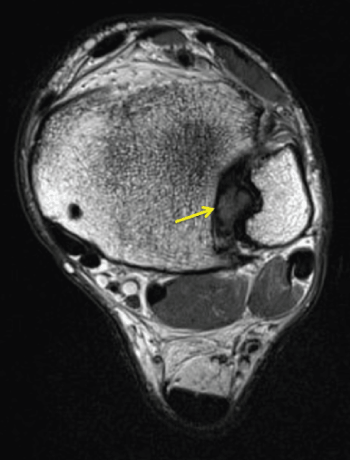
Figure 2: Axial MRI image showing hemosiderin deposition (arrows) suggesting focal pigmented villonodular synovitis in distal tibiofibular joint.
View Figure 2
Case 1
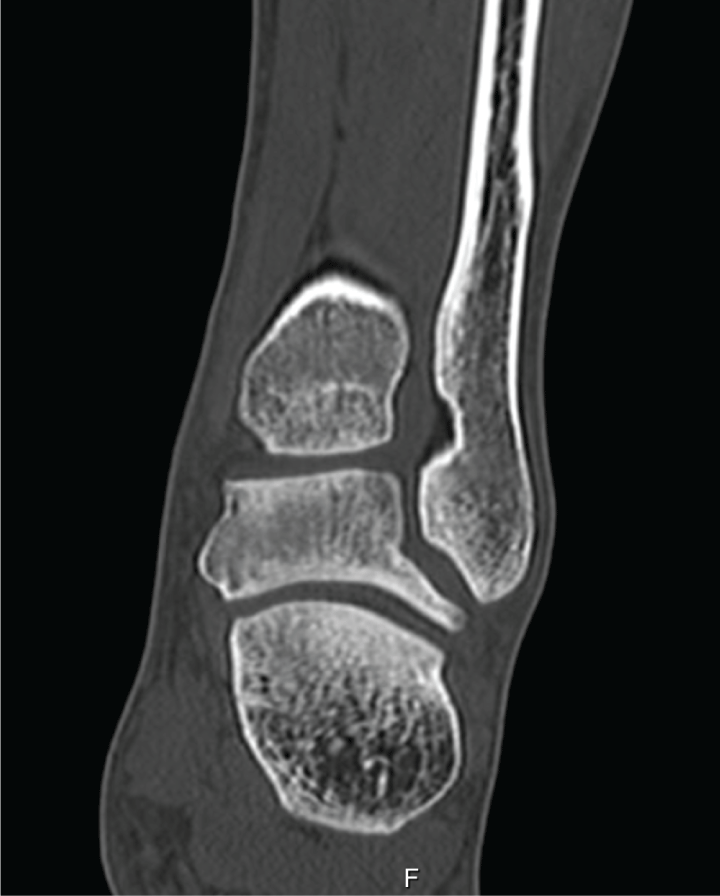
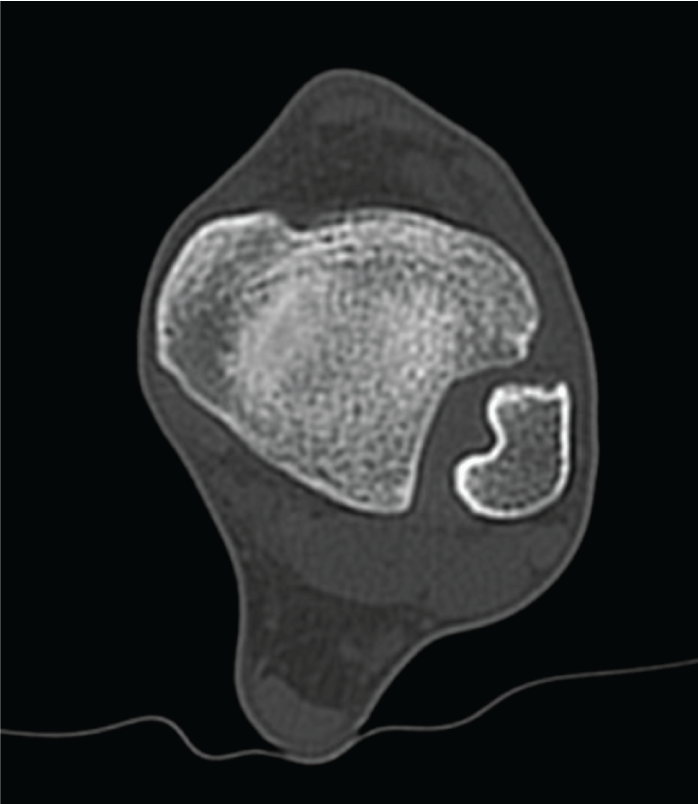
Seventeen year old male soccer player sprains his left ankle during a training session, causing severe pain in anterolateral aspect of the ankle complex and minimal/moderate swelling. Clinical examination demonstrated a normal ankle drawer test and forced varus test. Palpation of the distal tibiofibular joint (DTFJ), squeeze test and compression with combined external rotation of the foot were painful. Because respective injury occurred only one day before a match, MR imaging was performed, which led to the initial diagnosis of an anterior-inferior tibiofibular ligament injury. Figure 1 and Figure 2 demonstrate a round-shaped mass centered in the DTFJ-space, which made the clinicians assume possible presence of PVNS. Due to its proliferative and infiltrative behaviour, additional computed tomographic imaging (CT) was performed (Figure 3 and Figure 4).
.
Figure 3: Coronal CT view showing the proliferative, invasive and compressive behaviour of the pigmented villonodular synovitis in the fibula.
View Figure 3
.
Figure 4: Axial CT view showing the proliferative, invasive and compressive behaviour of the pigmented villonodular synovitis in the fibula.
View Figure 4
Case 2
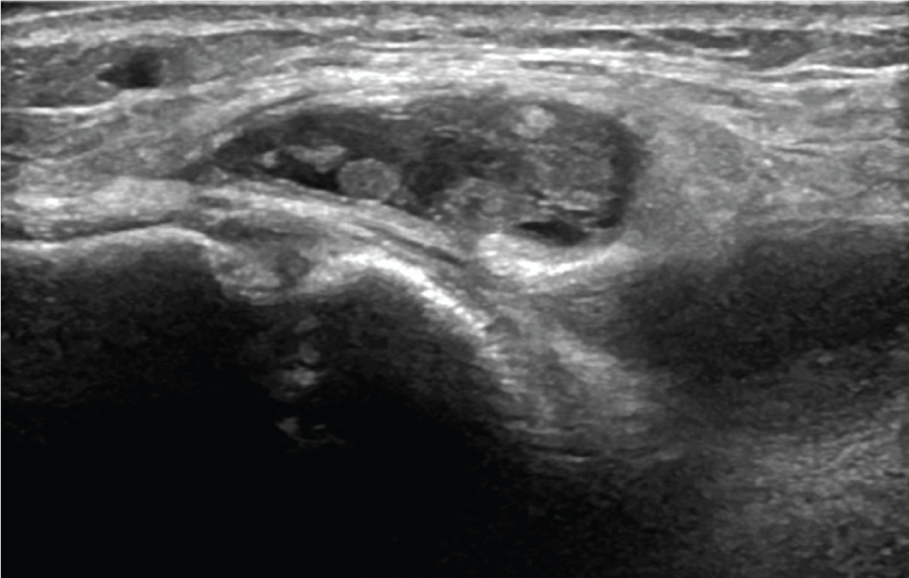
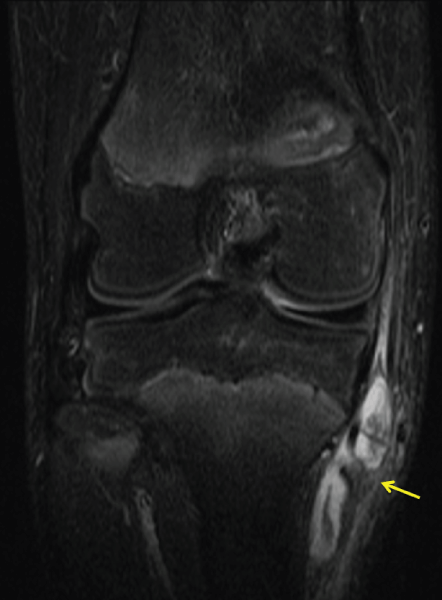
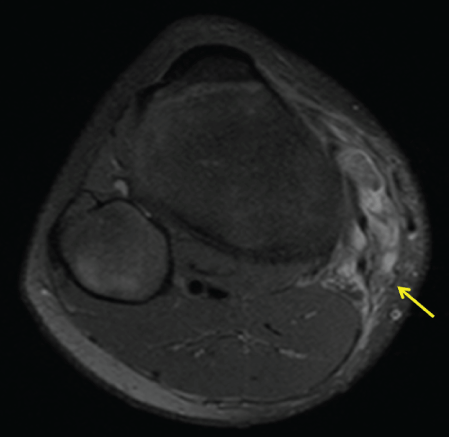
Thirteen year old boy with no medical history consulted our medical department for the spontaneous appearance of a progressively growing though painless mass on the medial aspect of his right knee. Intake excluded any kind of clinical or functional symptomatology or preceding traumatic events. Physical examination revealed a soft, painless, mobile, mass on the medial side of the knee joint. Strength and range of motion were preserved, painless medial joint interline palpation and negative medial meniscus manoeuvres. The ultrasound exam documented a cystic mass, apparently emerging from the bursa anserine (Figure 5). Additionally, 13 cubic centimetres of blood-synovial fluid were obtained when a puncture was performed. MRI demonstrated a bilobed collection that was located between the tendons of the pes anserinus and the tibial plateau (Figure 6 and Figure 7). As a focal extra-articular PVNS was suspected, the patient was referred to a hospital where an open bursectomy and pathological examination were performed. The result of microscopic and macroscopic exams confirmed the diagnosis of PVNS. No postoperative complications were reported and the patient remained asymptomatic.
.
Figure 5: Ultrasound exam of the medial side of the knee shows a cystic image with echoes inside emerging extra-articular from the bursa anserine.
View Figure 5
.
Figure 6: Coronal MRI image showing hemosiderin deposition (arrows) were observed in an extra-articular location, the bursa anserine.
View Figure 6
.
Figure 7: Axial MRI image showing hemosiderin deposition (arrows) were observed in an extra-articular location, the bursa anserine.
View Figure 7
Discussion
Pigmented villonodular synovitis (PVNS) is a benign, idiopathic proliferative disorder with hemosiderin pigmentation and stromal infiltration of histiocytes and giant cells [15] affecting the synovial-lined joints, bursae and tendon sheaths. Although it is considered a benign inflammatory state [1], its tumor-like behaviour is considered to be the main cause of associated joint destruction [10,16]. The incidence is around 1.8 cases per million annually [17]. The pathogenesis remains uncertain and trauma has been proposed as a precipitating event [18]. In our two cases, due to the frequent physical contacts in soccer and respective PVNS locations in this case report, trauma could possibly have been an evoking factor. DTFJ and bursa anserine are unusual locations [5-8], as PVNS rarely affects patients beneath the age limit of 15 [19,20]. A possible hypothesis for explaining these unusual locations in young people could be the sports activity? To date no investigations have connected directly sport and PVNS but the potential irritation during sports activities (contusions, dribblings, side-cutting manoeuvres, shoots...) could influence the development of this entity. It should be to take into account. More investigations are needed to clarify this key. Although MRI is election method to suggest the diagnostic of PVNS in relation to a clinical suspicion, the final and definitive diagnosis is always histopathological.
Case 1
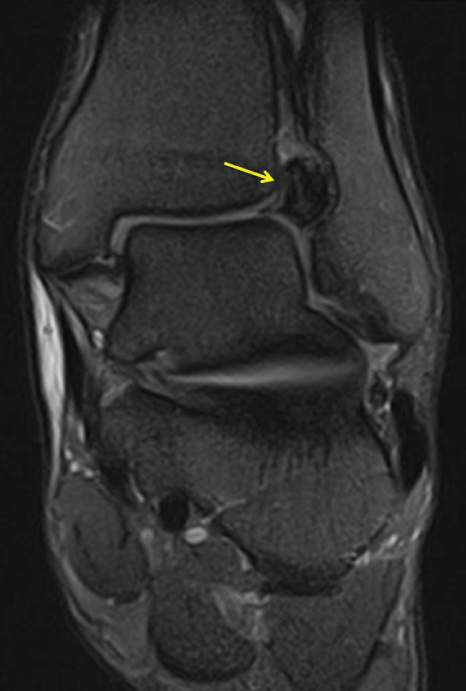
The incidence of PVNS in ankle joint is 2.5% but in DTFJ is relatively rare [1,21]. In this case the injury happened the day before a match. To identify its severity and to decide if this player could be available for the next day, MRI was performed. At first, ankle sprain causing injury to the anterior-inferior syndesmotic ligament was assumed. The subsequent diagnosis of PVNS in this joint was made accidentally because before respective event no pain, no effusion and no swelling in this ankle had been reported. First line treatment (physiotherapy and functional recovery) was conservative and aspired to heal the sprain in a rehabilitation period of 3 weeks, paying no additional attention to the PVNS in the involved joint, as this did not cause any symptoms nor functional deficits for this patient. According to available literature however, the general treatment for PVNS should consist of the surgical excision because recurrences are high (40-50%) [22]. Nonetheless, the recurrence rates of the localized PVNS type seems to be low [11-13]. In this particular case, comprising of a talented young athlete at the early start of a professional soccer career, conservative treatment and observation of the evolution were preferred. During the season, MRI exams were made every 3 months to control the size of this localized, nodular, PVNS. Additionally, because of bony involvement with intra-articular erosion due to overpressure, 2 CT were also performed during follow up (Figure 8, Figure 9, Figure 10 and Figure 11). Both exams were performed to monitor the progression of the lesion to control its aggressive component and take a different decision about the treatment (then surgical, not conservative) in case of overgrowth and if bone damage appears. Existing literature discusses similar cases of PVNS in DTFJ treated surgically (surgical resection of the mass with arthroplasty of the ankle joint) [1,18] with full stabilization of the synovial proliferation but with a lesser functional outcome, comprising the athletic future of the patient. In some cases, recurrences must be prevented with radiation therapies [2], next to surgical intervention. To date, 2 years after surgical resection, no pain, no new injuries and no decrease of functionality have been reported and this patient is able to participate in professional soccer play without any functional restriction.
.
Figure 8: Coronal MRI view of pigmented villonodular synovitis of distal tibiofibular joint made 8 months later: image is identical like the time of the diagnosis.
View Figure 8
.
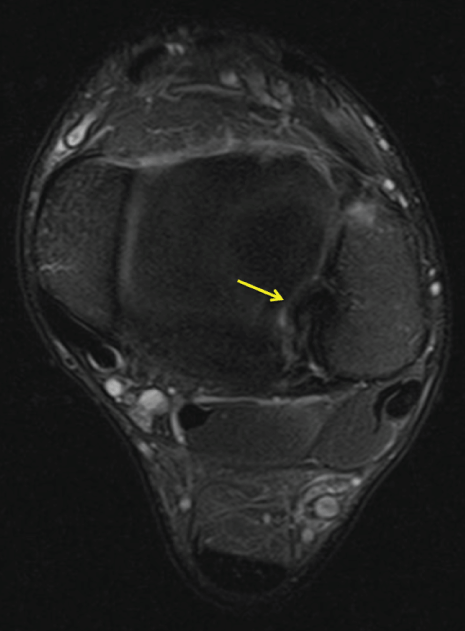
Figure 9: Axial MRI view of pigmented villonodular synovitis of distal tibiofibular joint made 8 months later: image is identical like the time of the diagnosis.
View Figure 9
Case 2
Although there are no epidemiology statistics on the paediatric group, the estimated incidence is thought to be low. The aetiology is uncertain and some authors postulate it to be a chronic inflammatory process while others consider it to be rather neoplastic [19]. The nature and clinical presentation of this condition would be similar as the one seen in adults, with the diffuse form being the predominant type and knee joint being most frequently affected. Its onset is insidious and nonspecific so the diagnosis often is delayed [19]. Involvement of bursa is the least frequent location and only a few cases with involvement of the pes anserine bursa have been described, mostly in adults. In all cases that have been reported to date, average time to diagnosis concerned a period of weeks or months [15]. The subject of our second case report was a child who suffered from a rare localized type of PVNS, with an extra-articular location, originated in the pes anserine bursa. Respective condition was characterized by a sudden onset, and an asymptomatic, rapidly growing soft tissue mass located at the medial aspect of the right knee. Although MRI was helpful in diagnosing and determine the extent of the synovial abnormality [8,19], additional histological assessment was necessary to confirm the diagnosis and rule out pathology of malignant origin (i.e. malignant synovial sarcoma), certainly given the unusual presentation. Unlike for our first case, the preferential treatment for this second patient was surgical (total open bursectomy), given the aggressive potential and the requirement to histologically confirm the diagnosis. An MRI control made 2 months after the surgical intervention showed no evidence of recurrence. The time to return to participate in a training session after resection was 3 months to avoid possible injuries or trauma. There is no consensus guideline about the return to play in cases like these and we choose this time together with the opinion of the orthopaedic surgeon once the scar was healed, the range of motion was complete and the strength after the operation was fully recovered.
.
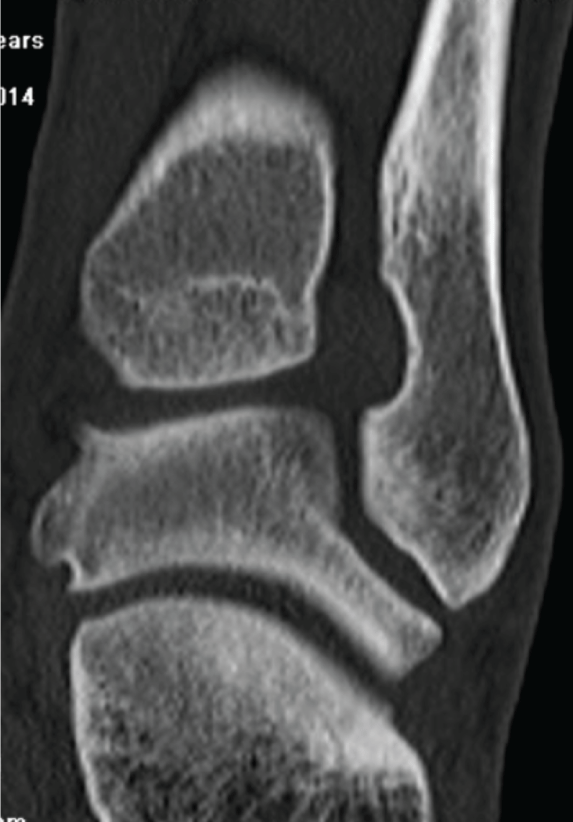
Figure 10: Coronal CT image made 8 months later show the same kind of compression like the time of the diagnosis.
View Figure 10
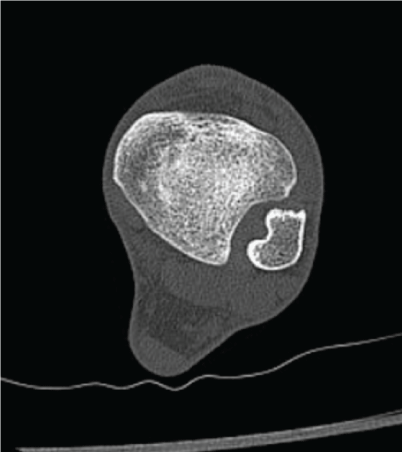
.
Figure 11: Axial CT image made 8 months later show the same kind of compression like the time of the diagnosis.
View Figure 11
Conclusion
Pigmented villonodular synovitis (PVNS) is a relatively rare idiopathic proliferative disorder and knee is the most affected joint (up to 80%) and more common between ages 20 and 50 with a median age of 30. Distal tibiofibular joint and pes anserinus bursa are unusual locations. Diagnoses of both cases were confirmed by magnetic resonance imaging. Generally, in PVNS the treatment must to be surgical due to the high risk of recurrence and to make the differential diagnosis with a malignant origin in some specific cases. However, the preferred treatment in these particular situations (professional soccer), if clinically is possible (no strength deficits, no articular effusion and no pain), could be conservative for not compromising the future professional carrier in young players with an aggressive surgical intervention in joints which could cause severe functional limitations to play at high performance level.
References
-
Mori H, Nabeshima Y, Mitani M, Ozaki A, Hideo F, et al. (2009) Diffuse pigmented villonodular synovitis of the ankle with severe bony destruction: treatment of a case by surgical excision with limited arthrodesis. Am J Orthop 38: E187-E189.
-
Schnirring-Judge M, Lin B (2011) Pigmented villonodular synovitis of the ankle-Radiation therapy as a primary treatment to reduce recurrence: a case report with 8-year follow-up. J Foot Ankle Surg 50:108-116.
-
Jaffe HL, Lichtenstein L, Sutro CJ (1941) Pigmented villonodular synovitis, bursitis and tenosynovitis. Arch Pathol 31: 731-765.
-
McGrath JR, Monu J (2015) Pigmented villonodular synovitis imaging.
-
Miller WE (1982) Villonodular synovitis: pigmented and nonpigmented variations. South Med J 75: 1084-1086, 1092.
-
González Della Valle A, Piccaluga F, Potter HG, Salvati EA, Pusso R (2001) Pigmented villonodular synovitis of the hip: 2- to 23-year followup study. Clin Orthop Relat Res : 187-199.
-
Ryan RS, Louis L, O'Connell JX, Munk PL (2004) Pigmented villonodular synovitis of the proximal tibiofibular joint. Australas Radiol 48: 520-522.
-
Tyler WK, Vidal AF, Williams RJ, Healey JH (2006) Pigmented villonodular synovitis. J Am Acad Orthop Surg 14: 376-385.
-
Villani C, Tucci G, Di Mille M, Di Gennaro S, Corsi A (1996) Extra-articular localized nodular synovitis (giant cell tumor of tendón sheath origin) attached to the subtalar joint. Foot Ankle Int 17: 413-416.
-
Goldman AB, DiCarlo EF (1988) Pigmented villonodular synovitis. Diagnosis and differential diagnosis. Radiol Clin North Am 26: 1327-1347.
-
Granowitz SP, D’Antonio J, Mankin HL (1976) The pathogenesis and long-term end results of pigmented villonofular synovitis. Clin Orthop Relat Res 114: 335-351.
-
Myers BW, Masi AT (1980) Pigmented villonodular synovitis and tenosynovitis: a clinical epidemiologic study of 166 cases and literature review. Medicine (Baltimore) 59: 223-238.
-
Flandry F, Hughston JC (1987) Pigmented villonodular synovitis. J Bone Joint Surg Am 69: 942-949.
-
Bertoni F, Unni KK, Beabout JW, Sim FH (1997) Malignant giant cell tumor of the tendon sheaths and joints (malignant pigmented villonodular synovitis). Am J Surg Pathol 21: 153-163.
-
Zhao H, Maheshwari AV, Kumar D, Malawer MM (2011) Giant cell tumor of the pes anserine bursa (extra-articular pigmented villonodular bursitis): a case report and review of the literature. Case Reports in Medicine.
-
Konrath GA, Shifrin LZ, Nahigian K (1994) Magnetic resonance imaging in the diagnosis of localized pigmented villonodular synovitis of the ankle: a case report. Foot Ankle Int 15: 84-87.
-
Pandey S, Pandey AK (1981) Pigmented villonodular synovitis with bone involvement. Arch Orthop Trauma Surg 98: 217-223.
-
Mavrogenis AF, Papaparaskeva KT, Galanakos S, Papagelopoulos PJ (2011) Pigmented villonodular synovitis of the distal tibiofibular joint: a case report. Clin Podiatr Med Surg 28: 589-597.
-
Masquijo J, Baroni E, Dello Russo B, Bassini O, Miscione H (2008) Sinovitis vellonodular pigmentada de rodilla en pacientes esquelé ticamente inmaduros. Rev Asoc Argent Orthop Traumatol 73: 20-26.
-
Pons Morales S, Salido Capilla C, Vega Martí nez M, Nebot Sanchis I (2010) Pigmented villonodular synovitis in children. An Pediatr (Barc) 73: 146-147.
-
Rao AS, Vigorita VJ (1984) Pigmented villonodular synovitis (giant-cell tumor of the tendon sheath and synovial membrane). A review of eighty-one cases. J Bone Joint Surg Am 66: 76-94.
-
Weiss SW, Goldburn JR (2001) Benign tumors and tumor-like lesions of synovial tissue. In: FM Enzinger and SW Weiss, Soft Tissue Tumors (4th Edition), Mosby, St Louis, Mo, USA,1037-1062.





