Trauma Cases and Reviews
Tillaux and Volkmann Fractures: A Report on Two Cases, Treatment Determined by Syndesmosis Instability
Jike Lu* and Masumi Maruo Holledge
Orthopaedic Department, Beijing United Family Hospital, Beijing, China
*Corresponding author: Jike Lu, MD, PhD, Orthopaedic Department, Beijing United Family Hospital, Beijing, 100016, China, Tel: +86-5927-7000, Fax: +86-5927-7407, E-mail: jike.Lu@ufh.com.cn
Trauma Cases Rev, TCR-2-042, (Volume 2, Issue 3), Case Report; ISSN: 2469-5777
Received: June 30, 2016 | Accepted: September 13, 2016 | Published: September 15, 2016
Citation: Lu J, Holledge MM (2016) Tillaux and Volkmann Fractures: A Report on Two Cases, Treatment Determined by Syndesmosis Instability. Trauma Cases Rev 2:042. 10.23937/2469-5777/1510042
Copyright: © 2016 Lu J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We report two cases of isolated Tillaux fracture and Volkmann fracture without other associated ankle fractures. The case of Tillaux fracture was a 15-year-old female who tripped and fell over during a 400 m hurdle running competition. Preoperative radiographs and CT scans showed Salter-Harris type III, an isolated Tillaux fragment, with more than 2 mm anterior and lateral displacement. Surgical stabilization of Tillaux fragment was performed via anterolateral minimal invasive approach with anatomic reduction of Tillaux fragment and two parallel cannulated screw fixation. The second case was a 21-year-old female who fell off a snowboard with her ankle in an odd position. Preoperative radiographs did not reveal any bony injuries. However, CT scans showed a Volkmann fracture at the posterolateral aspect of posterior malleolus without displacement. Non surgical management was given, after intraoperative imaging intensifier screening to confirm that there was no syndesmotic diastasis. The mechanism of injury and options of management are discussed in this report.
Keywords
Ankle fractures, Syndesmosis, Tillaux, Volkmann, Internal fixation
Introduction
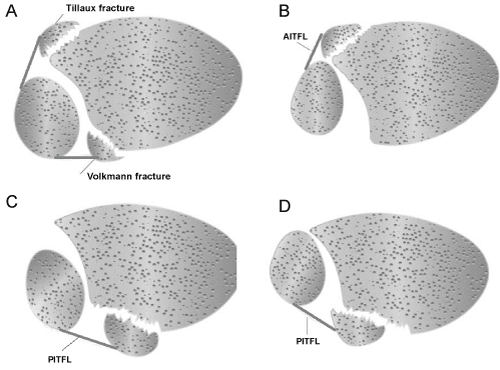
In Lauge-Hansen classification of ankle fractures [1], four major fracture types were described: supination- adduction, supination-external rotation (SER), pronation-abduction, and pronation-external rotation (PER) fractures. External rotation of the foot relative to the leg (SER-Lauge-Hansen) tightens the anterior tibiofibular ligament and may result in an avulsion fracture of the tibial attachment of AITFL (Tillaux or Tillaux-Chaput fracture) [2,3] or at the fibular attachment of the ligament (Wagstaffe-Le Fort fracture) [4]. Internal rotation of the foot relative to the leg (PER-Lauge-Hanson) tightens the posterior inferior tibiofibular ligament (PITFL) and may result in an avulsion fracture at the tibial attachment of PITFL [4], which presents as a Volkmann fragment (Figure 1). We present two cases who had isolated Tillaux or Volkmann fractures that are different from those fractures combined with other ankle bony injuries in literature [5,6] and our treatment methods were determined by syndesmosis instability.
.
Figure 1: Diagrams to illustrate Tillaux and Volkmann fragments. (a) Location of the Tillaux and Volkmann fragments; (b) Anterior and lateral displacement of the Tillaux fragment with fibula shifting anteriorly causing syndesmotic incongruency; (c) Posterior and medial displacement of the Volkmann fragment with the fibula shifting posteriorly causing syndesmotic incongruency; (d) Posterolateral displacement of the Volkmann fragment with the fibula shifting anteriorly causing syndesmotic incongruency.
View Figure 1
Case 1
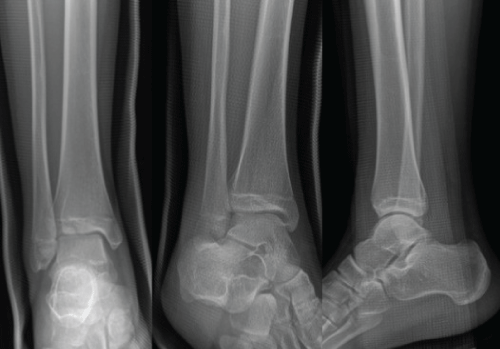
A 15-year-old female was present in our clinic 2 days after sustaining an injury to her right ankle during a 400 meters hurdle competition. On physical examination, mild swelling and localized tenderness at the anterior lateral aspect of her ankle was revealed. Plain radiographs were suspicious for a Tillaux fracture (Figure 2). A CT scan of her ankle revealed an isolated Tillaux fragment that is located at anterolateral aspect of distal tibial articular surface with syndesmosis diastasis (Figure 3).
.
Figure 2: Plain radiographs of anteroposterior (AP), mortise, and lateral views. AP view was showing that anterolateral intra-articular fracture of epiphysis. However, mortise and lateral views did not reveal any abnormalities.
View Figure 2
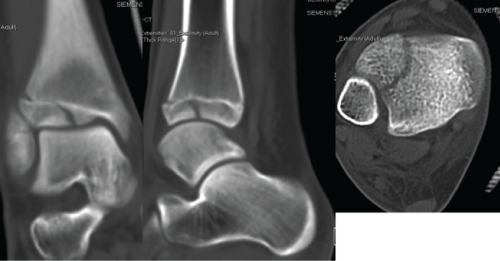
.
Figure 3: CT scans of the injured ankle. Anterolateral Tillaux fragment was displaced laterally on coronal reconstruction image and was displaced anteriorly on sagittal reconstruction image. Axial image showed that anterolateral fragment without posterior extension, but displaced anteriorly and laterally with fibula shifting anteriorly.
View Figure 3
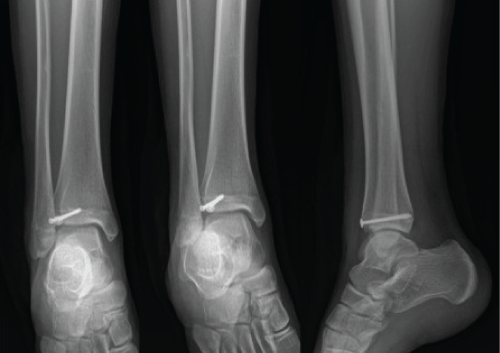
The patient was managed operatively via anterolateral minimal invasive approach, anatomic reduction of Tillaux fragment and stabilized with two parallel cannulated screws (Figure 4). She was in a non-weight bearing boot for 6 weeks, and was allowed to do range of movement of her ankle. When she was last seen 6 weeks postoperatively, she reported no symptoms. Her ankle examination was normal at that time and her radiographs revealed that there was no fracture line was detectable. At the patient's one-year follow-up visit, she had no symptoms and had returned to all activities.
.
Figure 4: Postoperative plain radiographs showed that there were no medial clear space increase on AP and mortise views, and two cannulated screws were well positioned. No anterolateral fracture line was visible.
View Figure 4
Case 2
A 21-year-old female was presented in our emergency department for a painful right ankle. She had injured the ankle a day earlier while snowboarding. Examination of her ankle revealed mild pain on the range of movement, no tenderness over medial and lateral aspect of her ankle. The post injury radiographs were generally normal (Figure 5). However, her CT scan of the ankle revealed a Volkmann fracture (Figure 6).
.
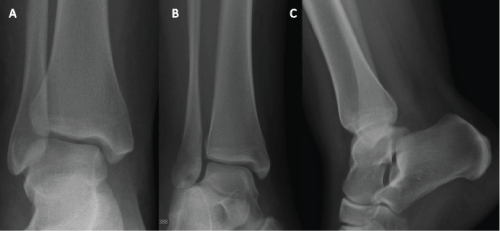
Figure 5: Plain radiographs of the injured ankle. AP and mortise views did not show any bony injuries. (a and b) the medial clear space was less than 4 mm; (c) there was no sagittal plane instability of her ankle on lateral view.
View Figure 5
.
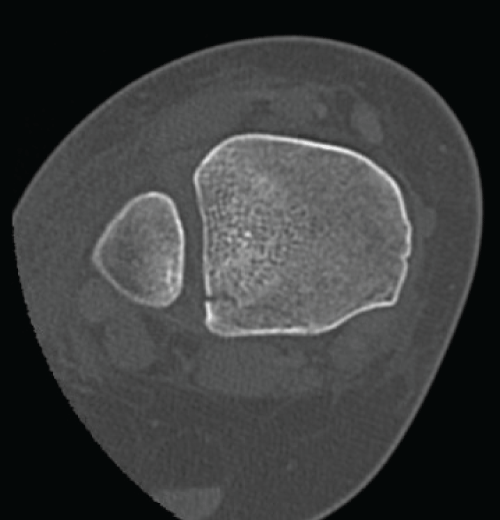
Figure 6: CT scans revealed posterolateral avulsion fracture but no displacement was noticed and no syndesmotic incongruency.
View Figure 6
She was examined under general anesthesia. Screening from an imaging intensifier did not show the medial clear space increase more than 4 mm while external rotation of her foot was enforced (Figure 7). Therefore, we diagnosed her syndesmosis is stable. Subsequently, a shot leg plaster was applied for six weeks. She was reviewed in clinic in one-year post-injury, and was pain-free.
.
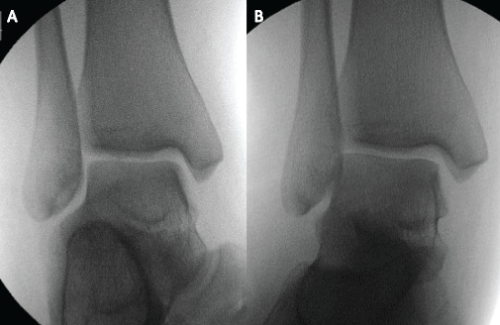
Figure 7: Intra-operative imaging intensifier screening showed that there was no significant medial clear space increase on external stress view (b) compared with non stress AP view (a).
View Figure 7
Discussion
Juvenile Tillaux fracture is anterior-inferior tibiofibular ligament avulsion fracture. The entire distal tibial epiphysis fracture can be Tillaux-Chaput fracture in adult [7]. In the Tillaux fracture, it is avulsion fracture, only anterolateral distal tibial epiphysis is involved (Salter-Harris III).
Posterior malleolus fractures are relatively common within the setting of ankle fractures, the most common of which are trimalleolar fracture with an incidence of approximately 7-14.2%. [5,6]. Isolated fractures of the posterolateral tibial lip (Volkmann's Triangle) are rare, with an estimated incidence of 0.5-1% [6,8,9]. The most common injury mechanism is SER, which accounts for the posterior inferior tibial fibular ligament avulsion fracture (Volkmann fracture) or posterior malleolus fractures, which may cause fibular rotational deformity or fibular shifting either anteriorly or posteriorly leading to syndesmotic instability (Figure 8A and Figure 8B). Injury mechanism of isolated Tillaux fracture is most likely PER, which is responsible for anterior inferior tibial fibular ligament avulsion fracture. The AITFL is intact but hinged on Tillaux fragment causing fibular rotation or shifting anteriorly leading to syndesmotic instability (Figure 3). The fibular rotational deformity or sagittal plane shifting is hardly to be assessed on plain radiographs. However, most of those injuries are missed from plain radiographs (Figure 8B).
.
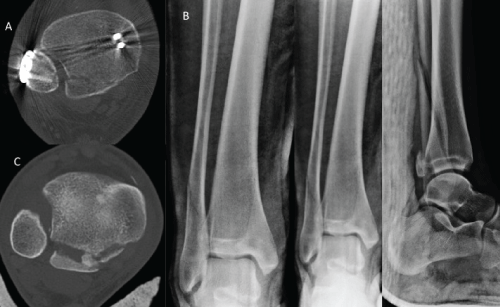
Figure 8: Axial CT scans in patients with Volkmann fractures combined with other ankle fractures. (a) a 59-year-old female, internal fixation of medial and lateral malleoli fractures without fixation of Volkmann fracture was given. Pre- and postoperative plain radiographs did not reveal any syndesmotic instability but postoperative CT scans showed the fibula was shifted anteriorly due to Volkmann fragment which is hinged on PITFL and displaced laterally in posterior part of the syndesmosis causing syndesmotic incongruency and instability; (b) a 17-year-old male, plain radiographs did not reveal any syndesmotic instability; (c) CT scan showed that the Volkmann fragment was displaced posteriorly and medially causing fibular shifting posteriorly and malrotation that was a main cause syndesmotic incongruency.
View Figure 8
Gardmer MJ, et al. [10] did cadaver PER injury with posterior malleolar fragment model and fixation of posterior malleolus that restored 70% syndesmotic stability compared with fixation of syndesmosis that restored 40% stability and notably, for osteoarthritis, 95% of patients had no signs of osteophytes, suggesting a low risk of developing osteoarthritis after fixation of posterior malleoli. Therefore, direct posterior malleolus fixation is suitable to stabilize syndesmotic injury, anatomic reduction and fixation of a Volkmann fracture will restore syndesmotic stability by restoring the length of the intact PITFL and by preventing sagittal shifting or rotation of the fibula causing syndesmotic incongruency.
Tillaux or Volkmann fractures may lead to "syndesmotic diastasis" with talar shifting laterally but may not be recognized on plain radiographs. Several studies have shown that even minimal lateral talar shift may significantly increase weight bearing stresses on the talus leading to early post-traumatic arthritic changes [11,12]. Therefore, avulsion of anterolateral (Tillaux, or Tillaux-Chaput) or posterolateral (Volkmann) aspect of distal tibia may cause chronic persistent syndesmotic instability if missed or untreated. CT scans are critical for assessment those unique, rare patterns of avulsion fractures. Any syndesmotic instability should be treated with internal fixation the fragments rather than syndesmotic fixation. Although syndesmotic injury can be fixed by standard trans-syndesmotic fixation, which has a high rate of syndesmotic malreduction (52%) [5]. Fixation of the Volkmann fragment might be superior to syndesmotic screw fixation [6,13].
Conclusion
The plain radiographs of patients with an avulsion injury of anterolateral tubercle (Tillaux fragment) or posterolateral tubercle (Volkmann fragment) should be carefully examined for evidence of syndesmotic widening. If there is any doubt, CT scans is helpful in differentiating patients with this injury from patients with triplane fractures or posterior malleolar fractures of the ankle. Further manipulation under general anesthesia should be initiated if CT images are in determined. Internal fixation of avulsion fragments would directly restore tension of AITFL or PITFL and position of the fibula in coronal, sagittal and axial planes if there is any evidence of syndesmotic incongruency on preoperative CT scans.
References
-
Lauge-Hansen N (1950) Fractures of the ankle. II. Combined experimental- surgical and experimental roentgenologic investigations. Arch Surg 60: 957-985.
-
Cooperman DR, Spiegel PG, Laros GS (1978) Tibial fractures involving the ankle in children. J Bone Joint Surg Am 60: 1040-1046.
-
Kleiger B, Mankin HJ (1964) Fractures of the lateral portion of the distal tibial epiphysis. J Bone Joint Surg Am 46: 25-32.
-
Geissler WB, Tsao AK, Hughes JL (1996) Fractures and injuries of the ankle. In: CA Rockwood, DP Green, RW Bucholz, JD Heckman, Rockwood and Green's Fractures in Adults Lippincott-Raven, Philadelphia, 2203.
-
Koval KJ, Lurie J, Zhou W, Sparks MB, Cantu RV, et al. (2005) Ankle fractures in the elderly: what you get depends on where you live and who you see. J orthop trauma 19: 635-639.
-
Ogilvie-Harris DJ, Reed SC, Hedman TP (1994) Disruption of the ankle syndesmosis: biomechanical study of the ligamentous restraints. Arthroscopy 10: 558-560.
-
Rosenbaum AJ, Dipreta JA, Uhl RL (2012) Review of distal tibial epiphyseal transitional fractures. Orthopedics 35: 1046-1049.
-
Court-Brown CM, McBirnie J, Wilson G (1998) Adult ankle fractures: an increasing problem? Acta orthopaedica Scandinavica 69: 43-47.
-
Kukkonen J, Heikkila JT, Kyyronen T, Mattila K, Gullichsen E (2006) Posterior malleolar fracture is often associated with spiral tibial diaphyseal fracture: a retrospective study. J trauma 60: 1058-1060.
-
Gardmer MJ, Brodsky A, Briggs SM, Nielson JH, Lorich DG (2006) Fixation of posterior malleolus fractures provides greater syndesmotic stability. Clin Orthop Relat Res 447: 165-171.
-
Leeds HC, Ehrlich MG (1984) Instability of the distal tibiofibular syndesmosis after bimalleolar and trimalleolar ankle fractures. J Bone Joint Surg Am 66: 490-503.
-
Ramsey PL, Hamilton W (1976) Changes in tibiotalar area of contact caused by lateral talar shift. J Bone Joint Surg Am 58: 356-357.
-
Gardner MJ, Demetrakopoulos D, Briggs SM, Helfet DL, Lorich DG (2006) Malreduction of the tibiofibular syndesmosis in ankle fractures. Foot Ankle Int 27: 788-792.





