Clinical Medical
Reviews and Case Reports
Hepatic Arterioportal Fistulae: Two Case Reports and Review of the Literature
Thanh Tran, Marc Burrell and William M. Lee*
Departments of Internal Medicine and Radiology, University of Texas Southwestern Medical Center at Dallas, USA
*Corresponding author: William M. Lee, University of Texas, Southwestern Medical Center at Dallas, 5959 Harry Hines Boulevard, HP4.420E, Dallas, TX 75390-8887, USA, Tel: 214-645-6111, E-mail: William.Lee@UTSouthwestern.edu
Clin Med Rev Case Rep, CMRCR-2-048, (Volume 2, Issue 8), Case Report; ISSN: 2378-3656
Received: March 07, 2015 | Accepted: August 17, 2015 | Published: August 20, 2015
Citation:Tran T, Burrell M, Lee WM (2015) Hepatic Arterioportal Fistulae: Two Case Reports and Review of the Literature. Clin Med Rev Case Rep 2:048. 10.23937/2378-3656/1410048
Copyright: © 2015 Lee WM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Hepatic arterio portal fistulae are inappropriate connections between the hepatic artery and portal vein and are obscure causes of acquired portal hypertension. There have been a small number of cases reported since it was first described in 1892 by Sachs [1-7]. These fistulae can cause significant morbidity and mortality as a result of the portal hypertension, but unlike cirrhosis, are potentially curable. Therefore, early diagnosis and treatment is important. The two cases presented here illustrate the vastly different severity and clinical outcomes that may be observed.
Case 1
A 47-year-old male with no significant past medical history presented to an outside hospital for new onset as cites. After several days, he was referred to our facility for further care. On admission, his vital signs were stable. Physical exam showed altered mental status and a mildly distended abdomen but no abdominal bruit or thrill. Initial laboratory data showed: platelets 124K/uL, sodium 125mmol/L, serum creatinine 4.74mg/dL, with a fractional excretion of urinary sodium of 0.29%; AST 54U/, ALT 97U/L; alkaline phosphatase 175U/L; total bilirubin 2.1mg/dL; albumin level 3.5mg/dL; INR 1.2; serum ammonia 266; Serum Ascites Albumin Gradient (SAAG) 2.92. He was hepatitis B core antibody (total) positive but negative for hepatitis B surface antigen, hepatitis B surface antibody, and for markers of hepatitis A and C.
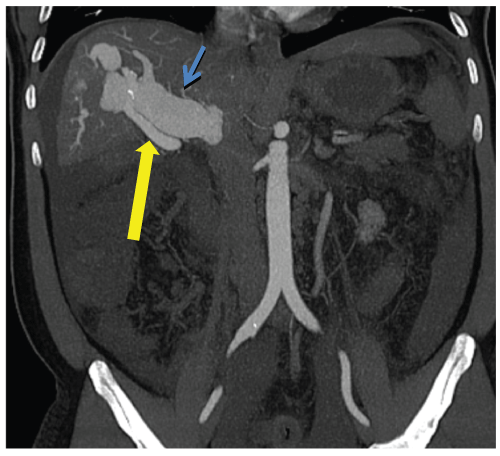
His acute renal failure was thought to be secondary to dehydration and contrast nephropathy from a Computed Tomography with Angiography (CTA) performed at the outside facility, where the overall initial impression was decompensated cirrhosis of unknown etiology. However, when the liver biopsy showed no evidence of fibrosis or inflammation, further review of the prior CTA showed a large shunt between the right hepatic artery and right portal vein with gross dilation of the main portal vein to nearly 4cm (Figure 1). The diagnosis was revised to portal hypertension from a large arterio portal fistula of unknown etiology.
.
Figure 1: Arterial Phase Coronal CT shows a fistula between the right hepatic artery and right portal vein with resulting severe dilation of the main portal vein. Yellow Arrow: Right Hepatic Artery. Blue Arrow: Right Portal Vein
View Figure 1
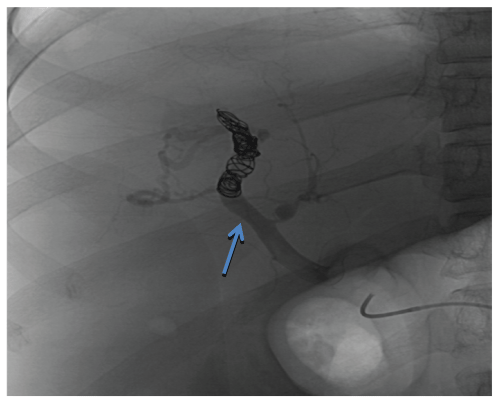
On the third hospital day, he developed hematemesis. Endoscopy revealed small, non-bleeding esophageal varices and a bleeding gastric varix. The arterio portal fistula was embolized by placing multiple coils within the distal right hepatic artery via an aortic approach. Flow through the fistula was greatly reduced but it could not be completely obliterated and remained patent because of its large size (Figure 2). A right hepatic lobe resection to remove the fistula was planned but the procedure was cancelled after the patient's clinical status deteriorated further and he was transferred to the intensive care unit for possible sepsis. His hospital course was complicated by recurrent variceal bleeding, multiple respiratory infections, sepsis and intractable as cites and he expired after a protracted 3-month course. The original cause of the fistula remains unknown as he had never experienced abdominal trauma, malignancy or prior liver biopsy.
.
Figure 2: Post-coil embolization angiogram of the arterio-portal fistula. Flow through the fistula was greatly reduced but the fistula remained patent. Blue Arrow: Fistula between the right hepatic artery and right portal vein.
View Figure 2
Case 2
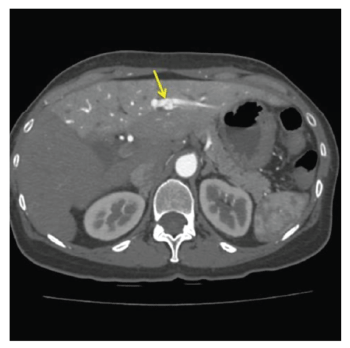
A 68-year-old female with a history of hepatitis C infection and no cirrhosis was seen in our hepatology clinic for follow-up of the treatment of her hepatitis C. A bruit was incidentally noted in the epigastrium. A Doppler right upper quadrant ultrasound showed hepato fugal flow within the main portal vein with the left portal vein demonstrating arterialization. CT angiography of the abdomen showed enhancement in the arterial phase of the left portal vein, confirming the presence of an arterio portal fistula from the left hepatic artery into the left portal vein (Figures 3,4). Of note, the patient had undergone liver biopsy elsewhere in 2002, complicated by bleeding that required her to stay overnight. Of interest, that biopsy report noted the presence of "large caliber arteries" in the histological section. The most likely cause of her fistula was the prior liver biopsy.
.
Figure 3: Arterial Phase Axial CT shows abnormal enhancement of the left portal vein, an 8mm pseudo-aneurysm arising from a branch of the left hepatic artery (yellow arrow), and global Transient Hepatic Attenuation Differences (THAD) of the left lobe of the liver.
View Figure 3
.
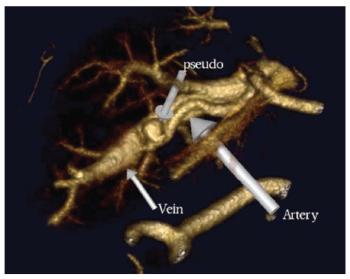
Figure 4: 3D volume rendering image showing the fistula between the left hepatic artery, left portal vein and the pseudo-aneurysm.
View Figure 4
After the incidental finding of the arterio portal fistula, there was concern about portal hypertension given the hepato fugal flow. However, an upper gastrointestinal endoscopy showed no evidence of varices. She also had no other indication of portal hypertension on lab work and imaging including normal platelets, liver function tests, and normal spleen on CT. Since the patient was asymptomatic and had no evidence of portal hypertension, no treatment of the fistula was pursued. The decision was to continue close monitoring. Over two and one half years, there was no change in the fistula diameter and she remained well; however, she elected to have the fistula closed because of continued concern for future enlargement (Figure 3,4).
Discussion
Arterio portal fistulae are usually discovered as an incidental finding during the work-up of liver disease such as in case 2, and can be congenital or acquired. Most cases in adults are acquired, the most common cause being either blunt or penetrating trauma [5]. In particular, a number of cases reported in the literature have followed percutaneous liver biopsies [5,6,8]. In a prospective study, Okuda et al showed that 5.4% of 93 patients had evidence of an arterio portal fistula on hepatic angiography 3 days to 4 weeks after a percutaneous liver biopsy [6]. Many of the fistulae that are acquired through trauma spontaneously close with time, especially if they are small [3,5,9]. In addition to trauma, arterio portal fistulae can also develop from the rupture of a hepatic artery aneurysm into a portal vein or from a focal liver lesion such as a tumor [10].
Up to 25% of patients are asymptomatic [5]. Others may only present with mild to moderate abdominal pain and diarrhea secondary to congestive vascular enteropathy [11]. Though small fistulae are usually clinically inconsequential and may even spontaneously close with time, some persist and cause devastating pathologic changes in hepato portal hemodynamics such as in case 1. Large arterio portal fistulae can lead to hepato fugal flow when the capacity of the draining portal vein is exceeded by the hepatic artery inflow. Persistent high flow within the portal system may lead to significant portal hypertension, with variceal bleeding, ascites, liver failure, hemobilia, or even cardiac failure [5,11]. As a result, early diagnosis is important. As case 2 demonstrates, an epigastric bruit is an important initial clue; imaging by ultrasound Doppler, CT and hepatic arteriography is more definitive.
Once a diagnosis is made, a decision about treatment to prevent or reverse the portal hypertension must be made. Unlike cirrhosis, portal hypertension from arterio portal fistulae is potentially curable. The decision about management is based upon multiple factors, including: size, location, symptoms, patient performance status, and past and concurrent hepatic disease. Small fistulae in an asymptomatic patient can close spontaneously and may be observed, such as in case 2 [11]. However, larger fistulae associated with significant symptoms or complications, as in case 1, require urgent intervention [11]. The first line of therapy currently is angiographic embolization. Closure by embolization with Gelfoam, steel coils, detachable balloons, or bucry late can be achieved in 92% to 100% with a recurrence rate of less than 20% [11-13]. Much of the case reports and literature on arterio portal fistulae in the first half of the twentieth century chose surgical intervention, but this is now reserved for those too large for safe embolization [11]. Surgical procedures range from simple ligation of the feeding arterial branches to resection of the liver parenchyma containing the arterioportal fistula [11]. Transjugular intra-hepatic port systemic shunting has not to our knowledge been performed in this setting. With hindsight, the fistula in the first case may have been too large for simple embolization; he might have benefited from early surgical intervention. However, the patient's functional and clinical status precluded a major surgical procedure without benefit of transplantation should the initial surgical intervention have proven unsuccessful.
Summary
Our two case examples demonstrate different diagnostic and management aspects of arterio portal fistulae. The first case reveals the potentially devastating complications of an arterio portal fistula and the need for accurate diagnosis and swift treatment. The second case, on the other hand, shows the diagnostic and management approach to an uncomplicated and asymptomatic fistula in an outpatient setting.
References
-
Foster JH, Sandblom P (1961) Portal hypertension secondary to an hepato-portal arteriovenous fistula. Ann Surg 154:300-304.
-
Cleveland RJ, Jackson BM, Newman PH, Nelson RJ (1970) Traumatic intrahepatic hepatic artery-portal vein fistula with associated hemobilia. Ann Surg 171:451-454.
-
Foley WJ, Turcotte JG, Hoskins PA, Brant RL, Ause RG (1971) Intrahepatic Arteriovenous Fistulas between the Hepatic Artery and Portal Vein. Ann Surg 174:849-855.
-
Fulton RL, Wolfel DA (1970) Hepatic artery-portal vein arteriovenous fistula. Report of a case with notes on the pathophysiology of this condition. Arch Surg 100:307-309.
-
Gabriel S, Maroney TP, Ringe BH (2007) Hepatic artery-portal vein fistula formation after percutaneous liver biopsy in a living liver donor. Transplant Proc 39:1707-1709.
-
Okuda K, Musha H, Nakajima Y, Takayasu K, Suzuki Y, et al. (1978) Frequency of intrahepatic arteriovenous fistula as a sequela to percutaneous needle puncture of the liver. Gastroenterology 74:1204-1207.
-
Ryan KG, Lorber SH (1968) Traumatic fistula between hepatic artery and portal vein. Report of a case. N Engl J Med 279:1215-1216.
-
Debray C, Leymarios J, Martin E, Hernandez C, Carayon J, et al. (1968) Hepato-portal arteriovenous fistula following needle-biopsy of the liver. Arteriographic detection. Presse Med 76:737-740.
-
Hellekant C (1976) Vascular complications following needle puncture of the liver. Clinical angiography. Acta Radiol Diagn (Stockh) 17:209-222.
-
Wachsberg RH, Bahramipour P, Sofocleous CT, Barone A (2002) Hepatofugal flow in the portal venous system: pathophysiology, imaging findings, and diagnostic pitfalls. Radiographics 22:123-140.
-
Oishi AJ, Nagorney DM, Cherry KJ (1993) Portal hypertension, variceal bleeding, and high output cardiac failure secondary to an intrahepatic arterioportal fistula. HPB Surg 7:53-59.
-
Kaude J, Dudgeon DL, Talbert JL (1969) The role of selective angiography in the diagnosis and treatment of hepatoportal arteriovenous fistula. 92:1271-1272 passim.
-
Tarazov PG, Prozorovskij KV (1991) Intrahepatic spontaneous arterioportal fistula: duplex ultrasound diagnosis and angiographic treatment. Am J Gastroenterol 86:775-778.





