Clinical Medical
Reviews and Case Reports
Untreated Chiari 1 Malformation in Adulthood with Massive Hydrosyringomyelia and Hydrocephalus
Carlo Nicola De Cecco1, Davide Bellini1*, Elisa Porretta2, Francesca Cortese2, Andrea Laghi2 and Gianluca Coppola3
1Department of Radiological, Oncological and Pathological Sciences, Italy
2Department of Medical-Surgical Sciences and Biotechnologies University of Rome, Italy
3Department of Neurophysiology of Vision and Neurophthalmology, Bietti Foundation IRCCS, Rome, Italy
*Corresponding author:
Davide Bellini, Department of Radiological, Oncological and Pathological Sciences, University of Rome "Sapienza" - Polo Pontino, Via Franco Faggiana, 34-04100 Latina, Italy, Tel: +39-3934335132, Fax: +39-6-44238611, E-mail: bellinidavide29@gmail.com
Clin Med Rev Case Rep, CMRCR-2-060, (Volume 2, Issue 10), Case Report; ISSN: 2378-3656
Received: July 28, 2015 | Accepted: September 29, 2015 | Published: October 01, 2015
Citation: Cecco CND, Bellini D, Porretta E, Cortese F, Laghi A, et al. (2015) Untreated Chiari 1 Malformation in Adulthood with Massive Hydrosyringomyelia and Hydrocephalus. Clin Med Rev Case Rep 2:060. 10.23937/2378-3656/1410060
Copyright: © 2015 Cecco CND, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We describe a case of untreated Chiari I malformation in adulthood. It is characterized by displacement of the cerebellar tonsils caudally through the foramen magnum, associated with massive hydrosyringomyelia and tetraventricular hydrocephalum. Magnetic Resonance (MR) imaging provides excellent visualization of intracranial and intraspinal malformations, and thus contributes greatly to their correct diagnosis and treatment.
Keywords
Chiari 1 malformation, Tetraventricular hydrocephalum, Hydrosyringomyelia, Adulthood, Magnetic resonance, Diagnosis
Introduction
Chiari I malformation is the most common variant of the Chiari malformations. It is a dynamic disease characterized by displacement of the cerebellar tonsils caudally through the foramen magnum, interfering with the physiological flow of cerebrospinal fluid [1]. Although is still considered a rare condition, has been recently reported a prevalence rates of 0.1-0.5% with a slight female predominance [2].
Often, it remains asymptomatic until adulthood. The likelihood of becoming symptomatic is proportional to the degree of downward descent of the tonsils.
The most common symptoms include headache and neck pain often exacerbated by cough and Valsalva maneuver. Hydrocephalus and Syringomyelia occurs less frequently and are usually associated with asymmetrical central cord symptoms such as hand weakness and dissociated sensory loss [3].
Magnetic Resonance (MR) is considered the imaging modality of choice [4]. The diagnosis is made by measuring how far the tonsils protrude below the margins of the foramen magnum; a displacement of tonsils > 6 mm from the inner margin of foramen magnum is considered diagnostic for Chiari I malformation [5]. MR imaging provides also excellent visualization of intracranial and intraspinal complications, addressing the proper diagnosis and treatment planning.
Treatment of Chiari malformation depends on the severity and associated symptoms. Regular monitoring, medications and surgery are treatment options. Surgery is usually reserved only for patients with syrinx and symptoms [6]. It consists of decompressing the posterior fossa, by removing part of the occipital bone, and posterior arch of C1.
Despite is not a common condition, it is mandatory to make a prompt and correct diagnosis as soon as possible. Unrecognised Chiari I malformation can leads to severe symptoms and massive complications, as reported in our case. We describe a unique case of untreated Chiari 1 malformation in adulthood associated with massive hydrosyringomyelia and tetraventricular hydrocephalus.
Case Report
A 35-year-old girl was admitted to our hospital because of progressively increasing problems with walking for five years. She had a severe scoliosis, she occasionally complained achy joints and she was showing apathetic behaviour. Neurological examination revealed normal mental functions, Bernard Horner syndrome to the right (Figure 1), spastic gait, positive Romberg, diminished motor strength in her legs and right arm with muscle atrophy in the same hand (4 out of 5) (Figure 2, claw hand). Pain and temperature sensation was impaired in both arms, in her face; chest and abdomen and vibration sense was lost in lower extremities while other sensations were preserved. There were brisk reflexes but in her right arm where they were only slightly diminished (1+), clonus in her left ankle, left positive Hoffmann sign and bilateral Babinski's reflex. She complained nocturnal incontinence. Cerebellar tests including finger to nose, heel to shin test and rapid alternating movements were normal.
.
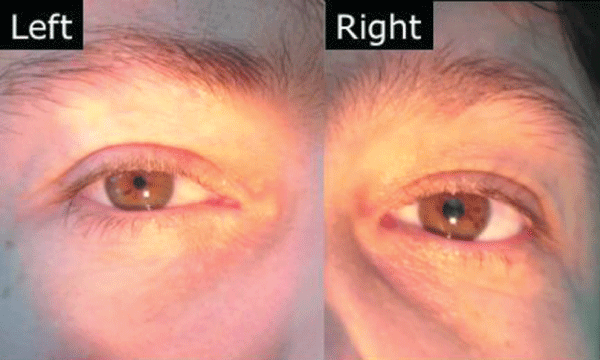
Figure 1: It's clearly visible a Bernard Horner syndrome on the right eye, characterized by constriction of the pupil (miosis) and mild dropping of the eyelid (ptosis).
View Figure 1
.
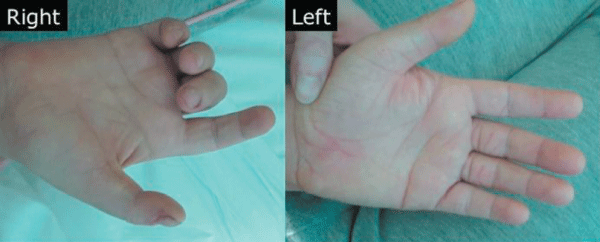
Figure 2: In this figure, on the right, is reported a claw hand, a deformity manifested by flattening of the transverse metacarpal arch and longitudinal arches, with hyperextension of metacarpophalangeal joints and flexion of the proximal a distal interphalangeal joints.
View Figure 2
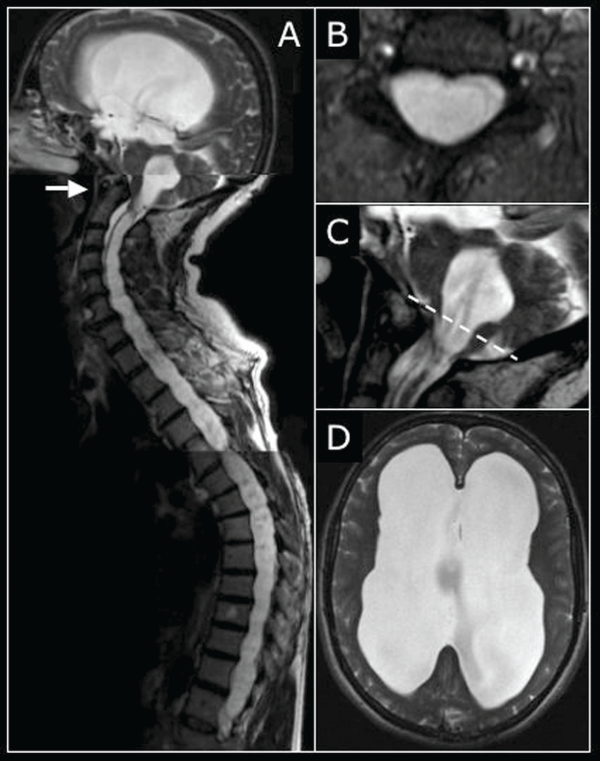
A spinal and cerebral MR examination was performed showing an extensive cylindrical hydro syringomyelia extending from C1 to L5 (Figure 3, Panel A). Complete medullary atrophy was observed with only residual fascicula identified (Panel B). No spinal dysraphisms were present. Downward displacement of the cerebellar tonsil at C2 level was noticed (Panel C) with associated horizontally oriented short clivus and posterior angulation of the odontoid process (Panel A, arrow), causing brain steam compression with flow void in the ependymal canal due to increase liquoral velocity. A severe tetra ventricular hydrocephalus with marked atrophy of the cerebral parenchyma was also present (Panel D). Patient was referred to surgical decompression.
.
Figure 3: In this figure is reported a spinal and cerebral MR examination, showing key findings of Chiari 1 Malformation with Massive Hydrosyringomyelia and Hydrocephalus.
View Figure 3
Discussion
Our case perfectly illustrates the pathophysiological evolution and features of untreated Chiari 1 malformation. The underestimation of early symptoms and the lack of a proper imaging evaluation as first step, can lead to massive life-threatening complications. Longstanding brain steam compression causes an increased cerebrospinal fluid (CSF) pressure with syrinx and hydrocephalus formation. Patients with Chiari 1 develop these anomalies respectively in 30-70% and 10% of cases [1,7,8]. Other foramen magnum or spinal pathologies that impede CSF flow can determine syrinx formation, including post-infectious arachnoiditis, spinal cord/column injury, cervical stenosis and basilar impression [9].
In the setting of Chiari malformation, cervical tether release or foramen magnum decompression represent effective interventions targeting the syrinx mechanism. The reestablishment of normal CSF flow has been demonstrated to allow syrinx resolution or stabilization; otherwise symptoms can progress to severe pain or disabling neurologic impairment [10], as reported in our case. MR represents the reference imaging technique in Chiari assessment and preoperative planning, evaluating the volume of the posterior fossa, CSF flow dynamics, medullary anomalies and spinal dysraphism. Computed Tomography can add useful information in case of complex bone anomalies. In conclusion, we reported a rare case of untreated Chiari I malformation in which the underestimation of early symptoms leaded to massive hydrosyringomyelia, hydrocephalus and to the development of serious neurological impairment.
References
-
Massimi L, Caldarelli M, Frassanito P, Di Rocco C (2011) Natural history of Chiari type I malformation in children. Neurol Sci 32: 275-277.
-
Speer MC, Enterline DS, Mehltretter L, Hammock P, Joseph J, et al. (2003) Review Article: Chiari Type I Malformation with or Without Syringomyelia: Prevalence and Genetics. J Genet Couns 12: 297-311.
-
Schijman E (2004) History, anatomic forms, and pathogenesis of Chiari I malformations. Childs Nerv Syst 20: 323-328.
-
McVige JW, Leonardo J (2014) Imaging of Chiari type I malformation and syringohydromyelia. Neurol Clin 32: 95-126.
-
Buoni S, Zannolli R, di Bartolo RM, Donati PA, Mussa F, et al. (2006) Surgery removes EEG abnormalities in patients with Chiari type I malformation and poor CSF flow. Clin Neurophysiol 117: 959-963.
-
Alden TD, Ojemann JG, Park TS (2001) Surgical treatment of Chiari I malformation: indications and approaches. Neurosurg Focus 11: E2.
-
Koyanagi I, Houkin K (2010) Pathogenesis of syringomyelia associated with Chiari type 1 malformation: review of evidences and proposal of a new hypothesis. Neurosurg Rev 33: 271-284.
-
Mottolese C, Szathmari A, Simon E, Rousselle C, Ricci-Franchi AC, et al. (2011) Treatment of Chiari type I malformation in children: the experience of Lyon. Neurol Sci 32: 325-330.
-
Milhorat TH, Capocelli AL Jr, Anzil AP, Kotzen RM, Milhorat RH (1995) Pathological basis of spinal cord cavitation in syringomyelia: analysis of 105 autopsy cases. J Neurosurg 82: 802-812.
-
Imperato A, Seneca V, Cioffi V, Colella G, Gangemi M (2011) Treatment of Chiari malformation: who, when and how. Neurol Sci 3: 335-339.





