Clinical Medical
Reviews and Case Reports
Ultra-High Resolution Optical Coherence Tomography Imaging of Unilateral Drusen in a 31 Year Old Woman
Talisa E de Carlo1,2, Mehreen Adhi1,2, Chen D Lu2, Jay S Duker1, James G Fujimoto2 and Nadia K Waheed1*
1New England Eye Center and Tufts Medical Center, Tufts University, Boston, MA, USA
2Department of Electrical Engineering and Computer Science, and Research Laboratory of Electronics, Massachusetts Institute of Technology, Cambridge, USA
*Corresponding author:
Nadia K Waheed, New England Eye Center and Tufts Medical Center, Tufts University, Boston, USA, Fax: 617-636-4866, Tel: 617-636-7950, E-mail: nwaheed@tuftsmedicalcenter.org
Clin Med Rev Case Rep, CMRCR-2-063, (Volume 2, Issue 10), Case Report; ISSN: 2378-3656
Received: August 11, 2015 | Accepted: October 07, 2015 | Published: October 10, 2015
Citation: de Carlo TE, Adhi M, Lu CD, Duker JS, Fujimoto JG, et al. (2015) Ultra-High Resolution Optical Coherence Tomography Imaging of Unilateral Drusen in a 31 Year Old Woman. Clin Med Rev Case Rep 2:063. 10.23937/2378-3656/1410063
Copyright: © 2015 de Carlo TE, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We report a case of widespread unilateral drusen in a healthy 31 year old Caucasian woman using multi-modal imaging including ultra-high resolution optical coherence tomography (UHR-OCT). Dilated fundus exam showed multiple drusen-like lesions in the posterior pole without heme or fluid. Fundus auto fluorescence demonstrated hyperautofluorescent at the deposits. Fluorescein angiography revealed mild hyperfluorescence and staining of the lesions. Spectral-domain optical coherence tomography (SD-OCT) OS showed accumulations in the temporal macula at Bruch's membrane. UHR-OCT provided improved axial resolution compared to the standard 5 μm on the commercial SD-OCT and confirmed the presence of deposits in Bruch's membrane, consistent with drusen. The retinal layers were draped over the excrescences but did not show any disruption.
Keywords
Drusen, Optical Coherence Tomography, Retinal Imaging, Retina
Introduction
Drusen was first described by Dr. Franciscus Donders in 1855 via histopathological observations as round accumulations under the retinal pigment epithelium (RPE) in Bruch's membrane [1]. They begin as small (< 63 μm) well-circumscribed accumulations (hard drusen) but over time may coalesce into larger, less-defined elevations (soft drusen). While a few drusen may occur in normal eyes, they are infrequently seen in patients under age 55 especially in large numbers [2]. In the Beaver Dam Offspring Study, soft drusen were seen in only 2% of patients age 21-34 [3]. When drusen occur in young adults, they are typically bilateral. A study of 488 Caucasians age 18-54 determined that only 2% of subjects had unilateral drusen and none of these eyes had more than 20 drusen [4].
We report a case of widespread unilateral drusen in a healthy 31 year old Caucasian woman.
Case Report
A 31 year old Caucasian woman with a history of prematurity was referred to New England Eye Center for drusen-like deposits in the left eye (OS). She denied smoking, renal disease, or a family history of retinal disorders.
The patient's uncorrected visual acuity was 20/20 in the right eye (OD) and 20/20-1 OS. Dilated fundus exam showed a normal fundus OD and multiple drusen-like lesions in the posterior pole without heme or fluid OS. Fundus Autofluorescence (FAF) OS demonstrated hyperautofluorescence at the deposits. Fluorescein Angiography (FA) OS revealed mild hyperfluorescence and staining of the lesions (Figure 1). Spectral-domain optical coherence tomography (SD-OCT) OS showed accumulations in the temporal macula at Bruch's membrane.
A prototype ultra-high resolution SD-OCT (UHR-OCT) system was employed to provide improved axial resolution of 2-3 μm compared to the standard 5 μm on the commercial SD-OCT [5,6]. The higher resolution provided by the UHR-OCT confirmed the presence of deposits in Bruch's membrane OS, consistent with drusen. The retinal layers were draped over the excrescences but did not show any disruption (Figure 1).
.
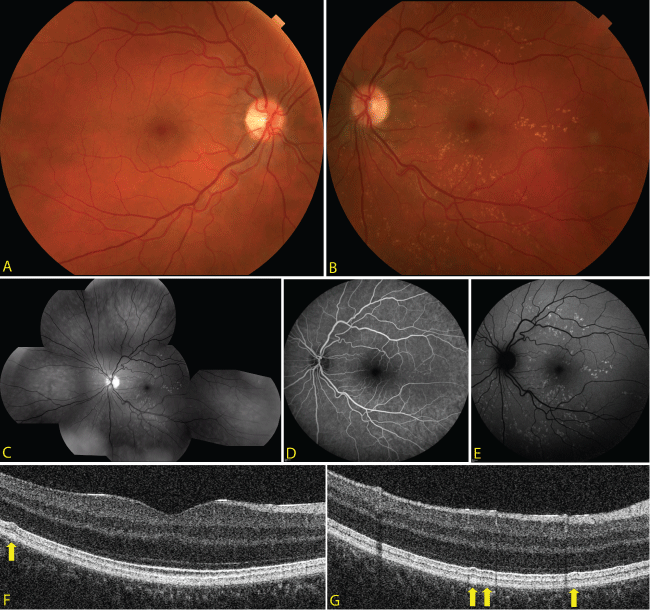
Figure 1: (a) Color fundus photo OD showing no drusen-like deposits in the posterior pole.
(b) Color fundus photo OS depicting multiple scattered small drusen-like deposits in the posterior pole without heme or fluid OS.
(c) Red-free fundus photo composition OS demonstrating multiple scattered drusen-like deposits centrally.
(d) Fluorescein angiography OS revealing mild hyperfluorescence and staining of the deposits but no dark choroid. (e) Fundus autofluorescence OS demonstrating hyperautofluorescence in the areas of the deposits.
(f and g) Ultra-high resolution optical coherence tomography b-scans examples of the drusen-like deposits, which are sub-RPE (arrows).
View Figure 1
Discussion
This report describes a case of unilateral drusen in a healthy 31 year old non-smoking Caucasian woman with no family history of retinal pathology. It is unusual to have extensive macular and extra macular unilateral drusen in young patients. To our knowledge this is the only reported case of widespread unilateral drusen in a patient in her 30s.
The patient had no family history of retinal diseases to suggest an inherited disorder, and lacked the characteristic radial pattern of malattia leventinese [7]. Although she was born premature, her normal vasculature and unilateral nature were inconsistent with retinopathy of prematurity [8]. The deposits were unlikely polar bear tracks as those lesions are typically peripheral, at the IS/OS junction, and hypoautofluroescent [9]. The patient's exam was most indicative of drusen despite the fact that she lacked any major risk factors for drusen: smoking, elevated HDL, male gender and advanced age [3]. The present case is therefore intriguing in its uniqueness because a young patient without a history of known major risk factors for drusen presented with florid unilateral drusen.
Acknowledgements
This work was supported by the National Institute of Health (NIH R01-EY011289-29, R44-EY022864-02, R01-CA075289-17), Air Force Office of Scientific Research (AFOSR FA9550-10-1-0551 and FA9550-12-1-0499), and Thorlabs matching funds to Praevium Research Inc. Additional support from the Massachusetts Lions Clubs, and a Natural Sciences and Engineering Research Council of Canada Scholarship.
Financial Disclosure
Jay S. Duker is a consultant for and receives research support from Carl Zeiss Meditec, Topcon, and OptoVue. James G. Fujimoto receives royalties from intellectual property owned by Massachusetts Institute of Technology and licensed to Carl Zeiss Meditec and OptoVue, and has stock options in Optovue.
References
-
Donders FC (1855) Beitrage Zur Pathologischen Anatomie des Auges. Graefes Arch Clin Exp Ophthalmol 1: 106-118.
-
Ryan SJ, Sadda SR, Hinton DR (2013) Age-Related Macular Degeneration. In: Ryan SJ (ed) Retinab China: Saunders 1150-1182.
-
Klein R, Cruickshanks KJ, Nash SD, Krantz EM, Nieto FJ, et al. (2010) The prevalence of age-related macular degeneration and associated risk factors. Arch Ophthalmol 128: 750-758.
-
Silvestri G, Williams MA, McAuley C, Oakes K, Sillery E, et al. (2012) Drusen prevalence and pigmentary changes in Caucasians aged 18-54 years. Eye (Lond) 26: 1357-1362.
-
Drexler W, Morgner U, Ghanta RK, Kartner FX, Schuman JS, et al. (2001) Ultrahigh-Resolution Ophthalmic Optical Coherence Tomography. Nature Medicine 7: 502-507.
-
Kakinoki M, Sawada O, Sawada T, Kawamura H, Ohji M (2009) Comparison of macular thickness between Cirrus HD-OCT and Stratus OCT. phthalmic Surg Lasers Imaging 40: 135-140.
-
Souied EH, Leveziel N, Letien V, Darmon J, Coscas G, et al. (2006) Optical coherent tomography features of malattia leventinese. Am J Ophthalmol 141: 404-407.
-
Ryan SJ, Sadda SR, Hinton DR (2013) Retinopathy of Prematurity. In: Ryan SJ (ed) Retina China: Saunders 1920-1932.
-
Kim DY, Hwang JC, Moore AT, Bird AC, Tsang SH (2010) Fundus autofluorescence and optical coherence tomography of congenital grouped albinotic spots. Retina 30: 1217-1222.





