Clinical Medical Reviews and Case Reports
A Case of Acute Pancreatitis without Enzyme Elevation - A Rare Presentation of a Common Condition
Edupuganti Mohan Mallikarjuna Rao1*, Vjayanthi Ganga2, Michael Moore2 and Srikanth Medarametla1
1Department of Cardiology, University of Arkansas for Medical Sciences, Arkansas, USA
2Baptist Health System, Internal Medicine Residency program, Baptist Medical Center, USA
*Corresponding author: Edupuganti Mohan Mallikarjuna Rao, Department of Cardiology, University of Arkansas for Medical Sciences, Little Rock, Arkansas 72205, USA, E-mail: mmedupuganti@gmail.com
Clin Med Rev Case Rep, CMRCR-2-066, (Volume 2, Issue 10), Case Report; ISSN: 2378-3656
Received: April 20, 2015 | Accepted: October 27, 2015 | Published: October 30, 2015
Citation: Rao EMM, Ganga V, Moore M, Medarametla S (2015) A Case of Acute Pancreatitis without Enzyme Elevation - A Rare Presentation of a Common Condition. Clin Med Rev Case Rep 2:066. 10.23937/2378-3656/1410066
Copyright: © 2015 Rao EMM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Acute Pancreatitis is most often diagnosed based on a threefold elevation of amylase and lipase in the appropriate clinical setting. Very rarely the enzyme levels may be completely normal casting a doubt on the diagnosis. We present a case of acute pancreatitis without elevation of enzymes, review the literature, enlist the situations where serum enzyme levels are not elevated, discuss the diagnostic criteria, enzyme kinetics and briefly delve into the newer biomarkers of acute pancreatitis.
Keywords
Acute pancreatitis, Amylase, Llipase, Computed tomographic scan, Abdominal pain
Introduction
The diagnosis of pancreatitis requires at least two of the following three criteria including a characteristic abdominal pain, enzyme elevation three times normal and findings on imaging studies. There are several reports in the literature of pancreatitis without elevation of amylase. However it is extremely rare not to have elevations of serum lipase. When faced with a patient with characteristic abdominal pain and normal enzyme levels very few clinicians are comfortable pursuing a diagnosis with imaging studies particularly in the presence of relative contraindication to administering contrast agents such as acute kidney injury which frequently accompanies this condition. Patients could be misdiagnosed as drug seeking or the symptoms could be labeled as a functional disorder leading to catastrophic outcomes.
On the other hand administering contrast agents and imaging everyone with abdominal pain to rule out a rare possibility of pancreatitis in the absence of enzyme elevation or to admit them for observation is not only inappropriate but also costly. There is a need for newer and better markers that not only help in the diagnosis but also provide useful prognostic information.
Case Presentation
A 44 year old Caucasian male presented with left upper quadrant abdominal pain of 2 days duration. The pain was constant, sharp, radiated to the back and was aggravated on movement and relieved by rest. Patient also had 3 to 4 episodes of loose non bloody watery bowel movements over a period of 48 hours. The past medical history was significant for obesity, BMI > 35 KG/M, fatty liver, chronic back pain, hypertension, dyslipidemia, a history of smoking, alcohol abuse and drug use. He was on benazepril, metoprolol, fenofibric acid, hydrochlorthizide, and oxycodone at the time of presentation.
Examination revealed a middle aged obese man in distress, the blood pressure was on the lower side measuring 93/50 mmHg and tenderness was elicited on palpation of the right upper quadrant, the bowel sounds were diminished.
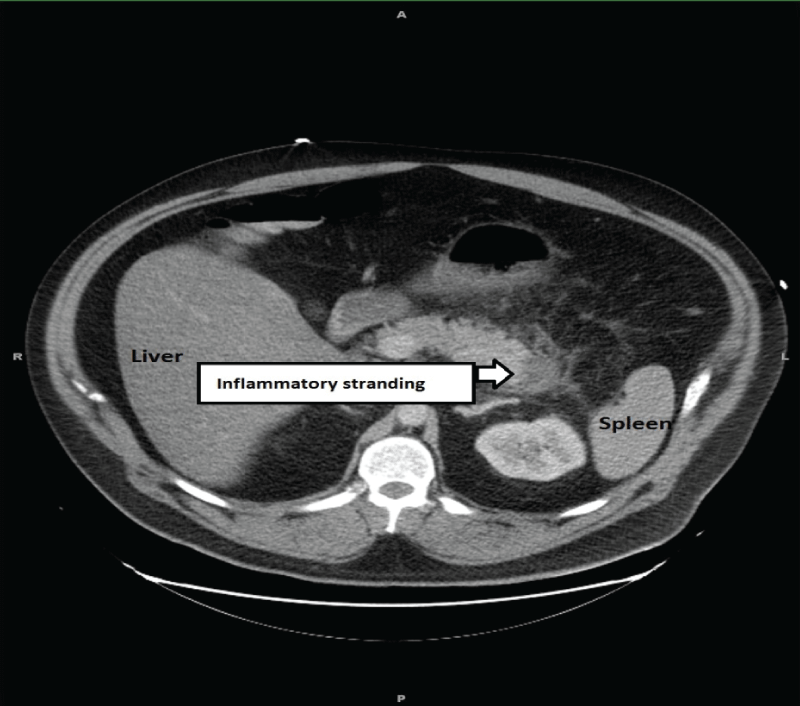
Laboratory examination revealed acute kidney injury with a blood urea nitrogen 32 mg/dl, creatinine 1.68 mg/dl, calcium 8.3 meq/dl, albumin 3.4g/dl, amylase 68 U/L, lipase 25 U/L and the white cell count was elevated at 18100. A computed tomographic scan of the abdomen revealed inflammatory stranding around the tail of pancreas (Figure 1).
.
Figure 1: Cross sectional computed tomographic image of the pancreas demonstrating peripancreatic stranding suggestive of acute pancreatitis.
View Figure 1
The patient was admitted to the hospital with a differential diagnosis of pancreatitis versus penetrating gastric ulcer eroding into the tail of pancreas. An upper gastrointestinal endoscopy was normal. The patient was managed conservatively and he quickly improved and was discharged after 5 days. The serum enzyme levels continued to be normal throughout the hospital course.
Discussion
In the appropriate clinical setting the diagnosis of pancreatitis is usually made on the basis of elevated amylase and lipase levels with or without imaging studies. After the onset of acute pancreatitis serum amylase increases over 3 to 6 hours with a half-life of 10 to 12 hours. It remains elevated for 3 to 5 days and is excreted by the kidneys. Serum lipase levels increases over 3 to 6 hours and peaks is 24 hours (t½ 6-13 hrs). Unlike amylase serum lipase is reabsorbed by the kidney and hence remains elevated for 1 to 2 weeks [1].
There are several case reports of pancreatitis with normal amylase levels. According to some authors 19-32% of patients presenting with acute pancreatitis have a normal amylase level [2,3]. The sensitivity of amylase is 79% with a range of 68 to 99.5%, the specificity is between 71 to 98%. The sensitivity of lipase is 96.5% with a range of 80 to 100% [3].
Role of serum amylase and lipase in the diagnosis of acute pancreatitis
Serum amylase and lipase can be normal in children with acute pancreatitis. Normal lipase in acute pancreatitis has also been reported in children with acute pancreatitis. Coffey et al studied pancreatitis in 125 patients and determined that the diagnostic yields, in descending order, were 93% for serum lipase, 67% for CT, 54% for serum amylase and 27% for ultrasound respectively. They concluded that the best way to diagnose the condition was to use a combination of tests [4].
A normal serum amylase and lipase does not exclude pancreatitis, at the same time, it is important to remember that these enzymes can be elevated in a number of other conditions mentioned in table 1.
![]()
Table 1: Differential diagnosis of elevated amylase lipase
View Table 1
Given the above limitations of serum amylase and lipase a number of other markers of the disease, each with its own advantages and limitations have been studied and are listed in table 2.
![]()
Table 2: Newer Enzymatic Markers of Pancreatitis
View Table 2
Conclusion
Pancreatitis is a common clinical problem and the usual enzymatic markers of pancreatitis can be falsely normal, furthermore their levels do not reflect the severity of the disease and the clinician is left with cumbersome tools such as acute physiologic and chronic health evaluation (APACHE) or ransons criteria. The newer enzymatic markers have the advantage of being sensitive and specific as well as being useful in gauging the severity of the condition. It is likely that these markers will be validated in clinical studies and will be increasingly used to diagnose acute pancreatitis and predict the risk of complications.
References
-
Shah AM, Eddi R, Kothari ST, Maksoud C, DiGiacomo WS, et al. (2010) Acute pancreatitis with normal serum lipase: a case series. JOP 11: 369-372.
-
Spechler SJ, Dalton JW, Robbins AH, Gerzof SG, Stern JS, et al. (1983) Prevalence of normal serum amylase levels in patients with acute alcoholic pancreatitis. Dig Dis Sci 28: 865-869.
-
Orebaugh SL (1994) Normal amylase levels in the presentation of acute pancreatitis. Am J Emerg Med 12: 21-24.
-
Coffey MJ, Nightingale S, Ooi CY (2014) Diagnosing acute pancreatitis in children: what is the diagnostic yield and concordance for serum pancreatic enzymes and imaging within 96 hours of presentation? Pancreatology 14: 251-256.
-
Williamson MA, Snyder LM, Wallach JB (2011) Wallach's interpretation of diagnostic tests. (9th edn) Philadelphia: Wolters Kluwer/Lippincott Williams & Wilkins Health.
-
Pieper-Bigelow C, Strocchi A, Levitt MD (1990) Where does serum amylase come from and where does it go? Gastroenterol Clin North Am 19: 793-810.
-
Chen CC, Wang SS, Chao Y, Chen SJ, Lee SD, et al. (1994) Serum pancreas-specific protein in acute pancreatitis. Its clinical utility in comparison with serum amylase. Scand J Gastroenterol 29: 87-90.
-
Buchler M, Malfertheiner P, Schadlich H, Nevalainen TJ, Friess H, et al. (1989) Role of phospholipase A2 in human acute pancreatitis. Gastroenterology 97: 1521-1526.
-
Clave P, Guillaumes S, Blanco I, Nabau N, Merce J, et al. (1995) Amylase, lipase, pancreatic isoamylase, and phospholipase A in diagnosis of acute pancreatitis. Clin Chem 41: 1129-1134.
-
Gudgeon AM, Heath DI, Hurley P, Jehanli A, Patel G, et al. (1990) Trypsinogen activation peptides assay in the early prediction of severity of acute pancreatitis. Lancet 335: 4-8.
-
Tenner S, Fernandez-del Castillo C, Warshaw A, Steinberg W, Hermon-Taylor J, et al. (1997) Urinary trypsinogen activation peptide (TAP) predicts severity in patients with acute pancreatitis. Int J Pancreatol 21:105-110.
-
Neoptolemos JP, Kemppainen EA, Mayer JM, Fitzpatrick JM, Raraty MG, et al. (2000) Early prediction of severity in acute pancreatitis by urinary trypsinogen activation peptide: a multicentre study. Lancet 355: 1955-1960.
-
Hedstrom J, Sainio V, Kemppainen E, Puolakkainen P, Haapiainen R, et al. (1996) Urine trypsinogen-2 as marker of acute pancreatitis. Clin Chem 42: 685-690.
-
Pezzilli R, Billi P, Plate L, Barakat B, Bongiovanni F, et al. (1994) Human pancreatic secretory trypsin inhibitor in the assessment of the severity of acute pancreatitis. A comparison with C-reactive protein. J Clin Gastroenterol 19: 112-117.
-
Kemppainen E, Hedstrom J, Puolakkainen P, Halttunen J, Sainio V, et al. (1997) Increased serum trypsinogen 2 and trypsin 2-1 antitrypsin complex values identify endoscopic retrograde cholangiopancreatography induced pancreatitis with high accuracy. Gut 41: 690-695.
-
Sainio V, Puolakkainen P, Kemppainen E, Hedstrom J, Haapiainen R, et al. (1996) Serum trypsinogen-2 in the prediction of outcome in acute necrotizing pancreatitis. Scand J Gastroenterol 31: 818-824.
-
Hedstrom J, Sainio V, Kemppainen E, Haapiainen R, Kivilaakso E, et al. (1996) Serum complex of trypsin 2 and alpha 1 antitrypsin as diagnostic and prognostic marker of acute pancreatitis: clinical study in consecutive patients. BMJ 313: 333-337.
-
Hedstrom J, Kemppainen E, Andersen J, Jokela H, Puolakkainen P, et al. (2001) A comparison of serum trypsinogen-2 and trypsin-2-alpha1-antitrypsin complex with lipase and amylase in the diagnosis and assessment of severity in the early phase of acute pancreatitis. Am J Gastroenterol 96: 424-430.
-
Pezzilli R, Billi P, Plate L, Bongiovanni F, Morselli-Labate AM, et al. (1994) Human pancreas-specific protein/procarboxypeptidase B: a useful serum marker of acute pancreatitis. Digestion 55: 73-77.
-
Appelros S, Thim L, Borgstrom A (1998) Activation peptide of carboxypeptidase B in serum and urine in acute pancreatitis. Gut 42: 97-102.





