Clinical Medical
Reviews and Case Reports
Case Series and Proposed System of Nomenclature for Aneurysms of the Portal Venous System
Anthony Visioni1, John Ammori2 and Jeffrey Hardacre2*
1Department of Surgical Oncology, Roswell Park Cancer Institute, Buffalo, New York, USA
2Department of Surgery, Division of Surgical Oncology, University Hospitals Case Medical Center, Cleveland, OH, USA
*Corresponding author: Jeffrey Hardacre, 11100 Euclid Ave, Department of Surgery, 7th Floor, Lakeside Building, Cleveland, OH 44106, USA, E-mail: jeffrey.hardacre@uhhospitals.org
Clin Med Rev Case Rep, CMRCR-2-068, (Volume 2, Issue 11), Case Series; ISSN: 2378-3656
Received: September 02, 2015 | Accepted: November 06, 2015 | Published: November 09, 2015
Citation: Visioni A, Ammori J, Hardacre J (2015) Case Series and Proposed System of Nomenclature for Aneurysms of the Portal Venous System. Clin Med Rev Case Rep 2:068. 10.23937/2378-3656/1410068
Copyright: © 2015 Visioni A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Aneurysms of the portal venous system (PVS) are rare clinical entities. The natural history and optimal management of this aneurysm are not fully understood. We present two cases of PVS aneurysms with their management. In addition, we review the literature and propose a system of classification to facilitate further research into this clinical entity.
Keywords
Aneurysm, Mesenteric veins, Portal vein, Portal system
Introduction
Aneurysms of the portal vein (PV), superior mesenteric vein (SMV), and splenic vein (SV) are rare. There are less than 200 cases reported in the English literature since the condition was first described in 1956 by Barzilai and Klecker [1]. Studies to date have commented on the radiographic characteristics, natural history, and possible management options of this clinical entity. While most of the literature falls under the category of portal venous aneurysms, there are also case reports of isolated SMV and SV aneurysms [2-4]. We present two cases, an SMV and an SV aneurysm, and propose a classification system to facilitate ongoing research into this clinical entity.
Case 1
The patient is a 75 year-old man referred to our surgical clinic for the work-up of a mass in the head of the pancreas. His surgical history is significant for a laparoscopic cholecystectomy and subsequent ERCP for retained common bile duct stone 4 years prior to presentation. He has also undergone a vagotomy and Billroth I gastrectomy for perforated peptic ulcer disease approximately 40 years ago.
The pancreatic mass was discovered by his gastroenterologist during the work-up and treatment of a common bile duct stone. The patient underwent an ERCP, which revealed an 8 mm common bile duct stone, which was removed with sphincterotomy and balloon extraction.
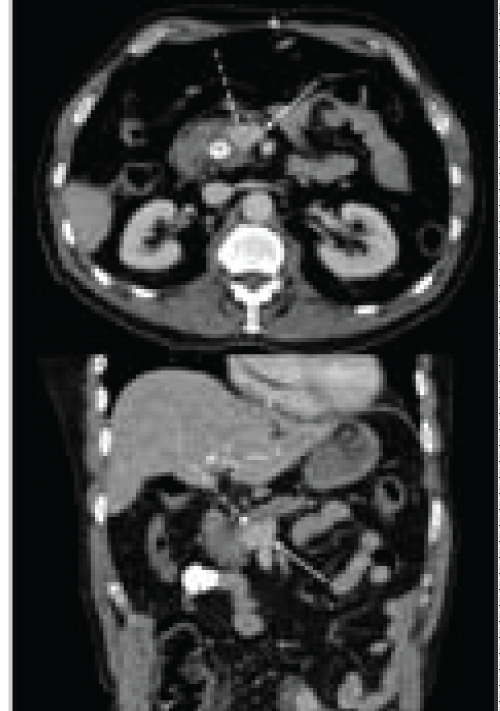
Immediately after the procedure the patient developed severe abdominal pain concerning for a perforation, and therefore, a contrast-enhanced CT of the abdomen and pelvis was obtained. This revealed a well-defined contrast-enhancing lesion in the uncinate process of the pancreas measuring approximately 2 cm by 2 cm with enlarged peripancreatic and porta hepatis lymph nodes compatible with a neuroendocrine tumor (Figure 1). The patient then underwent a follow-up endoscopic ultrasound, which did not show the pancreatic head mass.
.
Figure 1: Pre-operative contrast-enhanced CT scan showing 2 cm x 2 cm mass in the uncinate process of the pancreas (dashed arrow) closely associated with SMV (solid arrow). Black asterisk on top image indicates contrasted-filled common bile duct post ERCP. Axial images on top and coronal images on bottom
View Figure 1
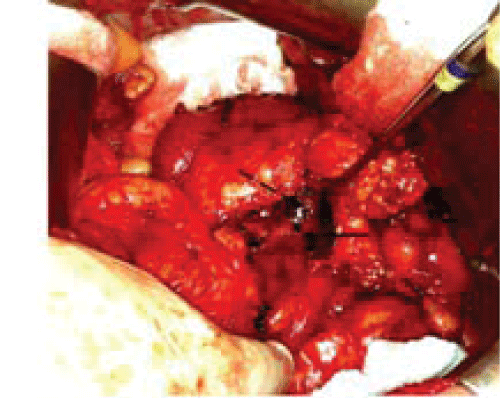
After being seen in our clinic, he underwent an octreotide scan, which was negative. After counseling the patient on the possible etiologies of this mass in the pancreas it was decided that he would undergo an operation with the intent to resect the lesion. In the operating room, after mobilization of the pancreas it was noted that the lesion was a superior mesenteric vein aneurysm with no pathology within the pancreas (Figure 2). The aneurysm was repaired via aneurysmorrhapy (Figure 3).
.
Figure 2: Intra-operative image of SMV (solid arrow) and saccular SMV aneurysm (dashed arrow). The inferior border of pancreas is under retractor. Patient's head oriented toward the top of photo.
View Figure 2
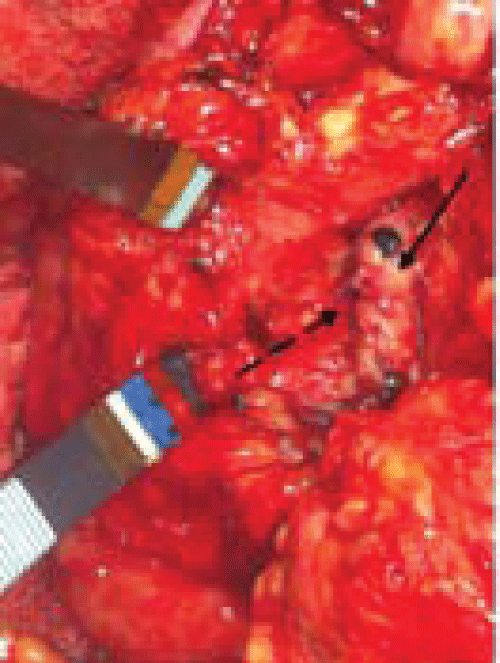
.
Figure 3: Intra-operative image status post aneurysmorrhaphy. Solid arrow indicates SMV with dashed arrow indicating suture line. Forceps are retracting pancreas. Patient's head oriented toward the top of photo.
View Figure 3
The patient recovered from this operation well. A post-op contrast-enhanced CT scan showed the SMV to be patent with resolution of the aneurysm. The patient was seen last in clinic four months post-operatively and has made a complete recovery with no further symptoms or complications.
Case 2
The patient is a 36 year-old man with no significant past medical history who was referred to our clinic for massive splenomegaly. The patient originally presented to his primary care physician for an unrelated complaint and was discovered to have palpable splenomegaly on abdominal exam. The patient reported vague abdominal fullness for a couple of years; however he had no other associated symptoms. Routine blood tests revealed thrombocytopenia but were otherwise unremarkable. A CT scan of the chest, abdomen, and pelvis demonstrated an 18 cm by 18 cm spleen with central irregular hypodensity measuring 7.4 cm. It also showed large splenic varices with enlargement of the portal and splenic veins. Interestingly, the splenic vein appeared quite tortuous, with a portion of the vein appearing to double back on itself.
The patient was referred to a hematologist/oncologist with a concern for lymphoma. A bone marrow biopsy was performed and revealed no signs of malignancy. Abdominal ultrasound with duplex demonstrated the enlarged spleen with a large heterogeneous echogenic mass. Also noted was dilatation of the portal vein to 2.7 cm with splenic vein dilatation, as well. Both had normal antegrade flow. Finally, a PET/CT of the abdomen and pelvis revealed no increased FDG activity in the spleen and no suspicious activity in the lymph node of the upper abdomen.
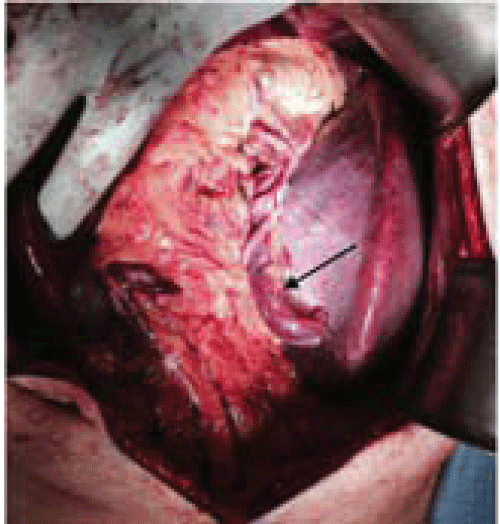
No studies to date had given a definitive diagnosis; he was, therefore, referred to our surgery clinic for consideration of splenectomy. When seen in our clinic the decision was made to proceed with splenectomy for a definitive pathologic diagnosis. In the operating room, the spleen was noted to have large varices (Figure 4) that required division with a vascular stapler. The spleen was resected without complication and sent to pathology fresh for lymphoma testing. On examination of the retroperitoneum with the spleen removed, an approximately 8 cm splenic vein aneurysm was noted around the tail of the pancreas. This was in the location on the CT scan where the splenic vein appeared to double back on itself. This was resected as well (Figure 5). The patient had an uneventful post-operative course and was able to be discharged home on post-operative day 4. Pathologic examination of the spleen revealed no signs of malignancy. The patient was seen in clinic 2 weeks post-operatively and noted to be recovering well.
.
Figure 4: Intra-operative image showing markedly enlarged spleen with splenic varix (solid arrow). Patient's head oriented toward the top of photo.
View Figure 4
Discussion
In this report, we present two aneurysms of the portal venous system, a saccular SMV aneurysm masquerading as a pancreatic neuroendocrine tumor and a SV aneurysm associated with splenomegaly and diffuse dilatation of the portal venous system. In both of these cases contrast enhanced imaging demonstrated these aneurysms in retrospect. It was not immediately recognized in the first case due to it's classical appearance as a neuroendocrine tumor in the head of the pancreas. In the second case, the diffuse dilatation of the portal and splenic veins distorted the normal anatomy such that the splenic vein appeared to fold back on itself, but was in fact aneurysmal.
These aneurysms are very rare clinically entities with a reported 0.43% prevalence for aneurysms of the portal venous system [5]. In fact, there are less than 200 cases reported in the English literature with the largest series being 6 patients [6]. Given the rarity of the condition, determining the causes and natural history of aneurysms of the portal venous system is difficult. There is evidence that portal hypertension, congenital anomalies, hereditary conditions, and inflammatory processes may play a role in the etiology of these aneurysms, either individually or in combination [7]. These aneurysms have been discovered in all age groups, from in utero to the elderly [8,9].
In terms of natural history, there are very little data to suggest the course of these aneurysms. The longest follow up in an untreated patient appears to be 10 years without any adverse events [10]. This has led some authors to suggest non-operative management with close follow-up for these aneurysms. There have even been reports of spontaneous regression [11]. This, however, does not mean that there are no complications from this clinical entity. Cases of biliary obstruction [12], thrombosis [13], and rupture [14] have been reported; and there are data to suggest 44.7% and 7.3% of these aneurysms present with abdominal pain and GI bleeding, respectively [15].
One of the difficulties with a very rare condition is developing a cohesive body of literature. This condition is also quite heterogeneous with various anatomic locations affected, different etiologies, and markedly different outcomes. Reports of these aneurysms are becoming more common, and with the increase in abdominal imaging being utilized these aneurysms will likely be detected more often. Therefore, we propose a system of naming to ensure direct comparisons between various aneurysms.
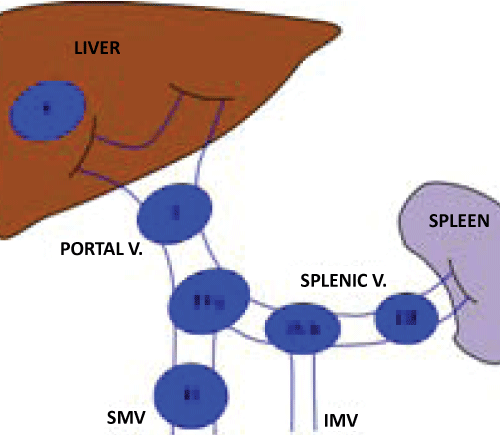
First we propose that the term portal system aneurysms be used to describe this clinical entity. While some authors use the term portal venous aneurysm to refer to any aneurysm of the portal, superior mesenteric or splenic veins, others describe each of these entities in isolation. The term portal system aneurysm allows for the inclusion of superior mesenteric and splenic vein aneurysms with less confusion. By using the term portal system aneurysm, however, more accurate description of the location is necessary. Therefore, we delineate 5 types of portal system aneurysms based on anatomic location (Figure 6). Type I aneurysms are located within the extra-hepatic portal vein. Type II aneurysms are within the superior mesenteric vein proximal to the confluence of the splenic vein. Type III aneurysms are within the splenic vein. Type IV aneurysms refer to aneurysms at the confluence of veins. Aneurysms at the confluence of the superior mesenteric vein and splenic vein are type IVa, while those at the confluence of the splenic vein and inferior mesenteric vein are IVb. Type V aneurysms refer to all aneurysms of the portal system that are intra-hepatic.
.
Figure 6: Proposed nomenclature of portal systems aneurysms. Type I are aneurysms of the extra-hepatic portal vein. Type II are aneurysms of the superior mesenteric vein. Type III are of the splenic vein. Type IV are aneurysm at the confluence of veins with IVa at the SMV/splenic vein confluence and IVb at the IMV/splenic vein confluence. Type V aneurysms are intra-hepatic.
View Figure 6
Conclusion
We present two cases of portal system aneurysms and their management. Previous reports have varied widely on the etiology, natural history, and, therefore, management of these aneurysms. Given the increasing reports of aneurysms of the portal venous system it is increasingly important that authors have a common nomenclature. This will allow more direction comparisons between aneurysms, which may elucidate different causes and outcomes for different types of aneurysms and provide for more rational treatment of this clinical entity.
References
-
Barzilai R, Kleckner MS Jr (1956) Hemocholecyst following ruptured aneurysm of portal vein; report of a case. AMA Arch Surg 72: 725-727.
-
Wolosker N, Zerati AE, Nishinari K, de Melo Galvao Filho M, Wolosker AM (2004) Aneurysm of superior mesenteric vein: case report with 5-year follow-up and review of the literature. J Vasc Surg 39: 459-461.
-
Gupta A, Kumar Singhal M, Maheshwarappa RP, Meena ML (2013) Splenic vein aneurysm: a rare clinical entity. Indian J Gastroenterol 32: 204-205.
-
Truong T, Vu JH, Matteo J (2012) Superior mesenteric vein aneurysm: a case report. Vasc Endovascular Surg 46: 89-92.
-
Koc Z, Oguzkurt L, Ulusan S (2007) Portal venous system aneurysms: imaging, clinical findings, and a possible new etiologic factor. AJR Am J Roentgenol 189: 1023-1030.
-
Ohnami Y, Ishida H, Konno K, Naganuma H, Hamashima Y, et al. (1997) Portal vein aneurysm: report of six cases and review of the literature. Abdom Imaging 22: 281-286.
-
Gallego C, Velasco M, Marcuello P, Tejedor D, De Campo L, et al. (2002) Congenital and acquired anomalies of the portal venous system. Radiographics 22: 141-159.
-
Gallagher DM, Leiman S, Hux CH (1993) In utero diagnosis of a portal vein aneurysm. J Clin Ultrasound 21: 147-151.
-
Schwope RB, Margolis DJ, Raman SS, Kadell BM (2010) Portal vein aneurysms: a case series with literature review. J Radiol Case Rep 4: 28-38.
-
Rafiq SA, Sitrin MD (2007) Portal vein aneurysm: case report and review of the literature. Gastroenterol Hepatol (N Y) 3: 296-298.
-
Lall P, Potineni L, Dosluoglu HH (2011) Complete spontaneous regression of an extrahepatic portal vein aneurysm. J Vasc Surg 53: 206-208.
-
Lall C, Verma S, Gulati R, Bhargava P (2012) Portal vein aneurysm presenting with obstructive jaundice. J Clin Imaging Sci 2: 54.
-
De Gaetano AM, Andrisani MC, Gui B, Maresca G, Ionta R, et al. (2006) Thrombosed portal vein aneurysm. Abdom Imaging 31: 545-548.
-
Smith TJ, Morehouse DL (2011) Superior mesenteric vein aneurysm rupture. Vasc Endovascular Surg 45: 559-560.
-
Sfyroeras GS, Antoniou GA, Drakou AA, Karathanos C, Giannoukas AD (2009) Visceral venous aneurysms: clinical presentation, natural history and their management: a systematic review. Eur J Vasc Endovasc Surg 38: 498-505.