Clinical Medical
Reviews and Case Reports
Use of Infraclavicular Temporary Perineural Catheter in the Exercise for Range of Joint Motion - Case Report
Ilke Kupeli1*, Ufuk Kuyrukluyildiz2, Hakan Gokalp Tas2 and Aysin Alagol2
1Mengucek Gazi Training and Research Hospital, Department of Anesthesiology and Reanimation, Erzincan, Turkey
2Department of Anesthesiology and Reanimation, Erzincan University, Erzincan, Turkey
*Corresponding author: Ilke Kupeli, Mengucek Gazi Training and Research Hospital, Department Of Anesthesiology and Reanimation, Erzincan, Turkey, Tel: 00905555485632, Fax: 00904462122200, E-mail: ilkeser2004@gmail.com
Clin Med Rev Case Rep, CMRCR-2-072, (Volume 2, Issue 12), Case Report; ISSN: 2378-3656
Received: November 09, 2015 | Accepted: November 28, 2015 | Published: December 02, 2015
Citation: Kupeli I, Kuyrukluyildiz U, Tas HG, Alagol A (2015) Use of Infraclavicular Temporary Perineural Catheter in the Exercise for Range of Joint Motion - Case Report. Clin Med Rev Case Rep 2:072. 10.23937/2378-3656/1410072
Copyright: © 2015 Kupeli I, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Olecranon fractures are the most common type of injury seen in the upper extremities and restricted joint mobility may be developed due to the long plaster cast time. Most of these patients will be required to participate in intense physical therapy in order to maintain and increase range of motion postoperatively. This physiotherapy process is a serious stressor for these patients because of pain. In addition to several modalities such as systemic administration of opioids, permanent/temporary perineural catheters are used in order to decrease pain and allow patients to exercise more comfortably. Local anesthetic administration through perineural catheter has been proven to improve patients' rehabilitation and healing. Herein, we present a 41 year old male patient with restricted motion of the elbow following treatment of olecranon fracture, in which infraclavicular temporary perineural catheter decreased pain and eased exercise during physiotherapy.
Temporary peripheral nerve catheter can be used for a short time or intermittently in order to provide a postoperative pain free physiotherapy course and to accelerate rehabilitation and healing providing a good maintenance and control processes.
Keywords
Bupivacaine, Infraclavicular temporary perineural catheter, Olecranon fracture
Introduction
Olecranon fractures are the most common type of injury seen in the upper extremities with an incidence of 10% [1,2]. Displaced olecranon fractures are intraarticular fractures which always require surgical treatment. Whereas conservative treatment is recommended for the fractures without displacement or a maximal displacement of 2 to 3 mm [3,4]. However, conservative treatment-related restricted joint mobility may develop due to a poor/inadequate reduction and long plaster cast time [3,4]. In olecranon fractures that are related to the elbow joint and displaced more than 2-3 mm, goal of the surgical treatment is to provide anatomical repair of the joint and to begin early elbow motions in order to prevent loss of motion and function [4]. Early movement of the elbow provides functional improvement of both the elbow and the forearm [5].
Pain management is an important aspect of orthopedic and trauma surgery. Continuous peripheral nerve block involves continuous or intermttent administration of the local anesthetic in low doses via a catheter inserted along the peripheral nerves. This method decreases the need for systemic drug administration and provides postoperative pain control in the upper extremities [6]. Therefore, it enables a comfort physiotherapy process for patients without feeling pain during the early elbow movements.
Herein, we present a case with restricted motion of the elbow following treatment of olecranon fracture, in which infraclavicular temporary perineural catheter decreased pain and eased exercise during physiotherapy. The patient was informed about the publication of this report and was written consent.
Case Report
A 41 year old male patient presented to the orthopedic clinic with the complaint of pain in the left elbow. It was found at the physical examination that, the left elbow was at 90° flexion posture following previous operation for left olecranon fracture. Following joint debridement, physiotherapy was scheduled in order to postoperatively increase the range of motion. Medical history of the patient who was consulted with the anesthesia polyclinic was unremarkable except an operated olecranon fracture and splenectomy. On his examination, the left elbow was at 90° flexion. Preoperative laboratory values were found as hemoglobin: 15 gr/dl, hematocrit: 42%, platelet: 302,000 u/L, International normalized ratio (INR): 1.00, prothrombin time (PT): 12 sec and activated thromboplastin time (aPTT): 39.2 sec, while biochemical parameters were in the normal range.
Since the patient scheduled for physiotherapy in the postoperative period; infraclavicular nerve block and insertion of temporary perineural catheter were decided for anesthesia management. Patient was taken to the waiting room in the morning of the operation. Peripheral vascular access was opened and standard monitoring was carried out. After intravenous administration of 2 mg midazolam (DORMICUM 15 mg/3 ml, Deva, Turkey), blood pressure was 120/70 mmhg, heart rate was 80 pulse/minute and peripheral oxygen saturation (SpO2) was 97%.
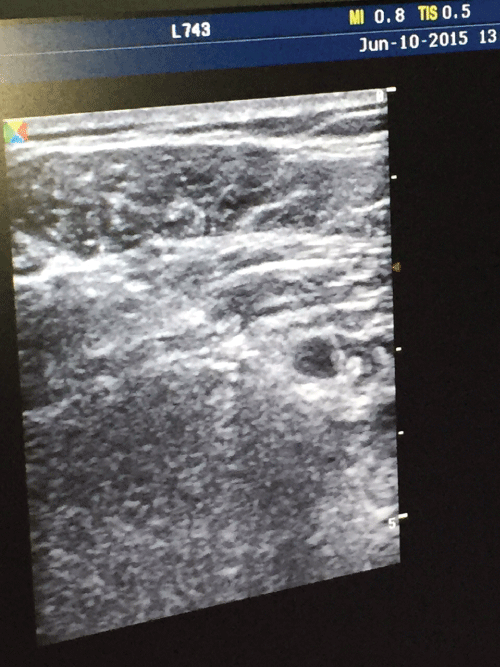
The patient was placed in the supine with his head facing side of the nerve block. The skin was disinfected with poviiodex antiseptic 10% and linear probe (6-13 MHz) of ultrasound (SonoSite M-Turbo®, Sonosite, USA) was placed on the parasagittal plane so that the axillary artery could be determined. Once the artery was identified, after subcutaneous local anesthesia with 2 cc lidocaine (Aritmal 2%, Osel, Turkey) the needle was inserted in-plane. It was guided toward posterior to axillary artery and 2 cc of lidocaine was injected in order to control adequate needle placement and distribution. After the location was confirmed, each cord was injected with 5 cc local anesthetic bupivacaine (% 0.5 Marcain® flakon, Astra Zeneca, Swiss). We had to use a long acting, slow onset local anesthetic because in those days there was no fast onset, short acting local anesthetic in our hospital due to economic problems. Following infraclavicular nerve block by this way and tip of the needle was inserted posterior of axillary arter, the catheter was inserted 2-4 cm forward from the tip of the needle (close to the posterior cord) and fixed to the skin (Image 1). The catheter was targeting ulnar and median nerve distributions.
Sensorial nerve block was assessed using pinprick test: dorsum for radial nerve, 5th finger for ulnar nerve, 3rd finger for median nerve; 0: no change, 1: decreased sense of pain, 2: no pain. Motor nerve block was assessed modified Bromage scale; thumb abduction for radial nerve, thumb adduction for ulnar nerve, thumb opposition strength for median nerve; 0: no change in strength, 1: decreased strength, 2: complete motor block. For a successful nerve block; 2 point for each 3 nerve were accepted for sensorial block, while 1 and higher points for each 3 nerves were accepted for motor nerve block.
Following the successful nerve block, patient was taken to the operating room. At the end of the operation lasted 1.5 hours, patient was sent to the ward.
Postoperative pain control was achieved with perineural catheter. Before daily exercises to increase range of the joing motion, 5 cc bupivacaine (% 0.5 Marcain® flakon, Astra Zeneca, Swiss) was administered from the perineural catheter by the responsible anesthesiologist to enable patient being pain free during exercise over one week. Before each perineural injection and after exercise, maintenance and control of the catheter was carried out by the responsible anesthesiologist. When one-week exercise program was completed, catheter was removed and the patient was discharged.
Discussion
Olecranon fractures are the most common injury type among all the upper extremity injuries [1,2]. Olecranon is directly covered by bursa, subcutaneous fat tissue and skin, providing easy access to the fracture, but on the other hand implants have to be subcutaneously inserted. Location of the implant insertion is responsible for the complaints of patients and restricted elbow movements. In olecranon fractures that are related to the elbow joint and displaced more than 2-3 mm, goal of the surgical treatment is to provide anatomical repair of the joint and to begin early elbow motions in order to prevent loss of motion and function [5].
A Strict pain control in the postoperative period provides both patient to remain hemodynamically stable and not to feel pain during exercise. It also provides a good patient satisfaction, a quicker rehabilitation and healing [7]. Regional anelgesia techniques have important advantages such as an excellent pain control, decreased side effects and shorter time in the postoperative recovery room compared to genereal anethesia and systemic analgesia [8,9]. Infraclavicular block is one of the peripheral nerve blocks used in the upper extremity surgery and although minimal, it has risk of pneumothorax, hematoma and nerve injury [10].
Nerve stimulator and ultrasound can be used both complementary and separately. Ultrasound has gained importance in peripheral nerve and plexus blocks. Local anesthetic is observed, enabling lower doses administered around the nerve [11]. With continuous local anesthetic infusion from catheter, postoperative pain control can be obtained with less opioid consumption, patient satisfaction is increased and the healing process is accelerated [12]. However the peripheral nerve catheter is more time consuming, more expensive, more painful procedure for patients with higher complication rate and more need for postoperative care [13], when performed with ultrasound guiding it can be inserted in a shorted time and more successfully.
To protect sensorial nerve conduction inhibition and for optimal conduction block effectiveness; selection and concentration of the local anesthetic solution which is effective as rate of the perineural infusion depend on the nerves close to the tip of the inserted continuous perineural cathater especially unmyelinated fibers that consist of C-fibers [14]. Power of the local anesthetics is related to their physico-chemical and concentration. For example perineural 0.025% bupivacaine depresses nerve impulse conduction in Aα, Aδ and C fibers in the cat saphenous nerve by 28%, 48% and 90%, while 0.05% bupivacaine depresses by 44%, 74% and 96% and it is less effective in the mylinated fibers [15].
In our case, efective pain control was achieved through local anesthetic which could be administered through infraclavicular temporary perineural catheter before exercise over one week. It was shown in a study by Szucs et al. [16] that continuous femoral nerve block using bupivacaine provide a more superior anelgesia at a rate of 4 ml/h for 72 hours in the femoral fractures. Similarly Yamakado [17] found that visual pain scores and number of interventions to relieve pain were significantly lower on the postoperative first and second days in the continuous suprascapular nerve block group compared to the controls.
There are some studies indicating that perineural infusion caused muscle weakness and undesired sensorial deficits [18]. As some studies reported that a low local analgesic concentration should be used in order to minimize this muscle weakness [19], while conversely other studies demonstrated that concentration and volume (rate) of the local anesthetic did not effect nerve block impact as long as the total dose was kept constant [20]. It was stated in a study by Bauer et al. [20] that concentration and volume of the local anesthetic was ineffective on the block characteristics (especially muscle weakness) during continuous nerve block and dose of the local anesthetic was primary responsible for the effects of perineural infusion.
Conclusion
In this study we demonstrated that temporary peripheral nerve catheter can be used for a short time or intermittently in order to provide a postoperative pain-free physiotherapy. It also accelerates rehabilitation and healing providing a good maintenance and control processes, especially in orthopedics and trauma patients.
Authors' contributions
"IK analyzed and interpreted the patient data, and was a major contributor in writing the manuscript. UK made scanning of literature. HGT revised the manuscript. AA edited the manuscript. All authors read and approved the final manuscript".
Acknowledgements
We would like to thank Mustafa Yurteken for his supports in preparing the manuscript.
References
-
Finsen V, Lingaas PS, Storrø S (2000) AO tension-band osteosynthesis of displaced olecranon fractures. Orthopedics 23: 1069-1072.
-
Hak DJ, Golladay GJ (2000) Olecranon fractures: treatment options. J Am Acad Orthop Surg 8: 266-275.
-
Crenshaw AH (1992) Fractures of Olecranon. In: Crenshaw AH Campbell's Operative Orthopaedics (81th edition) St. Luis, CV Mosby, 1025-1029.
-
Hotchkiss RN, Green OP (1991) Fractures and dislocations of the elbow. In: Rockwood CA, Green OP, Bucholz RW, Rockwood and Green's fractlures in adult (3rd edition), JB Lippincott Company, 795-805.
-
Karlsson MK, Hasserius R, Besjakov J, Karlsson C, Josefsson PO (2002) Comparison of tension-band and figure-of-eight wiring techniques for treatment of olecranon fractures. J Shoulder Elbow Surg 11: 377-382.
-
Bertini L, Borghi B, Grossi P, Casati A, Fanelli G (2001) Continuous peripheral block in foot surgery. Minerva Anestesiol 67: 103-108.
-
Weber SC, Jain R, Parise C (2007) Pain scores in the management of postoperative pain in shoulder surgery. Arthroscopy 23: 65-72.
-
Liu SS, Strodtbeck WM, Richman JM, Wu CL (2005) A comparison of regional versus general anesthesia for ambulatory anesthesia: a meta-analysis of randomized controlled trials. Anesth Analg 101: 1634-1642.
-
Liu SS, Wu CL (2007) The effect of analgesic technique on postoperative patient-reported outcomes including analgesia: a systematic review. Anesth Analg 105: 789-808.
-
Sandhu NS, Capan LM (2002) Ultrasound-guided infraclavicular brachial plexus block. Br J Anaesth 89: 254-259.
-
Mariano ER, Loland VJ, Sandhu NS, Bishop ML, Lee DK, et al. (2010) Comparative efficacy of ultrasound guided and stimulating popliteal-sciatic perineural catheters for postoperative analgesia. Can J Anaesth 57: 919-26.
-
White PF, Issioui T, Skrivanek GD, Early JS, Wakefield C (2003) The use of a continuous popliteal sciatic nerve block after surgery involving the foot and ankle: does it improve the quality of recovery? Anesth Analg 97: 1303-1309.
-
Ilfeld BM (2011) Continuous peripheral nerve blocks: a review of the published evidence. Anesth Analg 113: 904-925.
-
Liu SS, Salinas FV (2003) Continuous plexus and peripheral nerve blocks for postoperative analgesia. Anesth Analg 96: 263-272.
-
Ford DJ, Raj PP, Singh P, Regan KM, Ohlweiler D (1984) Differential peripheral nerve block by local anesthetics in the cat. Anesthesiology 60: 28-33.
-
Szucs S, Iohom G, O'Donnell B, Sajgalik P, Ahmad I, et al. (2012) Analgesic efficacy of continuous femoral nerve block commenced prior to operative fixation of fractured neck of femur. Perioperative Medicine 1:4.
-
Yamakado K (2014) Efficacy of arthroscopically placed pain catheter adjacent to the suprascapular nerve (continuous arthroscopically assisted suprascapular nerve block) following arthroscopic rotator-cuff repair. Open Access J Sports Med 5: 129-136.
-
Charous MT, Madison SJ, Suresh PJ, Sandhu NS, Loland VJ, et al. (2011) Continuous femoral nerve blocks: Varying local anesthetic delivery method (bolus versus basal) to minimize quadriceps motor block while maintaining sensory block. Anesthesiology 115: 774-781.
-
Lucic A, Chelly JE (2011) The relationship between ropivacaine infusions and postoperative falls after joint replacement: where is the evidence? Anesth Analg 113: 428-429.
-
Bauer M, Wang L, Onibonoje OK, Parrett C, Sessler DI, et al. (2012) Continuous Femoral Nerve Blocks: Decreasing Local Anesthetic Concentration to Minimize Quadriceps Femoris Weakness Anesthesiology. 116: 665-672.