Clinical Medical
Reviews and Case Reports
Coxofemoral Arthritis Caused by Mycobacterium Bovis after Bacillus Calmette-Guérin Therapy
R Bouchentouf1*, K Idrissi Koulali2, O Ghoundale3, A Elktaibi4 and A Benjelloun1
1Lung Disease service, Avicenne Military Hospital, Marrakech, Morocco
2Orthopaedic and Traumatology service, Military Hospital, Marrakech, Morocco
3Urology service, Avicenne Military Hospital, Marrakech, Morocco
4Anatomo-pathology service, Avicenne Military Hospital, Marrakech, Morocco
*Corresponding author: Bouchentouf Rachid, Lung disease Service, Avicenne Military Hospital, 12 bd la resistance, Marrakech 4000, Morocco, Tel: 212661295534, E-mail: bouchentouf_rachid@yahoo.fr
Clin Med Rev Case Rep, CMRCR-2-075, (Volume 2, Issue 12), Case Report; ISSN: 2378-3656
Received: November 18, 2015 | Accepted: December 04, 2015 | Published: December 08, 2015
Citation: Bouchentouf R, Idrissi Koulali K, Ghoundale O, Elktaibi A, Benjelloun A (2015) Coxofemoral Arthritis Caused by Mycobacterium Bovis after Bacillus Calmette-Guérin Therapy. Clin Med Rev Case Rep 2:075. 10.23937/2378-3656/1410075
Copyright: © 2015 Bouchentouf R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Intravesical therapy with bacillus calmette guérin (BCG) has proved to be effective in the treatment of superficial bladder tumors. BCG therapy is generally well tolerated, the osteo-articular adverse effects, occurring in approximately 0, 5 to 1% of patients.
Observation: We report the case of a 58-year-old man who presented with coxo-femoral arthritis after intra vesical BCG therapy performed 8 month earlier. The outcome was favorable following adapted antibiotic course.
Conclusion: Coxo-femoral arthritis is a rare complication of BCG therapy and diagnosis is often difficult to establish. This severe complication must be evoked in front of articular symptoms in patients treated with intra-vesical BCG therapy.
Keywords
BCG therapy, Arthritis, Mycobacterium bovis
Introduction
BCG therapy is the standard treatment for superficial bladder tumors. However, this treatment is not devoid of local and systemic side effects such as flu-like symptoms, liver granulomatosis, damage of both the gastrointestinal and the urinary tracts and bone lesions.
Rheumatological complications such as arthralgia, reactive arthritis and osteoarticular infections, although rare, were reported after BCG therapy [1].
Observation
We report the case of a 58 year-old male patient, heavy smoker (20 packs/year), not vaccinated with BCG, followed for superficial bladder tumor and treated with 6 instillations of BCG.
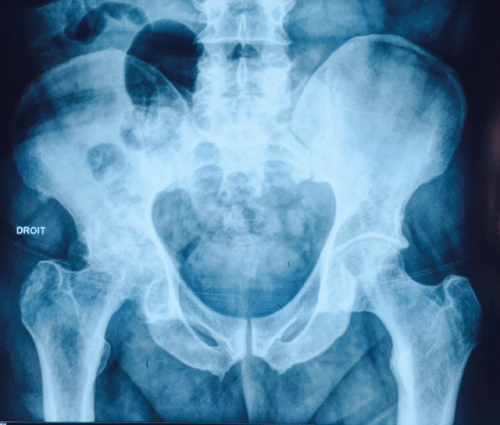
Eight months after the last instillation, the patient began to complain of pain in the right hip in a context of impaired general condition. This pain was of mechanical type without special radiation, but responsible for lameness. The clinical examination revealed a pelvic asymmetry with unequal legs. The usual blood tests showed normocytic normochromic anemia with a 10 g/dl Hb, normal leukocyte count, 30 mm erythrocyte sedimentation rate (ESR) in the first hour and a 25 mg/l CRP. Renal and hepatic biological assessments were normal. The tuberculin skin test was positive at 10 mm and HIV status was negative. Right hip and pelvis radiographs showed a narrowing coxo-femoral joint space with demineralization and geodes of the femoral head (Figure 1).
.
Figure 1: Pelvis radiographs showed a narrowing coxo-femoral joint space with demineralization and geodes of the femoral head.
View Figure 1
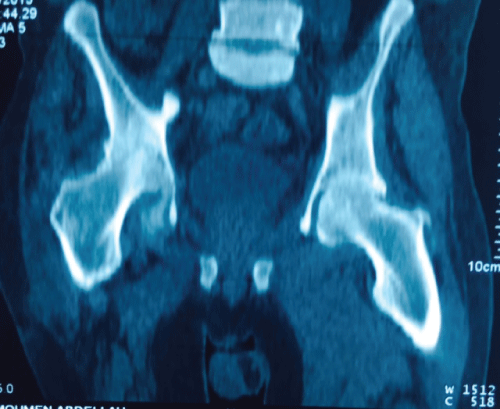
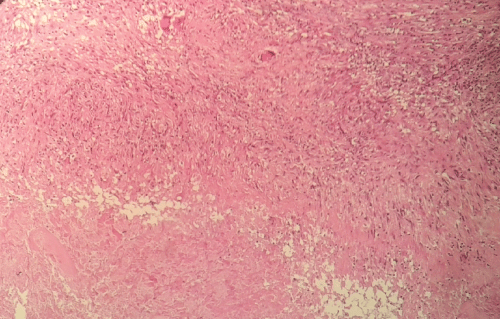
Pelvic CT scan showed an asymmetric basin, with the loss of the right femoral head sphericity and ankylosis of the coxo-femoral space with infiltration of the periarticular soft tissue (Figure 2). The search for germs in the joint fluid was negative on direct examination and the histological study of the synovial performed after a CT guided biopsy showed an epitheloid giant cell granuloma with caseous necrosis suggestive of coxo-femoral tuberculosis (Figure 3).
.
Figure 2: Pelvic CT scan showed an asymmetric basin, with the loss of the right femoral head sphericity and ankylosis of the coxo-femoral space.
View Figure 2
.
Figure 3: Photomicrograph of specimen showing epitheloid with Langhans giant cells and central caseous acellular necrosis. Hematoxylin-eosin staining × 250.
View Figure 3
Chest X-ray showed no abnormality and Koch bacillus research in sputum and urine was negative on direct examination. Culture of joint fluid showed smooth, whitish, small colonies (1-2 mm) of bacilli resistant to pyrazinamide which is evocative of Mycobacterium bovis. The patient received anti-tuberculous regimen with rifampicin, isoniazid and ethambutol for 2 months, then isoniazid and rifampicin combination for 10 months with good clinical and radiological evolution.
Discussion
The Bacillus Calmette Guerin (BCG) is a mycobacterium (Mycobacterium bovis) attenuated by successive passages on a culture medium. Besides its use as a vaccine for Tuberculosis, the BCG intravesical instillation is the reference treatment of high and intermediate risk superficial bladder cancer [2,3]. However, this treatment is not devoid of local or systemic complications such as flu-like symptoms, liver and lung granulomatosis, lesions of the gastrointestinal tract (ulcerative terminal ileitis and Crohn-like disease), lesions of the genito-urinary tract (prostatitis), bone lesions (osteomyelitis) and joint lesions [4-7]. Mycobacterium bovis infectious complications can be observed after intravesical BCG therapy or intradermal vaccination [1]. Arthritis after intravesical BCG therapy in literature is rare; only eight cases were reported [1]. The pathophysiologic mechanism is not yet well understood, but it seems that the granulomatous infection and systemic manifestations related to infection with BCG involve both direct infection and hypersensitivity reactions.
The positivity of mycobacterium cultures of samples take late after the BCG treatment is very evocative of a spread of the infection [8]. Several factors are involved in the mechanism of blood-borne dissemination of the musculoskeletal Mycobacterium bovis infection: bladder trauma, including recent endoscopic resection, cystitis and repeated instillations [9].
The time between instillations and systemic manifestations varies widely, from days to several years. The early symptoms usually concern lungs, liver, and joints [9]. The musculoskeletal Mycobacterium bovis infection typically affects a single joint, and preferentially the bearing big ones such as hips and knees, as is the case of our patient. After the responsible instillation, infection usually occurs later than aseptic bone and joint complications [1]. It typically achieves a subacute or chronic arthritis, moving towards the gradual worsening in several weeks or months. Pain, swelling, stiffness and functional impairment are the usual signs. General symptoms are inconstant, usually of moderate importance, and combine variably asthenia, anorexia, weight loss, night sweats and low-grade fever.
The blood tests such as ESR and CRP have little diagnostic value. The skin tuberculin test is of little interest. Radiologically, the association of demineralization, bone cysts and joint space narrowing is an evocative triad.
Ultrasound allows diagnosis of joint effusion and guides diagnostic punctures. CT is more sensitive than radiographs to search for small erosions or bone sequesters.
MRI is the gold standard for early diagnosis of bone lesions because it identifies the incipient damage of cartilage and synovium [10]. In the majority of cases, the diagnosis of coxitis is made at a late stage (stage III or IV X-ray).
At a very late stage; we can see a hip dislocation and acetabular protrusion. However, imaging is never pathognomonic and histological and/or bacteriological confirmation remains indispensable. In front of a monoarthritis after intravesical instillation, the differential diagnosis arises with pyogenic germs infections with reactive arthritis.
Before discussing the diagnosis of reactive arthritis-which usually responds to NSAIDs- Mycobacterium bovis septic arthritis should be formally eliminated by joint aspiration [11]. It is essential to clearly distinguish between strains of M. Bovis from those of M. Tuberculosis to make the difference between a BCG reaction and M. Tuberculosis infection. Extra-pulmonary locations of mycobacteria are pauci bacillary and culture remains the reference method in the diagnosis and determination of antibiotic susceptibility of isolates. Colonies of M. Bovis have a 3-6 weeks slow growth on Lowenstein- Jensen solid medium.
They appear flat, small (1 to 2 mm), smooth, white and shiny. The Polymerase Chain Reaction (PCR) new diagnostic methods allows the rapid highlighting of Mycobacterium in an average of 48-72 hours, and quickly identify the different species in the Mycobacterium Tuberculosis complex [12,13]. In our case, the identification of M. Bovis was performed after culture on Lowenstein- Jensen solid medium and phenotypic study.
Bone and joint infections complicating BCG therapy should be treated with rifampicin, isoniazid and ethambutol for two months, followed by rifampicin and isoniazid for ten more months [1]. Pyrazinamide should not be used because all M. Bovis strains are resistant to it. The evolution and articular prognosis is generally favorable in the forms treated early.
The effectiveness of these medical treatments significantly reduced surgical indications. To reduce the risk of spread through blood, it is now recommended not to practice the first BCG instillation sooner than two to three weeks after transurethral bladder resection or biopsy.
Conclusion
Bone and joint infections and hypersensitivity reactions secondary to intravesical BCG therapy are rare, but well recognized. These complications can sometimes occur months or years after completion of treatment. In front of any suspicion of mycobacterial osteoarticular infection, appropriate therapeutic measures must be taken without delay to prevent adverse developments and the occurrence of sequelae.
References
-
Clavel G, Grados F, Lefauveau P, Fardellone P (2006) Osteoarticular side effects of BCG therapy. Joint Bone Spine 73: 24-28.
-
Brosman SA (1992) Bacillus Calmette-Guérin immunotherapy. Techniques and results. Urol Clin North Am 19: 557-564.
-
Lugosi L (1992) Theoretical and methodological aspects of BCG vaccine from the discovery of Calmette and Guérin to molecular biology. A review. Tuber Lung Dis 73: 252-261.
-
Satgé D, Pommepuy I, Hassan T, Goburdhun J, Flejou JF (2002) Ulcerative terminal ileitis after BCG therapy for bladder carcinoma. Histopathology 41: 266-268.
-
Pizzi M, Albertoni L, Stefanizzi L, Mescoli C, Rugge M (2015) Gastrointestinal Crohn-like disease following BCG therapy. Int J Colorectal Dis.
-
Suzuki T, Takeuchi M, Naiki T, Kawai N, Kohri K, et al. (2013) MRI findings of granulomatous prostatitis developing after intravesical Bacillus Calmette-Guérin therapy. Clin Radiol 68: 595-599.
-
Gharehdaghi M, Hassani M, Ghodsi E, Khooei A, Moayedpour A1 (2015) Bacille Calmette-Guérin Osteomyelitis. Arch Bone Jt Surg 3: 291-295.
-
Elkabani M, Greene JN, Vincent AL, VanHook S, Sandin RL (2000) Disseminated Mycobacterium bovis after intravesicular bacillus Calmette Guerin treatments forbladder cancer. Cancer Control 7: 476-481.
-
Raffray L, Riviere P, Bonnet H, Duffau P, Longy-Boursier M (2015) Granulomatous hepatitis revealing a Mycobacterium bovis widespread infection following intravesical BCG therapy. Rev Med Int 36: 626-630.
-
De Vuyst D, Vanhoenacker F, Gielen J, Bernaerts A, De Schepper AM (2003) Imaging features of musculoskeletal tuberculosis. Eur Radiol 13: 1809-1819.
-
Miranda S, Vernet M, Héron F, Vittecoq O, Levesque H, et al. (2010) Acute reactive arthritis after intravesical instillation of bacillus Calmette-Guérin. Two case reports and literature review. Rev Med Int 31: 558-561.
-
Ninet B, Roux-Lombard P, Schrenzel J, Janssens JP (2011) [New tests for the diagnosis of tuberculosis]. Rev Mal Respir 28: 823-833.
-
Talbot EA, Williams DL, Frothingham R (1997) PCR identification of Mycobacterium bovis BCG. J Clin Microbiol 35: 566-569.





