Clinical Medical
Reviews and Case Reports
Massive Urinothorax; A Rare Complication after Percutaneous Nephrolithotomy
Ibrahim Halil Bozkurt, Salih Polat*, Ismail Gulden, Serkan Yarimoglu, Ozgu Aydogdu, Tarik Yonguc and Volkan Sen
Bozyaka Training and Research Hospital, Izmir, Turkey
*Corresponding author: Salih Polat, MD, Bozyaka Training and Research Hospital, Izmir, Turkey, Tel: +90 54 322 93 29, Fax: +90 232 26 44 44, E-mail: salihpolat@gmail.com
Clin Med Rev Case Rep, CMRCR-2-080, (Volume 2, Issue 12), Case Report; ISSN: 2378-3656
Received: December 05, 2015 | Accepted: December 19, 2015 | Published: December 22, 2015
Citation: Bozkurt IH, Polat S, Gulden I, Yarimoglu S, Aydogdu O, et al. (2015) Massive Urinothorax; A Rare Complication after Percutaneous Nephrolithotomy. Clin Med Rev Case Rep 2:080. 10.23937/2378-3656/1410080
Copyright: © 2015 Bozkurt IH, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The urinothorax or collection of urine in the pleural space is a rare complication following percutaneous nephrolithotomy (PCNL). We present a case of massive urinothorax who had undergone PCNL. Two weeks after PCNL, the patient was admitted to the emergency clinic with dyspnea, chest pain and fever. Thorax and abdomen computed tomography (CT) revealed massive pleural effusion on the left hemithorax and a stone located at the proximal segment of left ureter. A chest tube and a ureteral DJ stent was placed for drainage. In conclusion, the patients who underwent PCNL via intercostal access and had residual stones should be closely followed-up for signs and symptoms of urinothorax.
Keywords
Urinothorax, Percutaneous nephrolithotomy, Supracostal access, Pleural effusion
Introduction
Percutaneous nephrolithotomy (PCNL) has been the preferred surgical technique for the treatment of renal stones for many years [1]. Selection of percutaneous access point varies according to the placement of stones in pelvicalyceal system. Subcostal access is preferred mostly for PCNL to avoid possible injury to the lungs and pleura. Supracostal access may be required in patients with upper caliceal stones and staghorn stones for complete stone removal [2]. Pleural injury during percutaneous access may lead to complications including hydrothorax, pneumothorax, hydropneumothorax and urinothorax [3]. Urinothorax, the presence of urine in the pleural space, is a rare complication following PCNL [1].
We report a 45-year-old man who developed massive urinothorax two weeks after PCNL performed for left renal stones. In this case report, ethical approval was not required. Written informed consent was obtained from the patient.
Case Report
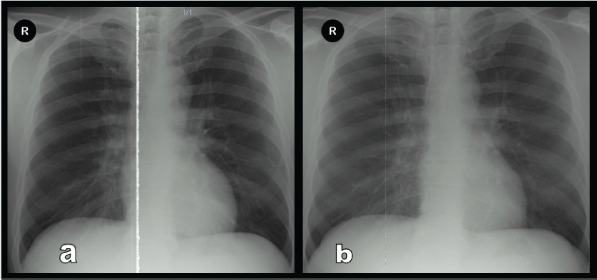
The patient underwent left PCNL at our clinic. Supracostal access was done between the 11th and 12th left ribs. 16-30 French Amplatz dilator was used for tract dilatation. There was no suspicion of complication during the PCNL. Oxygen saturation and peak airway pressure were within normal limits during operation. There was no residual fragments in fluoroscopy images at the end of the procedure. Extravasation and/or pleural leakage was not seen in pyelogram that was obtained after nephrostomy placement. We perform routine chest X-ray imaging at preoperative [Figure 1a] and postoperative day 1 (POD 1) in patients who had undergone PCNL using intercostal access. The control chest X-ray of this patient at POD 1 was normal [Figure 1b]. The nephrostomy tube was removed at POD 2. Postoperative course of the patient was uneventful without any complaints like dyspnea, chest pain or fever. The patient was discharged on the second postoperative day.
.
Figure 1: Pre-operatif Chest X-ray (a), postoperative day-1 Chest X-ray (b) showing no left pleural effusion.
View Figure 1
Two weeks later the patient admitted to emergency department with dyspnea, chest pain and fever which have developed in one day following acute left flank pain. On clinical examination, the patient was alert and tachypneic with a respiratory rate of 20 per minute and was febrile with 38.8°C, pulmonary auscultation showed no breath sounds in lower two thirds of the left hemithorax. Oxygen saturation was 84 percent.
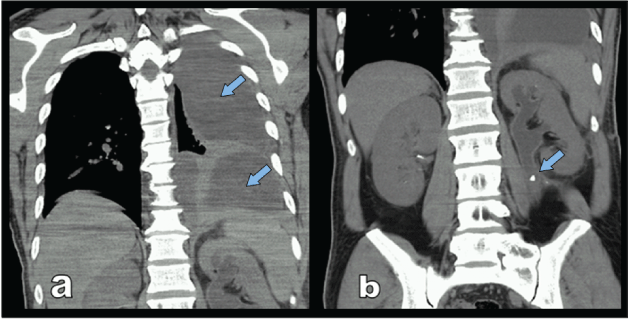
The chest radiograph showed massive pleural effusion on the left side and urinary ultrasound revealed grade 2 hydronephrosis of left kidney. Thorax CT confirmed the massive pleural effusion [Figure 2a]. Abdominal CT revealed a stone located at the proximal segment of left ureter [Figure 2b]. The diagnosis confirmed by demonstration of the pleural fluid that was found to be a transudate by thoracentesis with a pleural fluid creatinine of 19 mg/dl compared to a serum creatinine level of 1.2 mg/dl, and a pleural fluid LDH of 42 U/L compared to a serum LDH of 230 U/L, and a pleural fluid glucose of 76 mg/dl compared to a serum glucose level of 92 mg/dl. Pleural fluid-serum creatinine ratio was 15.8 (19/1,2)
.
Figure 2: Thorax CT showing that massive left pleural effusion (a) (arrow) and abdominal CT showing that stone located in the proximal ureter (b) (arrow).
View Figure 2
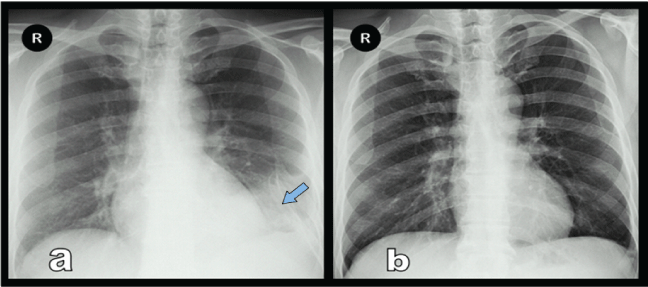
A chest tube was inserted and a ureteral DJ stent was placed for drainage. Repeated chest radiographs showed that minimal residual pleural effusion [Figure 3a]. The chest tube was removed on the fourth day and patient was discharged with oral antibiotic. The residual ureteral stone was treated with SWL and DJ stent was removed after four week. At 1st month visit the patient was asymptomatic and the chest X-ray was normal [Figure 3b].
.
Figure 3: Chest X-ray with minimal residual pleural effusion at the time of discharge (a) (arrow), Chest X-ray at 1st month visit (b).
View Figure 3
Discussion
Urinothorax that is a rare cause of pleural effusion is defined as accumulation of urine in pleural space. The reported etiologies of urinothorax in the literature are percutaneous nephrolithotomy, percutaneous nephrostomy, extracorporeal shock wave lithotripsy, renal biopsy, renal transplantation, blunt trauma to kidney, bladder laceration and retroperitoneal inflammatory fibrosis [4].
Eleven cases that reported after PCNL have been reported in the literature [4,5]. Overall complication rates after PCNL have been reported as %23.3 and thoracic complication rates have been reported as 0-11.6% [1]. Thoracic complications including pneumothorax, hydrothorax, hemothorax, and urinothorax were reported with a rate of 16% for supracostal versus 4.5% for subcostal access [6]. In the same study, complication rates in patients who underwent supra-11th rib and supra-12th rib access were %35 and %10, respectively. Lallas and colleagues reported that urinothorax never occurred with subcostal access but did complicate 2.3% of superior access to the 12th rib and 6.3% of superior access to the 11th rib [7].
In our case, urinothorax occurred as result of pleural injury due to supra-12th upper pole percutaneous access during PCNL. The patient who was expected to be spontaneously heal, was complicated with massive urinothorax due to an acute ureteral obstruction caused by a residual fragment. Our case is different from the previous reports because there was no signs of pleural injury intraoperatively and postoperatively. There was no pleural effusion on postoperative day-1 chest x-ray. In a study, 10.7% of the patients who underwent PNL had pleural effusion detected by CT scan and only 3.6% of patients were symptomatic [8]. Additionally, Ogan et al evaluated 104 patients who underwent supracostal and infracostal access; pleural effusion detection rate via CT were 45% and 29%, respectively [9].
Chest radiograph and thoracic CT imaging is the preferred imaging modality in the detection of pleural effusions and of underlying cause. However thoracentesis should be performed to confirm the diagnosis of urinothorax, and three parameters in pleural fluid should be evaluated: transudative pleural fluid, pleural fluid-serum creatinine ratio greater than 1.0 and low pleural fluid pH [10].
In conclusion, patients who underwent PCNL via intercostal access and had residual stones should be closely followed-up for signs and symptoms of urinothorax. The treatment of urinothorax includes drainage of urine from pleural space and relief of ureteral obstruction with a DJ stent or nephrostomy tube.
References
-
Seitz C, Desai M, Hacker A, Hakenberg OW, Liatsikos E, et al. (2012) Incidence, prevention, and management of complications following percutaneous nephrolitholapaxy. Eur Urol 61: 146-158.
-
Shaban A, Kodera A, El Ghoneimy MN, Orban TZ, Mursi K, et al. (2008) Safety and efficacy of supracostal access in percutaneous renal surgery. J Endourol 22: 29-34.
-
Gupta R, Kumar A, Kapoor R, Srivastava A, Mandhani A (2002) Prospective evaluation of safety and efficacy of the supracostal approach for percutaneous nephrolithotomy. BJU Int 90: 809-813.
-
Handa A, Agarwal R, Aggarwal AN (2007) Urinothorax: an unusual cause of pleural effusion. Singapore Med J 48: e289-292.
-
Shleyfer E, Nevzorov R, Jotkowitz AB, Novack V, Avnon L, et al. (2006) Urinothorax: An unexpected cause of pleural effusion. Eur J Intern Med 17: 300-302.
-
Munver R, Delvecchio FC, Newman GE, Preminger GM (2001) Critical analysis of supracostal access for percutaneous renal surgery. J Urol 166: 1242-1246.
-
Lallas CD, Delvecchio FC, Evans BR, Silverstein AD, Preminger GM, et al. (2004) Management of nephropleural fistula after supracostal percutaneous nephrolithotomy. Urology 64: 241-245.
-
Yadav R, Gupta NP, Gamanagatti S, Yadav P, Kumar R, et al. (2008) Supra-twelfth supracostal access: when and where to puncture? J Endourol 22: 1209-1212.
-
Ogan K, Corwin TS, Smith T, Watumull LM, Mullican MA, et al. (2003) Sensitivity of chest fluoroscopy compared with chest CT and chest radiography for diagnosing hydropneumothorax in association with percutaneous nephrostolithotomy. Urology 62: 988-992.
-
Stark DD, Shanes JG, Baron RL, Koch DD (1982) Biochemical features of urinothorax. Arch Intern Med 142: 1509-1511.





