Clinical Medical
Reviews and Case Reports
Chronic Stimulant Use: An Upcoming Cause of Neurocognitive Disorder in Later Life?
Anne Jacobs1,2*, Sonja C. Stalpers-Konijnenburg1,3, Cornelis A. de Jong3 and Radboud M. Marijnissen1
1Department of Old Age Psychiatry, Pro Persona, Arnhem/Wolfheze, the Netherlands
2Department of Geriatrics, Rijnstate Hospital, Arnhem, the Netherlands
3Department Nijmegen Institute for Scientist-Practitioners in Addiction (NISPA), Radboud University, Nijmegen, the Netherlands
*Corresponding author: Anne Jacobs, MD, Department of Old Age Psychiatry, Pro Persona, Arnhem/Wolfheze, the Netherlands, Tel: 0031653763593, E-mail: jacobs.anne@gmail.com
Clin Med Rev Case Rep, CMRCR-3-086, (Volume 3, Issue 1), Case Report; ISSN: 2378-3656
Received: December 09, 2015 | Accepted: January 23, 2016 | Published: January 26, 2016
Citation: Jacobs A, Stalpers-Konijnenburg SC, de Jong CA, Marijnissen RM (2016) Chronic Stimulant Use: An Upcoming Cause of Neurocognitive Disorder in Later Life?. Clin Med Rev Case Rep 3:086. 10.23937/2378-3656/1410086
Copyright: © 2016 Jacobs A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and
reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: Alert for chronic stimulant use as an etiological factor of a major neurocognitive disorder.
Methods: Single-case study.
Results: A 58-year-old woman, with a history of chronic daily stimulant use, was diagnosed with a major neurocognitive disorder with behavioral problems.
Conclusion: This case highlights the possibility of chronic daily stimulant use resulting in a major neurocognitive disorder. Since the prevalence of long-lasting illicit stimulant use among older adults is rising, we suggest considering this as a possible etiological factor of neurocognitive disorders.
Keywords
Aging, Cognitive disorders, Substance use
Introduction
The prevalence of illicit substance use among older adults is rising [1], partly as a consequence of the aging of the baby boom generation (born between 1946 and 1964), as within this cohort, drug use during youth has been found to be significantly higher compared to earlier cohorts [2]. It is likely this will be accompanied by greater risks to the older adult, because of age-related changes in drug metabolism and neurotransmitter systems mediating drug effects in the brain [3]. Furthermore, the prevalence of long-term effects of substance use might increase, such as cognitive disorders. Long-term substance use, particularly of cocaine, has frequently been associated with cognitive deficits [4]. These deficits may be the result of several pathophysiological mechanisms. For example, cocaine and amphetamine use have been associated with a higher prevalence of stroke [5,6] due to compromised cerebral blood flow caused by hypertensive surges, vasospasms, enhanced platelet aggregation, cerebral vasculitis, accelerated atherosclerosis and cardio-embolism [7,8]. Additionally, it has been suggested that chronic cocaine abuse may suppress normal brain maturation in adults [9], mainly of the frontal and temporal lobes, which could be accompanied by cognitive deterioration. It has also been reported that cocaine-dependent subjects have lower gray matter volume than healthy subjects [10]. Finally, cognitive disturbance might be the result of acute toxic leukoencephalopathy due to cocaine abuse [11,12], most likely caused by adulterants [13]. Toxic leukoencephalopathy is characterized by progressive damage to myelin and other white matter in the brain and is often accompanied by severe neurological symptoms.
Most studies on cognitive changes due to chronic stimulant use have a short follow-up time [14]. To our knowledge, permanent cognitive disorders due to chronic stimulant use have not yet been described in the literature. A major neurocognitive disorder (NCD), according to the newest edition of the Diagnostic and Statistical Manual of Mental Disorders (DMS-5), is an acquired cognitive decline in one or more cognitive domains which interfere significantly with a person's everyday independence [15]. Here we describe a case of NCD most likely caused by chronic stimulant use.
Case Report
A 58-year-old woman was admitted to a psychiatric ward because of a psychotic episode. Psychiatric history revealed chronic daily stimulant use for more than thirty years, specifically cocaine, amphetamine and nicotine. She also suffered from a psychotic episode at the age of 23 after the death of a child. Medical history did not report any somatic comorbidities.
The patient worked in prostitution and had been always able to take care of herself and her daughter. Over the past two years, her daughter noticed progressive memory problems and behavioral changes with self-neglect in the patient. A few months before admission her mother started to live more isolated than previously and even barricaded her house. She did not trust anybody and she seemed to hallucinate. There were also some episodes of aggression towards neighbors. Finally, the daughter informed us that her mother had said some time ago that she would stop taking drugs as a new grandchild had been born. So if she was suffering from withdrawal symptoms, it most likely would have been occurring in the weeks before admission.
Upon admission, we saw a small White woman (158 cm; 44.5 kg; Body Masss Index 17.8). Physical and neurological examinations did not reveal any abnormalities; however a psychiatric examination indicated paranoid delusions and auditory hallucinations. All routine haematological and biochemical tests (including complete blood count, electrolytes, vitamins, glucose, thyroid, kidney and liver function tests) were normal. Urinary drugs screening for cocaine, amphetamine and tetrahydrocannabinol were negative.
The patient was admitted to an adult psychiatric ward and psychotic symptoms were successfully treated with risperidone 4mg once daily. After the symptoms subsided, it was possible to reduce the antipsychotic treatment gradually. Psychotic symptoms did not relapse and risperidone treatment was stopped completely.
Subsequently, however, severe memory impairment and problems with planning and organization became apparent. Upon further psychiatric assessment, the patient was cooperative, although it was hard to make real contact. She was wearing clothes more typically worn by younger women. She displayed rapid psychomotor activity and was talkative with rapid speech. There were no abnormalities in consciousness and the attention of the patient could be drawn easily but it was hard to keep her attention on any particular subject. Some hypervigilance was observed, as she reacted to every stimulus. The patient was disorientated. There were evident disturbances in both short- and long-term memory, as well as confabulations. Frequent repetitive behavior and perseverations in speech were observed, such as continuously asking “When will I go to another city?”. Her thought processes were also affected, with flight of ideas seen, and mainly relating to smoking and moving to another city. Delusions or hallucinations were not observed. Insight and judgment were impaired. Mood and affect were normal. Additional examination by means of a comprehensive neuropsychological investigation was performed. To measure intelligence, the Wechsler Adult Intelligence Scale (WAIS) was undertaken. To interpret the scores, we made use of the systematic assessment by Kaufman and Lichtenberger [16]. Total intelligence level and intelligence on the three sublevels were assessed as low. To test her ability and speed to process information, a digit symbol substitution test and a symbol search test were carried out and the patient scored very low on both. Additionally, all scores on several cognitive tests were also low (clock drawing, trail making, 15 words memory, fluency, Stroop and Porteus Maze tests). On the Mini Mental State Examination [17] she scored 22 out of 30. All memory tests were performed chaotically by the patient. Consequently, some of the tests could not even be rated. In summary, the neuropsychological tests undertaken showed deficits in memory, attention, executive functions, information processing speed and visuospatial ability.
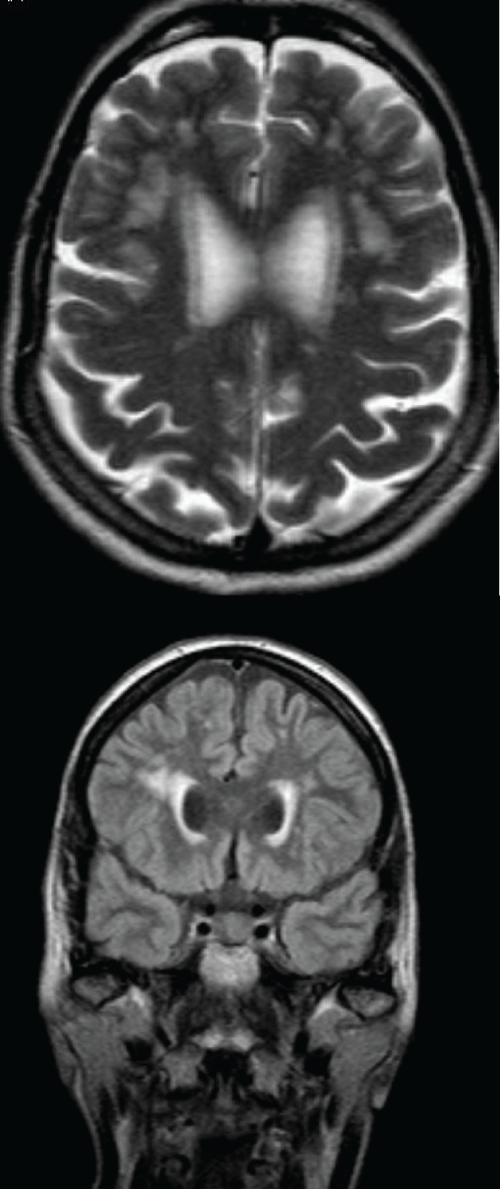
To investigate the underlying etiology of the established cognitive impairment, further assessments were performed. Cerebral Magnetic Resonance Imaging (MRI) showed confluent subcortical and periventricular white matter lesions (Fazekas 3) and dilated ventricles (Figure 1). Carotid ultrasound imaging did not show signs of atherosclerosis. Serology for borreliosis, syphilis, hepatitis, HIV and paraneoplastic antibodies did not reveal any abnormalities.
.
Figure 1: Magnetic Resonance Imaging (MRI) of the cerebrum showed strong confluent subcortical and periventricular white matter lesions (Fazekas 3; MTA 1).
View Figure 1
What could have caused the psychotic episode and what could be the underlying pathophysiological mechanism of the subsequently-observed cognitive impairment?
Discussion
This patient with a history of chronic daily stimulant use first presented with psychotic symptoms. Most likely the psychotic episode was induced by substance use, since this is a prevalent precipitator of psychosis [18], or by an abrupt cessation of substance use, resulting in withdrawal. It seemed likely that patient had been using until recently because her daughter found drugs lying around the house. However, the negative urinary drugs screening test could support the hypothesis of withdrawal as the cause of psychotic symptoms. In any case we could state there was vulnerability for psychosis, given the history of one psychotic episode. Although less likely, we could also consider the psychotic symptoms as neuropsychiatric symptoms emanating from a neurocognitive disorder, since cognitive impairment was already observed before the psychosis emerged.
After the psychotic symptoms were treated, severe cognitive impairment with behavioral problems persisted. Given the results of the neuropsychological investigations and combined with her decreased independence in daily life, a major neurocognitive disorder with behavioral problems was diagnosed.
Based on the clinical presentation and the additional diagnostic tests, several etiological subtypes could be excluded, including infections and Parkinson’s or Lewy Body’s disease. Due to the early onset of cognitive deterioration, with no family history of dementia and the absence of hippocampal and cortical atrophy, Alzheimer’s disease was deemed unlikely. A vascular or frontotemporal neurocognitive disorder was considered, the latter because of the observed behavioral disinhibition and perseverative behavior. However, neuropsychological investigation showed more global cognitive impairment and not exclusively frontotemporal features. Additionally, there was no frontal or temporal lobe involvement on neuroimaging. Most likely, the cognitive disorder could be attributed to the white matter lesions found by the cerebral MRI. Given no large vessel disease was found by the ultrasound scan, these lesions are most likely the result of microvascular disease due to the effect of cocaine and amphetamine on cerebral blood flow [7,8]. Possible causes of white matter abnormalities and cognitive impairment in substance use are stroke and toxic leukoencephalopathy. However, both disorders are most often accompanied by severe neurological symptoms. Therefore, we concluded these diagnoses were unlikely, since our patient did not have any aberrant neurological manifestations. Moreover, the damage from stroke as detected by an MRI scan is more localized than the damage seen in our patient. Cocaine use has, however, also been associated with the appearance of a more confluent pattern of white matter signal hyperintensities without neurological symptoms [19,20].
Therefore, we concluded that this major neurocognitive disorder with behavioral problems most likely had a vascular etiology as a consequence of chronic stimulant use, DSM-5 code 292.82 [15]. Giving the rising prevalence of illicit stimulant use among older adults [1], it is possible this condition might occur more often in the future. More attention should be paid to this upcoming cause of neurocognitive disorder. Older adults presenting with cognitive impairment should be asked about chronic stimulant use. In case of substance use we advise referral to a specialist for neurocognitive testing and cerebral imaging.
References
-
Wu LT, Blazer DG (2014) Substance use disorders and psychiatric comorbidity in mid and later life: a review. Int J Epidemiol 43: 304-317.
-
Johnson RA, Gerstein DR (1998) Initiation of use of alcohol, cigarettes, marijuana, cocaine, and other substances in US birth cohorts since 1919. Am J Public Health 88: 27-33.
-
Dowling GJ, Weiss SR, Condon TP (2008) Drugs of abuse and the aging brain. Neuropsychopharmacology 33: 209-218.
-
Spronk DB, van Wel JH, Ramaekers JG, Verkes RJ (2013) Characterizing the cognitive effects of cocaine: a comprehensive review. Neurosci Biobehav Rev 37: 1838-1859.
-
Sordo L, Indave BI, Barrio G, Degenhardt L, de la Fuente L5, et al. (2014) Cocaine use and risk of stroke: a systematic review. Drug Alcohol Depend 142: 1-13.
-
Fonseca AC, Ferro JM (2013) Drug abuse and stroke. Curr Neurol Neurosci Rep 13: 325.
-
Esse K, Fossati-Bellani M, Traylor A, Martin-Schild S (2011) Epidemic of illicit drug use, mechanisms of action/addiction and stroke as a health hazard. Brain Behav 1: 44-54.
-
Siniscalchi A, Bonci A, Mercuri NB, De Siena A, De Sarro G, et al. (2015) Cocaine dependence and stroke: pathogenesis and management. Curr Neurovasc Res 12: 163-172.
-
Bartzokis G, Beckson M, Lu PH, Edwards N, Bridge P, et al. (2002) Brain maturation may be arrested in chronic cocaine addicts. Biol Psychiatry 51: 605-611.
-
Sim ME, Lyoo IK, Streeter CC, Covell J, Sarid-Segal O, et al. (2007) Cerebellar gray matter volume correlates with duration of cocaine use in cocaine-dependent subjects. Neuropsychopharmacology 32: 2229-2237.
-
González-Duarte A, Williams R (2013) Cocaine-induced recurrent leukoencephalopathy. Neuroradiol J 26: 511-513.
-
Bianco F, Iacovelli E, Tinelli E, Lepre C, Pauri F (2011) Recurrent leukoencephalopathy in a cocaine abuser. Neurotoxicology 32: 410-412.
-
Blanc PD, Chin C, Lynch KL (2012) Multifocal inflammatory leukoencephalopathy associated with cocaine abuse: is levamisole responsible? Clin Toxicol (Phila) 50: 534-535.
-
Vonmoos M, Hulka LM, Preller KH, Minder F, Baumgartner MR, et al. (2014) Cognitive impairment in cocaine users is drug-induced but partially reversible: evidence from a longitudinal study. Neuropsychopharmacology 39: 2200-2210.
-
(2013) Diagnostic and Statistical Manual of Mental Disorders. (5th edn), American Psychiatric Association.
-
Kaufman AS, Lichtenberger EO, McLean JE (2001) Two- and three-factor solutions of the WAIS-III. Assessment 8: 267-280.
-
Folstein MF, Folstein SE, McHugh PR (1975) "Mini-mental state". A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12: 189-198.
-
Gururajan A, Manning EE, Klug M, van den Buuse M (2012) Drugs of abuse and increased risk of psychosis development. Aust N Z J Psychiatry 46: 1120-1135.
-
Lyoo IK, Streeter CC, Ahn KH, Lee HK, Pollack MH, et al. (2004) White matter hyperintensities in subjects with cocaine and opiate dependence and healthy comparison subjects. Psychiatry Res 131: 135-145.
-
Bartzokis G, Goldstein IB, Hance DB, Beckson M, Shapiro D, et al. (1999) The incidence of T2-weighted MR imaging signal abnormalities in the brain of cocaine-dependent patients is age-related and region-specific. AJNR Am J Neuroradiol 20: 1628-1635.





