Clinical Medical
Reviews and Case Reports
Aeroportia - A Rare Finding for a Frequent Disease
Marta Pereira1*, Luís Miguel Afonso1, Sofia Patrão2 and Rui Araújo3
1Internal Medicine Junior Doctor, Internal Medicine Residency Program, Portugal
2Oncology Junior Doctor, Hospital Pedro Hispano, Matosinhos, Portugal
3Intensive Medicine Consultant, Director of the Intensive Care Unit, Hospital Pedro Hispano, Matosinhos, Portugal
*Corresponding author: Marta Pereira, Internal Medicine Junior Doctor, Internal Medicine Residency Program, Portugal, E-mail: martabarpereira@gmail.com
Clin Med Rev Case Rep, CMRCR-3-089, (Volume 3, Issue 2), Case Report; ISSN: 2378-3656
Received: January 12, 2016 | Accepted: February 10, 2016 | Published: February 13, 2016
Citation: Pereira M, Afonso LM, Patrão S, Araújo R (2016) Aeroportia - A Rare Finding for a Frequent Disease. Clin Med Rev Case Rep 3:089. 10.23937/2378-3656/1410089
Copyright: © 2016 Pereira M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Case Report
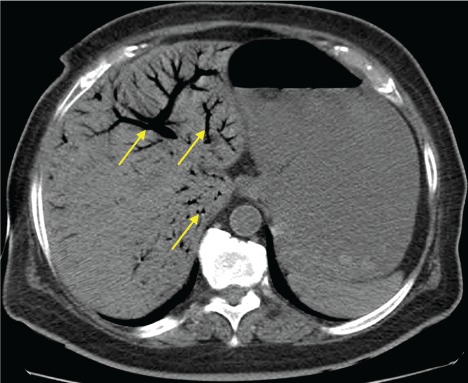
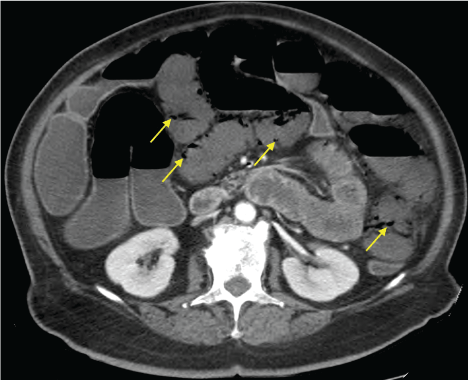
A 69-year-old female was admitted to our hospital with complaints of abdominal pain and diarrhea for the last 2 weeks. She was obese, diabetic, and had peripheral arterial disease, but no history of bowel disease or previous gastrointestinal symptoms. Physical examination revealed severe dehydration, hypotension, and diffuse abdominal discomfort. Acute kidney injury with anuria and significant leukocytosis were documented. Furthermore, the patient had severe lactic acidosis. The clinical presentation was suggestive of severe abdominal sepsis. Abdominal ultrasound was difficult to perform due to the marked obesity of the patient. Initial imaging study with abdominal x-ray showed no signs of bowel occlusion and, the main diagnostic hypothesis that remained at this time included abdominal sepsis and bowel ischemia, with hypovolemia and her history of diabetes and arterial disease being important risk factors supporting the latter diagnosis. Aggressive resuscitation and empirical antibiotics were started but the patient continued to show signs of deterioration. Abdominal CT scans showed branching pattern of gas lucencies in the hepatic portal venous system (Figure 1) and pneumatosis intestinalis (Figure 2) with vascular patency. No pneumoperitoneum was noted. In this context, these findings were suggestive of bowel ischemia, possibly due to hypovolemia and hypoperfusion. As this was the main hypothesis and one with an important mortality, the patient was submitted to an emergent exploratory laparotomy. Bowel ischemia was confirmed and extensive resection of necrotic small bowel was executed, after which she started to improve. Surgery for restoration of bowel continuity was successfully performed 3 weeks later.
Portomesenteric venous gas and pneumatosis intestinalis are uncommon but very important radiographic findings. They are two distinct entities, not pathognomonic of bowel infarction when separate, but when combined they are strongly associated with bowel ischemia. Nonetheless, some non-ischemic conditions have been described associated with these imaging findings (such as inflammatory bowel disease) [1]. The mechanisms involved are not yet clear but the mucosal damage appears to allow the passage of air from the intestine to the venous system. Some authors suggest that the presence of anaerobic bacteria also leads to the production of larger amounts of gas contributing to this presentation [2].
Patients with mesenteric ischemia, usually have multiple comorbidities that make this a very challenging diagnosis. Abdominal computed tomography is a useful exam in these cases, allowing early detection of subtle portomesenteric venous gas and pneumatosis intestinalis. Bowel ischemia has poor prognosis, with very high mortality rate (up to 75%, according to some authors [2]), and requires an early diagnosis and immediate surgical intervention.
Learning Points
The rare association between pneumatosis intestinalis and the presence portomesenteric venous gas (termed aeroportia) is a strong indicator of bowel ischemia [1-5], an urgent life-threatening vascular condition with a high mortality rate1. Early diagnosis and treatment are the keys to saving a patient’s life [3].
References
-
Pinto Pais T, Pinho R, Carvalho J (2014) Hepatic portal venous gas and intestinal pneumatosis as initial presentation of Crohn's disease: first case report. J Crohns Colitis 8: 1329-1330.
-
Seak CJ, Hsu KH, Wong YC, Ng CJ, Yen DH, et al. (2014) The prognostic factors of adult patients with hepatic portal venous gas in the ED. Am J Emerg Med 32: 972-975.
-
Milone M, Di Minno MN, Musella M, Maietta P, Iaccarino V, et al. (2013) Computed tomography findings of pneumatosis and portomesenteric venous gas in acute bowel ischemia. World J Gastroenterol 19: 6579-6584.
-
Sivrioglu AK, Incedayi M, Saglam M, Sonmez G (2013) Portomesenteric venous gas and pneumatosis intestinalis due to intestinal ischaemia. BMJ Case Rep 2013.
-
Hsin HT, Hwang JJ, Lo HJ (2006) Severe aeroportia in a patient with acute myocardial infarction complicated by acute ischaemic bowel syndrome. Heart 92: 1040.