Clinical Medical
Reviews and Case Reports
Spontaneous Spleen Rupture: An Unusual Involvement of the Spleen in Systemic Lupus Erythematosus
Maria do Socorro Teixeira Moreira Almeida*, Amanda Gualberto Carvalho, Lina Gomes dos Santos, Eliton Carlos Batista de Sousa and Gabriela Lustosa Said
Department of Medical Clinic, Federal University of Piaui, Piaui, Brazil
*Corresponding author: Maria do Socorro Teixeira Moreira Almeida, Adjunct Professor of Rheumatology, Department of Medical Clinic, Federal University of Piaui, Universitary Hospital, Campus Ministro Petrônio Portella, Teresina, Piaui, Brazil, E-mail: smoreira@ufpi.edu.br
Clin Med Rev Case Rep, CMRCR-3-096, (Volume 3, Issue 3), Case Report; ISSN: 2378-3656
Received: February 20, 2016 | Accepted: March 12, 2016 | Published: March 14, 2016
Citation: Almeida MSTM, Carvalho AG, dos Santos LG, de Sousa ECB, Said GL (2016) Spontaneous Spleen Rupture: An Unusual Involvement of the Spleen in Systemic Lupus Erythematosus. Clin Med Rev Case Rep 3:096. 10.23937/2378-3656/1410096
Copyright: © 2016 Almeida MSTM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The involvement of the reticuloendothelial system in systemic lupus erythematosus (SLE) concomitant to the disease activity is highly variable, and well-recognised but spontaneous splenic rupture is an unusual occurrence.
We report a 35-year-old woman with SLE who had spontaneous splenic rupture during the course of her illness. The spleen rupture was evident on histophatological analysis. A brief review of spontaneous splenic rupture in systemic lupus erythematosus (SLE) is also presented.
Knowledge of this condition allows the identification of risk factors and the patients characteristics with this rare disease; and can help in early diagnosis and proper treatment.
Keywords
Systemic lupus erythematosus, Spontaneous spleen rupture
Introduction
A traumatic rupture of the spleen has been described in the medical literature as a clinical oddity with grave consequences, if unrecognized and untreated [1]. Clinical features of splenic rupture include pain, tenderness and muscle guarding in the left upper quadrant of the abdomen along with features of hamorrhagic shock [2]. In the absence of a history of trauma, other clinical diagnoses may be found on presentation, most commonly perforated peptic ulcer [3].
The spleen can rupture after trauma or spontaneously to a normal or diseased spleen [4]. The spontaneous rupture of the spleen, which occurs suddenly or insidiously, was first described by Aktinson [5], and is a rare complication of infectious, haematological, neoplasic and rheumatic disorders, like SLE [6].
The clinical spectrum of patients with SLE is highly variable [7]. The involvement of the reticuloendothelial system is a well-recognized concomitant of the disease. However, it is usually mild, its course is independent of other disease manifestations, and it is not useful as a little use as a prognosis marker [8]. Spontaneous non-traumatic rupture is extremely rare and has been associated as an unusual event in patients with SLE and so far, only six cases have been reported in the literature [5,9-13]. Since in these cases there is no history of trauma, the diagnosis is often missed ou delayed.
We report a 35-year-old woman with SLE who had spontaneous splenic rupture during the course of her illness and present a brief review of spontaneous splenic rupture in SLE.
Case Report
A 35-year-old female patient presented in 2008 at the age of 31 with severe pericardial effusion, bilateral pleural effusion, ascites and polyarthralgia. At presentation, she had diagnostic criteria for SLE, according to the criteria of the American College of Rheumatology (ACR) [14]. Her laboratory tests revealed blood urea nitrogen of 87 mg/dL (normal 4-15 mg/dL), a creatinine level of 3.1 mg/dL (normal 0.6-1.3 mg/dL), 136 mEq/L of sodium, and a 5.3 mEq/L of potassium. Her complete cell blood count revelead lymphopenia (830/mm3), a platelet count of 591,000/mm3 (normal 150,000 - 400,000/ul) and anemia (hematocrit = 26% - normal 45%), without reticulocytosis and with a negative indirect Coombs test. The urinalysis revealed albuminuria (3+) and a 24-hour urine collection demonstrated 304 mg proteins. Furthermore she had a positive ANA (1:640), anti-dsDNA antibodies (75 UI/mL) with positivity to anti SSA, SSB and Histone.
Considering the multisystemic involvement of the diseease, she was treated with bolus therapy with three daily pulses of methylprednisolone at a dose of 1,000 mg/day, followed by 0.5 mg/kg/day prednisolone. At the time, ultrasonography showed no changes in the spleen or liver. The disease has been controlled gradually and the patient closely monitored, using 5 mg/day prednisolone, 5 mg enalapril daily and hydroxychloroquine, with no further signs of disease activity.
Four years later, in April 2012, she was re-admitted to our hospital complaining of dyspnea, left upper abdominal quadrant pain, diarrhea, fever for ten days, and painful left cervical lymphadenopathy, with no history of trauma. On physical examination, she presented symptoms compatible with systemic inflammatory response syndrome (SIRS) - her temperature was 38°C, cardiac rate of 120 bpm, and respiratory rate of 38/min. She also had joint pains, generalized maculo-papular rash for one week ad jaudice. Her abdomen was tense, tender with guarding to palpation and particularly painful in the left hypochondrium. The spleen was palpable, but its size could not be determined because of the presence of extreme abdominal tenderness and guarding.
Laboratory admission data included: white blood cells of 9.0 × 103/mm3 (normal 4000-11000/mm3) with segments 84.0%, band forms 10.0%, lymphocytes 5.0%, a platelet count of 50,000/uL (normal 150,000-400,000/uL), anemia (hematocrit = 23% - normal 45%), with no reticulocytosis. Indirect Coombs test was negative, total bilirubin level of 2.9 mg/dL (normal 0.2-1.3 mg/dL), indirect bilirubin of 1.8 mg/dL (normal 0.2-0.8 mg/dL), erythrocyte sedimentation rate (ESR) of 50 mm/h (normal westgreen 0-20 mm/h), electrolytes within normal limits and normal liver and kidney function. Urine, blood and stool culture were negative and serologic tests for cytomegalovirus (CMV), Epstein-Barr virus (EBV), human herpes virus type I (HHV-1) and hepatits were negatives, as well as anti cardiolipin and serum anti phospholipid antibodies.
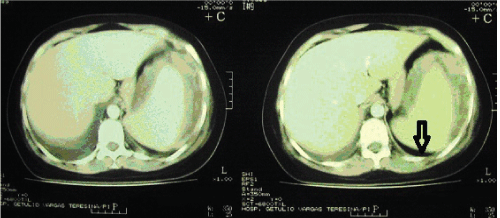
Abdominal ultrasound revealed the presence of subcapsular collection in the spleen and enlarged left ovary (5.0 × 7.0 cm). An abdominal computed tomography with contrast showed no evidence of gallbladder stones or abnormality of the liver, but revelead a left subphrenic collection with dense fluid in close contact with the spleen measuring 9.0 cm in diameter and also the presence of bilateral pleural effusions associated with subsegmental parenchymal consolidations (Figure 1).
.
Figure 1: Abdominal computed tomography with contrast showing a left subphrenic collection with dense fluid in close contact with the spleen.
View Figure 1
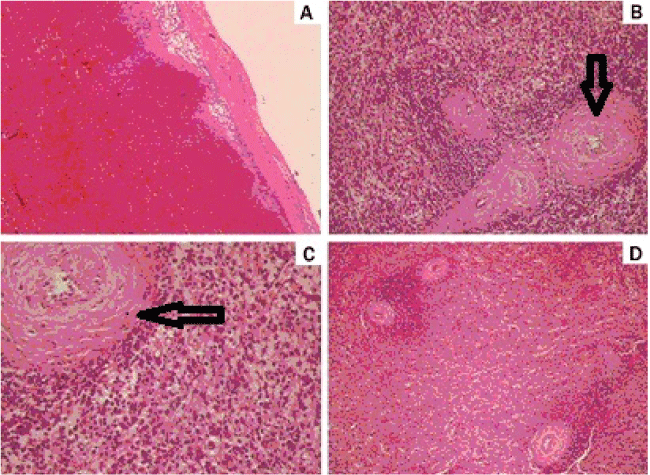
A laparotomy was performed and the exploration confirmed hemoperitoneum secondary to ruptured spleen with subcapsular hematoma. Splenectomy and a left oophorectomy were performed. Grossly, the spleen was 566 g, 140 × 100 × 70 mm. Its surface was lobulated, with lacerations. Microscopic examination (Figure 2) revealed splenic follicle atrophy, with an onionskin appearance of the splenic central artery and histiocytes proliferated. There was no significant vascular lesion.
.
Figure 2: H & E staining of the ruptured spleen. (A) Organized subcapsular hematoma (X40); (B) Onionskin appearance of the splenic central artery (X100); (C) Histiocytes proliferated (X200); (D) Splenic follicle atrophy (X40).
View Figure 2
She was admitted to the intensive care unit for post-operative care where she remained for three days. Jaundice was attributed to infectous process and it disappeared after surgery and the patient had clinical improvement being discharged home after 15 days of admission without symptoms.
Her follow-up care after discharge was performed regularly ar the hospital clinic and routine blood and urine tests, ESR, liver and kidney functions remained normal.
Three years after the event, the disease remains stable and the patient is currently taking 400 mg/day of hydroxychloroquine and 5 mg/day of prednisone to control her articular symptoms. The autoantibodies are still present in her serum.
Discussion
Splenic rupture in the absence of trauma, called spontaneous splenic rupture, is a rare complication of infectious, haematological and neoplastic disorders. Causes of atraumatic splenic rupture can be divided into six main categories: infectious, neoplastic, inflammatory, congenital or structural, iatrogenic and finally idiopathic. It complicates about 0.2% of cases of infectious mononucleosis. Others conditions reported in the paediatric age group include severe meningococcal septicaemia, congenital afibringenemia and malaria. An increased risk for pathologic splenic ruptures has also been reported in patients with systemic vasculitis, and several rheumatic conditions [5].
SLE is a multisystem disease and its clinical manifestations vary according to the organs involved [5].
The immune system functions are closely linked to the spleen. Involvement of the reticuloendothelial system in SLE is a well-recognized and can present with lymphadenopathy and splenomegaly, abscesses, abnormal spleen function, histological abnormalities, capsulitis, infarction, and spontaneous rupture [15]. Its reported frequency varies widely, from 9% to 46% [16]. However spontaneous spleen rupture is an extremely rare complication [6]. We found only six cases of this affection reported in the literature [5,9-13]. There are no case reports of SLE with splenic rupture in in the Brazilian literature. For unknown reasons, spontaneous and traumatic rupture of the spleen has male predominance as described in literature [17].
In most of these cases, the spleen rupture had been established close to the onset of SLE, but our patient only had this affection four years after her diagnosis corroborating the findings of other studies [6]. It is also noteworthy that the histopathological findings in analysis of the spleen can guide the etiological diagnosis of the rupture. The typical histological feature of splenic involvement in SLE is the onionskin lesion of periarterial fibrosis. Other pathological features include capsulitis and small infarcts, which are presumably secondary to arterial thrombosis, observed in association with the presence of a raised titer of anti-cardiolipin antibodies [15], not identified in this case. In agreement with previous reports, the microscopic examination revealed splenic follicle atrophy, onionskin appearance of the splenic central artery and histiocytes proliferated with no significant vascular lesion.
By virtue of the unusual nature of this disorder, its etiology has been the subject of considerable speculation and several hypotheses have been put forward to explain its origin. Barnard et al. (1990) suggested that spleens that ruptured were predisposed to the event due to some, yet unidentified, immunological stimulation [18]. Li et al. [19] described the case of a woman of 54 years old with a spontaneous spleen rupture and compared her spleen pathologic study with a control patient, with same sex and age, but with a ruptured spleen due to trauma. Differently than traumatic lesion, the patient with ruptured spleen and SLE had marked congestion of the red pulp and atrophy of white pulp. Congestion of red pulp may be the cause of spontaneous splenic rupture (SSR) in the SLE spleen.
Because of its rare occurrence, the clinical and pathophysiologic factors that may predispose the spleen to spontaneous rupture have not been defined [6]. It continues to pose a diagnostic challenge and dilemma in management [1]. Then, knowledge of this condition allows the identification of risk factors and the patients characteristics with this rare disease. The survival of these patients seems to be uncertain and an early diagnosis may be the only way to a proper and effective treatment improving survival.
We conclude that spontaneous organ rupture should be included in the differential diagnosis of acute abdomen pain in patients with SLE. Since SSR is quite rare, in case patients with abdominal pain, which locates mainly at upper quadrant, this entity should be suspected. Checking the hemoglobin level is also a simple and convenient measure.
Ethics Committee and Consent
The protocol for the research project has been approved by a suitably constituted Ethics Committee of the institution within which the work was undertaken and that it conforms to the provisions of the World Medical Association's Declaration of Helsinki. Written informed consent has been obtained from the patient for publication of this case report and any accompanying images.
References
-
Hyun BH, Varga CF, Rubin RJ (1972) Spontaneous and pathologic rupture of the spleen. Arch Surg 104: 652-657.
-
Jahadi MR, Bailey W, Crenshaw A (1975) Atraumatic splenic rupture simulating ruptured sigmoid diverticulitis: report of a case and review of the literature. Dis Colon Rectum 18: 59-61.
-
Orloff MJ, Peskin GW (1958) Spontaneous rupture of the normal spleen; a surgical enigma. Int Abstr Surg 106: 1-11.
-
Nicoll JA (1968) Splenic haematoma after spontaneous rupture of the spleen. Am J Surg 116: 117-119.
-
Han J, Li N, Wang JY, Zhou J, Zhand J (2012) Life-threatening spontaneous splenic rupture with sistemic lupus erythematosus: case report and literature rview. Clin Rheumatol 31: 1019-1025.
-
Debnath D, Valerio D (2002) Atraumatic rupture of the spleen in adults. J R Coll Surg Edinb 47: 437-445.
-
Tan EM, Cohen AS, Fries JF, Masi AT, McShane DJ, et al. (1982) The 1982 revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 25: 1271-1277.
-
Milder MS, Aptekar RG, Larson SM, Decker JL, Johnston GS (1974) Letter: Spleen size in SLE. Arthritis Rheum 17: 190-191.
-
Zimmermann-Gorska I, Bielska K (1971) [Splenic rupture in the course of systemic lupus erythematosis]. Pol Tyg Lek 26: 1991-1992.
-
Krauser RE (1976) Spontaneous rupture of the spleen in systemic lupus erythematosus. JAMA 236: 1149.
-
Wu CC, Lan JL, Liu TJ (1985) [Systemic lupus erythematosus with spontaneous rupture of the spleen--a case report]. Taiwan Yi Xue Hui Za Zhi 84: 1186-1190.
-
Tolaymat A, Al-Mousily F, Haafiz AB, Lammert N, Afshari S (1995) Spontaneous rupture of the spleen in a patient with systemic lupus erythematosus. J Rheumatol 22: 2344-2345.
-
Karassa FB, Isenberg DA (2001) Spontaneous rupture of the spleen: an unusual complication of systemic lupus erythematosus. Lupus 10: 876-878.
-
Hochberg MC (1997) Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 40: 1725.
-
Fishman D, Isenberg DA (1997) Splenic involvement in rheumatic diseases. Semin Arthritis Rheum 27: 141-155.
-
Quismorio FP (1993) Hemic and lymphatic abnormalities in SLE. In: Wallace D, Hahn B, Dubois' Lupus Erythematosus. Lea and Febiger, Philadelphia, PA, 418-430.
-
Nadri QJ, Alfurayh O (2010) Spontaneous rupture of the spleen: a rare complication in a patient with lupus nephritis on hemodialysis. Saudi J Kidney Dis Transpl 21: 712-714.
-
Barnard H, Dreef EJ, van Krieken JH (1990) The ruptured spleen. A histological, morphometrical and immunohistochemical study. Histol Histopathol 5: 299-304.
-
Li N, Wang JC, Zhu MH, Wang JY, Fu XL, et al. (2013) Pathologic diagnosis of spontaneous splenic rupture in systemic lupus erythematosus. Int J Clin Exp Pathol 6: 273-280.





