Clinical Medical
Reviews and Case Reports
Giant Mucinous Cystadenoma of the Ovary Mimicking Ascites: A Case Report
Marco Rossato1*, Marta Burei2 and Roberto Vettor1
1Department of Medicine - DIMED, Clinica Medica 3, University of Padova, Padova, Italy
2Radiotherapy and Nuclear Medicine Unit, Veneto Institute of Oncology, IRCCS Padova, Italy
*Corresponding author: Marco Rossato, MD, PhD, Department of Medicine - DIMED, University of Padova, Clinica Medica 3, Via Giustiniani, 235128 Padova, Italy, Tel: +39-049-8218747, Fax: +39-049-8213332, E-mail: marco.rossato@unipd.it
Clin Med Rev Case Rep, CMRCR-3-103, (Volume 3, Issue 4), Case Report; ISSN: 2378-3656
Received: April 06, 2016 | Accepted: April 28, 2016 | Published: April 30, 2016
Citation: Rossato M, Burei M, Vettor R (2016) Giant Mucinous Cystadenoma of the Ovary Mimicking Ascites: A Case Report. Clin Med Rev Case Rep 3:103. 10.23937/2378-3656/1410103
Copyright: © 2016 Rossato M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
In the present case report we describe a 67 years old woman with clinically apparent ascites and no systemic causes for it and a giant mucinous cystadenoma of the right ovary diagnosed utilizing the CT scan and confirmed by the histological findings.
Keywords
Ascites, Mucinous cystadenoma, Ovary
Introduction
Ascites consists in the accumulation of fluid within the peritoneal cavity and is a common finding with a wide range of causes [1]. Although at least 80% of patients with ascites are found to have liver cirrhosis other pathologies as well as heart failure, peritonitis, nephrotic syndrome, peritoneal neoplasms have also to be considered.
Clinical manifestations of ascites range from complete absence of symptoms to severely distended abdomen with respiratory distress, pyrosis, abdominal pain, nausea, anorexia. On physical examination the flanks are bulged, and a fluid wave can be apparent together with a shifting dullness. Umbilical herniation may further confirm the presence of ascites. Among the different causes of ascites not associated with liver and peritoneal diseases, it is known that ovarian pathologies may determine it although this symptom is not specific and ascites due to ovarian malignant pathology (i.e. ovarian cancer due to metastasization to the peritoneal cavity) may suggest the existence of a disease of the abdominal organs since patients report abdominal fullness, dyspepsia, early satiety [2].
Here we describe a woman presenting with a giant cystic neoplasm of the ovary mimicking ascites.
Report of the Case
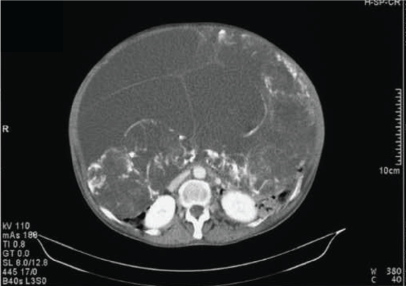
We have recently evaluated a 67 years old woman referred to our hospital for ascites. Her clinical history was negative. She referred a slow progressive increase of the abdominal circumference over the past 4-5 years. On arrival at our hospital the patient showed slight dyspnea, normal arterial pressure and pulse. On physical examination we observed bilateral elevation of pulmonary inferior margins, no signs of cardiocirculatory failure nor peripheral oedema, a remarkable ascites with eversion of the umbilicus. No venous reticula, fullness in the flanks, fluid thrill, defense reaction nor shifting dullness were present. Splanchnic organs were not palpable, the bowel sounds were muffled. Laboratory investigations were normal with normal liver and kidney function tests, normal albumin plasma concentration and normal plasma ion concentrations. Also plasma osmolarity was in the normal range. The alpha-fetoprotein plasma levels were normal as were other tumoral markers investigated (CA-125, CEA, hCG, CA 19-9). The urine analysis was normal. Chest X-ray did not show any remarkable finding. On abdominal ultrasound examination performed on site upon arrival at the emergency care unit, the liver appeared normal with the description of important ascites. An abdominal CT scan was then performed. The liver, gallbladder, intrahepatic biliary tree, common bile duct, spleen, pancreas, kidneys, large vessels and bladder were all normal. The uterus was homogeneous and hypotrophic. A giant intraperitoneal cystic mass measuring 28.5 × 17.8 × 46.2 cm (with a calculated volume of about 12 liters) was visualized originating from the right ovary with numerous septa displacing the colon, the stomach and pushing up the liver and the spleen with no compression of other abdominal organs (Figure 1). There was no free fluid in the abdomen and no sign of infiltration. The patient underwent the surgical removal of the ovarian mass that was diagnosed by the pathologist as a giant mucinous cystadenoma of the ovary.
.
Figure 1: CT scan of the abdomen showing a multiseptated mass originating from the right ovary and occupying the whole abdomen.
View Figure 1
Discussion
Among the different causes of ascites, liver cirrhosis is the most common one but there are many other causes [1]. Furthermore different abdominal lesions, out of giant ovary cystadenomas, may mimic ascites such as giant renal cyst [3], giant mesenteric cyst [4], pelvic echinococcosis [5], peritoneal mesothelioma [6], and pelvic tuberculosis [7]. Aspiration of the abdominal fluid evaluates its physico-chemical characteristics, the cellular composition, and the presence of malignant cells and can help to relieve abdominal distension, splanchnic organ displacement and compression. In the presence of abdominal cystic masses of unknown origin the aspiration of fluid is to be avoided since it might produce clinical complications due to cyst perforation or possible dissemination of malignant cells in the case the mass was a cancer as previously described [8]. For this reason we did not perform any aspiration of the abdominal fluid in our patient before investigating the precise nature of ascites. The cystic mass detected in our patient originated from the right ovary. The slow growth velocity of the mass, its homogeneous content, the absence of inner vegetations, the normality of all tumoral markers investigated (CA-125, CEA, hCG, CA 19-9, alpha-fetoprotein) suggested its possible benign nature. Indeed the histological analysis diagnosed a giant mucinous cystadenoma. It is very difficult to estimate the actual incidence of giant mucinous cystadenomas of the ovary in post-menopausal women since previous published data in the literature are scarce, probably because of the fact that they are now diagnosed at earlier stages and before their development as huge intra-abdominal masses. A literature search using the Medline database through PubMed (www.ncbi.nlm.nih.gov/pubmed) considering all published papers with at least the presence in the title and/or in the abstract of the terms giant, mucinous cystadenoma, ovary, returned only 3 reports of giant mucinous cystadenoma of the ovary in post-menopausal women while twelve papers were present for pre-menopausal women, mainly adolescent women (Table 1). In a previous study in pre-menopausal women, the incidence of mucinous cystadenomas of the ovary was established to be about 0.3% of subjects with ovarian tumours [9]. The histopathological classification of mucinous cystadenoma of the ovary involves three types: mucinous cystadenoma (accounting for 70% of cases), borderline mucinous cystadenoma (accounting for 10% of cases) and malignant mucinous carcinoma (accounting for 20% of cases) [9]. Ovarian mucinous cystadenomas are usually unilateral and develop as multilocular large masses full of mucinous fluid as in the present case report.
![]()
Table 1: Clinical features of the case reports present in the literature of giant mucinous cystadenoma of the ovary.
View Table 1
The clinical symptoms are usually due to the progressive increase of abdominal circumference and pressure, non specific diffuse abdominal pain, nausea, vomiting and other symptoms related to splanchnic organs compression. Physical examination usually shows abdominal distension mimicking ascites. Routine laboratory investigations are not of help in case of mucinous cystadenoma of the ovary unless functional ovarian epithelium is present thus possibly leading to elevation of plasma levels of tumours markers such as CA 125 and CA 19-9, although this is not always true [9]. On the contrary, laboratory investigations could be of help in the diagnosis of other causes of ascites such as liver cirrhosis. Ultrasound and CT scan of the abdomen are fundamental for the differential diagnosis, tumour size and extension.
The surgical removal of the mass is the only therapeutic option in case of giant mucinous cystadenoma of the ovary because of symptoms due to mass effect and the above-mentioned risk of malignancy. After surgical removal, the follow up consists in abdominal morphological examination with ultrasound and CT scan together with the analysis of tumour markers if elevated preoperatively. The clinical prognosis of ovarian giant mucinous cystadenomas is usually good since the malignant transformation occurs in less than 10% of cases [9].
In conclusion ovarian neoplasms presenting with very large cystic masses can be mislead with ascites and in these cases morphological examination using ultrasound and CT scan appears fundamental to evaluate their precise origin and relationships with the other abdominal organs.
References
-
Bender (2004) Diseases of the peritoneum. In: Goldman L, Ausiello D, Cecil Textbook of Medicine. (22nd edn), Pa: Saunders, Philadelphia, 941-943.
-
Cannistra SA (2004) Cancer of the ovary. N Engl J Med 351: 2519-2529.
-
Viganò P, Picozzi SC, Casu M, Manganini V, Giuberti A, et al. (2007) Giant renal cyst complicated with acquired crossed renal ectopia, hypertension and renal cell carcinoma: case report and review of the literature. Arch Ital Urol Androl 79: 151-154.
-
Zamir D, Yuchtman M, Amar M, Shoemo U, Weiner P (1996) Giant mesenteric cyst mimicking ascites. Harefuah 130: 683-684, 727.
-
Ertas IE, Gungorduk K, Ozdemir A, Emirdar V, Gokcu M, et al. (2014) Pelvic tuberculosis, echinococcosis, and actinomycosis: great imitators of ovarian cancer. Aust N Z J Obstet Gynaecol 54: 166-171.
-
Liu Q, Zhang Q, Guan Q, Xu JF, Shi QL (2014) Abdominopelvic tuberculosis mimicking advanced ovarian cancer and pelvic inflammatory disease: a series of 28 female cases. Arch Gynecol Obstet 289: 623-629.
-
Dulger C, Adali E, Avcu S, Kurdoglu Z (2010) Large mesenteric cyst mimicking tuberculous ascites. Case Rep Med 2010: 725050.
-
Jones DR, Vasilakis A, Pillai L, Timberlake GA (1992) Giant, benign, mucinous cystadenoma of the ovary: case study and literature review. Am Surg 58: 400-403.
-
Cevik M, Guldur ME (2013) An extra-large ovarian mucinous cystadenoma in a premenarchal girl and a review of the literature. J Pediatr Adolesc Gynecol 26: 22-26.
-
Mehboob M, Naz S, Zubair M, Kasi MA (2014) Giant ovarian cyst--an unusual finding. J Ayub Med Coll Abbottabad 26: 244-245.
-
Olesen H, Eisum AK (2001) Recurrent mucineous cystadenoma in an 11-year-old premenarchal girl. Ugeskr Laeger 163: 6601-6602.
-
Yazici M, Etensel B, Gursoy H, Erkus M (2002) Mucinous cystadenoma: a rare abdominal mass in childhood. Eur J Pediatr Surg 12: 330-332.
-
Flotho C, Rückauer K, Duffner U, Bergstässer E, Böhm N, et al. (2001) Mucinous cystadenoma of the ovary in a 15-year-old girl. J Pediatr Surg 36: E6.
-
Vizza E, Galati GM, Corrado G, Atlante M, Infante C, et al. (2005) Voluminous mucinous cystadenoma of the ovary in a 13-year-old girl. J Pediatr Adolesc Gynecol 18: 419-422.
-
Grapsa D, Kairi-Vassilatou E, Hasiakos D, Kondi-Pafiti A (2006) Ovarian mucinous cystadenoma with extended calcification in an 11-year-old girl: case report and review of the literature. Clin Exp Obstet Gynecol 33: 181-182.
-
Karaman A, Azili MN, Boduroglu EC, Karaman I, Erdogan D, et al. (2008) A huge ovarian mucinous cystadenoma in a 14-year-old premenarchal girl: review on ovarian mucinous tumor in premenarchal girls. J Pediatr Adolesc Gynecol 21: 41-44.
-
Willems RP, Slangen B, Busari JO (2012) Abdominal swelling in two teenage girls: two case reports of massive ovarian tumours in puberty. BMJ Case Rep 2012.
-
Gorgone S, Minniti C, Ilaqua A, Barbuscia M (2008) Giant mucinous cystadenoma in a young patient. A case report. G Chir 29: 42-44.
-
Lefebvre B, Philippart P, Brandelet B, Mendes da Costa P (2000) Giant cystadenoma of the ovary in an adolescent: clinical case and review of the literature. Rev Med Brux 21: 157-159.
-
Sri Paran T, Mortell A, Devaney D, Pinter A, Puri P (2006) Mucinous cystadenoma of the ovary in perimenarchal girls. Pediatr Surg Int 22: 224-227.
-
Zanini P, Cavalca A, Benatti E, Drei B (1996) Benign giant ovarian cystadenoma. Description of a clinical case. Minerva Ginecol 48: 215-219.





