Clinical Medical
Reviews and Case Reports
The Biliary Sinus: A Rare Late-Stage Complication of Cholecystectomy
Ihsan Yıldız*, Yavuz Savaş Koca and İbrahim Barut
Department of General Surgery, Hepatobiliary Surgery Unit, Suleyman Demirel University School of Medicine, Isparta, Turkey
*Corresponding author: İhsan Yıldız, Department of General Surgery, Hepatobiliary Surgery Unit, Suleyman Demirel University School of Medicine, 32100 Isparta, Turkey, Tel: +90-246-2119248, Fax: +90-246-2112830, E-mail: drihsanyildiz@gmail.com
Clin Med Rev Case Rep, CMRCR-3-109, (Volume 3, Issue 6), Case Report; ISSN: 2378-3656
Received: April 29, 2016 | Accepted: June 01, 2016 | Published: June 03, 2016
Citation: Yıldız I, Koca YS, Barut I (2016) The Biliary Sinus: A Rare Late-Stage Complication of Cholecystectomy. Clin Med Rev Case Rep 3:109. 10.23937/2378-3656/1410109
Copyright: © 2016 Yıldız I, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: The complications of cholecystectomy still remain a serious challenge for the surgeons. These complications may occur within several days, weeks, months, or years after the surgery. For the diagnosis of these complications such as biliary sinus or fistulas, percutaneous radiopaque imaging is more appropriate.
Case report: A 53-year-old female patient who had undergone open cholecystectomy due to cholelithiasis 6 years earlier was admitted to hepatobiliary surgery unit with a painful mass in the right upper quadrant and fever. Ultrasonography showed that a 3-cm fluid-filled mass in the right upper quadrant subcutaneously, in computed tomography a fluid-filled tubular lesion extending from the right lobe of liver to right upper quadrant, and percutaneous cholangiography showed that a radio-opaque density communicating with the liver. The biliary sinus tract was totally excised. The patient was uneventfully discharged on day 6 after the surgery. Histopathological examination of the lesion was reported as a bile sinus.
Conclusion: The sinus tract with communication of the intrahepatic biliary tree can be diagnosed by using percutaneous radiopaque imaging and surgical excision may be required if the sinus tract becomes fibrotic and infected. In conclusion, biliary sinus should be kept in mind in patients with recurrent symptom after cholecystectomy.
Keywords
Cholecystectomy, Cholecystectomy complications, Biliary tract surgery
Background
Since open cholecystectomy was performed the complications have been remaining a serious challenge for the surgeons, and severe complications often require surgical intervention. These interventions are performed by surgeons experienced in hepatobiliary surgery through multidisciplinary approaches [1,2].
Common complications after cholecystectomy and biliary tract surgeries include biliary leakage caused by bile duct injury, incomplete cholecystectomy, biloma, and biliary leakage from the drain and the T-tube tract. These complications may occur within several days, weeks, months, or years after the surgery. Ultrasonography (USG), computed tomography (CT), magnetic resonance cholangiopancreatography (MRCP), and endoscopy are commonly used, however the presence of biliary sinus or fistula, percutaneous radiopaque imaging is more proper for the diagnosis [3-5].
In this report, we present a case with biliary sinus that extending from the liver to the abdominal wall subcutaneously, which is a rare and late-stage complication of cholecystectomy.
Case Report
The 53-year-old female patient had undergone open cholecystectomy due to cholelithiasis 6 years earlier was admitted to our hepatobiliary surgery unit with the complaints of weakness, a painful mass in the right upper quadrant, fever, nausea, and vomiting. Anamnesis revealed that the patient had been hospitalized and undergone medical treatment with antibiotics and analgesics for three times due to a recurrent pain in the right upper quadrant. Physical examination revealed that a 3-cm painful subcutaneous mass.
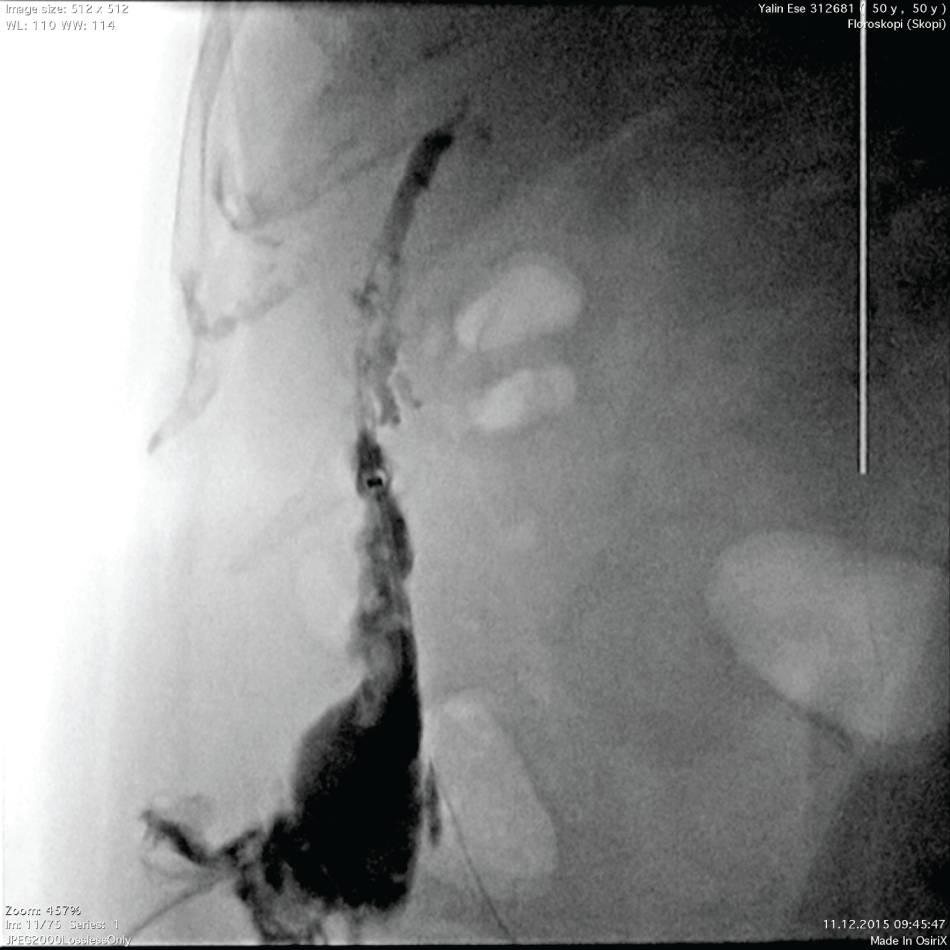
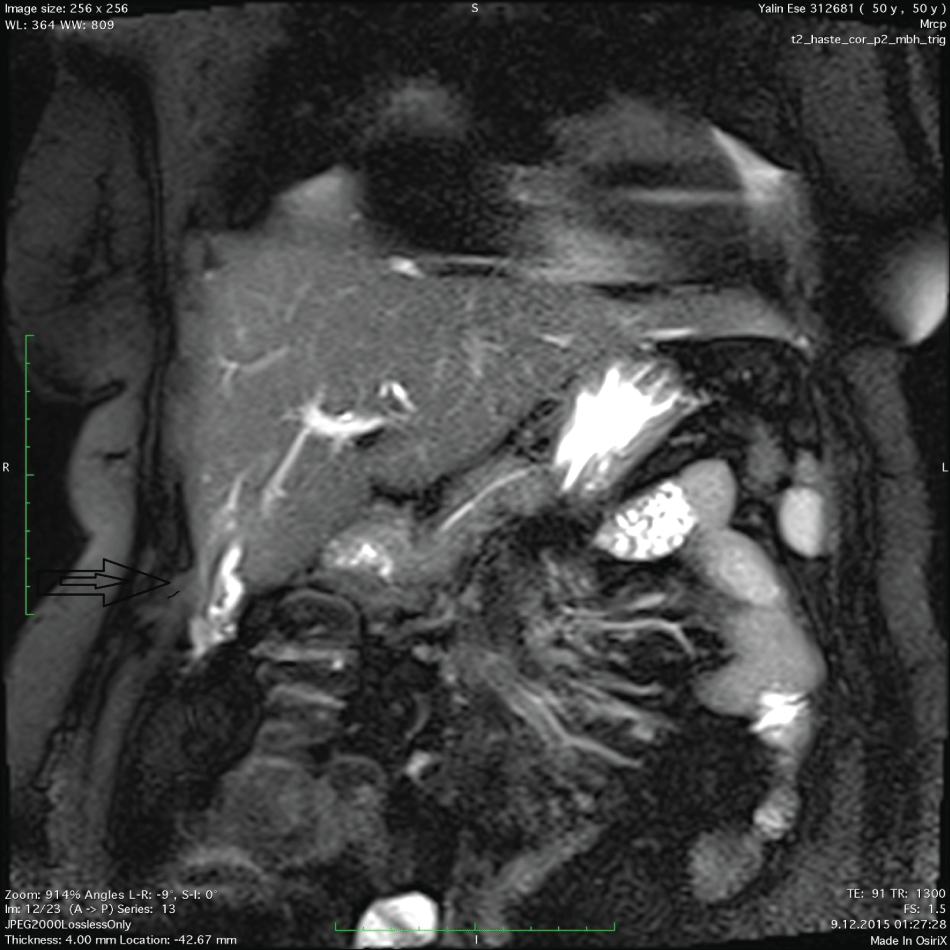
Laboratory parameters were as follows: leukocyte 12000/mcl (4000-10000), AST 80 (5-40 U/L), ALT 70 (7-56 U/L), amylase 100 U/L (60-180 U/L), crp 3(0-0.5), ALP 76 (25-100), no hyperbilirubinemia and GGT 34 (10-44 mg/dl). USG showed a 3 cm fluid-filled lesion extending from the right lobe of liver to the right upper quadrant. Computed tomography also viewed a radio-opaque, fluid-filled tubular structure under the skin, extending from the right lobe of the liver to subcutane right upper quadrant (Figure 1). Percutaneous cholangiography showed a radio-opaque density from the right upper quadrant and reaching to the 4th Segment of the right lobe of the liver (Figure 2). MRCP showed a lesion communicating with intrahepatic biliary tree (Figure 3).
Surgical technique
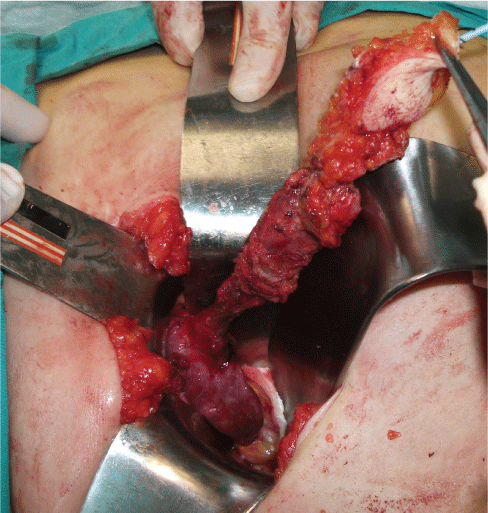
Under general anesthesia, a circular incision was made including the entire lesion and a plastic drain (No. 8 one feeding tube) was placed in the sinus tract. The tract was dissected to the 4th segment of the right lobe of the liver by passing through all the abdominal wall layers, without impairing the integrity of the tract. The communication of the tract with the liver was viewed and ligated and then the biliary sinus was totally excised (Figure 1). A soft drain was placed surgical site. No postoperative complication occurred, the drain was removed on day 3 after the surgery and the patient was uneventfully discharged on sixth postoperative day. Histopathological examination of the lesion was reported as a epithelialized biliary sinus tract and there was no carcinoma.
Discussion
Cholecystectomy is a commonly performed surgical procedure and thus often leads to complications. These complications may occur in the early stage or may be associated with the removal of the drain or the T-tube in the late stage of the surgical procedure [2]. Of these, biliary leakage into the peritoneal cavity and external biliary drainage from the T-tube tract are the most common complications. While external biliary drainage closes spontaneously, the biliary leakage into the peritoneal cavity requires invasive methods such as surgery or percutaneous drainage with interventional radiology [6,7].
T-tube tracts may often close spontaneously but sometimes it remains as a biliary sinus in such casesan interventional radiology may be sufficient for drainage. However, if the sinus communicates with the intrahepatic biliary tree, it may become infected and thus lead to cholangitis [5,6]. In these circumstances surgery is required. The late-stage complications of the biliary tract surgery commonly occur after the liver resections performed due to cancer.
Our case had undergone cholecystectomy six years before, but had no history of liver resection or biliary tract surgery; no drain or T-tube placement and no presence of liver parenchymal injury or a missed bile duct injury was suspected in this case during the surgical procedure. And this condition has not been reported before. However we thought that an accessory bile duct such as Luschka might be injured in this patient.
The decision of surgery was made based on the patient had undergone medical treatment with antibiotics and analgesics several times due to recurrent fever, abdominal pain, nausea and vomiting after cholecystectomy and the detection of a communication between the biliary sinus tract and the biliary tree in the liver.
A plastic drain (No. 8, one feeding) was inserted in sinus tract to avoid the impairment of the integrity of the sinus tract and to guide the progress of the surgery. The insertion of the drain facilitated the dissection procedure.
The cases which were detected with a communication between the biliary sinus tract and the biliary tree can be treated by using sphincterotomy and stent placement under the guidance of endoscopic retrograde cholangiopancreatography (ERCP). However, in our patient, surgical excision was performed since the sinus tract had become fibrotic and had formed an infected pouch under the skin.
Conclusion
As a complication after cholecystectomy the biliary sinus is in possibilities in patients with developing recurrent symptom such as abdominal pain, fever, nausea and vomiting.
Acknowledgements
The study has been previously presented on 20. Turkısh Surgery Congress/Antalya
There is no financial and other material support.
References
-
Dannenberg S, Eder F (2012) 130 Years of bile duct surgery-a short historical review of the pioneering contributions to surgery of the gallbladder and bile duct by Professors Carl Langenbuch and Hans Kehr. Zentralbl Chir 137: 16-19.
-
Parra-Membrives P, Martinez-Baena D, Marquez-Munoz M, Pino-Diaz V (2013) Does laparoscopic ap-proach impair T-tube-related sinus-tract formation? Surg Laparosc Endosc Percutan Tech 23: 55-60.
-
Chowbey PK, Goel A, Bagchi N, Sharma A, Khullar R, et al. (2006) Abdominal wall sinus: an unusual presentation of spilled gallstone. J Laparoendosc Adv Surg Tech A 16: 613-615.
-
Fork FT, Rimer U, Ekberg O, Nyman U, Zederfeldt B (1985) Post-operative lesions of the com-mon bile-duct.A cholan-giographic investigation. Acta Radiol Diagn 26: 569-575.
-
Nimura Y, Hayakawa N, Kamiya J, Kondo S, Shionoya S (1990) Hepatic segmentectomy with caudate lobe resection for bile duct carcinoma of the hepatic hilus. World J Surg 14: 535-543.
-
Schmidt SC, Langrehr JM, Hintze RE, Neuhaus P (2005) Long-term results and risk factors influencing outcome of major bile duct injuries following cholecystectomy. Br J Surg 92: 76-82.
-
Machado NO (2011) Biliary complications postlaparoscopic cholecystectomy: mechanism, preventive measures, and approach to management: A review. Diagn Ther Endosc.