Clinical Medical
Reviews and Case Reports
Primary Epiploic Appendagitis
Neha Gupta*, Tony A Abdel Maseeh, Leyden Standish-Parkin and Yekaterina Sitnitskaya
Departments of Pediatrics, Lincoln Medical Center, Bronx, NY, USA
*Corresponding author: Neha Gupta, Department of Pediatrics, Lincoln Medical Center, 234 E 149th street, Bronx, New York 10451, USA, Tel: 347-500-6980, E-mail: neha_gupta_2008@hotmail.com
Clin Med Rev Case Rep, CMRCR-3-110, (Volume 3, Issue 6), Case Report; ISSN: 2378-3656
Received: May 09, 2016 | Accepted: June 08, 2016 | Published: June 10, 2016
Citation: Gupta N, AbdelMaseeh TA, Standish-Parkin L, Sitnitskaya Y (2016) Primary Epiploic Appendagitis. Clin Med Rev Case Rep 3:110. 10.23937/2378-3656/1410110
Copyright: © 2016 Gupta N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Epiploic appendagitis is a rare diagnosis in pediatric population. It is a benign, self-limiting condition caused by infarction, torsion or thrombosis of the fatty appendages on the serosal surface of the colon. It can be a diagnostic dilemma as it can mimic acute appendicitis or diverticulitis, depending on its location. We report a case of a teenage girl who presented with right lower quadrant abdominal pain without any associated vomiting, fever, and diarrhea. Laboratory work up was non-contributory. Computed tomography of the abdomen helped in the diagnosis of epiploic appendagitis. She was successfully treated with non-steroidal anti-inflammatory medications which resulted in full recovery.
Keywords
Appendicitis, CT scan, Appendices, Omental infarction
Abbreviations
PEA: Primary Epiploic Appendagitis, RLQ: Right Lower Quadrant, CT: Computed Tomography, WBC: White Blood Count, UA: Urinalysis, LFT: Liver Function Test, CRP: C-reactive Protein, NAAT: Nucleic Acid Amplification Test, IV: Intravenous, NSAIDS: Non-Steroidal Anti-Inflammatory Drugs, US: Ultrasound
Introduction
Primary epiploic appendagitis (PEA) is a very rare cause of abdominal pain which is caused by infarction, torsion or thrombosis of the fatty appendages on the serosal surface of the colon. It can mimic acute appendicitis or diverticulitis, depending on its location. Here we present a teenager with right lower quadrant (RLQ) abdominal pain who was diagnosed with epiploic appendagitis by computed tomography (CT) scan.
Case
A 16-year-old sexually active female with a history of migraine headaches presented with 3 days of RLQ abdominal pain (7/10), improved with Ibuprofen and with no associated symptoms like anorexia, nausea, vomiting, changes in bowel or urinary habit, or vaginal discharge. Her last menstrual period started the same day as the RLQ pain.
The patient was afebrile, with heart rate 72 bpm and blood pressure 105/69 mmHg. Her Body mass index (BMI) was 24 kg/m2 (80th percentile). The abdominal exam remarkable for a soft, non-distended abdomen, with RLQ tenderness, but no guarding or rebound tenderness. Psoas and obturator signs were negative. The white blood count (WBC) count was 8.2 x 109/L. The urinalysis (UA), lipase, liver function test (LFT) and C-reactive protein (CRP) were normal. Urine culture and urine Gonorrhea and Chlamydia Nucleic Acid Amplification Test (NAAT) were negative. Pelvic Ultrasound (US) showed a 1.5 × 0.9 × 0.8 cm left ovarian cyst. CT scan of the abdomen with oral and intravenous (IV) contrast showed inflammation of the fat in the right aspect of the pelvis consistent with epiploic appendagitis; a 1.9 cm left adnexal cyst and normal appendix (Figure 1). Given the absence of fever, leukocytosis or elevated inflammatory markers, it was decided to abstain from giving antibiotics and the patient was managed supportively, with non-steroidal anti-inflammatory drugs (NSAIDS) and IV fluids. Her symptoms improved gradually over the course of one week and on day 9 she was tolerating regular diet. The patient was discharged after a 9 day inpatient stay. Patient was readmitted after 8 months with recurrence of epiploic appendagitis, and again treated supportively with NSAIDS with full resolution of symptoms in one week.
.
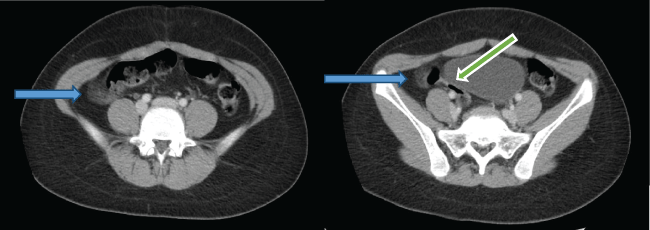
Figure 1: CT scan of the abdomen with oral and IV contrast: Inflammation of the fat in the right aspect of the pelvis (blue arrow) with normal appendix (green arrow).
View Figure 1
Discussion
Epiploic appendices are small pouches of peritoneum laden with fat and small vessels that protrude from the serosal layer of the colon or the caecum into the peritoneal cavity [1]. They are about 0.5-5 cm long and 1-2 cm thick [2]. Epiploic appendices have a very limited blood supply [3]. Primary epiploic appendagitis (PEA), first described by Vesalius in 1543 [4], is a rare, benign self-limiting condition caused by thrombosis, spontaneous infarction or torsion of these epiploic appendages. Other causes are lymphoid hyperplasia and bacterial invasion due to diverticulitis [5].
PEA most commonly presents in the 4th or 5th decades of life, however, a few cases of PEA have been reported in the pediatric population as well. It is more common in males [3,5,6]. Obesity has been associated with this entity, however our patient had a normal BMI [6].
Abdominal pain is the most common presenting symptom in PEA, which can be dull, sharp or colicky, constant, non-migrating; localized in the left or the right lower quadrant and may or may not be associated with rebound tenderness [3,6-8]. Other associated symptoms, though rare, may include nausea, vomiting, anorexia and fever [5,9].
Because of its non-specific presentation, PEA is difficult to diagnose clinically. Labs are usually unremarkable, but leukocytosis and elevated CRP levels have been observed [10]. PEA was mainly a surgical diagnosis until the advent of US and CT scan. US may show a solid paracolic hyperechoic, non- compressible ovoid mass with a subtle hypoechoic rim, with no color on Doppler flow [11-13]. Currently CT scan is the preferred imaging study and the findings include oval shaped, 2-3 cm dense paracolic lesion with adjacent fat stranding and hyper attenuating ring, representing an inflamed and thickened visceral peritoneum surrounding the appendage (ring sign - a pathognomonic sign of PEA) or a central hyperattenuated dot which might represent a thrombosed vessel [11-13]. MRI may also be used which is visualized as an oval shaped fat intensity mass with a central point sign on T1- and T2-weighed images, enhanced better by gadolinium contrast [9,14,15]. If the imaging study does not support the diagnosis of PEA, laparoscopy becomes diagnostic [3].
PEA can present as acute abdomen [16] and mimic many disorders depending on its location. In adult population, it often needs to be differentiated from colonic diverticulitis and the use of colonoscopy in such patients can be justified. However, in children, the common differential for PEA are acute appendicitis, segmental omental infarction, ovarian torsion or abscess, ruptured ovarian cyst, renal stones or acute cholecystitis. Thus, the role of colonoscopy in the pediatric population for PEA is limited.
PEA is a self-limiting condition, with the mainstay of management being anti-inflammatory drugs [17]. The role of antibiotics or surgical intervention remains elusive. Sand et al. [3] reported a recurrence rate of 40% in patients who were treated conservatively, thus favoring surgical therapy to prevent recurrence, inflammation induced adhesions and other less common complications. It is believed that surgical intervention might help in recurrent cases. However, such results were not reciprocated in other studies. For example, a recent study by Hwang et al did not find any difference in rate of recurrence whether PEA was managed conservatively or surgically [18]. Our patient did not have the pathognomonic CT scan finding. Her clinical picture, as well as the laboratory findings and pericolic fat stranding on CT scan suggested a diagnosis of PEA, and this was further bolstered by the resolution of symptoms overtime with NSAIDs. Although rare, PEA can be complicated by intussusception, bowel obstruction, abscess and peritonitis and managing these conditions might need surgical intervention [3,9].
Conclusion
PEA should be considered in the differential diagnosis of acute abdominal pain when the diagnosis remains unclear. A timely diagnosis of PEA with imaging modalities like US and CT scan might help in avoiding unnecessary surgical interventions. Physicians should remember that the classical CT scan findings of PEA might not be evident in all cases and they should have low threshold for diagnosing PEA. Although it is a self-limiting condition mainly managed with anti-inflammatory drugs, PEA can often recur or develop serious complications. In such cases, further prevention of complications and recurrence might necessitate surgical intervention.
Funding Source
No funding was secured for this article.
Financial Disclosure
The authors have no financial relationships relevant to this article to disclose.
Conflict of Interest
The authors have no conflicts of interest to disclose.
References
-
Rioux M, Langis P (1994) Primary epiploic appendagitis: clinical, US, and CT findings in 14 cases. Radiology 191: 523-526.
-
Ozdemir S, Gulpinar K, Leventoglu S, Uslu HY, Turkoz E, et al. (2010) Torsion of the primary epiploic appendagitis: a case series and review of the literature. Am J Surg 199: 453-458.
-
Sand M, Gelos M, Bechara FG, Sand D, Wiese TH, et al. (2007) Epiploic appendagitis--clinical characteristics of an uncommon surgical diagnosis. BMC Surg 7: 11.
-
De Vesalius A (1543) Humanis corporis fabricia libri septem. In: Basileae, Andreae vesalii bruxellensis, scholaemedicorumpatauiniae professoris de humani corporis fabricia libri septem. Ex officinal Joannis Oporini, Basel, Switzerland.
-
Ozdemir S, Gulpinar K, Leventoglu S, Uslu HY, TurkozE, et al. (2010) Torsion of the primary epiploic appendagitis:a case series and review of the literature. Am J Surg 199: 453-458.
-
van Breda Vriesman AC, de Mol van Otterloo AJ, Puylaert JB (2001) Epiploic appendagitis and omental infarction. Eur J Surg 167: 723-727.
-
Son HJ, Lee SJ, Lee JH, Kim JS, Kim YH, et al. (2002) Clinical diagnosis of primary epiploic appendagitis: differentiation from acute diverticulitis. J Clin Gastroenterol 34: 435-438.
-
Boulanger BR, Barnes S, Bernard AC (2002) Epiploic appendagitis: an emerging diagnosis for general surgeons. Am Surg 68: 1022-1025.
-
Sangha S, Soto JA, Becker JM, Farraye FA (2004) Primary epiploic appendagitis: an underappreciated diagnosis. A case series and review of the literature. Digest Dis Sci 49: 347-350.
-
Schnedl WJ, Krause R, Tafeit E, Tillich M, Lipp RW, et al. (2011) Insights into epiploic appendagitis. Nat Rev Gastroenterol Hepatol 8: 45-49.
-
Mollà E, Ripollés T, Martínez MJ, Morote V, Roselló-Sastre E (1998) Primary epiploic appendagitis: US and CT findings. Eur Radiol 8: 435-438.
-
Singh AK, Gervais DA, Hahn PF, Sagar P, Mueller PR, et al. (2005) Acute epiploic appendagitis and its mimics. Radiographics 25: 1521-1534.
-
Rao PM, Wittenberg J, Lawrason JN (1997) Primary epiploic appendagitis: evolutionary changes in CT appearance. Radiology 204: 713-717.
-
Shrestha B, Hampton J (2014) Recurrent epiploic appendagitis and peritoneal dialysis: A case report and literature review. World J Nephrol 3: 114-117.
-
Ozkurt H, Karatag O, Karaarslan E, Rozanes I, Basak M, et al. (2007) CT findings in epiploic appendagitis. Surgery 141: 530-532.
-
Carmichael DH, Organ CH Jr (1985) Epiploic disorders. Conditions of the epiploic appendages. Arch Surg 120: 1167-1172.
-
Buresh CT, Graber MA (2006) Unusual causes of recurrent abdominal pain. Emerg Med 38: 11-18.
-
Jeong Ah Hwang, Sun Moon Kim, Hyun Jung Song, Yu Mi Lee, Kyung Min Moon, et al. (2013) Differential diagnosis of left-sided abdominal pain: Primary epiploic appendagitis vs colonic diverticulitis. World J Gastroenterol 19: 6842-6848.





