Clinical Medical
Reviews and Case Reports
An Underdiagnosed ARVC Case until the Age of 67-Years with Two Large Aneurysms in the Right Ventricle
Kevser G Balcı1, Mustafa M Balcı1, Samet Yilmaz2* and Ramazan Akdemir3
1Cardiology Clinic, Turkey Yuksek Ihtisas Education and Research Hospital, Turkey
2Cardiovascular Department, Yozgat State Hospital, Turkey
3Cardiovascular Department, Sakarya University Hospital, Turkey
*Corresponding author: Samet Yilmaz, MD, Cardiovascular Department, Yozgat State Hospital, 66200, Yozgat/Turkey, Tel: 0090-507-5883, Fax: 0090-354-2121070, E-mail: sametyilmazmd@gmail.com
Clin Med Rev Case Rep, CMRCR-3-120, (Volume 3, Issue 8), Case Report; ISSN: 2378-3656
Received: May 04, 2016 | Accepted: July 28, 2016 | Published: August 01, 2016
Citation: Balcı KG, Balcı MM, Yilmaz S, Akdemir R (2016) An Underdiagnosed ARVC Case until the Age of 67-Years with Two Large Aneurysms in the Right Ventricle. Clin Med Rev Case Rep 3:120. 10.23937/2378-3656/1410120
Copyright: © 2016 Balcı KG, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Arrhythmogenic right ventricular cardiomyopathy (ARVC) is a cardiomyopathy that manifests with ventricular tachycardia (VT), ventricular fibrillation (VF) and sudden cardiac death (SCD). Hence immediate intervention is necessary for this type of presentation. A 67-year-old man was admitted to our emergency department with palpitation. Electrocardiogram (ECG) showed VT. Despite amiodarone and lidocaine administration VT persisted. After the cardioversion (CV) the rhythm became sinus and in the right precordial leads inverted T waves were present. Transthoracic echocardiography (TTE) showed two large aneurysms divided by a septum in the right ventricle (RV). Cardiac magnetic resonance imaging (CMR) also revealed two aneurysms and a dyskinetic segment in the RV. In the intensive care unit, patient was treated with amiodarone (400 mg/daily). In the meantime, the patient had an advanced lung cancer that extended to the pleura and pulmonary artery. Implantable cardiac defibrillator (ICD) was not implanted because the predicted survival was under six months and also the patient refused any invasive treatment including VT ablation. Therefore, we discharged patient with metoprolol (100 mg/daily) and amiodarone (400 mg/daily). In the follow-up period, no VT attacks occurred. After three years of the first diagnosis, patient woke up with a sense of palpitation and then died suddenly. In this case, double chamber RV due to ARVD and the therapy guidance were discussed.
Keywords
Arrhythmogenic right ventricular cardiomyopathy, Double chamber right ventricle, Ventricular tachycardia
Introduction
Arrhythmogenic right ventricular cardiomyopathy (ARVC) is a genetic form of cardiomyopathy characterized by akinesia, dyskinesia, or an aneurysm in the right ventricle (RV) [1,2]. ARVC accounts for 20 percent cases of sudden cardiac death (SCD). Among young athletes dying suddenly, the prevalence of this condition is higher [3,4]. Patients typically present between the teenage years to the forties, with only 10% falling out of this age range. Mostly, the first manifestation is unexplained syncope or SCD. Here, we present the case of a man who admitted to the emergency department with ventricular tachycardia (VT) and survived until the age of 67 years without the diagnosis of ARVD.
Case Presentation
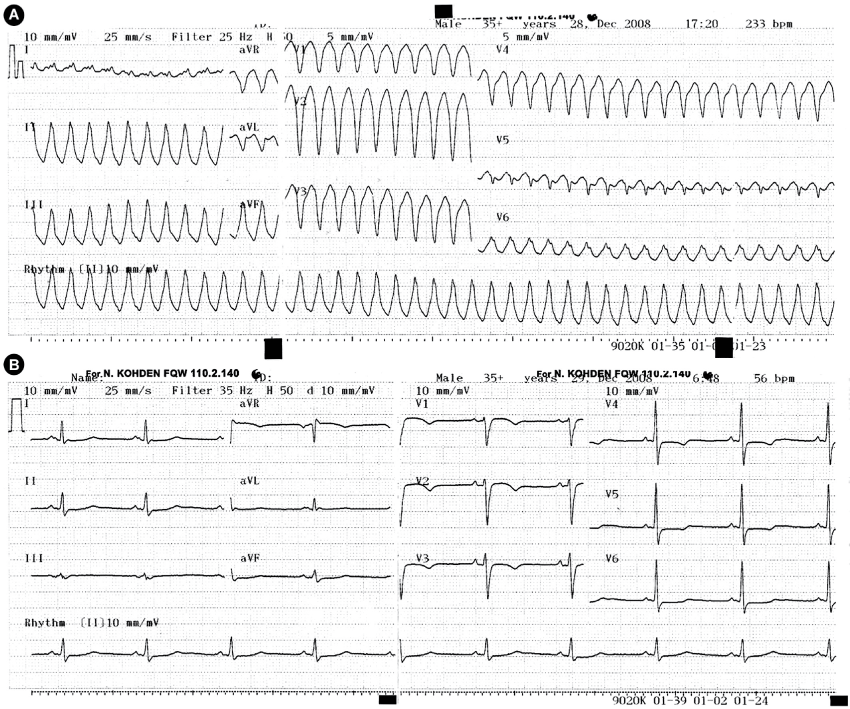
A 67-year-old man was admitted to our emergency department with palpitation and deterioration. At presentation, he was alert but aware and hemodynamically stable. The pulse was regular at 220 per minute; the blood pressure was 140/90 mmHg. An electrocardiogram (ECG) showed ventricular tachycardia (VT) with left bundle branch block (LBBB) morphology (Figure 1A). After 100 mg lidocaine and 300 mg amiodarone intravenous administration, the rhythm was still VT. The patient became unconscious, and cardioversion (CV) with 300 Joules was performed. After the CV the rhythm was sinus: in the right precordial leads inverted T waves were present, also QRS width was longer than 110 ms (Figure1B).
.
Figure 1: A) Presentation ECG; VT with LBBB; B) After CV, inverted T waves in the right precordial leads, QRS prolongation in V1-V3 being longer than 110 ms.
View Figure 1
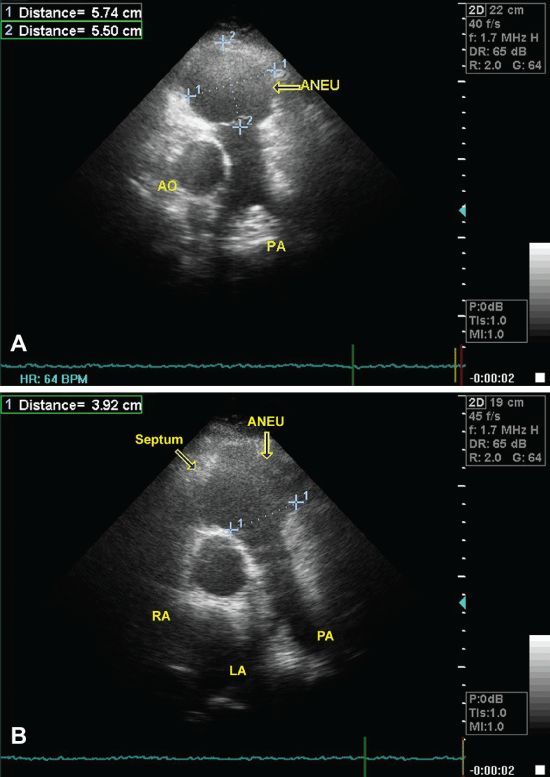
Transthoracic echocardiogram (TTE) revealed two large aneurysms divided by a septum in the RV (Figure 2A). The largest aneurysm was in the RV outflow tract with a dimension 5.74 x 5.5 cm (Figure 2B). RV dilatation and thinning of the RV free wall was present. RV outflow tract diameter was 3.92 cm and RV systolic pressure was in the low-normal range; RV ejection fraction was < 40% but left ventricle ejection fraction was normal. Admission laboratory tests were also normal.
.
Figure 2: A) A large aneurysm that was placed in the RV outflow tract; B) Arrows show aneurysm and the septum.
View Figure 2
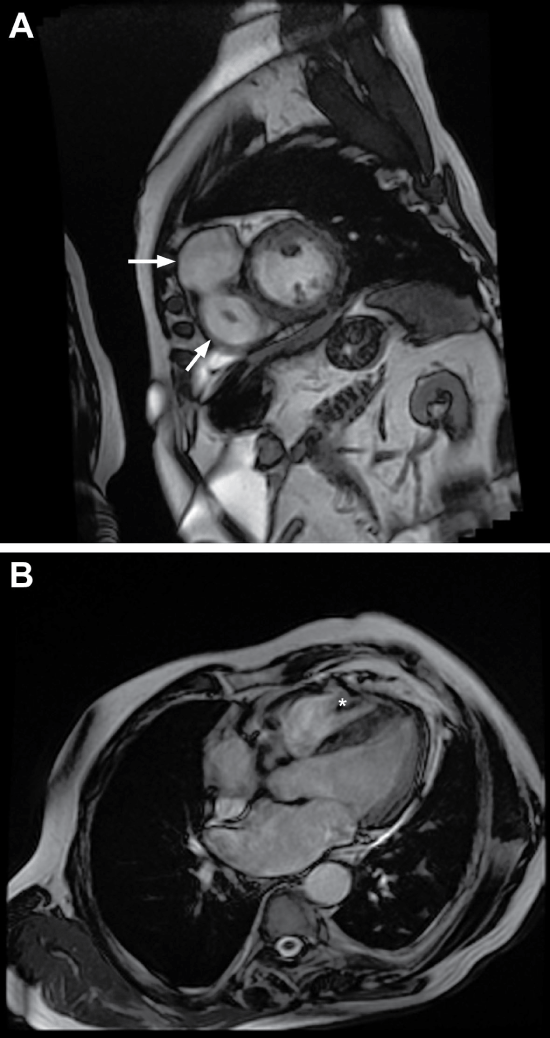
He had a history of lung squamous cell cancer. In the first TTE that was done just before the first chemotherapy (CT) showed dilated RV and a normal RV systolic pressure. Since then patient had three CTs and all of the TTEs that were done before the CT showed a persistent RV dysfunction. Although the patient had a coronary angiogram five years ago, to exclude the ischemic reasons of VT we repeated the coronary angiogram that showed normal coronary arteries. Cardiac magnetic resonance imaging (CMR) identified a dyskinetic segment placed in the RV outflow tract and two large aneurysms divided by a septum in the RV (Figure 3A and Figure 3B). There were no LV abnormalities.
.
Figure 3: A) Arrows show two large aneurysms divided by a septum; B) *shows the septum in the right ventricle.
View Figure 3
We planned ICD implantation but first we consulted the patient to the oncology department for the predicted survival. In the meantime, the patient was treated with amiodarone and followed in the intensive care unit. Thorax MRI revealed extension of the tumor to the pleura and pulmonary artery. In conclusion, the survival was estimated less than one year, and we agreed on VT ablation. However, the patient refused VT ablation. Therefore, the patient was treated with amiodarone (300 mg/daily) and metoprolol (100 mg/daily) and then discharged. After three years, in the midnight patient woke up with a sense of a palpitation and then he died suddenly.
Discussion
Estimated prevalence of the ARVC is 0.02% to 0.1% [5]. Except 10% of cases, patients mostly present at early ages. Our case is very unusual related to the patient’s late presentation and CMR findings. Until 67 years old the patient was under-diagnosed and in the previous reviews and cases, double chamber RV due to the ARVC has not been mentioned.
Patients with ARVC present with RV outflow tachycardias usually during exercise [4]. However, also coronary artery disease, right or biventricular cardiomyopathy, sarcoidosis and congenital heart disease cause this type of arrhythmias. While making the differential diagnosis, we considered coronary artery disease, Uhl disease, cardiomyopathies (CMP) and other causes of arrhythmias. According to the diagnostic 2010 Task Force criteria for ARVC: presentation with VT, family history, inverted T waves in the right precordial leads, QRS prolongation in V1-V3 being longer than 110 ms, RV dilatation and aneurysms revealed by TTE and CMR, we made the definite diagnosis of ARVC [6]. In his family history, three of his first-degree relatives died at the ages between 50-70 because of tachyarrhythmias. We repeated coroner coronary angiogram to eliminate coronary artery disease that showed normal coronary arteries. The Uhl disease is an early childhood presented form of RV disease characterized by congenital absence of RV myocardium [7]. For our case, we excluded Uhl disease because of the late presentation.
While treating ARVC, the primary aim is to avoid SCD. For our case because of the diminished survival, we did not implant ICD. It is interesting that patient presented at an older age and was under-diagnosed till this time. In his family history, three of the first-degree relatives died at the ages between 50-70 because of SCD. We think this circumstance is related to the late-onset form of ARVC described by this unusual case.
References
-
Basso C, Corrado D, Marcus FI, Nava A, Thiene G (2009) Arrhythmogenic right ventri- cular cardiomyopathy. Lancet 373: 1289-1300.
-
Marcus FI, Fontaine GH, Guiraudon G, Frank R, Laurenceau JL, et al. (1982) Right ventricular dysplasia: a report of 24 adult cases. Circulation 65: 384-398.
-
Corrado D, Basso C, Rizzoli G, Schiavon M, Thiene G (2003) Does sports activity enhance the risk of sudden death in adolescents and young adults? J Am Coll Cardiol 42: 1959-1963.
-
Thiene G, Nava A, Corrado D, Rossi L, Pennelli N (1988) Right ventricular cardiomyopathy and sudden death in young people. N Engl J Med 318: 129-133.
-
Kiès P, Bootsma M, Bax JJ, Schalij MJ, van der Wall EE (2006) Arrhytmogenic Right Ventricular dysplasia/cardiomyopathy: screening, diagnosis, and treatment. Heart Rhythm Society 3: 225-234.
-
Marcus FI, McKenna WJ, Sherrill D, Basso C, Bauce B, et al. (2010) Diagnosis of arrhythmogenic right ventricular cardiomyopathy/dysplasia: proposed modification of the Task Force Criteria. Eur Heart J 31: 806-814.
-
Richardson JD, Teo KS, Bertaso AG, Wong DT, Disney P, et al. (2012) Uhl's anomaly. Int J Cardiol 154: e36-37.





