Clinical Medical
Reviews and Case Reports
Non-Puerperal Uterine Inversion in a Young Woman: A Case Report, Brief Surgical Review, and Clinical Insights
Leeya F Pinder1,2,3,4*, Kennedy O Ouma3,4 and Brett D Nelson1,5
1Department of Emergency Medicine, Division of Global Health and Human Rights Massachusetts General Hospital, USA
2Department of Obstetrics and Gynecology, Boston University School of Medicine, USA
3Department of Family Medicine and Community Health, Maseno University, Kenya
4Sagam Community Hospital, Sagam, Kenya
5Harvard Medical School, Boston, USA
*Corresponding author: Leeya F. Pinder, MD, MPH, Department of Emergency Medicine, Division of Global Health and Human Rights, Massachusetts General Hospital, 125 Nashua Street, Suite 910, Boston, MA 02114, USA, Tel: +1-617-643-4294, E-mail: leeyapinder@gmail.com
Clin Med Rev Case Rep, CMRCR-3-122, (Volume 3, Issue 8), Case Report; ISSN: 2378-3656
Received: June 15, 2016 | Accepted: August 03, 2016 | Published: August 06, 2016
Citation: Pinder LF, Ouma KO, Nelson BD (2016) Non-Puerperal Uterine Inversion in a Young Woman: A Case Report, Brief Surgical Review, and Clinical Insights. Clin Med Rev Case Rep 3:122. 10.23937/2378-3656/1410122
Copyright: © 2016 Pinder LF, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Uterine inversion is usually encountered in the puerperal period and is considered a life-threatening event. The incidence of puerperal uterine inversion is 1 in 3500 deliveries; however, the incidence of non-puerperal uterine inversion is largely unknown. With few more than 100 cases reported in the literature, the management of this condition poses many challenges. We introduce the case of a 24-year-old presenting to a rural, private hospital in western Kenya, with isolated severe pelvic pain and a protruding vaginal mass for several days. Non-puerperal uterine inversion was identified and surgical interventions included the Haultain procedure and supracervical hysterectomy. Edema and strength of the constriction ring in addition to necrosis and infection of the uterus increased the difficulty of this procedure. Rarity of disease, delayed presentation to a healthcare facility, and atypical symptoms can additionally pose challenges to the management of this condition, as it did in our case.
Keywords
Uterine inversion, Non-puerperal uterine inversion, Uterine prolapse, Submucosal uterine fibroid, Total inversion, Prolapse inversion
Introduction
Non-puerperal uterine inversion is a rare clinical condition not associated with pregnancy, in which the uterine fundus descends into or through the endometrial cavity or the cervix, resulting in propulsion of the uterus out of the pelvis and potentially into the vagina or outside the body. Other reproductive structures such as the fallopian tubes and ovaries may be displaced from the pelvis and confined within the inverted uterus. The incidence of non-puerperal uterine inversion remains unclear [1], with little more than 100 cases reported worldwide. This type of inversion is typically associated with pathological processes such as sub-mucosal uterine fibroids, endometrial polyps, uterine sarcomas, endometrial carcinomas, and mixed mesodermal tumors [2,3]. More than a quarter of cases (27%) are associated with malignant tumors, mostly sarcomas [2,4]. The mechanism in which the tumors result in inversion of the uterus is largely unknown; however, thin uterine wall, rapid growth of the tumor, dilation of the cervix by the tumor and abrupt expulsion of the tumor have been cited [3].
This disorder can be classified as acute or chronic based on the onset and evolution of symptoms. The acute manifestation is often dramatic, presenting with severe pain and hemorrhage, while the chronic manifestation, which is more common, has an insidious onset, presenting with pelvic discomfort, vaginal discharge, and irregular vaginal bleeding [4]. Important diagnostic tools for uterine inversion include ultrasound, CT, or MRI scans, and findings will depend on the stage or degree of prolapse. However, the diagnosis is often confirmed during examination under anesthesia or laparotomy. Management and treatment largely depends on the pathologic or histologic results, and frozen section is recommended pre- or intra-operatively, if feasible, to determine presence of malignancy [5]. For women who wish to preserve childbearing capabilities, conservative surgery is preferred; although, in malignant cases, radical hysterectomy may be recommended [5].
Case Report
A 24-year-old gravida 2, para 2 woman presented ambulatory to the emergency department of a rural, private hospital in western Kenya, with complaints of a protruding mass and lower abdominal pain. She reported that, while attempting a bowel movement with some difficulty several days earlier, a mass was expelled from her vagina. She additionally reported that the expulsion of this mass was accompanied with acute onset severe lower abdominal pain without bleeding, and several days later she experienced a foul-smelling vaginal discharge. Further review of her history revealed a previous diagnosis of uterine fibroids without follow-up for management. Records were unavailable for review.
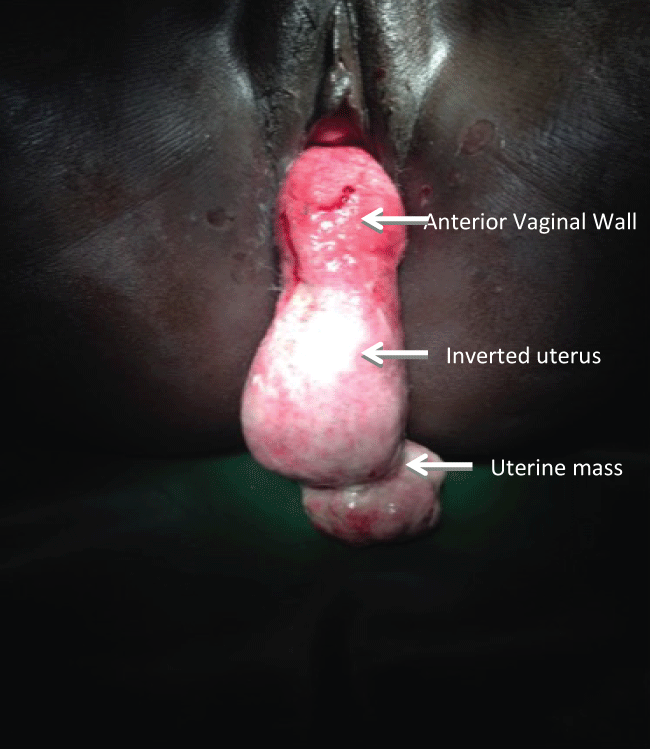
On examination, she was found to be in obvious pain; however, her initial vital signs were blood pressure 105/68 mmHg and pulse 85 beats per minute. Local examination exhibited an approximately 12 cm mass with a necrotic-appearing undersurface, widespread white patchy flakes, and friable regions to the touch. Additionally, a large lesion on the distal portion of this mass measuring 8 ± 6 cm and covered with suppurative material was noted (Figure 1). Bedside abdominal ultrasound was performed, revealing absence of the uterus and ovaries in the pelvis and a mass contained in the vagina. A diagnosis of total uterine inversion, likely secondary to a suspected uterine fibroid, was made.
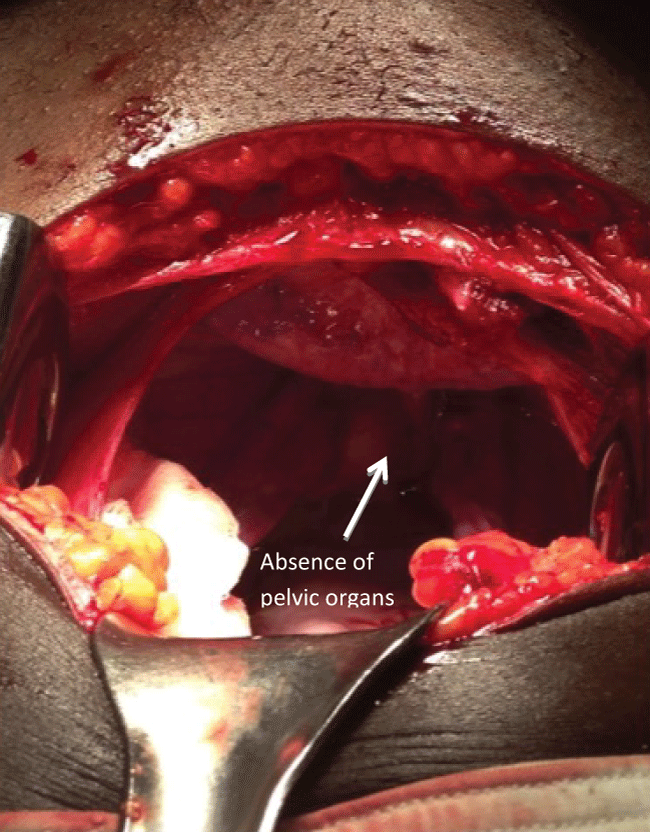
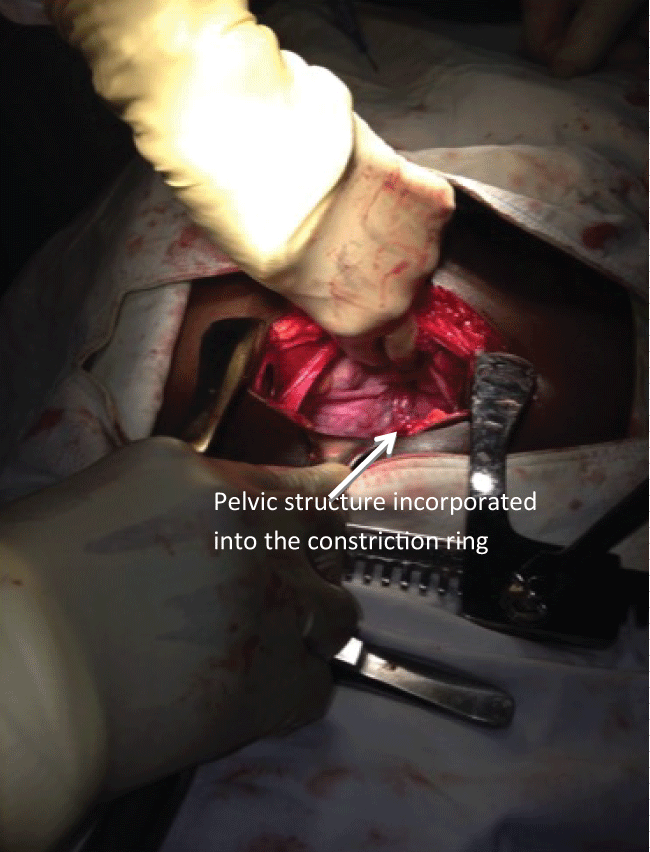
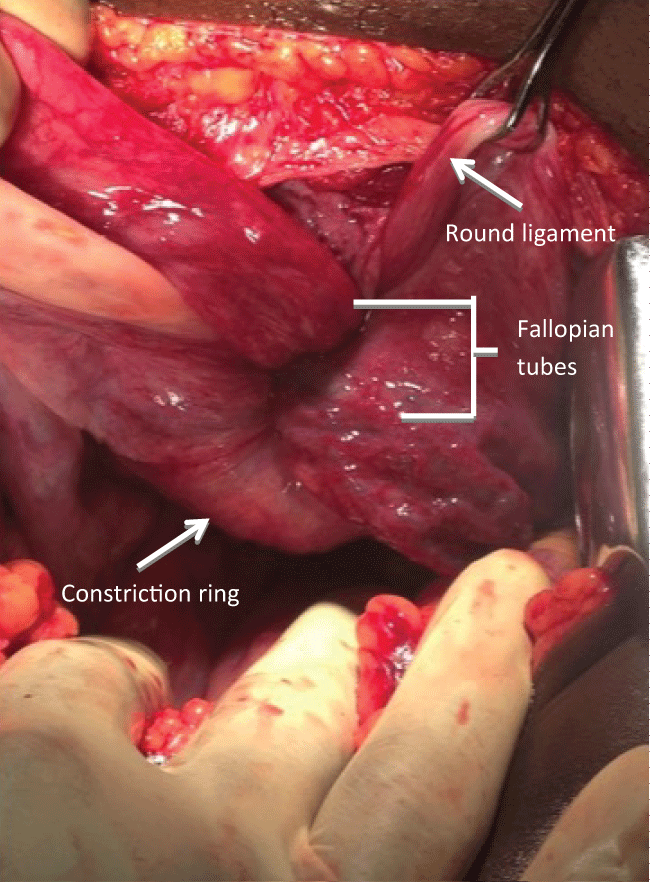
Following stabilization of her clinical condition, she was moved to the operating room for surgical management. An abdomino-vaginal approach was undertaken. The distal mass remaining in situ hindered the process of reverting the uterus and was necessary for pathologic diagnosis; consequently, it was excised, and the defect suture ligated for hemostasis. The uterus and vaginal walls were explored post excision, and necrosis, marked friability of the endometrial cavity and suppurative material were noted diffusely, making the ability to salvage the uterus unlikely. Attention was turned to the abdomen to perform a Haultain procedure following laparotomy, which was made difficult by the necrosis and edema of the uterus and the strength of the constriction ring (Figure 2, Figure 3 and Figure 4). A longitudinal incision was made along the constriction ring and extended to include the inferior posterior uterine wall. Thereafter, the uterine fundus was successfully reverted and, following restoration of pelvic anatomy to its normal position, a supracervical hysterectomy was performed. The decision to perform hysterectomy was predicated by the extensive necrosis and infection of the uterus, which posed additional risks to the patient if left in situ, in addition to the knowledge of patient-determined completion of childbearing.
The patient had an uneventful post-operative course and was discharged home on the fifth postoperative day. Pathologic findings were consistent with uterine leiomyoma.
Brief Surgical Review
Unlike puerperal uterine inversion, manual reduction of the uterus is often unsuccessful in the non-puerperal form, as a result of the lower uterine segment and the cervix contracting over time to create a constriction ring, making manual replacement of the uterus progressively more difficult. As such, surgical correction becomes inevitable [6]. There are different surgical techniques proposed for reverting the prolapsed uterus: abdominally coinciding with laparotomy, laparoscopically, and trans-vaginally. At times, a combination of approaches may be necessary to rectify this disorder. Once the uterus is reverted to its position, subsequent management will depend on the patient's future reproductive desires, pathologic results and current clinical condition [6].
Two abdominal approaches for reduction of the inverted uterus have been documented: the Haultain and Huntington techniques [7]. In Huntington's technique, the cup or dimple of the inversion is identified, Allis forceps are introduced into the cup and placed on the round ligaments, and gentle upward traction is exerted on the clamps containing the ligaments. While further upward pressure is exerted on the advancing uterus, traction is continually applied on the ligaments until correction of the inversion is accomplished. In Haultain's technique, the technique utilized in this case, a longitudinal incision is made in the posterior uterine wall and through the cervical constriction ring. This releases the constrictive pressure and facilitates anatomical restoration of the uterus with continued upward pressure until it reverts to normal positioning [7,8].
Lastly, we consider the trans-vaginal approaches: Tew's and Kustners's procedures. In Tew's procedure, the constriction ring is released by performing an anterior hysterotomy after dissection of the bladder off of the cervix and lower uterine segment. The uterus is then reverted, and the hysterotomy is closed in several layers in cases of uterine preservation; otherwise, hysterectomy is performed. The Kustner's technique involves replacing the uterine fundus after opening the posterior cul-de-sac and incising the cervix and posterior wall, providing the clearance for correcting the inversion [7]. The defect in the posterior uterine wall and cervix is then closed in layers, followed by closure of the colpotomy [8].
Clinical Insights and Discussion
With the rarity of this clinical condition, proper management and appropriate surgical techniques can be complex matters to undertake. It is believed that most gynecologic surgeons will not encounter a case of non-puerperal uterine inversion during their careers. Without prior exposure to this disorder, surgeons may find themselves venturing into the acute management of a very complicated clinical condition. We highlight the following considerations to assist with navigating this potential challenge based on the literature available.
Non-puerperal uterine inversion can pose a major diagnostic dilemma, since it is associated with non-specific clinical symptoms. Complaints such as lower abdominal pain, urinary disturbances, pressure, or a feeling of something coming down the vagina are often reported. In addition, patients may complain of vaginal discharge or vaginal bleeding [2]. These complaints are similar to other common gynecologic conditions, which may lead to misdiagnosis. Recognizing the inversion on pelvic examination may be difficult; however, recognition that normal anatomical structures are not easily visible or palpable, such as the cervix, cervical os, or uterine fundus, will aid in diagnosis.
Our patient had no preceding symptoms and a less common presentation having no acute hemorrhage once inversion occurred, which is in contrast to other cases reported [2,4,9-11]. The patient experienced severe pain initially, however, this did not prompt evaluation as pain was alleviated with padding her undergarments to support the mass. She sought medical care only in the setting of a new-onset odor several days following the expulsion of her uterus, highlighting the occurrence of delays in decision to seek care not solely in cases of obstetric emergencies. Poor understanding of her medical condition and financial implications contributed to her delay in seeking medical attention and resulted in a complex chronic uterine inversion.
Most cases of non-puerperal uterine inversion reported in the literature are in women beyond childbearing age, with few reported in women under the age of 35, as in our case [3,12-14]. Fertility preservation is of concern when non-puerperal uterine inversion occurs in the presence of infection and/or necrosis, also noted in our report. There are no clear management strategies in these instances, and when the inversion is chronic, reverting maneuvers may prove difficult, rendering fertility-sparing techniques implausible. If available, substances that cause relaxation of the uterus may be considered, but risks versus benefits should be assessed before trialing.
Should uterine preservation be successful, there is no evidence to suggest the appropriate interval before attempting pregnancies following these techniques; however, in other recommendations of pregnancy interval following uterine surgery, greater than 12 months is suggested [15]. As with all uterine surgery, the risk of uterine rupture with subsequent delivery should be addressed. For vertical incisions extending the entire length of the uterus, the risk for uterine rupture is upwards of 10% and may be higher with use of induction agents [16,17]. Women should be cautioned and counseled appropriately about risks in future pregnancies as many of the fertility-preserving techniques involve considerable extension through the myometrium.
While the majority of tumors found are benign fibroids, several studies reported malignancy in up to 20% of pathologic specimens [10,18] and many of those reported in young women [3]. Uterine leiomyosarcomas (LMS) accounts for about 1% of all uterine malignancies and the incidence of LMS in a series of hysterectomies performed for presumed uterine leiomyomas was approximately 0.1-0.3% [19]. The true prevalence in many regions of the world, however, is largely unknown. Accordingly, pathologic evaluation of the specimen is critical to the complete management of women with a uterine mass as the source of uterine inversion since local recurrence or distant metastasis may occur many years after the initial surgery.
Conclusion
Non-puerperal uterine inversion, while a rare clinical event, should be considered in the setting of a mass protruding from the vagina, with or without bleeding, and a non-palpable uterus on abdominal examination or invisible pelvic organs on ultrasound. Surgical technique will depend on provider skill and experience and desire for fertility preservation. In the setting of fertility preservation, malignancy must be ruled out, and the patient must be counseled on interval pregnancy and risks to modalities of delivery. While most gynecologic surgeons will not experience this condition during their careers, there is utility in awareness of this clinical condition and its appropriate interventions and considerations.
Consent
Written informed consent was obtained from the patient for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
References
-
Chen YL, Chen CA, Cheng WF, Huang CY, Chang CY, et al. (2006) Submucous myoma induces uterine inversion. Taiwan J Obstet Gynecol 45: 159-161.
-
Nahid E (2007) Non‑puerperal uterine inversion in a virgin woman. Iranian Journal of Reproductive Medicine 5: 135-136.
-
de Vries M, Perquin DA (2010) Non-puerperal uterine inversion due to submucous myoma in a young woman: a case report. J Med Case Rep 4: 21.
-
Tahere A (2005) Non-puerperal uterine inversion: A case report. Arch Iranian Med 8: 63-66.
-
Nelson JH, Sites JG (1956) Non-puerperal inversion of the uterus. Am J Obstet Gynecol 72: 660-662.
-
Lozo S, Khulpateea N, Choi C (2015) Surgical approach to nonpuerperal uterine inversion: case series.
-
Shamsudin F, Morton K (2007) Novel correction technique of chronic puerperal inversion of the uterus. J Obstet Gynaecol 27: 197-198.
-
Shivanagappa M, Bhandiwad A, Mahesh M (2013) A case of acute on chronic uterine inversion with fibroid polyp. J Clin Diagn Res 7: 2587-2588.
-
Suprasert P, Srisomboon J, Phongnarisorn C, Euathrongchit J, Siriaunkgul S, et al. (2000) Non-Puerperal Uterine Inversion. Thai Journal of Obstetrics and Gynaecology 12: 61-65.
-
Hu CF, Lin H (2012) Ultrasound diagnosis of complete uterine inversion in a nulliparous woman. Acta Obstet Gynecol Scand 91: 379-381.
-
Yakasai I, Ibrahim S, Muhammad Z (2012) Chronic non-puerperal uterine inversion: Case series. Nigerian Journal of Basic and Clinical Sciences 9: 87-90.
-
Lupovitch A, England ER, Chen R (2005) Non-puerperal uterine inversion in association with uterine sarcoma: case report in a 26-year-old and review of the literature. Gynecol Oncol 97: 938-941.
-
Setu Rathod, Samal SK, Pallavee P, Ghose S (2014) Non puerperal uterine inversion in a young female- a case report. J Clin Diagn Res 8: OD01-OD02.
-
Gomez-Lobo V, Burch W, Khanna PC (2007) Nonpuerperal uterine inversion associated with an immature teratoma of the uterus in an adolescent. Obstet Gynecol 110: 491-493.
-
Zhang Y, Hua KQ (2014) Patients' age, myoma size, myoma location, and interval between myomectomy and pregnancy may influence the pregnancy rate and live birth rate after myomectomy. J Laparoendosc Adv Surg Tech A 24: 95-99.
-
Varma R, Gupta JK, Smith GCS (2007) Birth After Previous Cesarean Birth. Royal College of Obstetricians and Gynaecologists 1-17.
-
G. Saade, MA Belfort, MR Foley, JP Phelan, GA Dildy (2010) Etiology and Management of Hemorrhage. In: Stafford I, Belfort MA, GAD III, Critical Care Obstetrics. John Wiley & Sons, 310-312.
-
Fofie CO, Baffoe P (2010) Non-puerperal uterine inversion: a case report. Ghana Med J 44: 79-81.
-
El-Khalfaoui K, Bois A, Heitz F, Kurzeder C, Sehouli J, et al. (2014) Current and future options in the management and treatment of uterine sarcoma. Ther Adv Med Oncol 6: 21-28.