Clinical Medical
Reviews and Case Reports
Erythromelalgia in an Infant Caused by Adenovirus Gastroenteritis
Gulsum Alkan1*, Melike Keser Emiroglu1 and Hüseyin Tokgoz2
1Department of Pediatric Infectious Diseases, Selcuk University, Turkey
2Department of Pediatric Hematology, Necmettin Erbakan University, Turkey
*Corresponding author: Gulsum Alkan, Fellow, MD, Faculty of Medicine, Department of Pediatric Infectious Diseases, Selcuk University, Konya, Turkey, Tel: +9-0506-681-2293, E-mail: galkan-85@hotmail.com
Clin Med Rev Case Rep, CMRCR-3-133, (Volume 3, Issue 10), Case Report; ISSN: 2378-3656
Received: August 12, 2016 | Accepted: October 01, 2016 | Published: October 04, 2016
Citation: Alkan G, Emiroglu MK, Tokgoz H (2016) Erythromelalgia in an Infant Caused by Adenovirus Gastroenteritis. Clin Med Rev Case Rep 3:133. 10.23937/2378-3656/1410133
Copyright: © 2016 Alkan G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Reactive thrombocytosis (RT) is typically a result of bacterial infections in children. RT due to viruses is rarely seen and is most often secondary to a respiratory tract infection. Erythromelalgia (EM) is a rare condition caused by arteriovenous shunting and reduced capillary perfusion. Thrombocytosis can cause microvascular thrombi and can result in EM.
A 2.5-month-old infant with EM due to RT secondary to adenoviral gastroenteritis was presented because of its rarity. The EM gradually improved with hydration, and the platelet count returned toa normal level after one month. Primary thrombocytosis and primary EM are seldom seen in children; therefore, secondary causes, especially infectious diseases, must be evaluated. The management of patients must be monitored for underlying disease, not for platelet counts.
Keywords
Reactive thrombocytosis, Adenovirus gastroenteritis, Erythromelalgia
Introduction
Thrombocytosis is defined as an elevated platelet count (> 450,000/mm3) in peripheral blood. Pediatric primary thrombocytosis is very rare, but RT can be frequently observed. RT can be seen due to nonmalignant hematologic conditions (iron deficiency anemia, acute hemolytic anemia), malignant conditions (lymphoma), acute and chronic inflammatory conditions (Kawasaki disease and celiac disease), tissue damage (severe trauma) infections (acute bacterial or viral infections), exercise, allergic reactions, asplenia and reactions to medications [1].
Drenth, et al. distinguished three types of EM; thrombocythemia, primary EM, and secondary EM. EM is a rare neurovascular pain characterized by burning extremity pain, erythema, and increased temperature of affected skin. EM may be secondary to other underlying diseases, such as myeloproliferative, polycythemia vera, essential thrombocytosis, connective tissue, cardiovascular, infectious and neurological diseases, diabetes mellitus, vasculitis, and neoplasia [2]. The histopathological changes in cases of EM related to thrombocythemia have been considered arteriolar inflammation, fibromuscular intimal proliferation, and thrombotic occlusion [3].
Thromboembolism has not been reported in children due to RT with infections. Antiplatelet therapyis not required even though the platelet count is as high as > 1000.000/mm3. A conservative approach and treatment of the underlying infection is the main management of RT [4]. Management of EM addresses treatment of the accompanying diseases or conditions [2].
Case Report
A 2.5-month-old female was admitted with a fever for the past three days. Her systemic examination was unremarkable, except for irritability and fever (38.9°C). The laboratory data included: white blood count (WBC) 17 × 103/mm3, neutrophils 51%, lymphocytes 35%, hemoglobin (Hb) 9, 2 g/dL, platelets 666,000/mm3, erythrocyte sedimentation rate (ESR) 68 mm/hr and C-reactive protein (CRP) 40 mg/dL. The serum iron, iron-binding capacity, serum electrolytes, liver enzymes, urine analysis, and chest x-ray were within normal limits. A lumbar puncture was rejected by the family. Empiric cefotaxime and ampicillin were started for a possible late neonatal sepsis after the cultures were obtained. The echocardiography and abdominal ultrasonography were normal. The fever resolved one day later then gastroenteritis developed. Examination of stool samples, adenovirus was detected. Studied with qualitative immunoassay methods that detect the adenovirus serotype 40-41 (Adenovirus Rapid Test Device sensitivity and specificity, respectively, 98.8% and 99.9%).
The blood, urine and stool cultures were negative, so the antibiotic treatment was discontinued. After the general condition healed, she was discharged.
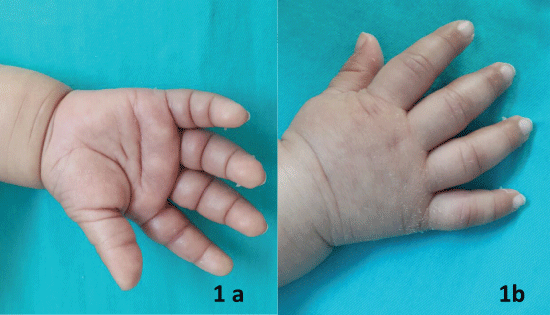
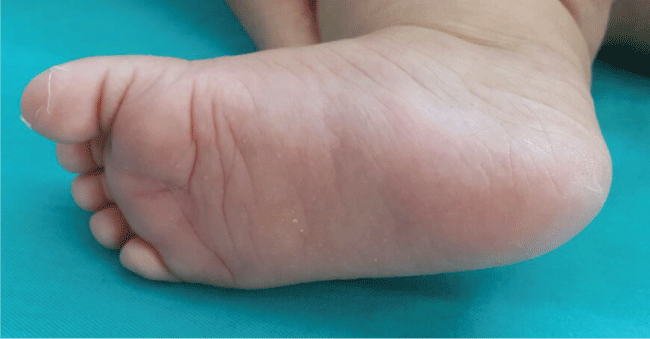
One week later, she presented with restlessness without a fever. In the examination, erythema, swelling and tenderness of the hands and feet, and peeling at the toes and fingertips were observed (Figure 1 and Figure 2). A maculopapular rash on the trunk and arms was detected. The rest of the physical examination was normal. In her history, siblings had peeling at the fingertips and toes after every antibiotic usage. The laboratory data were WBC 20 × 103/mm3, neutrophils 80%, Hb 9.2 g/dl, platelet 1098.000/mm3 with an absence of atypical lymphocytes in the peripheral blood, ESR 48 mm/hr and CRP 16 mg/dL. The control echocardiography was normal. Other acute infections, including (cytomegalovirus, Epstein-Barr virus, rubella, parvovirus, human immunodeficiency virus (HIV), and toxoplasma) were excluded by serological tests. The polymerase chain reaction assay tests for respiratory viruses were negative.
With hydration, the platelet count decreased within five days. The erythema, swelling and tenderness of the hands and feet were gone within eight days; the irritability also disappeared. One month later, the platelet count got below 350,000/mm3.
Discussion
Bacterial infections are more frequently associated with childhood RT than viral infections. Respiratory tract infections are the most common infections, followed by gastrointestinal and urinary tract infections. RT is typically found with complicated lower respiratory tract infections in children. The respiratory syncytial virus and the rhinovirus are the most common viruses that cause thrombocytosis; the adenovirus causing thrombocytosis is rare [4,5].
The mechanism of thrombocytosis is estimated to cause an increase of serum cytokines, such as thrombopoietin, interleukin-6, interleukin-8 and tumor necrosis factor alpha. A recombinant adenovirus encoding human thrombopoietin gene transfer protocol in mice, demonstrates that it leads to transient thrombocytosis [6,7].
EM is characterized by erythema, warming, and burning pain, especially in the extremities. HIV, infectious mononucleosis, poxvirus, hepatitis B vaccine, and the influenza vaccine are reported to cause secondary EM [8].
The relationship between EM and thrombocythemia is considered to cause, platelet-mediated inflammatory and occlusive arteriolar changes [9].
In this patient, thrombocytosis and EM were thought to be due to adenoviral gastroenteritis. Other reasons were excluded by the patient’s history, physical examination, culture, and serological tests. Kawasaki disease was excluded with the absence of a prolonged fever. The maculopapular rash supported a viral infection. A bone marrow aspiration was not performed because of the absence of organomegaly, cytopenia, and atypical cells. The peeling of fingertips could develop during the course of EM. Infectious diseases, such as (Kawasaki disease, scarlet fever, and measles), and medication, such as anticonvulsants, and antibiotics, including (penicillin and sulfonamides) could cause the peeling of fingers and toes [10]. In this case, the peeling was considered to be linked to the antibiotics or EM.
Thrombocytosis due to infections does not usually require platelet aggregation inhibitors. Medical professionals should aim to treat the underlying diseases, not platelet counts. In this case, the hyperviscosity was gradually reduced with hydration, and the clinical condition improved.
References
-
Fred F Ferri, FACP (2016) Thrombocytosis. In: Fred F Ferri, Ferri's Clinical Advisor. 1214-1215.
-
Cato Mørk, Knut Kvernebo (2013) Erythromelalgia. In: Mark G Lebwohl, Warren R Heymann, John Berth-Jones, Ian Coulson, Treatment of Skin Disease: Comprehensive Therapeutic Strategies. (4th edn), 242-244.
-
Mark DP Davis, Thom W Rooke (2012) Erythromelalgia. In: Mark Creager, Joshua A Beckman, Joseph Loscalzo, Vascular Medicine: A Companion to Braunwald's Heart Disease. (2nd edn), 604-612
-
Cecinati V, Brescia L, Esposito S (2012) Thrombocytosis and Infections in Childhood. The Pediatric Infectious Disease Journal 31: 80-81.
-
Jae Kyung, Jae-Sik Jeon, Jong Wan, Ga-Yeon (2016) Correlation Between Abnormal Platelet Count and Respiratory Viral Infection in Patients From Cheonan, Korea. J Clin Lab Anal 30: 185-189.
-
Zheng SY, Xiao QY, Xie XH, Deng Y, Ren L, et al. (2016) Association between secondary thrombocytosis and viral respiratory tract infections in children. Sci Rep 6: 22964.
-
Abina MA, Tulliez M, Duffour MT, Debili N, Lacout C, et al. (1998) Thrombopoietin (TPO) knockout phenotype induced by cross-reactive antibodies against TPO following injection of mice with recombinant adenovirus encoding human TPO. J immunol 160: 4481-4489.
-
Al-Minshawy SM, El-Mazary AA (2014) An Egyptian child with erythromelalgia responding to a new line of treatment: a case report and review of the literature. J Med Case Rep 8: 69.
-
Michiels JJ, Abels J, Steketee J, van Vliet HH, Vuzevski VD (1985) Erythromelalgia caused by platelet-mediated arteriolar inflammation and thrombosis in thrombocythemia. Ann Intern Med 102: 466-471.
-
Boris Garber, Rita K Cydulka. Dermatologic Presentation. Chapter 120, Rosen's Emergency Medicine, 1558-1585.