Clinical Medical
Reviews and Case Reports
Right Superior Vena Cava Draining into the Left Atrium
Songul Usalp1*, Ali Rıza Karaci2, Kevser Gülcihan Balcı3, Volkan Yazıcıoglu2, Murat Baskurt1 and Nurcan Arat Koc1
1Department of Cardiology, Istanbul Bilim University, Turkey
2Department of Thoracic & Cardiolovascular Surgery, Istanbul Bilim University, Turkey
3Specialist of Cardiology, Turkiye Yuksek Ihtisas Research and Education Hospital, Turkey
*Corresponding author: Songul Usalp, M.D, Department of Cardiology, Istanbul Bilim University, Sisli, Istanbul, Turkey-34394, Tel: +90-507-853-21-53, Fax: +90-212-272-34-61, E-mail: dr.songulusalp@hotmail.com
Clin Med Rev Case Rep, CMRCR-3-134, (Volume 3, Issue 10), Case Report; ISSN: 2378-3656
Received: May 10, 2016 | Accepted: October 03, 2016 | Published: October 06, 2016
Citation: Usalp S, Karaci AR, Balcı KG, Yazıcıoglu V, Baskurt M, et al. (2016) Right Superior Vena Cava Draining into the Left Atrium. Clin Med Rev Case Rep 3:134. 10.23937/2378-3656/1410134
Copyright: © 2016 Usalp S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Anomalous systemic venous connection with the left atrium (LA) is an unusual congenital cause of a right-to-left shunt. The most common variant is persistent left superior vena cava (SVC), which is estimated to occur among 2.1% to 4.3% of the people with congenital hearts defects [1]. Much less frequently, an anomalous right superior vena cava (SVC) connects to the LA [2]. However, patients are often asymptomatic because a greater volume of venous blood returns by way of the inferior vena cava, empties into the right atrium and oxygenated normally. Accompanying lung infection or metabolic conditions in which stress due to hypoxia occurs, because the symptoms arise. Usually, an important finding is cyanosis, but it may not be detected in these patients, and this can lead the right to left shunt to be overlooked. Transthoracic echocardiography that is performed in suspicion of congenital anomalous of the heart chambers is in most cases normal.
When we scan the publications written in English have found 14 adult patients who have been published so far. Here, in an adult patient who presented with cyanosis after pneumonia, an abnormal drainage from superior vena cava to left atrium was shown by computerized thorax tomography. We wanted to present this phenomenon because of being asymptomatic until adulthood and accompanying venous return anomaly with right superior vena cava draining into the left atrium. A review of previously reported cases of the anomaly is being discussed.
Case Report
31-years-old male patient with a cough and shortness of breath that started ten days ago, has been prescribed antibiotic and bronchodilator therapy. However, due to the cyanosis of the hands and lips after the treatment, the patient was referred to our hospital. In physical examination, general condition was good, his vital signs were: blood pressure was 130/80 mmHg, heart rate 108 per minute, temperature 37.9 °C, respiratory rate of 18 breaths per minute and oxygen saturation was 89% on room air, but the lips and hands were cyanotic. Existing cardiac sounds were normal, but at the lower left basal lung segment, there were coarse crackles. The abdomen was relaxed, there was no organomegaly, no pretibial edema, and peripheral pulses were palpable. Laboratory results showed hemoglobin level was 17.7 g/dL and Alanine Aminotransferase (ALT) levels was slightly elevated.
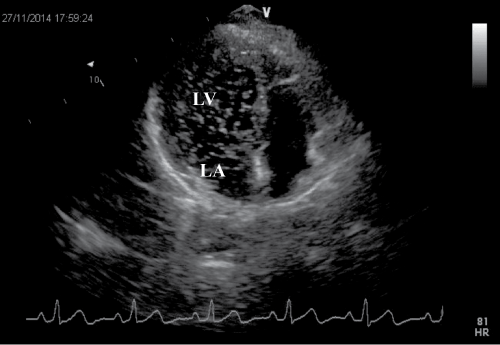
12-lead Electrocardiography (ECG) showed normal sinus rhythm. In chest radiography, normal cardiothoracic index was found with a density increase in the lower left lung. Transthoracic Echocardiography showed that heart chambers, ejection fraction, and pulmonary artery pressure were normal. A two-dimensional contrast echocardiogram using the injection of an agitated saline solution into right and left antecubital vein revealed a prompt appearance of the contrast in the left atrium and left ventricle (Figure 1). Chest Computed Tomography (CT) obtained after contrast material injection into the right arm vein confirmed the right-to-left shunt caused by the right-sided superior vena cava (SVC) draining into the left atrium (Figure 2C). Also, this CT scan showed a right upper (RUPV) (Figure 2A) and middle pulmonary vein (RMPV) (Figure 2B) draining into the right SVC. Cardiac catheterization was performed by introducing a catheter into the right femoral vein; that could easily be passed through the inferior vena cava into the right atrium. However, it could not be advanced out of the right atrium into the superior vena cava (Figure 3), and contrast injection into the right atrium revealed a dead end at the cranial portion and the absence of the superior vena cava in its normal position. The catheter was passed from the right atrium into the right ventricle and into both pulmonary arteries, which appeared to be normal. A second catheter was introduced into the right cubital vein and passed into the superior vena cava. Contrast media injected into the superior vena cava then opacified the left atrium, left ventricle and aorta, in that order. An arterial catheter was introduced into the left femoral artery and passed through the ascending aorta into the left ventricle. No gradients were present (Table 1). Selective coronary arteriography showed no evidence of obstructive coronary artery disease. A diagnosis of anomalous drainage of the right superior vena cava into the left atrium with resultant right-to-left shunt was made. There was no atrial septal defect. A diagnosis of isolated drainage of the superior vena cava into the left atrium was made, and the patient was submitted to surgery.
.
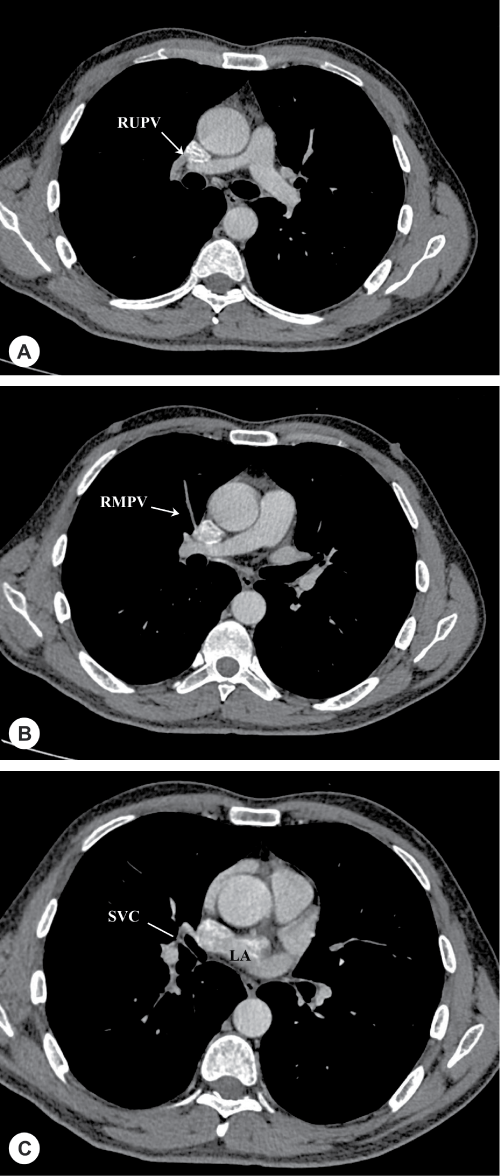
Figure 2: Contrast-enhanced chest computed tomography reveals an anomalous right superior vena cava draining into the left atrium. There is also partial anomalous pulmonary venous drainage of the right upper pulmonary vein (RUPV). (A) and right middle pulmonary vein (RMPV); (B) into the superior vena cava (SVC) with normal drainage of the right superior vena cava into the right atrium. LA: left atrium.
View Figure 2
.
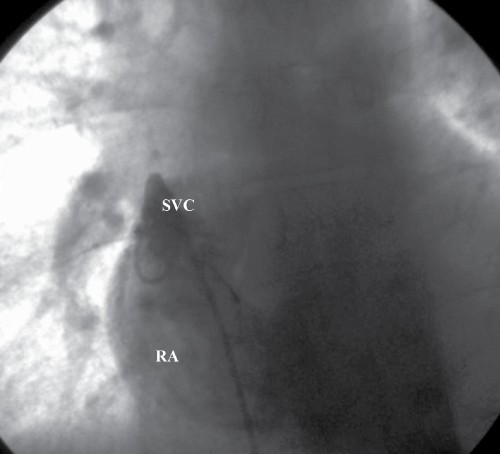
Figure 3: Cardiac catheterization shows the catheter could not be advanced out of the atrium into the superior vena cava, and contrast injection into the right atrium revealed a dead end at the cranial portion and the absence of the superior vena cava in its normal position.
View Figure 3
Surgery
The chest was opened through a median sternotomy incision. Venous cannulation made of the where opening location proximal pulmonary veins to the superior vena cava from the innominate vein and the inferior vena. The right atrium was opened. There was no atrial septal defect. The atrial septum was incised superiorly with the incision extending into the superior vena cava. A pericardial patch was formed so as to divert the superior vena cava blood into the right atrium and the pulmonary venous return into the left atrium. The right atrium was also patched with the pericardium to increase its size. The right atrium was closed. Post- operative transesophageal echocardiography was performed and pulmonary veins and superior vena cava stenosis were not observed.
Discussion
In 1975, de Leval and colleagues reported that only 28 of 5,127 consecutive congenital cardiac patients had SVC drainage into the LA, and all 28 instances were associated with other cardiac anomalies. There have been 19 reported cases of right SVC drainage into the LA, mostly in children who had mild hypoxemia and cyanosis [1]. In the literature, there are very rare case series of superior vena cava to the left atrium drainage diagnosed over the age of 18. The age of reported cases varies between 22 and 84 years (Table 2).
![]()
Table 1: Arterial catheter findings.
View Table 1
![]()
Table 2: Findings of previously reported cases including primary diagnostic tools and therapeutic approaches.
View Table 2
Patients usually present with shortness of breath, chest pain, brain abscess or mild cyanosis. In our case, there was shortness of breath and cyanosis. Except for symptomatic patients presenting to the emergency department, it can be found in asymptomatic patients infrequently. The patient Baggette C. and colleagues published in their case was a 34-year-old hypoxemic woman who admitted to the hospital for her third childbirth [2]. They avoided radiological examinations due to the pregnancy, and contrast echocardiography and cardiac magnetic resonance imaging were performed. We primarily used non-invasive tests to confirm the right-to-left shunt. For the demonstration of the right-left shunt, contrast echocardiography was performed. When agitated saline injected via a right arm vein, it immediately opacified the left atrium and left ventricle without any microbubbles in the right heart (Figure 1). Agitated saline via a left arm vein produced the same result. In cardiac catheterization, contrast injection via a right femoral venous line confirmed inferior vena cava connection to the RA, but the right superior vena cava was displayed as a stump (Figure 2).
The drainage of right superior vena cava to the left atrium was firstly diagnosed by Wood and colleagues in 1956, by the cardiac catheterization of a ten years old girl who presented with cyanosis [3]. Until 1980's, the first diagnosis was done by catheterization or radionuclide angiography options, after the start of widespread use of echocardiography in the diagnosis ıt has become the first non-invasive tests [4]. Cardiac MRI was used for the first time used by Rosenkroz, et al. [5] in 1988, and contrast enhanced thorax CT was used by Aminololama-Shaker, et al. [6] in 2007, they are both reliable noninvasive methods being used for the identification of this disease. Our patient was diagnosed using invasive and non-invasive methods as well to be complementary to each other.
22-years-old patient, the first case to be defined in adulthood by Park, et al. who diagnosed technetium 99 m macroaggregates with albumin has used radionuclide angiography [7]. In approximately half of the patients, because the first symptoms are shortness of breath and chest pain, studies directed at for pulmonary embolism. An abnormal venous return was suspected when radionuclide distribution in the left heart chambers and arterial system was seen injected in the upper arm [5,8-10].
In adults, this anomalous most likely to be presented with cyanosis after related lung disease. Such being that, it was considered which disease lead to the cyanosis, example methemoglobinemia, hemoglobinopathies, Ebstein's anomaly, eisenmenger's syndrome, congenital pulmonary arteriovenous [6]. Drainage of the superior vena cava into the left atrium is frequently associated with other cardiac or extra cardiac malformations that particularly affect the pattern of circulation. Cardiac defects include atrial and ventricular septal defect, single atrium or single ventricle, Eisenmenger's complex, Fallot's tetralogy and transposition of the great vessels. Extracardiac abnormalities associated with this anomaly include coarctation of the aorta, pulmonary arterial venous fistulae, patent ductus arteriosus and abnormalities of the inferior vena cava. Once a diagnosis of the superior vena cava entering the left atrium is made, these commonly associated malformations should be excluded. None of these abnormalities was found in this patient [7]. When literature was scanned in three patients, persistent left superior vena cava anomaly with right superior vena cava drainage into the left atrium was reported [11-13]. In our patient, the upper and middle right pulmonary veins pouring out the superior vena cava and another anomaly were not detected.
Although the exact embryological mechanism is not known, there are various discourses. In 2003, Van Praagh and associates reported observations from echocardiographic and postmortem anatomic findings in instances of multiple sinus venosus defects [14]. An SVC type of sinus venosus defect was believed to result from a deficiency in the wall that was shared by the right SVC and the right upper pulmonary veins. The interatrial communication of a sinus venosus defect is not a defect in the atrial septum; rather, it involves drainage of the LA orifice of unroofed pulmonary veins into the right SVC or right atrium. An isolated right SVC-to-LA anomaly forms upon a combination of predominant blood flow between those structures and an atresia that affects the right SVC-to-right atrial orifice [14].
Patients with this connection between venous and arterial system, are at high risk for brain abscess and paradoxical embolism [15]. In adults, it can be diagnosed with a cerebral embolism or brain abscess and presents with cyanosis, cardiomegaly, dyspnea [7,8,11,12,15]. Among patients who diagnosed in adulthood that right SVC drained into the LA, 20% of them had brain abscesses [8,11,16]. Therefore, surgical intervention should be planned when the diagnosis is confirmed. Our patient presenting with cyanosis has not yet developed such complications.
Conclusion
In summary, we believe that any patient with unexplained cyanosis, hypoxemia, brain abscess, shortness of breath and stroke should undergo contrast echocardiography. In the case of RSVC into the LA, cardiac catheterization should be performed to rule out other intracardiac lesions and to evaluate pulmonary venous drainage, and right ventricular size. The diagnosis of this anomaly in our patient was made predominantly from the noninvasive studies. Computed tomography or magnetic resonance imaging may be required for confirmation of the side of the SVC and visualization of the anomalous right PV and for detecting other congenital anomalies.
Regardless of clinical presentation, surgical correction is indicated once the diagnosis of systemic venous connection to the LA is determined [11]. Of note, intravenous infusions that use veins of the upper body should be avoided once a patient with this anomaly is recognized [17].
References
-
de Leval MR, Ritter DG, McGoon DC, Danielson GK (1975) Anomalous systemic venous connection. Surgical considerations. Mayo Clin Proc 50: 599-610.
-
Baggett C, Skeen SJ, Gantt DS, Trotter BR, Birkemeier KL (2009) Isolated Right Superior Vena Cava Drainage into the Left Atrium Diagnosed Nonivasively in the Peripartum Period. Tex Heart Inst J 36: 611-614.
-
Wood PH (1956) Diseases of the heart and circulation. (2nd edn), Lippincott, Philadelphia, 457.
-
Park HM, Smith ET, Silberstein EB (1973) Isolated right superior vena cava draining into left atrium diagnosed by radionuclide angiocardiography. J Nucl Med 14: 240-242.
-
Rosenkranz S, Stablein A, Deutsch HJ, Verhoeven HW, Erdmann E (1998) Anomalous drainage of the right superior vena cava into the left atrium in a 61-year-old woman. Int J Cardiol 64: 285-291.
-
Aminololama-Shakeri S, Wootton-Gorges SL, Pretzlaff RK, Reyes M, Moore EH (2007) Right-sided superior vena cava draining into the left atrium: a rare anomaly of systemic venous return. Pediatr Radiol 37: 317-320.
-
Park HM, Summerer MH, Preuss K, Armstrong WF, Mahomed Y, et al. (1983) Anomalous drainage of the right superior vena cava into the left atrium. J Am Coll Cardiol 2: 358-362.
-
Nazem A, Sell JE (1993) Closed technique for repair of right superior vena cava draining to left atrium. Ann Thorac Surg 55: 1568-1570.
-
Pretorius PM, Gleeson FV (2004) Case 74: Right-sided Superior Vena Cava Draining into Left Atrium in a Patient with Persistent Left-sided Superior Vena Cava. Radiology 232: 730-734.
-
Theron A, Paule P, Metras D (2009) Right superior vena cava draining into the left atrium, associated with abnormal pulmonary vein drainage. Archives of Cardiovascular Disease 102: 249-250.
-
Schick EC Jr, Lekakis J, Rothendler JA, Ryan TJ (1985) Persistent left superior vena cava and right superior vena cava drainage into the left atrium without arterial hypoxemia. J Am Coll Cardiol 5: 374-378.
-
Leys D, Manouvrier J, Dupard T, Kassiotis P, Rey C, et al. (1986) Right superior vena cava draining into the left atrium with left superior vena cava draining into the right atrium. Br Med J 293: 855.
-
Courand PY, Girerd N, Chauveau S, Chevalier P (2013) Right superior vena cava drainage into the left atrium revealed by multiples strokes after pacemaker implantation. Heart Rhythm 10: 1735-1736.
-
Van Praagh S, Geva T, Lock JE, Nido PJ, Vance MS, et al. (2003) Biatrial or left atrial drainage of the right superior vena cava: anatomic, morphogenetic, and surgical considerations-report of three new cases and literature review. Pediatr Cardiol 24: 350-363.
-
Shapiro EP, Al-Sadir J, Campbell NP, Thilenius OG, Anagnostopoulos CE, et al. (1981) Drainage of right superior vena cava into both atria. Review of the literature and description of a case presenting with polycythemia and paradoxical embolization. Circulation 63: 712-717.
-
Hong SN, Nayar A, Srichai MB, Morgan JA, Meyer D, et al. (2011) A Case of an Anomalous Superior Vena Cava with Anomalous Pulmonary Veins-When Two Wrongs Do not Make a Right. Echocardiography 28: 39-41.
-
Ezekowitz MD, Alderson PO, Bulkley BH, Dwyer PN, Watkins L, et al. (1978) Isolated drainage of the superior vena cava into the left atrium in a 52-year-old man: a rare congenital malformation in the adult presenting with cyanosis, polycythemia, and an unsuccessful lung scan. Circulation 58: 751-756.
-
Alexis Theron, Philippe Paule, Dominique Metras (2009) Right superior vena cava draining into the left atrium, associated with abnormal pulmonary vein drainage. Archives of Cardiovascular Disease 102: 249-250.
-
David Cohen, Jonathan Reiner, Jalil Ahari, Jannet Lewis (2013) Isolated Right Superior Vena Cava Into the Left Atrium Detected by Contrast Echocardiography. Circulation 128: 1129-1130.