Clinical Medical
Reviews and Case Reports
Some Diagnostic Aspect on Abnormal Nitric Oxide Metabolism and Some Pharmacological Aspects of the most used Drugs in Rheumatoid Arthritis
Dejan Spasovski*
Department of Rheumatology, University Clinical Centre, Republic of Macedonia
*Corresponding author: Dejan Spasovski, Department of Rheumatology, University Clinical Centre, Skopje, Republic of Macedonia, E-mail: drspasovski@yahoo.co.uk
Clin Med Rev Case Rep, CMRCR-2-046, (Volume 2, Issue 7), Research Article; ISSN: 2378-3656
Received: July 10, 2015 | Accepted: July 28, 2015 | Published: July 31, 2015
Citation: Spasovski D (2015) Some Diagnostic Aspect on Abnormal Nitric Oxide Metabolism and Some Pharmacological Aspects of the most used Drugs in Rheumatoid Arthritis. Clin Med Rev Case Rep 2:046. 10.23937/2378-3656/1410046
Copyright: © 2015 Spasovski D. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: To evaluate the diagnostic test for Assymetric Dimethyl Arginine (ADMA), rheumatoid factor (RF), C-reactive protein (CRP), Disease Activity Score with 28 joint ( DAS 28 index ), and to define the effect of untreated rheumatoid arthritis on endothelial function. In order to determine whether ADMA changes depending on the disease evolution, ADMA was used as an indicator for endothelial dysfunction in subclinical atherosclerosis.
Methods: Using a ELISA technology of DLD-Diagnostika-GMBH for detection of ADMA, the samples of serum and urine have been examined in 70 participants (35 RA who were not treated, 35 healthy controls). RF was defined with the test for agglutination (Latex RF test) in the same participants.
Result: Out of 35 examined patients with RA, RF appeared in 18 patients (sensitivity of the test 48.57 %), while ADMA is positive in 20 patients (sensitivity of the test 57.14 %) in the same group. In 23 of the 35 examined patients with RA, we found presence of anti-citrulinated peptide antibodies (anti-CCP2 ) from the second generation (anti-CCP2 antibodies ) (sensitivity of the test 65.71%). There is association between ADMA and anti-citrulated peptide antibodies (anti-CCP2 ) from the second generation in early RA (p<0.05).
Conclusion: ADMA higher sensitivity than RF in the detection of asymptomatic subclinical lesions in untreated RA. ADMA has equal sensitivity and specificity from RF in untreated RA.
Keywords
Asymmetric dimethyl arginine, Rheumatoid arthritis, Rheumatoid factor
Introduction
Pathophisyological role of ADMA
Cardiovascular Disease (CVD) is main reason for mortality in RA in literature. About 80% of the cardiovascular strokes are explained with the traditional risk factors such as hypercholesterolemia, hypertension, cigarettes and diabetes mellitus. Vascular endothelium has a great role in the appearance of early functional changes in vascular wall, which initiate and promote atherogenesis, as well as a central role in maintenance of physiological vascular tonus and structures. The role of regulation of vascular structure and function is mostly through formation of endothelial nitric oxid (NO), which is one of the main mediators liberated from the healthy endothelial cells. Except potent vasodilatation effect, NO acts as an endogenous inhibitor of platelet aggregation; it inhibits adhesion of monocytes and leucocytes in normal vascular endothelium, and also inhibits proliferation of vascular smooth muscle cells. It diminishes vascular liberation of superoxide radicals which are involved in inflammatory and cytokine processes as well as in inhibition of LDL oxidation. NO is also called endogenous anti-atherogenous molecule. In the in-vivo investigations, cultures with human endothelial cells in presence of ADMA produce O2. It confirms the hypothesis that ADMA interferes with NOS synthesis. Monocytes of patients with hypercholesterolemia, in culture, adhere stronger to endothelium in comparison with monocytes of patients with normocholesterolemia. The monocyte hyperathession is normalised with supplements of L-arginine. This shows that competitive displacement of endogenous L-arginine from ADMA is reason for this pathologic situation [1].
Role and significance of endothelial cell in maintenance of endothelial integrity
In the regulation and control of vascular tonus and blood perfusion endothelial cell has direct influence through smooth muscle cells in blood vessels. This is realized through synthesis and liberation of vasoactive substances which participate in contraction or relaxation of the smooth muscles. Most important are: Endothelial relaxing and hyperpolarized factor (EDRF, EDHF), Endothelin1 (E1), Prostacyclin (prostaglandine (PGE2). Proliferative effect of smooth muscle cells and fibroblasts is realised through factors for growth and cytokines, such as IL-1, IL-6, colony stimulating factors, platelet growth factor. They take part in the process of coagulation through processes of platelet aggregation and adhesion, which are realised through thrombomoduline, anithrombin 3, protein C. The activated endothelial cell as well as activated T lymphocytes and macrophages, produces TNFα, stimulates the adhesion of leucocytes for endothelium through adhesion molecules: E-selectin, P-selectin, L-selectin, intracellular adhesion molecule (ICAM-1), vascular cellular adhesion molecule (VCAM-1), endothelial leukocyte adhesion molecule (ELAM-1). They take part in the synthesis of the components of the basal membrane through creation of fibronectins, von Willebrandt factor (vWF), proteoglycans. Activated smooth muscle cells in arterial walls produce monocyte hemoatractant protein (MCP-1), which makes monocytes to migrate towards the intima. All these promote macrophage and lipid accumulation, the appearance and the beginning of growth of atherosclerotic plaque, especially present in RA, because of the chronic inflammation expressed through C-reactive protein (CRP). Normally, there is balance between relaxing and contracting factors that participate in the maintenance of the normal diameter of the blood vessels, aiming to maintain normal blood perfusion.
Many different stimuli make the endothelial cells to produce EDRF, substrate, known to be NO. It causes endothelial relaxation through activation of soluble guanilat ciklase and formation of cyclic 3, 5 guanosine monophosphate (3,5GMP). It results with the inhibition of liberation of Ca2+ from cellular depots, i.e. inhibition of its entrance through receptor channels in smooth muscle cells, which causes relaxation of the muscle tonus. Synergistically, PGE2 realises endothelial relaxation through the increase of the cyclic adenosine monophosphate (cAMP), through adenil cyclase. It inhibits platelet adhesion and relaxation [2-5].
Normally, in arterioles dominate endothelial relaxing factors, while in venules endothelial contracting factors. In normal individuals balance between mutual interactions are kept with physiological vasoconstriction, and not pathological vasospasm, or physiological vasodilatation, and not pathological hyperemia. Two local mechanisms are described to be involved in the regulation of the micro-vascular resistance:
1. Pressure sensitive myogenic mechanism
2. Metabolic vasoregulation, which through changes in resistance influences the blood supplying.
In the intact endothelial cells are present α2-Adrenoreceptors, which once stimulated produce EDRF or NO. They are present in coronary microcirculation, located on the endothelial cells, especially in little coronary arterioles <100μm in diameter.
A lot of substances influence in the liberation of dilator or constrictor substances, with mutual complex interactions. Substances may originate from circulation and in the same time to activate receptors of the endothelial cells, but also may originate from perivascular nerves [6-10]. The hemorheolitics depend on the blood viscosity, proportions of the formed blood elements and their morphology, on the thermoregulatory effect mechanisms, as well as on the circulatory hormones: catecholamins, angiotensin 2, oxitocine, insulin, that influence the tonus of the smooth muscle wall through activation of the receptors of the endothelial and smooth muscle cells, as well as through sympathetic nerve endings.
Diagnostic and prognostic meaning of biomarkers
In contemporary medicine there is tendency in finding most specific and most sensitive biomarkers as indicators of disease and as diagnostic tools for follow-up of treatment and success of therapy. Aiming from the group of potential biomarkers to chose those which are most significant in clinical practise and which give best diagnostic information, extensive examinations are necessary, like determination of analytical, clinical and economic implementation of them. Successful biomarker has to fulfil several conditions.
1. Its concentration to be relatively high in certain tissue, while irrelevant in other.
2. To have suitable sub-cellular distribution; to be found quickly in the examined solution after cell damage.
3. To be constant long enough to be able to follow its concentration.
4. To be determined by available, suitable and sensitive analytical methods, which give quick results.
5. To exist cut-off values, taking in consideration clinical sensitivity, specificity, and their accuracy.
In the introduction of every new diagnostic method it is necessary to assess its quality i.e. to find the usefulness of the information that should be compared with the risk for the patient and the price of the test. This is present in the last few years, when due to the technologic development a lot of diagnostic methods are introduced. Although subjective assessment of the doctor responsible for the patient is decisive in the choice of the diagnostic method offered, one objective quantitative evaluation of every method would help for most rational approach. The contribution which gives every method, quantitatively expressed, would be able also to classify methods according to their efficacy, but also to compare diagnostic values in laboratory variables, to show quantitative evaluation of the diagnostic test or test of distribution, defining sensitivity, specificity, predictive values for positive and negative test, as well as accuracy of the test for examined variables in non treated RA.
In the last few years, great attention is given to the evaluation of NO endothelial dysfunction i.e. ADMA, as non invasive marker for assessment and early detection of atherosclerosis. Criteria that make ADMA suitable for proving for certain abnormalities in the function of the endothelium are:
- Low level of the present substance in physiological conditions.
- Sensitive method for determination of the activity of the product in serum.
- High concentration of the examined product in RA.
- Visible increase of the activity during damage of the endothelium and its structures.
Some mathabolitical aspect of ADMA and sublicinal atherosclerosis
Fast development of the medical science put the doctor in safer situation, giving him strong diagnostic and therapeutic tools, but in the same time put him in very complicated and difficult problems. Such complicated problem is the appearance of atherosclerosis in RA, i.e. the possibility of its detection in its asymptomatic phase.
The endothelial function could be evaluated with numerous methods such as immunologic, radiologic, cytologic analyses, but important role plays also biochemical methods as non-invasive with great importance for early detection of certain pathological conditions such as conditions for onset of clinical appearances and situations. Among them an important role plays determination of the activity of derivatives and their isoforms in serum. Pathogenetic mechanisms responsible for the destruction and dysfunction of the endothelial cells are: immunological mechanisms antibody-mediated, compliment, pro-inflammatory cytokines, reactants of the acute phase, cell components, adhesion molecules, but also toxic substances and drugs.
There are methods for estimation of atherosclerosis, roughly divided to non-invasive: oscilometry, pletismography, thermometry, using flowmetry through dilatation or vascular dopller technology, computational tomography and magneting resonance angiography, radioactive isotopes, and invasive: angiography; with their advantages and disadvantages. They are important when disease is in advanced pfase, with changes in blood perfusion and appearance of subjective difficulties urging the patient to ask for medical help.
There are several biomarkers as indicators for endothelial dysfunction, such as endothelial vasoactive substances, leukocyte adhesion substances, pro-inflammatory cytokines, prostaglandines, and reactants of the acute phase, hormones, and enzymes etc., everyone with its own importance in the functioning of the blood vessels. ADMA is the unique substance on which depends the multi-functional role of NO, but as endogenous anti-atheogenic molecule. Direct effect in the auto-regulation: of the normal myogenic activity and vasomotion (potent vasodilatator effect), adhesion (inhibition of the platelet aggregation, inhibition of adhesion of the monocytes and leukocytes in normal vascular endothelium), proliferation (inhibition of proliferation of vascular smooth muscle cells), with basic aim-achievement and maintenance of trans-muscular, capillary pressure. Indirect effect of the process of atherosclerosis: it decreases vascular liberation of superoxide radicals involved in the inflammatory and cytokine processes, and inhibition of LDL oxidation.
Until recently ADMA was detected with liquid chromatography, making it complex, inaccessible, technologically dependent and expensive. With introduction of ELISA method in detection of ADMA, determination becomes more accessible and more practical.
There is strong association between ADMA and anti-cyclic citrulated peptide antibodies (anti-CCP2 ) from the second generation, in early RA without cardiovascular risk factors as result of the activity of disease and inflammatory activation [11].
There are confronting results from the effect of DMARDs and improvement of endothelial dysfunction. They improve the disease activity expressed through Disease activity index with 28 joint (DAS 28 index) and microcirculation, but do not decrease significantly the level of ADMA in RA [12]. In some of them, corticosteroids are with dual effect, potentially positive in comparison with the level of inflammation, but also negative (dyslipidemia, hypertension, hyperglycemias, insulin resistance) on the onset and course of the endothelial dysfunction, while some biological DMARDs targeted towards one mediator of the immune reaction (IL-6,TNFα disturb lipid profile, to the level of statins necessity. Co-morbidities, like osteoporosis, present in long-term use of CSs, with the use of Ca supplements, with their influence on atherosclerosis, emphasize necessity of processing and throw off the mask of the problem [13]. There are no reports in the Republic of Macedonia or in the Clinic for Rheumatology as evidence that the problem has been processed.
Taking in consideration great attention given to the prevention in contemporary medical but also rheumatology science, the necessity of investigation of the dependence of the presence of biomarkers of endothelial dysfunction with the activity of the disease is imposed, with basic aim to serve latter as early indicator for assessment of early, asymptomatic endothelial dysfunction, occurring in the absence of manifest CVD and is not connected with traditional atherosclerotic risk factors. ADMA is endogenous NO inhibitor and is new independent risk factor for endothelial dysfunction and CVD [14].
Some pharmacological aspects of the most used drugs in RA
Cardiovascular morbidity and mortality in RA could be explained with several mechanisms:
1. Chronic inflammation.
2. Increased prevalence of traditional cardiovascular risk factors, including dyslipoproteinemia.
3. Decreased use of statins.
4. Chronic treatment of RA with steroids.
It is difficult to make a difference between the role of pharmacological treatment on one hand and strength and duration of the disease on the other hand, because these parameters are closely connected.
Atherosclerosis is accelerated and supported by the selective cyclo oxygenase 2(COX-2) inhibitors, as well as non-selective NSAID. They increase the risk of CVDs and cerebro-vascular conditions [15-17].
Corticosteroids (CSs): Widely used drugs in the treatment of RA with anti-inflammatory effect. They increase the triglyceride concentration, induce hypertension and diabetes. But, their role in the degree of appearance atherosclerosis is for discussion. They decrease the risk for cardiovascular morbidity, but with less effect than the other DMARDs [18].
CSs have dual effect; potentially positive (anti-inflammatory), but also potentially negative (dyslipidemia, hypertension, hyperglycemias, insulin resistance). They are also dose dependant; low doses stabilise atherogenic lipid profile of RA, but there is also individual variability in the acceleration of the atherosclerosis [19]. Most studies show that corticosteroids do not increase cardiovascular risk in RA, but there is an increased incidence of carotid plaques in RA [20].
Synthetic DMARDs: Methotrexate (MTX) does not change the lipid profile in treated patients with RA. After 1 year the atherogenic index is improved. It decreases the risk for cardiovascular morbidity and mortality in treated patients with RA. MTX interferes with folate metabolism through inhibition of dihydrofolate reductase. MTX induce 5-methyltetrahydrofolate depression with secondary decrease of remetylation of homocistein in methionin. Theoretically, MTX can decrease S-adenosylmethionine (SAM) dependant methylation reaction with successive decrease of ADMA plasma level. But, the level of ADMA is not changed in these patients besides the use of folate supplements and B vitamins (B6 and B12) [21-24].
Biological DMARDs: Tocilizumab (TCZ); anti-interleukin 6 (IL-6) receptor antibody. Lipid parameters in 6 months follow-up in controlled clinical conditions are increased like total cholesterol, triglycerids, LDL cholesterol and/or HDL cholesterol. About 24% of patients that receive TCZ show elevation of total cholesterol ≥6.2mmol/L; and in 15% increase of LDL cholesterol ≥ 4.1mmol/L. Parameters are stabilized with the use of suitable drugs like statins. But, after 5-year-follow-up of the drug, the atherogenic index (total cholesterol/HDL cholesterol) or log (triglicerids/HDL cholesterol) is stabile. The increase of the total cholesterol not always means increased risk of CVD. Similar happens with the lipid profile in the use of other anti TNFα biological antibodies (Inflximab,Remicade); Etanercept; Adalimumab) [25-27].
Material and Methods
This is a prospective cross-sectional study, which is performed in the University Clinic for Rheumatology, Skopje. In this study 35 patients was included, and 35 healthy individuals, age 18 to 65 years. They were divided in 3 groups.
I. group: 18 patients with RA, newly diagnosed and not treated, Rheuma factor positive (RF +), anti-cyclic cetrulated peptide antibodies (anti-CCP2 ) positive.
II. Group: 17 patients with RA, newly diagnosed and not treated, Rheuma factor negative (RF -), anti-cyclic citrulated peptide antibodies (anti- CCP2) positive.
III. Group: 35 healthy individuals.
The activity of RA were determined on the base of clinical and biochemical parameters. Examination was performed in 0-time.
Selection criteria: all examined individuals that participate in this study, is men and women that voluntarily take part, so that ethical criteria for making this study is satisfied. It was approved by the Ethical Committee of the Medical Faculty in Skopje.
Including criteria
In this study are included patients with RA, age 18-65, newly diagnosed and not treated.
The diagnosis of the disease is made on the revised diagnostic criteria for classification of RA suggested in 1987 by the American Rheumatology Association (ARA) [28]. In order to include the patient in the group with RA, he should satisfy 4 of the 7 provident criteria. Criteria from 1 to 4 have to be present at least 6 months.
Changes in the evolution of disease, i.e. clinical improvements would be assessed through suitable indexes of activity (clinical parameters) (Disease Activity Score-DAS 28) [29-32]. The index uses mathematical formula in order to get unique composite quantitative score composed of palpatory painfully- sensitive joints (maximal score 28), swollen joints (maximal score 28), Westergren Eritrocite Sedimentation Rate (ESR) and patients global evaluation for disease activity (0-100mm Visual Analogue Scale - VAS).
DAS 28 index ranges from 0 to 10 and score bellow 3.2 qualifies the disease as low active.
DAS 28: 0.56 0.56 -28 palpatory painfully- sensitive joints + 0.28 -28 swallen joints + 0.70 (logn ESR) + 0.014 (global estimation of the patient for disease activity: VAS 0-100).
In the same time reactants of the acute phase like CRP, Erythrocyte Sedimentation Rate (ESR) is used.
Excluding criteria
From the study is excluded all patients/individuals with diseases or conditions that could directly or indirectly influence changes of the endothelial functions, like:
1. Patients with past history for disease of the spleen, liver damage, renal, hematological, cardiological, neurological, lung injuries, auto-immune diseases, AIDS, age <18 years.
2. Patients in whom in 0-time is found increased level of glycose, degradation products, like serum and urine creatinin, serum urea, hypertension that affect lipid profile, such as smoking, diabetes, hypothyreosis, Cushing's syndrome, obesity (body mass index>30), with family history of dyslipidemia.
3. Patients with acute infections, malignant diseases, febrile conditions.
4. Patients previously treated with some basic drug for RA, including corticoseroids and nonsteroid antiinflamatory drugs (NSAIDs).
5. Patients with hypertension, uric gastritis, urinary infections, Systemic lupus erythematosus, mixed connective tissue disease, vasculitis, systemic sclerose, primary and secondary Raunaud phenomenon, periferal vascular diseases, congenital CVD.
6. Patients treated with anti-hypertensive, anti-diabetic and cardiologic therapy, drugs for decrease of the lipid profile, oral contraceptives, estrogens, progesterone, tocopherol (vitamin E).
7.Patients previously blood transfused, changes in hematological parameters or enzymatic status.
Biochemical examination
The standard routine laboratory examination is performed in the Institute for Clinical Biochemistry: blood count (erythrocytes, leukocytes, platelets, hemoglobin, hematocrit, blood differential), alkaline phosphatase, alanine aminotransferase, aspartate aminotransferase, creatin kinase, lactate dehidrogenase, glycemia, urea/serum, creatinine/serum, Asymetric dimetil L-arginin (ADMA).
Reactants of the acute phase (ESR, RF, CRP and anti-CCP2 ) are performed in the University Clinic for Rheumatology.
1. Determination of the activity of Asymetric dimetyl L-arginine (ADMA): ELISA method (DLD-diagnostics, GMBH) - Enzyme immunoassay: for quantitative determination of the endogenous Asymetric dimetyl L-arginine (ADMA) in serum or plasma. Principle: ADMA is adhered in solid phase on micro-titer plate. ADMA standard, samples and positive control are pre-acilated, in combination with rabbit anti-N-acyl-ADMA, incubated 15-20h at 2-8°C. After that they are washed, and second antibody is added, anti-rabbit IgG, conjugated with peroxidase. After 1 hour incubation on room temperature they are washed. In order to achieve colour, tetramethyl benzidine is added as a substrate solution (TMV). After 20-30 minutes incubation it is stopped with adding sulphur acid. The absorbtion is read on 450nm on automatically micro-titar reader. With the standard figure is determined ADMA concentration. Basically, the quantity of antibodies adhered in the solid phase of ADMA is reverse proportional to the concentration of ADMA in the samples.
2. Determination of the C-reactive protein (CRP) with test for agglutination (Latex CRP test).
3. Determination of Rheumatoid factor (RF) with test for agglutination (Latex RF test).
4. Determination of the Erythrocyte Sedimentation Rate (ESR) with quantitative method of Westergren.
5. Determination of anticyclic citrulated peptide antibodies (anti-CCP2 ) with semi-quantitative/qualitative ELISA technique, based on detection of IgG auto-antibodies in human serum or plasma, directed towards synthetic Cyclic Citrulated Peptides (CCP) that contain modified arginine residues.
6. Determination of blood count and differentia with haematological electronic Counter Cobas Micros ABX (Roche haematology) and Sysmex KX-1.
7. Determination of alkaline Phosphatase (AP) with kinetic method.
8. Determination of Alanine Aminotransferase (ALT) with kinetic UV method.
9. Determination of Aspartate Aminotransferase (AST) with kinetic UV method.
10. Determination of creatine phospho kinase (CPK) with kinetic UV method.
11. Determination of lactate dehydrogenase (LDH) with kinetic UV method.
12. Determination of glycemia: enzymatic method with glucose-oxidase (GOD) and 4-aminophenason (PAP).
13. Determination of total lipids with the method by "Zolner and Kirsh".
14. Determination of triglycerides with enzymatic colorimetric Pap method.
15. Determination of total cholesterol in serum with enzymatic chod pap method.
16. Determination of HDL and LDL cholesterol with photometric chod pap method.
17. Determination of serum urea with the method by "Kassier".
18. Determination of serum creatinine with the method by "Jaffe".
Stastical analysis
The results is statistically processed with the following statistical methods and shown with statistical package Statististica 7.0.
-Test for sensitivity and specificity, predictive values for positive and negative results and accuracy;
- Statistical series according to all defined variables of interest is shown with tables and figures;
- Analysis of the structure of numeric series is made by the measures of the central tendency (average) and measures of dispersion (standard deviation);
- Analysis of the structure of the attributive statistical series is made by coefficients of correlations and proportions;
- Analysis of correlation between numeric statistical series is made by Pearson's coeficient of correlation - p;
- Analysis of correlation between attributive statistical series is made by Pearson's χ2 -test.
- To test the significance of differences between two arithmetical medians i.e. proportions Student's t-test is used;
- To test the significance of differences among three or more arithmetical medians Analysis of variance (ANOVA) is used.
Results
The ever growing prevalence of the CVD, not only in RA, but also the use of drugs that change the disease activity in disease treatment, contributes to the deepening of the investigations towards finding easy, cheap, practical screening method, in order to detect the early stadium of disease of the endothelium (Figure 1).
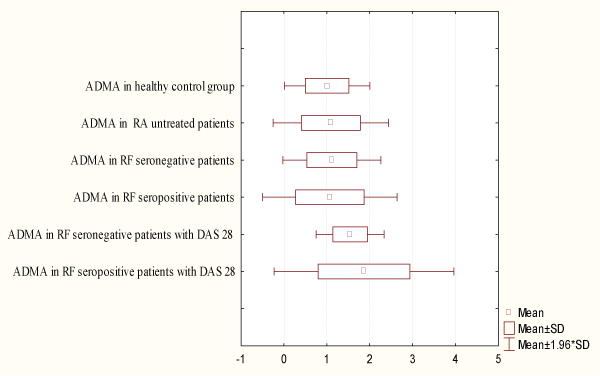
.
Figure 1: Distribution of Asymmetric Dimehylarginine (ADMA) in serum with and without Disease Activity Score (DAS28)
View Figure 1
Out of 35 examined patients with RA, RF appeared in 18 patients (sensitivity of the test 48.57 %), while ADMA is positive in 20 patients (sensitivity of the test 57.14 %) in the same group. In 23 of the 35 examined patients with RA, we found presence of anti-CCP2 antibodies (sensitivity of the test 65.71%) in table 1 and table 2.
![]()
Table 1: Distribution of ADMA, reactant of acute phase in patients with RA and healthy control group
View Table 1
![]()
Table 2: Diagnostic values of ADMA, and other laboratory variables in patients with RA
View Table 2
ADMA plasma level is increased in RA without CVD or presence of risk factors. ADMA plasma level to show dependence on duration and disease evolution.Sero-positivity in RA has influence ADMA plasma level. There is association between ADMA and anti-citrulated peptide antibodies (anti-CCP2 ) from the second generation in early RA (p<0.05).
The results obtained from the investigation would provide better prognostic, clinic and economic efficacy in patients. The practical significance of the determination of ADMA plasma level in everyday clinical practise results from the fact that the doctor, according to the results of its concentration could change not only diagnostic, but also therapeutic tactics. With the follow-up of the dynamics of changes of concentration of ADMA, he could judge for the nature and development of the disease and its outcome. These possibilities make determination of ADMA plasma level practically important for on-time information to the doctor, considering disease nature and its severity.
The obtained results would point that the quantity of ADMA in plasma is important, not only for diagnosis, but also for follow-up and treatment of patients.
Discussion
As the principal endogenous inhibitor of nitric oxide synthase, ADMA (asymmetric dimethylarginine), regulates rates of nitric oxide (NO) formation. Nitric oxide acts as a signal molecule in the nervous system, as a weapon against infections, as a regulator of blood pressure, and as a gate keeper of blood flow to the organs. Elevated ADMA has been associated with various cardiovascular risk factors, renal failure, and erectile dysfunction. Factors contributing to elevated ADMA include increased oxidative challenge and folic acid insufficiency. ADMA is a better predictor of insulin resistance than any other single marker. It is a better predictor of vascular endothelial impairment than cholesterol. Homocysteine increases in proportion to ADMA. The inhibition of nitric oxide synthesis may explain why homocysteine has been associated with impaired endothelium mediated, nitric oxide-dependent vasodilatation.
An elevated concentration of ADMA is a potential contributory factor for pre-eclampsia, and is associated with endothelial dysfunction in some women. A glucose-induced impairment causes ADMA accumulation and may contribute to endothelial vasodilator dysfunction in diabetes mellitus. In the cardiovascular system, decreased NO biosynthesis has the potential to increase blood pressure, enhance platelet and white cell adhesiveness, increase vascular smooth muscle growth, alter mitochondrial oxygen consumption and accelerate the development of atherosclerotic-like lesions [33-35].
In pre-clinical and clinical studies, ADMA has been found to be elevated by hypercholesterolemia, hyperglycemia, hypertriglyceridemia, or hyperhomocysteinemia. ADMA levels are highly correlated with triglyceride levels. ADMA is elevated in peripheral and carotid artery blockage in proportion to the blockage. Lower ADMA and restore nitric oxide production Antioxidants speed breakdown of ADMA Arginine (3-6 grams daily) increases NO production. The common mechanism by which folic acid, H4B, vitamin C, w-3 fatty acids, and L-arginine bring about their beneficial actions in various vascular diseases is by enhancing endothelial nitric oxide (eNO) production.. A unique, independent marker of NO competence A cost-effective addition to any cardiovascular risk assessment Included with the Metametrix Metabolic Syndrome Profile Additional Profiles to help assess risk of cardiovascular disease: Asymmetric dimethylarginine (ADMA) is an endogenous inhibitor of NO-synthase. It is formed during proteolysis of methylated proteins and removed by renal excretion ormetabolic degradation by the enzyme dimethylarginine dimethylaminohydrolase (DDAH). Several cell types, including human endothelial and tubular cells, are capable of synthesizing and metabolizing ADMA. Elevated ADMA concentrations in the blood are found in numerous diseases associated with endothelial dysfunction. For example, elevated ADMA levels in the blood of individuals on dialysis correlate significantly with the degree of arteriosclerosis and cardiovascular risk [36].
Conclusion
Elevated ADMA levels are found in individuals with hypercholesterolemia, hypertension, arteriosclerosis, chronic renal failure, and chronic heart failure, and are associated with restrictions in endothelial vasodilatation.
There is strong association between ADMA and anti-cyclic citrulated peptide antibodies (anti- CCP2 ) from the second generation, in early RA without cardiovascular risk factors as result of the activity of disease and inflammatory activation.
References
-
Surdacki A (2008) L-arginine analogs-inactive markers or active agents in atherogenesis? Cardiovasc Hematol Agents Med Chem 6 :302-311.
-
Khan F, Galarraga B, Belch JJ (2010) The role of endothelial function and its assessment in rheumatoid arthritis. Nat Rev Rheumatol 6: 253-261.
-
Vallance P, Leiper J (2004) Cardiovascular biology of the asymmetric dimethylarginine: dimethylarginine dimethylaminohydrolase pathway. Arterioscler Thromb Vasc Biol 24: 1023-1030.
-
Leiper J, Murray-Rust J, McDonald N, Vallance P (2002) S-nitrosylation of dimethylarginine dimethylaminohydrolase regulates enzyme activity: further interactions between nitric oxide synthase and dimethylarginine dimethylaminohydrolase. Proc Natl Acad Sci USA 99: 13527-13532.
-
Remans PH, van Oosterhout M, Smeets TJ, Sanders M, Frederiks WM, et al. (2005) Intracellular free radical production in synovial T lymphocytes from patients with rheumatoid arthritis. Arthritis Rheum 52: 2003-2009.
-
Middleton J, Americh L, Gayon R, Julien D, Aguilar L, et al. (2004) Endothelial cell phenotypes in the rheumatoid synovium: activated, angiogenic, apoptotic and leaky. Arthritis Res Ther 6: 60-72.
-
Marliss EB, Chevalier S, Gougeon R, Morais JA, Lamarche M, et al. (2006) Elevations of plasma methylarginines in obesity and ageing are related to insulin sensitivity and rates of protein turnover. Diabetologia 49: 351-359.
-
Sydow K, Hornig B, Arakawa N, Bode-Böger SM, Tsikas D, et al. (2004) Endothelial dysfunction in patients with peripheral arterial disease and chronic hyperhomocysteinemia: potential role of ADMA. Vasc Med 9: 93-101.
-
Zhang WZ, Venardos K, Chin-Dusting J, Kaye DM (2006) Adverse effects of cigarette smoke on NO bioavailability: role of arginine metabolism and oxidative stress. Hypertension 48: 278-285.
-
Mittermayer F, Krzyzanowska K, Wolzt M (2008) [Asymmetric dimethylarginine (ADMA): A cardiovascular risk factor]. Wien Klin Wochenschr 120: 462-466.
-
Surdacki A, Martens-Lobenhoffer J, Wloch A, Gluszko P, Rakowski T, et al. (2009) Plasma asymmetric dimethylarginine is related to anticitrullinated protein antibodies in rheumatoid arthritis of short duration. Metabolism 58:316-318.
-
Turiel M, Tomasoni L, Sitia S, Cicala S, Gianturco L, et al. (2010) Effects of long-term disease-modifying antirheumatic drugs on endothelial function in patients with early rheumatoid arthritis. Cardiovascular Therapeutics 28: 53-64.
-
Leiper J, Nandi M (2011) The therapeutic potential of targeting endogenous inhibitors of nitric oxide synthesis. Nat Rev Drug Discov 10: 277-291.
-
Böger RH (2004) Asymmetric dimethylarginine, an endogenous inhibitor of nitric oxide synthase, explains the "L-arginine paradox" and acts as a novel cardiovascular risk factor. J Nutr 134: 2842S-2847S.
-
Johnsen SP, Larsson H, Tarone RE, McLaughlin JK, Norgard B, et al. (2005) Risk of hospitalization for myocardial infarction among users of rofecoxib, celecoxib, and other NSAIDs: a population-based case-control study. Arch Intern Med 165: 978-984.
-
Garcia Rodriguez LA, Gonzalez-Perez A (2005) Long-term use of non-steroidal anti-inflammatory drugs and the risk of myocardial infarction in the general population. BMC Med 3: 17.
-
Kearney PM, Baigent C, Godwin J, Halls H, Emberson JR, et al. (2006) Do selective cyclo-oxygenase-2 inhibitors and traditional non-steroidal anti-inflammatory drugs increase the risk of atherothrombosis? Meta-analysis of randomised trials. BMJ 332: 1302-1308.
-
del Rincón I, O'Leary DH, Haas RW, Escalante A (2004) Effect of glucocorticoids on the arteries in rheumatoid arthritis. Arthritis Rheum 50: 3813-3822.
-
Boers M, Nurmohamed MT, Doelman CJ, Lard LR, Verhoeven AC, et al. (2003) Influence of glucocorticoids and disease activity on total and high density lipoprotein cholesterol in patients with rheumatoid arthritis. Ann Rheum Dis 62: 842-845.
-
del Rincon I, O'Leary DH, Haas RW, Escalante A (2004) Effect of glucocorticoids on the arteries in rheumatoid arthritis. Arthritis Rheum 50: 3813-3822.
-
Westlake SL, Colebatch AN, Baird J, Kiely P, Quinn M, et al. (2010) The effect of methotrexate on cardiovascular disease in patients with rheumatoid arthritis: a systematic literature review. Rheumatology (Oxford) 49: 295-307.
-
Georgiadis AN, Papavasiliou EC, Lourida ES, Alamanos Y, Kostara C, et al. (2006) Atherogenic lipid profile is a feature characteristic of patients with early rheumatoid arthritis: effect of early treatment-a prospective, controlled study. Arthritis Res Ther 8: 82.
-
Gazi IF, Boumpas DT, Mikhailidis DP, Ganotakis ES (2007) Clustering of cardiovascular risk factors in rheumatoid arthritis: the rationale for using statins. Clin Exp Rheumatol 25: 102-111.
-
Surdacki A, Martens-Lobenhoffer J, Wloch A, Marewicz E, Rakowski T, et al. (2007) Elevated plasma asymmetric dimethyl-L-arginine levels are linked to endothelial progenitor cell depletion and carotid atherosclerosis in rheumatoid arthritis. Arthritis Rheum 56 : 809-819.
-
Seriolo B, Paolino S, Sulli A, Fasciolo D, Cutolo M (2006) Effects of anti-TNF-alpha treatment on lipid profile in patients with active rheumatoid arthritis. Ann N Y Acad Sci 1069: 414-419.
-
Tam LS, Tomlinson B, Chu TT, Li TK, Li EK (2007) Impact of TNF inhibition on insulin resistance and lipids levels in patients with rheumatoid arthritis. Clin Rheumatol 26: 1495-1498.
-
Vis M, Nurmohamed MT, Wolbink G, Voskuyl AE, de Koning M, et al. (2005) Short term effects of infliximab on the lipid profile in patients with rheumatoid arthritis. J Rheumatol 32: 252-255.
-
Arnett FC, Edworthy Sm, Bloch Da, McShane DJ, Fries JF, et al. (1988) The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum 31:315-324.
-
van Gestel AM, Prevoo ML, van 't Hof MA, van Rijswijk MH, van de Putte LB, et al. (1996) Development and validation of the European League Against Rheumatism response criteria for rheumatoid arthritis. Comparison with the preliminary American College of Rheumatology and the World Health Organization/International League against Rheumatism Criteria. Arthritis Rheum 39: 34-40.
-
Prevoo ML, van't Hof MA, Kuper NH, van Leeuwen MA, van de Putte LB, et al. (1995) Modified disease activity scores that include 28-joint counts. Development and validation in a prospective longitudinal study of patients with rheumatoid arthritis. Arthritis Rheum 38:44-48.
-
Balsa A, Carmona L, González-Alvaro I, Belmonte MA, Tena X, et al. (2004) Value of Disease Activity Score 28 (DAS28) and DAS28-3 compared to American College of Rheumatology-defined remission in rheumatoid arthritis. J Rheumatol 31: 40-46.
-
Prevoo MLL, van Gestel AM, van't Hof MA, van Rijswijk MH, van de Putte LBA, et al. (1996) Remission in a prospective study of patients with rheumatoid arthritis. American Rheumatology Association preliminary remission criteria in relation to the disease activity score. Br J Rheumatol 35:1101-1105.
-
Vaudo G, Marchesi S, Gerli R, Allegrucci R, Giordano A, et al. (2004) Endothelial dysfunction in young patients with rheumatoid arthritis and low disease activity. Ann Rheum Dis 63: 31-35.
-
Surdacki A, Martens-Lobenhoffer J, Wloch A, Gluszko P, Rakowski T, et al. (2009) Plasma asymmetric dimethylarginine is related to anticitrullinated protein antibodies in rheumatoid arthritis of short duration. Metabolism 58: 316-318.
-
Turiel M, Tomasoni L, Sitia S, Cicala S, Gianturco L, et al. (2010) Effects of long-term disease-modifying antirheumatic drugs on endothelial function in patients with early rheumatoid arthritis. Cardiovasc Ther 28: e53-64.
-
Khan F, Galarraga B, Belch JJ (2010) The role of endothelial function and its assessment in rheumatoid arthritis. Nat Rev Rheumatol 6: 253-261.





