Clinical Medical
Reviews and Case Reports
Spindle Cell Carcinoma of the Oral Cavity: A Case Report
Ezulia T1*, Saim L2, Primuharsa Putra Sha2 and MS Kenali2
1Department of Otorhinolarygology, School of Medicine, KPJ Healthcare University College, Malaysia
2KPJ Healthcare University College, KPJ Tawakkal Specialist Hospital, Malaysia
*Corresponding author: Ezulia T, Department of Otorhinolarygology, Head and Neck Surgery, School of Medicine, KPJ Healthcare University College, Malaysia, Tel: + 60162065908, E-mail: tengkuezulia@gmail.com
Clin Med Rev Case Rep, CMRCR-2-015, (Volume 2, Issue 1), Case Report; ISSN: 2378-3656
Received: November 10, 2014 | Accepted: January 28, 2015 | Published: January 30, 2015
Citation: Ezulia T, Saim L, Sha PP, Kenali MS (2015) Spindle Cell Carcinoma of the Oral Cavity: A Case Report. Clin Med Rev Case Rep 2:015. 10.23937/2378-3656/1410015
Copyright: © 2015 Ezulia T, et al. This is an open-access article distributed under the terms ofthe Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Spindle Cell Carcinoma (SpCC) also known as sarcomatoid carcinoma is a rare biphasic malignant neoplasm that occurs mainly in the upper aerodigestive tract. It has spindled or pleomorphic tumor cells which simulate a true sarcoma but of epithelial origin. WHO classification has placed this tumour under a highly malignant variant of squamous cell carcinoma and labelled it spindle cell carcinoma. It is known for propensity for recurrence and metastases.
Material and methods: A 33 -years old lady presented with a rapidly enlarging fungating mass over right lower alveolar in the molar region of two month duration. It was associated with pain, odynophagia and trismus. She had foetor ex ore, and there was large fungating mass in the right lower alveolar measuring 4-5 cm in its largest diameter. The buccal mucosa and the floor of mouth in the vicinity of the tumour were spared. There were multiple small nodes palpable in the submandibular area. Biospy reported as spindle carcinoma.
Results: A pre-operative Computed Tomography (CT) of the neck showed a lytic lesion in the alveolar margin of right angle of mandible. She then underwent surgery to remove the tumour entailed: right segmental mandibulectomy along with the primary tumour and right modified neck dissection. However, the posterior end of the intraoral wound broke down and closure of the wound with a tongue flap was performed one week later. The tongue flap took well and the pedicle is intact.
Conclusion: SpCC of oral cavity is potentially more aggressive than SCC and a high index of suspicion is the prerequisite for an early diagnosis.
Keywords
Spindle cell carcinoma, Oral cavity, Squamous cell carcinoma, Head and neck
Introduction
Spindle cell carcinoma is a biphasic tumour [1]. It has spindled or pleomorphic tumor cells which simulate a true sarcoma but of epithelial origin [2]. This tumour has been called by several alternative names because of their microscopic peculiarities including sarcomatoid carcinoma, carcinosarcoma, pseudosarcoma, pleomorphic carcinoma and polypoid carcinoma [3,4]. WHO classification has placed this tumour under a highly malignant variant of squamous cell carcinoma and labelled it spindle cell carcinoma [1,3]. It occurs most commonly in upper aerodigestive tract [3]. However, it may also occur in other sites of body. The mean age of diagnosis is in the sixth decades of life [5]. It has male predilection [5]. The predisposing factors are the same as squamous cell carcinoma, including alcohol abuse, cigarette smoking, poor oral hygiene and previous radiotherapy [2,5]. Growth is usually exophytic polypoid [5] or pedunculated [1] and can cause obstructive symptoms. It is potentially aggressive and have a propensity for recurrence and metastases [3]. This makes accurate diagnosis critical [4]. Immuno histochemistry along with routine histopathology is essential in establishing the diagnosis [5].
Case History
A 33 years old female patient presented with a large fungating mass over right lower alveolar in the molar region. The tumour grew to that extend within the last two months prior to consultation. Biopsy was taken. The report came back as spindle cell carcinoma. She complained of pain, odynophagia and some degree of trismus with occasional episodes of bleeding from the tumour. She had no history of any medical illness.
On examination she had foetor ex ore. There was a large fungating mass in the right alveolar measuring 4-5cm in its largest diameter. The buccal mucosa and the floor of mouth in the vicinity of the tumour were spared. There were multiple lymph nodes palpable in the submandibular area on the right side with the largest diameter of 2.5cm (Figure 1).
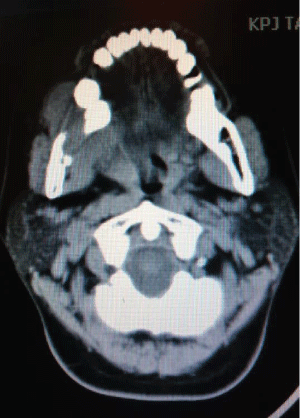
Figure 1: CT scan of neck showing lytic lesion in the alveolar margin of right
angle of mandible.
View Figure 1
There is a soft tissue swelling medially and laterally and shows contrast enhancement. The lesion measures 39x 28mm (axial) and 33mm (height). There are small lymph nodes noted on both sides of the neck with three small nodes on the right side showing central lucencies.
She underwent surgery to remove the tumour entailed a right segmental mandibulectomy along with the primary tumour and right modified neck dissection. Reconstruction of the mandible and closure of the wound with a tongue flap performed.
However, the posterior end of the intraoral wound broke down and closure of the wound with a tongue flap performed. The tongue flap took well and the pedicle was intact. She was then referred for radiotherapy.
Histologically, sections from the fungating tumour reveals ulcerated surface. The intact covering epithelium is of stratified squamous epithelium. The underlying stroma is infiltrated by cellular spindle cells displaying mild to moderately pleomorphic nuclei with increase mitosis. There is no margin of tumour with overlying tumour noted. No area of necrosis seen. The tumour is seen abutting the bone but not infiltrating it. The margins of resections are free of tumour and the neck dissection specimens were negative of cancer (Figure 2).
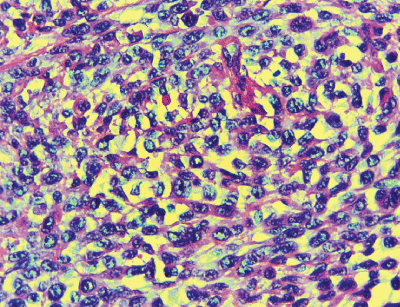
Figure 2: Histology of spindle cell carcinoma showing cellular spindle cells
displaying mild to moderately pleomorphic nuclei with increase mitosis (H&E
stain 400x)
View Figure 2

Figure 3: Spindle cell positive for EMA
View Figure 3
Immunohistochemical analysis revealed that the spindle cells showed positive immunoreactivity for Epithelial Membrane Antigen (EMA) and vimentin but negative for Cytokeratin AE1/AE3 and Cytokeratin 7 (Figures 3-5).

Figure 4: Spindle cells positive for vimentin
View Figure 4
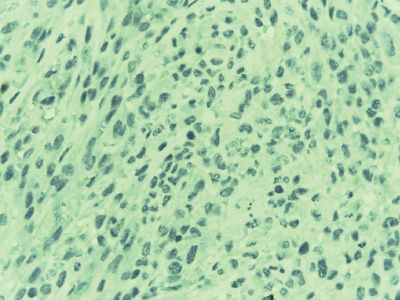
Figure 5: Spindle cells negative for Cytokeratin AE1/AE3
View Figure 5
Discussion
Spindle cell carcinoma is very rare [1,3], with a reported incidence of less than 1% of all tumours of oral regions [2,3] and 3% of Squamous cell carcinoma [5]. It is considered a biphasic malignant tumour, as it has spindled or pleomorphic tumor cells which simulate a true sarcoma but of epithelial origin [1,2]. However, about one-third are monophasic spindled or pleomorphic histologically, making the diagnosis more challenging [4].
Spindle cell carcinoma has been thought to be a collision tumour, combination tumour or composition tumours [6]. There was a great confusion on whether it is carcinoma or sarcoma, and benign or malignant. It was later when studies of the morphologic, immune histochemical, ultra structural and molecular features of spindle cell carcinoma have been established, that this tumour is recognized as a carcinoma that has surface epithelial changes and an underlying spindle-shaped neoplastic proliferation [3]. Because of its microscopic peculiarities, this tumour has several names which include sarcomatoid carcinoma, carcinosarcoma, pseudosarcoma, pleomorphic carcinoma and polypoid carcinoma [3,4]. WHO classification has placed this tumour under a highly malignant variant of squamous cell carcinoma and labelled it spindle cell carcinoma [1,3].
This tumour occurs mainly in upper aerodigestive tract [3]. The larynx, particularly the glottis in 70% of cases is the commonest primary site [1]. The second commonest site is the oral cavity [7], which may arise from the tongue, floor of the mouth, alveolar ridge, gingivae or lower lip [5]. It may also occur in other sites of body such as head and neck skin, in the soft tissues of the scalp and orbit. The mean age of diagnosis is in the sixth decades of life, but it can be diagnosed in younger age group and older age group (range 29 -93) [5]. Some authors have reported male predilection [1,3-6] with ratio of 12:1 [1]. However, it is becoming more common in females [1]. The predisposing factors are the same as squamous cell carcinoma, including alcohol abuse, cigarette smoking, poor oral hygiene and previous irradiation site [2,5]. In the present case, patient was 33 years old lady with no predisposing factor.
Growth of this tumour is exophytic polypoid or pedunculated in 98.9% of cases [1]. It can also be sessile, nodular or endophytic [5]. The present case showed exophytic fungating mass. This tumour has tendency to cause obstructive symptoms especially when it occurs in larynx. Patients may present with cough, voice change, and hoarseness of voice, dyspnea or stridor. Tumours of oral cavity and oropharynx typically present with just complaint of a mass or with painful, non healing ulcer or bleeding.
Histologically, Spindle cell carcinoma exhibits both epithelial cell component and sarcomatoid or spindle cell component. The spindle cell component may demonstrate varied histological appearance ranging from benign reactive lesion to malignant lesions [3]. The most common ones are pleomorphic (malignant hisiocytoma like) and spindle cell sarcoma (fibrosarcoma like) [2]. While spindled component usually predominates, the squamous component is either focal dysplacia, carcinoma in situ or invasive SCC [6]. Histological and immune histochemistry demonstration of both squamous cell component and the spindle cells with sarcomatous appearance is essential in establishing the diagnosis [5]. Differential diagnosis ranges from benign to malignant lesions, such as fibromatosis, reactive epithelial proliferations, fibrosarcoma, rhabdomyosarcoma and malignant melanoma.
Immuhistochemical studies are useful to know the histogenesis of the spindle cells within these tumours and nature of SpCC. There are numerous histogenetic hypothesis have been proposed over the years, with 3 principal theories, including: 1) it is a collision tumour or a carcinosarcoma; whereby a separate epithelial and mesenchymal cell have each become malignant; 2) it is a spindle cell carcinoma or sarcomatoid carcinoma � an epithelial cell that differentiates into spindle cell component; or 3) it is pseudosarcoma � a squamous cell carcinoma that undergoes benign reactive stromal.
Epithelial markers include keratin (AE1/AE3, CK 1,8,9), epithelial membrane antigens, KI, and K18. The most sensistive and reliable ones are keratin and epithelial membrane antigen. They are helpful in differential diagnosis from other sarcomatous lesions. EMA was positive is in this study while cytokeratin was negative. It reflects that the neoplastic cells are of epithelial origin but have undergone alteration resulting in loss of keratin. Mesenchymal markers include vimentin, desmin, S-100, Osteopontin and BMP. In this study, the spindle shaped tumour cells were positive for vimentin. It suggests that the bizarre fibroblast-like cells are carcinoma cells with true mesenchymal metaplasia that have acquired mesenchymal properties both morphologically and functionally through metaplastic changes, resulting in loss of keratin and acquiring vimentin as the cytoskeletal protein [2,3]. Double labelling with keratin and vimentin in spindle cells illustrating the versatility of the intermediate filament phenotype. An additional epithelial marker, P63 has been reported as useful for spindle cell carcinoma [2,3].
Spindle cell carcinomas are staged according to the TMN classification of American Joint Committee on Cancer staging, based on their size and the presence or absence of metastases to local lymph nodes or other parts of the body [1]. The treatment option in Spindle cell carcinoma has been debated. Some authors are of the opinion that wide radical resection alone is sufficient while some prefers surgery with radiotherapy. The best long term outcome for patient is surgery followed by radiotherapy [3]. Radiotherapy is considered an acceptable choice for inoperable patients and useful in case with surgical margin positive or extensive nodal disease [5].
Spindle cell carcinoma in the oral cavity and oropharynx is potentially aggressive and has a propensity for recurrence and metastases [3]. The survival and reaction to treatment of SpCC are still controversial [3,8]. The prognosis depends upon distant metastases, depth of tumour invasion, and polypoid configuration. Patients with deeply invasive tumour tend to have poor prognosis whereas those with early stage tumours usually have excellent prognosis [2].
In a study that was conducted on 15 patients of spindle cell carcinoma of oral cavity and oropharynx receiving surgery, a high local recurrence rate (73.3%) and distant metastasis rate (33.3%) were observed [8]. Anupam et al [9] had concurred the recurrence rate of 71.4% and metastasis rate of 21.4% in their study. Some literatures stated that the prognosis is poorer than the conventional SCC at a similar stage [3,8,9]. About 30% of all oral cases ended with mortality within one year [3,9]. This outcome is similar to the high grade SCC [9].
Conclusion
Spindle cell carcinoma of head and neck is a rare and unique subtype of squamous cell carcinoma. It is potentially aggressive than the classical Squamous Cell Carcinoma (SCC). It also seems to recur easily and to metastasize. It mimics other connective tissue sarcomas & spindle cell malignancies at light microscopic level. Immunohistochemistry is helpful to know the histogenesis and nature of SpCC. The prognosis of disease is controversial. Patients whose tumors are deeply invasive tend to have a poor prognosis, whereas those with early-stage tumors have an excellent prognosis.
References
-
Boamah H, Ballard B (2012) A case report of spindle cell (sarcomatoid) carcinoma of the larynx. Case Rep Med 2012: 370204.
-
Parikh N, Desai N (2011) Spindle Cell Carcinoma of the oral cavity: A case report of a rare entity and review of literature. J Academy Adv Dental Research 2: 2.
-
Ravindran R, Mohan V, Saji AM (2013) Spindle Cell Carcinoma of Maxilla: Case report of a rare entity and review of literature. Oral & Maxillofacial Pathology Journal: 4.
-
Lewis JS Jr (2008) Spindle cell lesions--neoplastic or non-neoplastic?: spindle cell carcinoma and other atypical spindle cell lesions of the head and neck. Head Neck Pathol 2: 103-110.
-
Sarma A, Das R, Sharma JD, Kataki AC (2012) A Clinicopathological and Immunohistochemical Study of 40 Cases. Journal of Cancer Therapy 3: 1055-1059.
-
Thompson LD, Wieneke JA, Miettinen M, Heffner DK (2002) Spindle cell (sarcomatoid) carcinomas of the larynx: a clinicopathologic study of 187 cases. Am J Surg Pathol 26: 153-170.
-
Chang NJ, Kao DS, Lee LY, Chang JW, Hou MM, et al. (2013) Sarcomatoid carcinoma in head and neck: a review of 30 years of experience--clinical outcomes and reconstructive results. Ann Plast Surg 71: S1-7.
-
Su HH, Chu ST, Hou YY, Chang KP, Chen CJ (2006) Spindle cell carcinoma of the oral cavity and oropharynx: factors affecting outcome. J Chin Med Assoc 69: 478-483.
-
Anupam Sarma, Rajjyoti Das, Sharma JD, Kataki AC (2012) Spindle Cell Carcinoma of the Head and Neck: A Clinicopathological and Immunohistochemical Study of 40 Cases. Journal of Cancer Therapy 3: 1055-1059.





