Clinical Medical
Reviews and Case Reports
Outcomes of Influence of Dimethylarginine Derivats, PAD Isoenzymes, or both as Hallmark on Citrullinisation Process on Autoantigens ACPA/Anti CCP Antibodies overall for Diagnosis in Rheumatoid Arthritis
Dejan Spasovski1* and Tatjana Sotirova2
1Department of Rheumatology, University Clinical Centre, Skopje, Republic of Macedonia
2University Clinic of Heamatology, Cyril and Methodius University, Skopje, Rebublic of Macedonia
*Corresponding author: Dejan Spasovski, Deparment of Rheumatology, University Clinical Centre, Skopje, Republic of Macedonia, Tel: +389 2 3147 668, E-mail: drspasovski@yahoo.co.uk
Clin Med Rev Case Rep, CMRCR-2-016, (Volume 2, Issue 2), Review Article; ISSN: 2378-3656
Received: | August 22, 2014 | Accepted: February 23, 2015 | Published: February 26, 2015
Citation: Spasovski D, Sotirova T (2015) Outcomes of Influence of Dimethylarginine Derivats, PAD Isoenzymes, or both as Hallmark on Citrullinisation Process on Autoantigens ACPA/Anti CCP Antibodies overall for Diagnosis in Rheumatoid Arthritis. Clin Med Rev Case Rep 2:016. 10.23937/2378-3656/1410016
Copyright: © 2015 Spasovski D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: When establishing new diagnostic method for detection of the endothelial dysfunction in Rheumathoid Arthritis (RA), it is necessary to compare the diagnostic values with other laboratory variables.
Aim: To Assess Asymmetric Dimethylarginine (ADMA) in RA and study its relation to ACPA and different clinical and laboratory parameters of disease activity in early non treated RA patients. Also, to determine the association between the asymmetric dimethylarginine (ADMA) and anti-cyclic citrullinated peptide antibodies (ACPA, Anti-CCP2) of the second generation in RA and to explain their connection in the process of citrulination of autoantigens in RA. Also, to determine the association between ADMA and the acute phase reactants: Rheumatoid factor (RF), C-reactive protein (CRP), as well as the index of disease intensity (DAS28) in early diagnosis in non-treated RA patients and to determine whether the amount of ADMA changes in the course of the evolution of disease.
Methods: Using the ELISA method (DLD-Diagnostika-GMBH for ADMA and BioSystems S.A. Reagens & Instruments Costa Brava 30, Barselona, Spain), the sera of 70 subjects have been examined (35 RA not-treated, 35 healthy control group).
Results: Of 35 patients with RA, presence of ADMA was detected in 13 patients (37.14%); RF was present in 17 patients (48.57%), while anti-CCP2 antibodies were present in 23 patients (65.71%). Of 18 patients who were RF negative, ADMA was detected in 9 patients (50%), while 11 patients (31.43%) were anti-CCP2 positive. In 17 RF positive patients with RA, ADMA was detected in 4 patients, while 12 patients (34.28%) were anti-CCP2 and RF positive. In the healthy control group 8 patients (22.85%) showed ADMA positivity. There was moderate correlation between ADMA and anti-CCP2 antibodies in the group of patients with RA (r=0.34).
Conclusion: There was an association between ADMA and anti-CCP2 antibodies of the second generation in patients with RA.
Keywords
Asymmetric dimethylarginine (ADMA), Rheumatoid arthritis, Rheumatoid factor
Introduction
The association between arginine and citrulline, i.e. between asymmetric dimethylarginine (ADMA) as dimethyl derivative of the amino acid L-arginine and anti-cyclic citrullinated peptide antibodies (Anti-CCP2) of the second generation in patients with Rheumatoid Arthritis (RA) is the isoform of the enzyme Peptidylarginine Deiminase (PAD). Enzymatic deimination or protein citrullination is a process catalyzed by PAD enzymes which take part in the pathogenesis of RA. [1,2] In humans five PAD isoforms (PAD1-4 and PAD6) are present. The greatest attention is paid to PAD2 and PAD4, as potential candidates that could play role in the process of citrullination of autoantigens in RA. Both enzymatic forms are present in the rheumatoid synovium and fluid. [3-5] The polymorphism of PAD4 is genetically associated with RA [6]. There is a difference in the tissue and cellular distribution of these two forms: PAD2 is ubiquitously distributed in tissue (on the cytoplasmic level), while PAD4 is more dominant in the hematopoietic cells (on nuclear level) [7-11]. In human neutrophils three different PAD isoforms (PAD2-4) are expressed. PAD targets are different cells� substrates on cellular or sub-cellular level. In the process of intracellular protein citrullination, different auto-antibodies recognize these substrates as citrullinated substrates. But, this explanation is probably partial, because the protein citrullination can take place also extracellularly. Cellular targets, identified as potential citrullinated autoantibodies with extracellular distribution are: filaggrin, vimentin, β-actin, collagen type I and II, gamma enolase etc [12-19]. Extracellular citrullination of fibrinogen is probably derived by PAD from damaged cells [4,20], but, so far it is not known in which conditions it occurs. Citrullinated autoantibodies play key role in the immune answer in RA. Few unique characteristics of protein citrullination enrolled in the pathogenesis of RA are identified: 1. The cytoplasmic content has autoantigenic features and is a target in the process of citrullination; 2. Although there are great number of proteins citrullinated by the active neutrophils, anti- CCP2 recognises only small number of these molecules; 3. Citrulline activity of each PAD isoforms is characterized by the unique substrate specificity, independently of their subcellular distribution. Only PAD2 is capable of citrullination of native β/γ actine, while H3 hystones are only citrullinated by PAD4 isoform. PAD4 isoform which is cytoplasmic enzyme similar to PAD2 is not able to citrullinate actine and H3 hystone; 4. Different reactive abilities of different sera in RA support the hypothesis that anti CCP2 antibodies recognize the unique sequence [2,21]. The variations in the specificity of anti CCP2 antibodies in different patients with RA are impressive. Probably all PAD isoforms share similar epitopes and their possible presence in the extracellular space indicate possible pass through the subcellular barriers.
Some Aspects of Dimethylarginine Derivatives of the Amino Acid L-Arginine
There are 2 stereoisomers of the L-arginine: symmetric (SDMA) and asymmetric dimethylarginine (ADMA). ADMA interferes with L-arginine in the production of nitric oxide (NO), which plays key role in the normal endothelial function. Namely, NO is synthesized in the endothelial cells with the enzyme - endothelial nitric oxide synthetase (NOS). The physiological substrate (precursor) for NOS in this enzymatic process is L-arginine, converted in NO and L-citrulline. The NOS is inhibited by ADMA. The plasma level of ADMA is elevated in RA.
ADMA is synthesized by protein methylation mostly in the cellular nucleus. The methylation is catalyzed by the group of enzymes called protein arginine N-methyl tranferases (PRMTs type I and II). Both PRMT subtypes have the ability to methylate monomethyl arginine (MMA); type 1 asymmetrically dimethylates arginine and creates ADMA, while type 2 catalyzes symmetrical dimethylation of arginine and creates SDMA (Figure1).
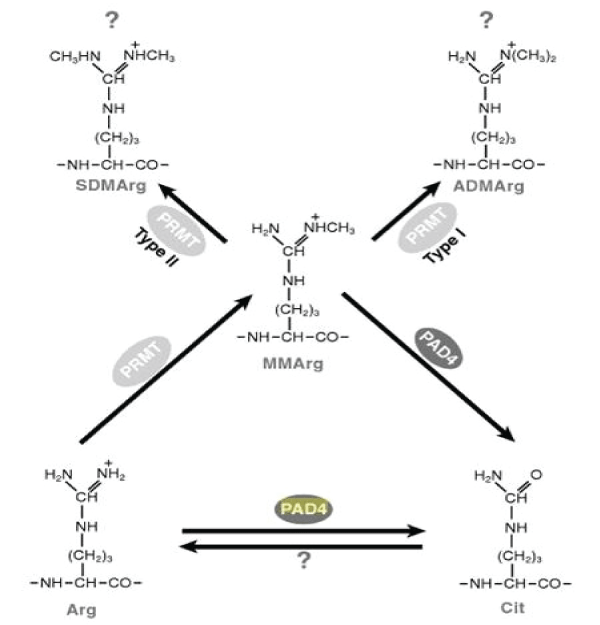
Figure 1: Metabolic aspects of dimethyl derivates of the amino acid l-arginine and peptidylarginin deiminase (PAD).
View Figure 1
Aim
The aim of this study is to determine the association between ADMA and anti-cyclic citrullinated peptide antibodies (Anti-CCP2) of the second generation in patients with Rheumatoid Arthritis (RA) and to explain their connection in the process of citrullination of autoantigens in RA.
Material and methods
In the patients examined for this study, the diagnosis of the disease was established on the basis of revised diagnostic criteria for the classification of RA, suggested in 1987 by the American Association for Rheumatism (ARA) [22]. In order for a patient to be diagnosed with rheumatoid arthritis, patients must fulfill at least four out of seven criteria. Criteria from one to four are present for at least six month. In order to be included in the study every patient should fulfill at least 4 of the predicted 7 criteria. Criteria of diagnosis are related to American Colleague of Rheumatology (ACR).
In the study are included 70 patients, 35 patients with RA (28 women and 7 men), as well as 35 patients as healthy control group (18 women and 17 men). The mean age is 56, 68 years (±6.79) (40-65 years) in the group with RA and 46.2 years (±12.49) (29-65 years) in the healthy control group. The median duration of the disease in months is 43.97 (±45,23) in the interval of 1-168 months. Three patients were previously treated with oral steroids, while nobody was treated with NSAIDs. The others denied the use of other drugs such as arginine or nitroglycerin before the entrance in the study.
Inclusion criteria
In the study are included patients with RA aged 18-65 years, previously non-treated with NSAIDs or DMARDs.
Exclusion criteria
In the study are not included patients with diseases or conditions that could directly or indirectly influence the results, such as: 1. Patients with previous history of spleen disease, thyroid disorders, hepatic damages, kidney, hematologic, neurologic and pulmonary disorders, autoimmune diseases, age < 18 years; 2. Patients with Diabetes mellitus, acute infections, malignant diseases, febrile conditions ; 3. Patients with uric arthritis, urinary infections, SLE, mixed connective tissue disease, vasculitis; 4. Patients with previous history of blood trasfusions, as well as overweight patients; 5. Patients treated with basic drugs for RA are excluded from the study; 6. Also, patients with the presence of hypeglycemia and elevated level of degradation products (serum urea and creatinin, urine creatinin), smokers, patients with arterial hypertension, hematologic and enzymatic disorders detected in 0 point, are excluded from the study; 7. Patients treated with cardiologic and hypolipidemic drugs, oral contraceptive drugs (estrogens, progesterone), vitamin E, nitroclycerin, arginine or analogues, and patients who received inhalational anesthetics one month before the start of the study are also excluded.
All participants voluntarily participated in the study, so the ethic criteria for the preparation of the study were fulfilled.
clinical evaluation for disease activity
The clinical evaluation is made by the subspecialist in the field. Disease activity is evaluated using the DAS28 index (Disease Activity Score (DAS28). [23] The index uses mathematical formula in order to obtain unique composite quantitative score which consists of palpable painful joints (maximal number � 28), swollen joints (maximal number � 28), Westergren�s Erythrocyte Sedimentation Rate (ESR) and patient�s global evaluation for the disease activity (0-100 mm Visual Analogue Scale -VAS) as morning stiffness (in minutes). The DAS28 index ranges from 0 to 10, and score bellow 3.2 qualifies the disease as low active.
Laboratory evaluation
For clinical evaluation of RA several variables were taken into account: Complete Blood Count (CBC), differential blood count, reactants of the acute phase such as C-reactive protein (CRP), Rheumatoid Factor (RF) and Erythrocyte Sedimentation rate (ESR), anti CCP2 antibodies, Alkaline Phosphatase (AP), Aspartate Aminotransferase (AST), Alanine Aminotransferase (ALT), Kreatinin Kinase (KK), Lactate dehydrogenase (LDH), serum urea and creatinin. The specimens are processed immediately (not frozen), respecting the rules of good laboratory practice.
Determination of the activity of the serum Asymmetric Dimethylarginine : ELISA method (DLD Diagnostika-GMBH)-Enzyme Immunoassay)
For quantitative determination of the endogen Asymmetric Dimethylarginine (ADMA) in plasma or serum
Principle: ADMA is connected in the solid phase of the micro titer plate. The ADMA standard, the specimens and positive control are pre-acylated in combination with rabbit anti-N-acyl-ADMA, and are incubated for 15-20 hours on 280C. Later they are washed and the second antibody is added - anti rabbit IgG conjugated with peroxidase. They are incubated for 1 hour on room temperature. After washing, in order to get dying, tetramethylbenzidine is added as a substrate solution (TMB). After 20-30 minutes of the incubation it is stopped adding sulfuric acid. The absorbance is read on microtiter read on 450 nanometers. ADMA concentration is determined with the standard curve. Basically the amount of antibodies connected in the solid phase of ADMA is conversely proportional to the ADMA concentration in the specimens.
Reference range: ADMA in serum is 0.4-0.75 micromol/L.
CRP is determined by the agglutination test (Lateks CRP test) (BioSystems S.A. Reagens & Instruments Costa Brava 30, Barselona, Spain).
Reference range: < 6 mg/L CRP in serum.
RF is determined by the agglutination test (Lateks CRP test) (BioSystems S.A. & Instruments Costa Brava 30, Barselona, Spain).
Reference range: < 8 IU/ml in serum.
Anti CCP2 antibodies are determined by the ELISA method (BioSystems S.A. Reagens & Instruments Costa Brava 30, Barselona, Spain).
Reference range: < 20 IU/ml in serum.
Quantitative method for determination of the ESR is the Westergren method.
Reference range: 7-8mm for men, 11-16 for women.
Statistical analysis
To test the significance of differences between two arithmetic means (proportions), the Student�s t-test is used in comparison with the mean values of the determined numerical parameters between two groups, as well as Wilcoxon-matched test for independent specimens. The sensitivity and the prediction for the positive and negative test of the examined markers are determined with the test for sensitivity and specificity. The P-value in the range 0.05 and 0.1 is considered statistically significant. The data processing is made with the statistical package - Statistica 7.0.
Results
Of the 35 patients with RA, 13 patients (37,14%) showed presence of ADMA. RF was present in 23 patients (65.71%). Of 18 RF negative patients, ADMA was detected in 9 patients (50%), while 11 patients (31,42%) were anti CCP2 positive. In 17 RF positive patients ADMA was present in 4 patients; 12 patients (34,28%) were anti CCP2 and RF positive. In the healthy control group 8 patients (22,85%) showed ADMA positivity. RF was present in 2 patients (5,71%), while 1 patient (2,85%) showed anti CCP2 positivity. In 35 patients with RA, DAS28>3.2 was present in 28 patients (80%). In 17 seropositive RF patients, DAS28>3.2 was present in 15 patients (88,23%) (Tables 1,2).
![]()
Table 1: Laboratory results in RA and control healthy group (M ± SD)
View Table 1
![]()
Table 2: Some diagnostic performance of laboratory variables in rheumatoid arthritis
View Table 2
There is no statistical significance using Wilcoxon-matched test between ADMA in RA and the healthy control group for p< 0.05 (p=0.555). 2. There is statistical correlation using Wilcoxon-matched test between ADMA in RA and age, duration of disease in months, DAS28 index, RF and CRP, ESR, morning stiffness, in the same group for p< 0.05: (ADMA vs age p=0.000; ADMA vs duration of disease in months p=0.000; ADMA vs DAS28 p=0,000; ADMA vs RF p=0,018; ADMA vs CRP p=0,040; ADMA vs ESR p=0,000). 3. Although the presence of anti CCP2 positive patients in DAS28>3.2 seropositive and seronegative patients is almost the same (10 vs 9 patients), the range of anti CCP2 titre is higher in 10 RF seopositive patients with DAS28>3.2 than in RF seronegative patients with DAS28>3.2 (2.23 ± 0.61vs1.92 ± 0.45). There is no statistical correlation between these two groups (p=0.374) (Chart 1). 4. There is statistical correlation using Wilcoxon-matched test between anti CCP2 in RA and the healthy control group for p< 0.05 (p=0.000), as well as between anti CCP2 in RA and DAS28, RF, CRP, ESR and morning stiffness in the same group for p< 0.05 (anti CCP2 vs DAS28 p=0,000; anti CCP2 vs RF p=0,018; anti CCP2 vs CRP p=0,041; anti CCP2 vs ESR p=0.000, anti CCP2 vs morning stiffness p=0,000). There is moderate correlation between ADMA and anti CCP2 antibodies in the group of patients with RA (r=0.34) (Chart 2).
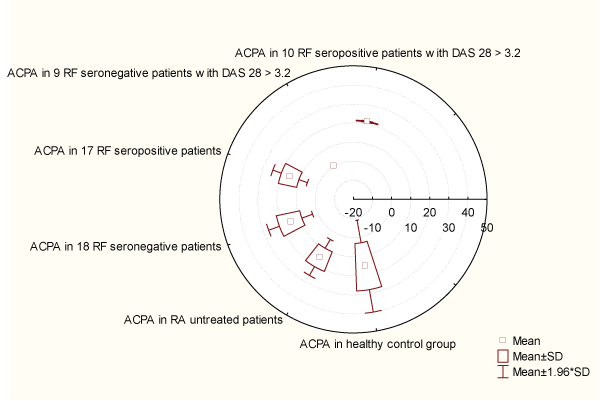
Chart-1: Distribution of ACPA antibodies in Rheumatoid arthritis in all groups.
View Chart-1
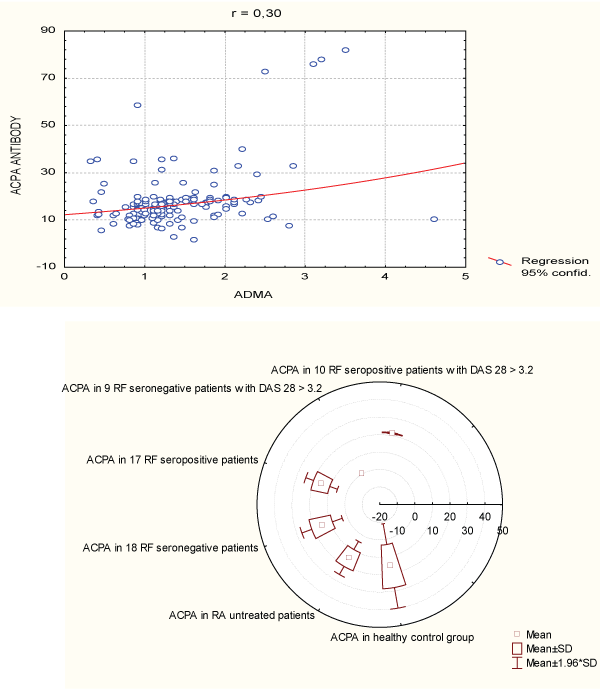
Chart-2: Correlation between ADMA and different parameter of RA. Pearson�s coefficient of correlation (r) between the values of ADMA and ACPA antibodies in the group of patients with RA. There is a moderate correlation between ADMA and ACPA antibodies (r=0,30).
View Chart-2
Discussion
The ADMA activity in serum is normally low. It is elevated in endothelial dysfunction, because of the presence of the chronic inflammation in RA. Its presence is quantified by the degree of inflammation in RA which correlates with the disease activity. There is a strong correlation between ADMA and anti-CCP2 antibodies from the second generation in early RA as a result of the disease activity and chronic inflammation [24-26].
Seropositivity influences the ADMA induction (present also in our case) - seropositive RF patients with DAS28>3.2 have higher ADMA induction than seronegative RF patients with DAS28>3.2.
The association between ADMA and anti CCP2 antibodies in patients with RA is confirmed also by other authors. They confirm the hypothesis that ADMA accumulation is associated with elevated titer of anti CCP2 antibodies. Their conclusion is that excessive ADMA accumulation is associated with elevated titer of anti CCP2 antibodies in patients with RA which duration is less than 3 years [25].
The association between anti CCP2 antibodies and RF IgM in patients with RA and their predictive value is shown by other authors [27]. They conclude that anti CCP2 antibodies and RF IgM are associated with the impaired endothelial function, independently from other cardiovascular risk factors. These autoantibodies could be reflection of the early atherosclerotic conditions and can induce increased risk of cardiovascular diseases.
The process of citrullination is desribed by other authors, also [28]. They demonstrate that human PAD4 regulates the histone arginine methylation through conversion of methyl arginine in citrulline, releasing methylamine. The targets of PAD4 are multiple areas in H3 and H4 histones that are methylated by the co-activators CARM1 (H3Arg17) and PRMT1 (H4Arg3). The decrease of the histone arginine methylation is secondarily associated with the increase in the process of citrullination. They point out that PAD4 is mediated by the genetic expression through the regulation of arginine methylation and histone citrullination.
Other authors have almost equal perception [29]. They emphasize that PAD enzymes catalyze the conversion of arginine residues in proteins with citrulline residues. The citrulline is not a standard amino acid. It is not incorporated in proteins during translation, but is generated post-translationally by PAD enzymes. In normal conditions only nuclear histones possess this amino acid.
Other authors also agree with the principle of auto-antigenicity in RA [30]. They relate auto-antigenic citrullination and different PAD enzymes in RA, emphasizing that PAD enzymes have intrinsic capacity for selection of protein targets. Such specificity could play role in auto-antigenic selection in RA. Other authors [31,33] conclude that citrullination of the proteins is enabled with the enzymatic conversion (by PAD enzyme) from proteins that contain arginine residues towards citrulline residues. They agree that PAD enzymatic activity fulfill the criteria as additive marker in monitoring disease progression, together with anti CCP2 and RF. They emphasize that the PAD method for detection is rapid, sensitive and relatively cheap.
They suggest that citrullination and methylation of the arginine residues is a process of competition. It is theoretically reversible in regard of methylation of arginine residues through conversion of mono-methyl-peptydyl-arginine (MMA) in citrulline. But, contradictory results are shown in terms of the capacity of the PAD enzymatic activity towards citrullination of MMA. In regard of the reversibility of the arginine methylation, in general, the protein methylation is one-way process and the methylated arginine residues rest as an integral part of the proteins so far, until they are degraded in the process of proteolysis. The protein methylation, generally, is considered as an irreversible process, due to the lost of demethylating enzymes in the process of conversion.
PAD4 is not able to citrullinate directly ADMA, but, it interferes in ADMA synthesis via citrullination of MMA as an intermediary product in ADMA synthesis.
Conclusion
ADMA is indirectly linked between autoantigenic citrullination and peptydyl-arginines� enzymatic isoforms in RA. Determination of ADMA together with other biological parameters contributes in the early diagnosis of RA.
References
-
Vossenaar ER, Zendman AJ, van Venrooij WJ, Pruijn GJ (2003) PAD, a growing family of citrullinating enzymes: genes, features and involvement in disease. Bioessays 25: 1106-1118.
-
Wegner N, Lundberg K, Kinloch A, Fisher B, Malmstr�m V, et al. (2010) Autoimmunity to specific citrullinated proteins gives the first clues to the etiology of rheumatoid arthritis. Immunol Rev 233: 34-54.
-
Foulquier C, Sebbag M, Clavel C, Chapuy-Regaud S, Al Badine R, et al. (2007) Peptidyl arginine deiminase type 2 (PAD-2) and PAD-4 but not PAD-1, PAD-3, and PAD-6 are expressed in rheumatoid arthritis synovium in close association with tissue inflammation. Arthritis Rheum 56: 3541-3553.
-
Chang X, Yamada R, Suzuki A, Sawada T, Yoshino S, et al. (2005) Localization of peptidylarginine deiminase 4 (PADI4) and citrullinated protein in synovial tissue of rheumatoid arthritis. Rheumatology (Oxford) 44: 40-50.
-
Kinloch A, Lundberg K, Wait R, Wegner N, Lim NH, et al. (2008) Synovial fluid is a site of citrullination of autoantigens in inflammatory arthritis. Arthritis Rheum 58: 2287-2295.
-
Suzuki A, Yamada R, Chang X (2003) Functional haplotypes of PADI4, encoding citrullinating enzyme peptidylarginine deiminase 4, is associated with rheumatoid arthritis. Nat Genet 34: 395-402.
-
Nakashima K, Hagiwara T, Yamada M (2002) Nuclear localization of peptidylarginine deiminase V and histone deimination in granulocytes. J Biol Chem 277: 49562-49568.
-
Mastronardi FG, Wood DD, Mei J (2006) Increased citrullination of histone H3 in multiple sclerosis brain and animal models of demyelination: a role for tumor necrosis factorinduced peptidylarginine deiminase 4 translocation. J Neurosci 26: 11387-11396.
-
Harris ML, Darrah E, Lam GK, Bartlett SJ, Giles JT, et al. (2008) Association of autoimmunity to peptidyl arginine deiminase type 4 with genotype and disease severity in rheumatoid arthritis. Arthritis Rheum 58: 1958-1967.
-
Andrade F, Darrah E, Gucek M, Cole RN, Rosen A, et al. (2010) Autocitrullination of human peptidyl arginine deiminase type 4 regulates protein citrullination during cell activation. Arthritis Rheum 62: 1630-1640.
-
Go�b V, Thomas-L'Otellier M, Daveau R, Charlionet R, Fardellone P, et al. (2009) Candidate autoantigens identified by mass spectrometry in early rheumatoid arthritis are chaperones and citrullinated glycolytic enzymes. Arthritis Res Ther 11: R38.
-
Schellekens GA, de Jong BA, van den Hoogen FH, van de Putte LB, van Venrooij WJ (1998) Citrulline is an essential constituent of antigenic determinants recognized by rheumatoid arthritis-specific autoantibodies. J Clin Invest 101: 273-281.
-
Girbal-Neuhauser E, Durieux JJ, Arnaud M, Dalbon P, Sebbag M, et al. (1999) The epitopes targeted by the rheumatoid arthritis-associated antifilaggrin autoantibodies are posttranslationally generated on various sites of (pro) filaggrin by deimination of arginine residues. J Immunol 162: 585-594.
-
Vossenaar ER, Radstake TR, van der Heijden A, van Mansum MA, Dieteren C, et al. (2004) Expression and activity of citrullinating peptidylarginine deiminase enzymes in monocytes and macrophages. Ann Rheum Dis 63: 373-381.
-
Vossenaar ER, Despr�s N, Lapointe E, van der Heijden A, Lora M, et al. (2004) Rheumatoid arthritis specific anti-Sa antibodies target citrullinated vimentin. Arthritis Res Ther 6: R142-150.
-
Kinloch A, Tatzer V, Wait R, Peston D, Lundberg K, et al. (2005) Identification of citrullinated alpha-enolase as a candidate autoantigen in rheumatoid arthritis. Arthritis Res Ther 7: R1421-1429.
-
Matsuo K, Xiang Y, Nakamura H, Masuko K, Yudoh K, et al. (2006) Identification of novel citrullinated autoantigens of synovium in rheumatoid arthritis using a proteomic approach. Arthritis Res Ther 8: R175.
-
Suzuki A, Yamada R, Ohtake-Yamanaka M, Okazaki Y, Sawada T, et al. (2005) Anti-citrullinated collagen type I antibody is a target of autoimmunity in rheumatoid arthritis. Biochem Biophys Res Commun 333: 418-426.
-
Burkhardt H, Sehnert B, Bockermann R, Engstr�m A, Kalden JR, et al. (2005) Humoral immune response to citrullinated collagen type II determinants in early rheumatoid arthritis. Eur J Immunol 35: 1643-1652.
-
Takizawa Y, Suzuki A, Sawada T, Ohsaka M, Inoue T, et al. (2006) Citrullinated fibrinogen detected as a soluble citrullinated autoantigen in rheumatoid arthritis synovial fluids. Ann Rheum Dis 65: 1013-1020.
-
Snir O, Widhe M, von Spee C, Lindberg J, Padyukov L, et al. (2009) Multiple antibody reactivities to citrullinated antigens in sera from patients with rheumatoid arthritis: association with HLA-DRB1 alleles. Ann Rheum Dis 68: 736-743.
-
Arnett FC, Edworthy Sm, Bloch Da, McShane DJ, Fries JF, et al. (1998) The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum 31: 315-324.
-
Balsa A, Carmona L, Gonz�lez-Alvaro I, Belmonte MA, Tena X, et al. (2004) Value of Disease Activity Score 28 (DAS28) and DAS28-3 compared to American College of Rheumatology-defined remission in rheumatoid arthritis. J Rheumatol 31: 40-46.
-
Vaudo G, Marchesi S, Gerli R, Allegrucci R, Giordano A, et al. (2004) Endothelial dysfunction in young patients with rheumatoid arthritis and low disease activity. Ann Rheum Dis 63: 31-35.
-
Surdacki A, Martens-Lobenhoffer J, Wloch A, Gluszko P, Rakowski T, et al. (2009) Plasma asymmetric dimethylarginine is related to anticitrullinated protein antibodies in rheumatoid arthritis of short duration. Metabolism 58: 316-318.
-
Turiel M, Tomasoni L, Sitia S, Cicala S, Gianturco L, et al. (2010) Effects of long-term disease-modifying antirheumatic drugs on endothelial function in patients with early rheumatoid arthritis. Cardiovascular Therapeutics 28: 53-64.
-
Hjeltnes G, Hollan I, F�rre �, Wiik A, Mikkelsen K, et al. (2011) Anti-CCP and RF IgM: predictors of impaired endothelial function in rheumatoid arthritis patients. Scand J Rheumatol 40: 422-427.
-
Wang Y, Wysocka J, Sayegh J, Lee YH, Perlin JR, et al. (2004) Human PAD4 regulates histone arginine methylation levels via demethylimination. Science 306: 279-283.
-
Raijmakers R, Zendman AJ, Egberts WV, Vossenaar ER, Raats J, et al. (2007) Methylation of arginine residues interferes with citrullination by peptidylarginine deiminases in vitro. J Mol Biol 367: 1118-1129.
-
Darrah E, Rosen A, Giles JT, Andrade F (2012) Peptidylarginine deiminase 2, 3 and 4 have distinct specificities against cellular substrates: novel insights into autoantigen selection in rheumatoid arthritis. Ann Rheum Dis 71: 92-98.
-
Basu PS, Majhi R, Ghosal S, Batabyal SK (2011) Peptidyl-arginine deiminase: an additional marker of rheumatoid arthritis. Clin Lab 57: 1021-1025.
-
Zhang Y (2004) Molecular biology: no exception to reversibility. Nature 431: 637-639.
-
Cuthbert GL, Daujat S, Snowden AW, Erdjument-Bromage H, Hagiwara T, et al. (2004) Histone deimination antagonizes arginine methylation. Cell 118: 545-553.





