Clinical Medical
Reviews and Case Reports
Combined Lensectomy with Vitrectomy for Secondary Glaucoma and Traumatic Iridocyclitis after Ocular Blunt Trauma
Wei Xu, Zheng Wang and Ao Rong*
Department of Ophthalmology, Tongji Hospital, Tongji University School of Medicine, China
*Corresponding author: Ao Rong, M.D, Department of Ophthalmology, Tongji Hospital, Tongji University School of Medicine, 389 XinCun Road, Shanghai 200065, China, Tel: 86-21-66111047, Fax: 86-21-62282028, E-mail: weixutj@126.com
Clin Med Rev Case Rep, CMRCR-2-020, (Volume 2, Issue 3), Case Report; ISSN: 2378-3656
Received: February 12, 2015 | Accepted: March 07, 2015 | Published: March 10, 2015
Citation: Xu W, Wang Z, Rong A (2015) Combined Lensectomy with Vitrectomy for Secondary Glaucoma and Traumatic Iridocyclitis after Ocular Blunt Trauma. Clin Med Rev Case Rep 2:020. 10.23937/2378-3656/1410020
Copyright: © 2015 Xu W, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Keywords
Combined lensectomy with vitrectomy, Ocular blunt trauma, Secondary glaucoma, Traumatic iridocyclitis
Introduction
Traditional trabeculectomy has been the main surgery for many kinds of glaucoma [1]. However, it is of limitation and high risk in some cases. Vitrectomy is a significant microsurgery developed in the early 1970s. Anterior segment laceration and traumatic cataract is one of indications of vitrectomy [2]. Besides, malignant glaucoma, soft cataract, crystal located off the anterior chamber and vitreous cornea contact syndrome are also the adaptation disease. For the indications of posterior segment, they mainly include vitreous hemorrhage, intraocular foreign body, endophthalmitis and retinal detachment [2]. Recent advancement of technology in vitreous and cataract surgery systems enable certain surgeries, such as micro incision vitrectomy and cataract surgery, safer and less invasive [2,3]. The strategy that combines anterior with posterior segments procedure brings us a novel treatment for glaucoma. We present a case of traumatic glaucoma and traumatic iridocyclitis after an ocular blunt trauma due to aggressive assault by the fist, which was successfully treated with a 23 gauge (G) vitrectomy combined with phacoemulsification and artificial lens implantation.
Case Report
A 46-year-old Chinese male with a history of erythematous tender left eye with decreased vision acuity for 3+ weeks after aggressive assault by the fist was enrolled in the study. The protocol was performed with informed consent and following all the guidelines for investigations required by the Ethics Committee of Shanghai Tongji Hospital. Intraocular pressure (IOP) was 60mmHg (1mmHg=0.133kPa) O.S. at outpatient service. The eye symptoms alleviated slightly after administration of glaucoma medication: injection Mannitol 20% 250ml stat followed by topical Timolol maleate 0.5% twice-a-day and Brimonidine tartrate 0.2% twice a day. He had a history of uveitis, O.U. and rheumatoid arthritis for more than 30 years.
The patient had swollen left eyelids with conjunctiva injection, ciliary flushes of the left eye and cornea edema with keratic precipitate (KP)�s. The vision acuity was 1.2, O.D.; counting fingers only, OS and IOP was 14 mmHg, O.D. and 40.4 mmHg, OS. The left eye had shallow anterior chamber (AC), central 1 mm, peripheral ac closed. There was anterior chamber flare, posterior synechia with irregular and a fixed pupil about 1 mm in diameter, probably cloudy lens. Fundus could not be viewed, and cloudy vitreous was detected by B-scan. Anterior segment optical coherence tomography (OCT) revealed central AC 0.8 mm, anterior chamber angle closed. The diagnosis was made as secondary glaucoma O.S. and chronic traumatic iridocyclitis, O.U.
Initially, the patient was treated with glaucoma medication: Topical Timololmaleate 0.5% twice-a-day, Brimonidine tartrate 0.2% twice-a-day and Travoprost 0.004% once-a-day. But IOP did not descendmore after 4 days� treatment. Combined lensectomy with vitrectomy were implemented afterwards. To lower the high IOP, the incision was performed at 3.5- 3.8 mm from limbus at 8 o�clock, using 23G vitretor for anterior vitrectomy. The IOP was successfully relieved. Irrigation needle was inserted to keep normal eye pressure. Papillary membrane was removed following a superior 3 mm cornea incision. Viscoat was introduced into the anterior chamber, and pupil was dilated to 5.5mm. Lens was found mildly cloudy and subluxated, so cataract was removed using phaco technique after anterior capsularexis. Posterior chamber intraocular lens (PC IOL) was inserted into capsular bag, and cornea incision was closed with one interrupted 10-0 nylon suture. Additional sclera incision was made at 2 o�clock and 10 o�clock using 23 G knife, for illumination and 23G needle vitrector, respectively. Plenty of inflammatory exudation in posterior vitreous was found by a non-contact wide-angle viewing system (Resight�, Carl Zeiss, Oberkochen, Germany). Complete vitrectomy was performed. Optic nerve head had sharp disc margin with normal color. Retina was flat, without bleeding, edema or exudates. Viscoelastic material was removed from anterior chamber. Eye pressure was rechecked by FP. No intraoperative or postoperative complications were encountered.
Inflammatory exudation in anterior chamber was found the next day and treated with dexamethasone 10mg, IV; eye drops of tobramycin and dexamethasone (TobraDex, Alcon) and tropicamide. The best-corrected visual acuity recovered to 0.5 O.S. IOL was in good position and IOP was 14.3 mmHg. Anterior OCT indicated that central AC was 3.86 mm and anterior chamber angle was open (Figure 1). At 3 month follow-up, the visual acuity remained 0.5 and IOP was normal without symptoms of traumatic iridocyclitis of the left eye.
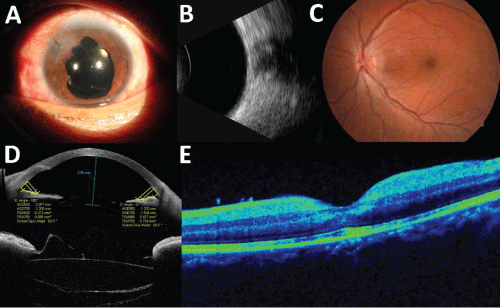
Figure 1: Improved results at 1 day after operation.
A: slit lamp, B: ultrasound, C: ophthalmoscope, D: anterior segment optical coherence tomography, E: posterior segment optical coherence tomography
View Figure 1
Discussion
This is the first case of secondary glaucoma and traumatic iridocyclitis in an eye after ocular blunt trauma that was successfully treated by combining lensectomy with vitrectomy. The case we reported revealed that, for secondary glaucoma cases merged with traumatic iridocyclitis, combining surgery had the potential to control IOP more effectively and to improve postoperative visual function faster compared with the sequential operation. It also strengthened the safety of high pressure operation, reduced the times of trauma surgery and shortened the course of the disease.
In recent years, studies revealed that the clinical magnification of iridocyclitis was far more complicated than what was described by Fuchs [1-3]. In comparison with other infectious, autoimmune or genetic eye disease, there is no confirmed laboratory method for iridocyclitis yet, and also lacking of conclusive evidence to substantiate its pathogenesis. Based on the current theories, iridocyclitis may not result from a single factor, but caused by a group of different diseases with similar magnificence. Another possibility is that iridocyclitis is caused by various factors including infection, immunity etc., and ultimately goes through a particular way, such as sustained secondary immune response [4,5]. In general, it is complex and difficult to treat glaucoma secondary to blunt trauma, and there are various options based on different situation [3]. For the case we presented, severe tunica pigmentosa response to trauma could cause occlusion of pupil, blockage of aqueous humor circulation, and elevated the IOP of traumatic eye. Another culprit could be lens dislocation, pushing iris forward and blocking the anterior chamber angle. In a conventional way, we would perform the trabeculectomy or lensectomy to reduce IOP when drugs didn�t work. However, it is of high risk to operate trabeculectomy or lensectomy, which could cause severe complications such as explosive cavity bleeding on the choroid [4].
The integrated idea inspires us to combined lensectomy with vitrectomy to treat glaucoma. We gave a priority to vitrectomy of anterior segments to lower IOP within normal range, herein assuring the safety of the follow-up operation. This method is suitable for almost all high intraocular pressure condition in eye surgery, such as implementation of trabeculectomy glaucoma or cataract combined with glaucoma surgery and so on.
For the implementation of lensectomy, resection of the pupil membrane could relieve pupillary blockage. Resection of lens subluxation, on the other hand, reopened the chamber angle and normalized aqueous humor circulation. Moreover, the implant of artificial crystal with great elasticity and tension increased the stability of lens bag [5]. To further increase the security, capsular tension ring could also be implanted simultaneously when necessary, preventing the occurrence of postoperative intraocular lens eccentric.
The vitrectomy of posterior segments still remained dispute. Traditionally, conservative treatment is a preferred choice, and surgery is under reconsideration when postoperative patients remain visual obstacle. Nevertheless, our case presented higher density shadow in posterior segment vitreous body by preoperative ultrasound, which suggested uveitis inflammatory infiltrates or vitreous hemorrhage. So conservative treatment would extend the course of the disease, induce psychological pressure and increase the economic burden.
The merits of combining surgery were as follows. First, vitrectomy made iris diaphragm retreat, further effectively reducing intraocular pressure. At the same time, it enabled us to identify the essence of higher density shadow in the shortest possible time and then to intervene surgery. For example, if higher density shadow was uveitis inflammatory exudation, surgery could help remove allergens to speed up the treatment cycle. If higher density shadow was vitreous hemorrhage, surgery could help find fundus lesions and then applied intraocular photocoagulation treatment, etc. Besides, it quickly improved the postoperative visual acuity, promoting visual rehabilitation. Finally, it effectively reduced the times of operation as well as the economic burden of patients with secondary surgery and mental pressure, which was a preferred acceptance for patients. Our case highlights the novel approach combined lensectomy with vitrectomy to be a potential alternative of traditional trabeculectomy for treating traumatic glaucoma and traumatic iridocyclitis.
References
-
Jea SY, Francis BA, Vakili G, Filippopoulos T, Rhee DJ (2012) Ab interno trabeculectomy versus trabeculectomy for open-angle glaucoma. Ophthalmology 119: 36-42.
-
Enaida H, Kadonosono K, Emi K, Inoue M, Someya K, et al. (2013) New micro forceps with high utility for various uses in microincision vitrectomy surgery. Retina 33: 244-246.
-
Tse DM, Titchener AG, Sarkies N, Robinson S (2009) Acute angle closure glaucoma following head and orbital trauma. Emerg Med J 26: 913.
-
Ono T, Yuki K, Ozeki N, Shiba D, Tsubota K (2013) Ocular surface complications after trabeculectomy: incidence, risk factors, time course and prognosis. Ophthalmologica 230: 93-99.
-
Lee SW, Seo JM, Ha S, Kim ET, Chung H, et al. (2009) Development of microelectrode arrays for artificial retinal implants using liquid crystal polymers. Invest Ophthalmol Vis Sci 50: 5859-5866.





