Clinical Medical
Reviews and Case Reports
Effect of Cardiac Resynchronization Therapy on Left Ventricular Diastolic Function
Kammoun Ikram*, Marrakchi Sonia, Jebri Faten and Kachboura Salem
Department of cardiology, Ariana hospital, Tunisia
*Corresponding author: Kammoun Ikram, Department of Cardiology, Ariana hospital, Tunisia, Tel: 21698644048, E-mail: kammounikram@yahoo.fr
Clin Med Rev Case Rep, CMRCR-2-022, (Volume 2, Issue 3), Research Article; ISSN: 2378-3656
Received: August 27, 2014 | Accepted: March 19, 2015 | Published: March 23, 2015
Citation: Ikram K, Sonia M, Faten J, Salem K (2015) Effect of Cardiac Resynchronization Therapy on Left Ventricular Diastolic Function. Clin Med Rev Case Rep 2:022. 10.23937/2378-3656/1410022
Copyright: © 2015 Ikram K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Aims: Cardiac Resynchronization Therapy (CRT) improves systolic performance in Heart Failure (HF). However, the effects of CRT on Left Ventricular (LV) diastolic function were variable and not fully understood. The aim of this study was to determine the effects of cardiac resynchronization therapy on LV diastolic filling pattern and the relation between the diastolic filling pattern and the response to CRT.
Methods and Results: Twenty nine patients (mean age, 66 ± 8 years; 26 men; mean LV ejection fraction 25±7%) with severe HF were included. Measurements included LV volumes and Ejection Fraction (EF), pulsed-wave Doppler (PWD)-derived transmitral filling indices (E- and A-wave velocities, E/A ratio, Ewave deceleration time).
Clinical responders were defined as survived patients with an improvement by one or more NYHA functional class, echocardiographic response to CRT was defined as a decline in LV end-systolic volume >15% during follow-up. In clinical responder group, both diastolic and systolic LV volumes decreased significantly (p=0.02 and p< 0.001 respectively) and LVEF increased significantly (p=0.001) in 26 of 29 patients (89%) and were accompanied by reduction in mitral E-wave velocity and E/A ratio (both p< 0.001), and increased A-wave velocity and Ewave deceleration time (p=0.03 and p< 0.001). In echocardiographic responders, reverse remodelling (52%) was coupled to the improvement in LV diastolic function but diastolic filling pattern improved also in 42% in patients without reverse remodelling.
Conclusion: Left ventricular diastolic indices after CRT improved in the clinical responder group, but there was no significant change in these indices among non-responders. CRT enhances diastolic filling patterns in both echocardiographic responder and nonresponder patients. This may be related to improvement in symptoms even in echocardiographic nonresponders who were clinical responders.
Keywords
Cardiac resynchronization therapy, Responders, Diastolic function
Introduction
Cardiac Resynchronization Therapy (CRT) can be an adjunctive treatment in patients with medically refractory heart failure symptoms, severe Left Ventricular (LV) systolic dysfunction, and an interventricular conduction delay.
CRT has been shown to improve symptom class, exercise capacity, quality of life, and systolic function [1]. The LV diastolic function is physiologically coupled to LV systolic performance and is an important determinant of symptoms and outcomes in patients with LV systolic dysfunction [2]. The effects of CRT on LV filling velocities (E-wave, E/A ratio) and Deceleration Time (DT) have been variable [3-5].
The aims of this study were to evaluate the effects of CRT on LV diastolic filling pattern and to whether an association existed between improvement of LV diastolic function and the response to CRT.
Methods
Study population
A total of 29 patients (mean age, 66 ± 8 years, 86% male) with New York heart Association (NYHA) functional class III or IV HF symptoms despite maximal medical therapy, LV ejection fraction ≤35%, sinus rhythm, and intraventricular echocardiographic asynchrony were enrolled in the study, between June 2004 and April 2008.
Clinical evaluation
Clinical evaluation included assessment of NYHA class, and measurement of the QRS duration on the surface ECG using the widest QRS complex.
Echocardiography
A commercially available ultrasound system was used (Aloca 5000 and ATL 3000) for the echocardiography studies. Two-dimensional (2D) measurements included LV volumes at end-diastole and end-systole from the apical four and two-chamber views (method of discs), LVEF calculated by the biplane method, The PWD-derived transmitral velocities were obtained at the mitral leaflet tips according to American Society of Echocardiography guidelines [6]. Measurements included the early diastolic (E) and atrial (A) wave velocities, the E/A ratio, and the E-wave DT. Mitral regurgitation was assessed by PISA method to determine ERO (effective regurgitant orifice) and RV (regurgitant volume). The extent of intraventricular dyssynchrony was defined if the maximal difference between the time intervals from Q-wave to peak Sm at each annular site is superior to 65ms [7] or if there is an overlap of the lateral wall [8].
CRT device implantation
CRT device implantation included pacemaker-only and -defibrillator CRT devices. First, the Right Ventricular (RV) lead was implanted using the cephalic vein or the subclavian vein. The LV pacing lead was inserted transvenously via the subclavian route if an appropriate coronary sinus branch was present. Otherwise, an epicardial approach was used and the lead was placed at the lateral LV free wall using a limited thoracotomy. The right ventricular lead was positioned at the apex and the right atrial lead in the atrial appendage.
Definition of response
Clinical responders were predefined as survived patients with an improvement by one or more NYHA functional class. Echocardiographic responders were those who reduced LV end-systolic volume by >15% during follow-up.
Statistical analysis
All statistical analysis was performed using SPSS software (version 15.0); continuous variables are expressed as mean ± one standard deviation. A comparison of the clinical and echocardiographic variables prior to and after CRT was performed using paired and unpaired Student t test and Pearson correlations as appropriate. Statistical significance was determined as a p value of < 0.05.
Results
Clinical parameters
29 patients (age 66 ± 8 years, 86% male) were included. The aetiology of heart failure was primarily nonischemic (79%). Medications included angiotensin-converting enzyme inhibitors in 89%, beta-blockers in 76% and potassium-sparing diuretics in 48%.
The QRS duration was prolonged (≥120ms) in 65% (left bundle branch block in 18 and non specific intraventricular conduction disturbance in one patient).
The LV pacing lead was placed in a mid-lateral or posteriolateral vein in the majority of patients (86%), and 4 patients� required thoracotomy. 6 patients (20%) had an implantation of a pacemaker-defibrillator. There were no complications from CRT device implantation.
All patients were restudied at a mean of 8 ± 2 months after CRT; 26 (89%) were clinical responders. These clinical responders were often in class III of NYHA (62%), with non ischemic aetiology (73%).
Echocardiographic parameters
The echocardiographic parameters of all patients are resumed in the Table 1. LV end-diastolic and end-systolic diameters and volumes decreased significantly in the clinical responder group (70 ± 5 vs 67 ± 10mm, p=0.02 and 61 ± 8 vs 55 ± 10mm, p< 0.001 respectively for diameters, 181 ± 56 vs 150 ± 52ml, p=0.02 and 138 ± 49 vs 104 ± 50ml, p< 0.001 respectively for volumes).
![]()
Table 1: Baseline echocardiographic characteristics of the patients
View Table 1
The LV ejection fraction increases significantly only in responder group (26 ± 5 vs 34 ± 12, p=0.001). The PWD-derived parameters of diastolic function improved significantly (decreased E-wave velocity and E/A ratio; increased A-wave velocity and DT) in the clinical responder group (Table 2) (Figure 1 and Figure 2).
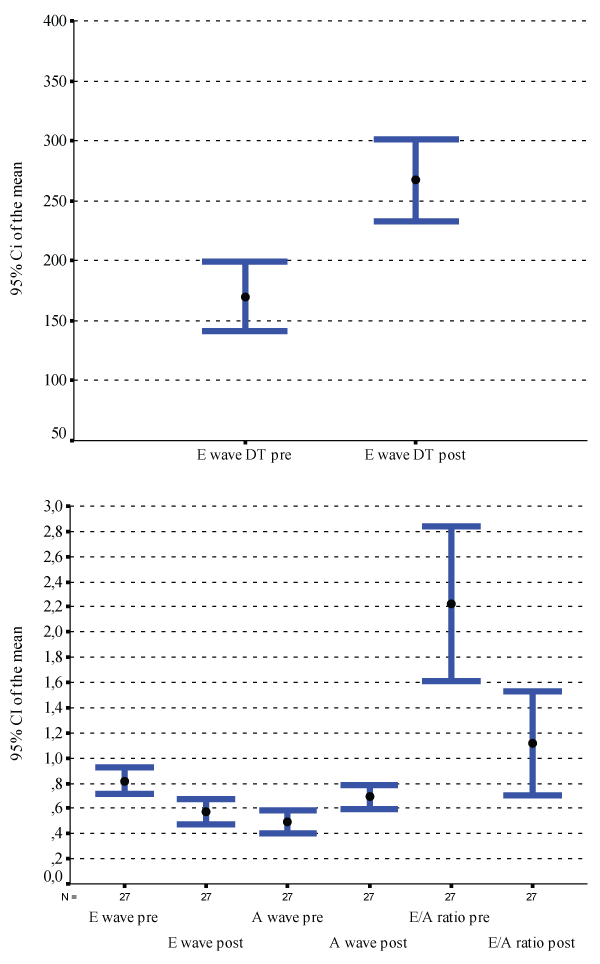
Figures 1 and 2: A significant improvement of diastolic parameters after CRT in clinical responders
View Figures 1 and 2
![]()
Table 2: The PWD-derived parameters of diastolic function improved significantly
in the clinical responder group.
View Table 2
A restrictive diastolic filling pattern before CRT was noted in 16 patients (55%) and did not predict clinical response (p=0.15). It was more frequent in echocardiographic nonresponders (63% versus 37%) but remained insignificant (p=0.08). A cut-off value of DT at 180ms predict significantly an echocardiographic response (p=0.017).
Reverse remodelling, occurring in 52%, was coupled to the improvement in LV diastolic function in all patients (Figure 3 and Figure 4) but diastolic filling pattern improved also in (6/11) in clinical responders without reverse remodelling , and parameters of diastolic function (Ewave, E/A ratio and Ewave DT) were significantly improved even in non echocardiographic responders (Table 3).
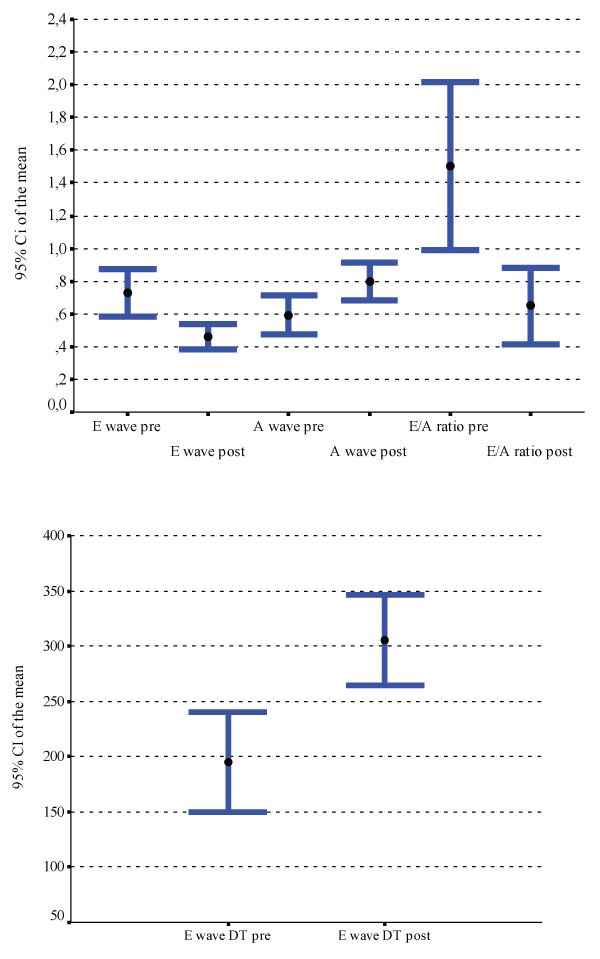
Figures 3 and 4: Improvement of diastolic parameters in echocardiographic responders
View Figures 3 and 4
![]()
Table 3: Comparison of echocardiographic parameters between echocardiographic responders and non-responders
View Table 3
Then CRT enhances diastolic filling patterns in both echocardiographic responder and nonresponder patients. This may be related to improvement in symptoms even in echocardiographic nonresponders who are clinical responders.
Discussion
Cardiac Resynchronization Therapy (CRT) has become a therapeutic option for patients with severe heart failure (HF), particularly in cases that are refractory to conventional medical treatment [9,10].
Various studies have demonstrated improvement in functional class and quality of life, with increased exercise tolerance and fewer hospitalizations for heart failure and, as shown in the CARE-HF trial, reduced mortality [1,9]. The effects of CRT on LV diastolic function were less studied.
The main findings of our study are as follows: the PWD-derived parameters of diastolic function improved significantly in the clinical responder group and diastolic filling pattern improved in 42% in patients without reverse remodelling, and then CRT enhances diastolic filling patterns in both echocardiographic responder and nonresponder patients.
Prior studies that have evaluated the effects of CRT on LV diastolic function by use of PWD-derived transmitral filling parameters have reported variable results; the mitral E-wave velocity or E/A ratio may not be significantly altered [11-13].
Other investigations have reported that the PWD-derived E-wave velocity decreases after CRT [14,15]. Deceleration slope and deceleration time of the E-wave increased significantly at 3 and 6 months in the CRT group but did not change in the control group which is consistent with improved diastolic function in the CRT group [15]. Waggoner showed that CRT decreases the mitral E-wave velocity and the E/A ratio only in those patients who exhibit significant decreases in LV volumes and significant improvements in LVEF [16].
In our study, reverse remodelling, occurring in 52%, was coupled to the improvement in LV diastolic function but diastolic filling pattern improved also in 42% in patients without reverse remodelling, then enhancement of diastolic filling patterns after CRT may explain improvement in symptoms in the absence of reverse remodelling.
Similar to our results, Jansen and Aksoy suggested that patients with reverse remodelling and symptomatically improved patients without reverse remodelling showed decreased filling pressures after CRT [17,18]. Recently, Doltra�s study demonstrated that patients with clinical but no echocardiographic response had significant improvement in E-wave and deceleration time and non significant improvement in other parameters [19].
In our study, the restrictive diastolic filling pattern before CRT was more frequent in echocardiographic non responders (63% versus 37%). The more frequent restrictive mitral patterns in the non responders suggests that these patients were at a more advanced stage of heart failure, which was confirmed by their higher pro-BNP and lower oxygen consumption in Galrinho�s study [20]. Then, diastolic function before CRT must be more studied as a predictor for response after CRT.
Study Limitations
The major limitation of this study is the relatively small sample size. One third of the patients had a QRS duration < 120ms and inclusion criteria for CRT were based on the mechanical asynchrony but this may be explain the high rate of clinical response. Inclusion period was before the publication of PROSPECT study which not supported echocardiographic criteria.
Conclusion
Cardiac resynchronization therapy improves LV diastolic filling in the clinical and echocardiographic responders. Enhancement of diastolic filling pattern in clinical responders without reverse remodelling may explain improvement of symptoms in these patients.
References
-
Bradley DJ, Bradley EA, Baughman KL, Berger RD, Calkins H, et al. (2003) Cardiac resynchronization and death from progressive heart failure. A meta-analysis of randomized controlled trials. JAMA 289: 730-740.
-
Rihal CS, Nishimura RA, Hatle LK, Bailey KR, Tajik AJ (1994) Systolic and diastolic dysfunction in patients with clinical diagnosis of dilated cardiomyopathy. Relation to symptoms and prognosis. Circulation 90: 2772-2779.
-
Lau CP, Yu CM, Chau E, Fan K, Tse HF, et al. (2000) Reversal of left ventricular remodeling by synchronous biventricular pacing in heart failure. Pacing Clin Electrophysiol 23: 1722-1725.
-
Linde C, Leclercq C, Rex S, Garrigue S, Lavergne T, et al. (2002) Long-term benefits of biventricular pacing in congestive heart failure: results from the MUltisite STimulation in cardiomyopathy (MUSTIC) study. J Am Coll Cardiol 40: 111-118.
-
St John Sutton MG, Plappert T, Abraham WT, Smith AL, DeLurgio DB, et al. (2003) Effect of cardiac resynchronization therapy on left ventricular size and function in chronic heart failure. Circulation 107: 1985-1990.
-
Qui�ones MA, Otto CM, Stoddard M, Waggoner A, Zoghbi WA; Doppler Quantification Task Force of the Nomenclature and Standards Committee of the American Society of Echocardiography (2002) Recommendations for quantification of Doppler echocardiography: a report from the Doppler Quantification Task Force of the Nomenclature and Standards Committee of the American Society of Echocardiography. J Am Soc Echocardiogr 15: 167-184.
-
Bax JJ, Marwick TH, Molhoek SG, Bleeker GB, van Erven L, et al. (2003) Left ventricular dyssynchrony predicts benefit of cardiac resynchronization therapy in patients with end-stage heart failure before pacemaker implantation. Am J Cardiol 92: 1238-1240.
-
Cazeau S, Bordachar P, Jauvert G, Lazarus A, Alonso C, et al. (2003) Echocardiographic modeling of cardiac dyssynchrony before and during multisite stimulation: a prospective study. Pacing Clin Electrophysiol 26: 137-143.
-
Rivero-Ayerza M, Theuns DA, Garcia-Garcia HM, Boersma E, Simoons M, et al. (2006) Effects of cardiac resynchronization therapy on overall mortality and mode of death: a meta-analysis of randomized controlled trials. Eur Heart J 27: 2682-2688.
-
Abraham WT (2006) Cardiac resynchronization therapy. Prog Cardiovasc Dis 48: 232-238.
-
Porcianai MC, Puglisi A, Colella (2000) Echocardiographic evaluation of the effect of biventricular pacing: the In-Sync Italian Registry. Eur Heart J: J23-30.
-
Yu CM, Fung WH, Lin H, Zhang Q, Sanderson JE, et al. (2003) Predictors of left ventricular reverse remodeling after cardiac resynchronization therapy for heart failure secondary to idiopathic dilated or ischemic cardiomyopathy. Am J Cardiol 91: 684-688.
-
Saxon LA, De Marco T, Schafer J, Chatterjee K, Kumar UN, et al. (2002) Effects of long-term biventricular stimulation for resynchronization on echocardiographic measures of remodeling. Circulation 105: 1304-1310.
-
Yu CM, Chau E, Sanderson JE, Fan K, Tang MO, et al. (2002) Tissue Doppler echocardiographic evidence of reverse remodeling and improved synchronicity by simultaneously delaying regional contraction after biventricular pacing therapy in heart failure. Circulation 105: 438-445.
-
St John Sutton MG, Plappert T, Abraham WT, Smith AL, DeLurgio DB, et al. (2003) Effect of cardiac resynchronization therapy on left ventricular size and function in chronic heart failure. Circulation 107: 1985-1990.
-
Waggoner AD, Rovner A, de las Fuentes L, Faddis MN, Gleva MJ, et al. (2006) Clinical outcomes after cardiac resynchronization therapy: importance of left ventricular diastolic function and origin of heart failure. J Am Soc Echocardiogr 19: 307-313.
-
Jansen AH, van Dantzig Jm, Bracke F, Peels KH, Koolen JJ, et al. (2007) Improvement in diastolic function and left ventricular filling pressure induced by cardiac resynchronization therapy. Am Heart J 153: 843-849.
-
Aksoy H, Okutucu S, Kaya EB, Deveci OS, Evranos B, et al. (2010) Clinical and echocardiographic correlates of improvement in left ventricular diastolic function after cardiac resynchronization therapy. Europace 12: 1256-1261.
-
Doltra A, Bijnens B, Tolosana JM, Gabrielli L, Castel M�, et al. (2013) Effect of cardiac resynchronization therapy on left ventricular diastolic function: implications for clinical outcome. J Card Fail. 19: 795-801.
-
Galrinho A, Branco LM, Oliveira MM, Da Silva N, Abreu J, et al. (2009) Cardiac resynchronization therapy--clinical and echocardiographic characteristics of responders and exceptional responders. Rev Port Cardiol 28: 959-969.





