Clinical Medical
Reviews and Case Reports
Symptomatic Cervical Perineural (Tarlov) Cyst: A Case Report
Zibis H. Aristeidis1*, Fyllos C. Apostolos2 and Arvanitis L Dimitris1
1Department of Anatomy, Medical School, University of Thessaly, Greece
2Department of Orthopedics, General Hospital of Karditsa, Greece
*Corresponding author:
Zibis H. Aristeidis, University of Thessaly, School of Health Sciences, Department of Anatomy Panepistimiou Biopolis , 41110, Larisa, Greece, Tel: +306977228250, Fax: +302410289266, E-mail: ahzibis@gmail.com
Clin Med Rev Case Rep, CMRCR-2-030, (Volume 2, Issue 5), Case report; ISSN: 2378-3656
Received: March 18, 2015 | Accepted: May 20, 2015 | Published: May 23, 2015
Citation: Aristeidis ZH, Apostolos FC, Dimitris AL (2015) Symptomatic Cervical Perineural (Tarlov) Cyst: A Case Report. Clin Med Rev Case Rep 2:030. 10.23937/2378-3656/1410030
Copyright: © 2015 Aristeidis ZH, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Perineural cysts, also known as Tarlov cysts, are benign cerebrospinal fluid-filled cysts of the spinal cord. They were first described by IM Tarlov in 1938.
Case presentation: We describe a Tarlov cyst located in the cervical spine, a location quite rare in literature. The patient is a 44-year-old woman who presented with a 3-week history of radicular symptoms of the right C6 root. A perineural cyst was identified at the C5-6 level after Magnetic Resonance Imaging of the cevical spine. A conservative approach was chosen, with the use of a soft collar for two weeks, a 15-day course of oral non-steroidal anti-inflammatory medication and specific instructions concerning limitation of her activities. After two weeks of this conservative treatment the patient had no pain and 90% improvement of her numbness. During 12 months follow up she was satisfied with no pain, no recurrent symptoms and no need for any additional treatment.
Conclusions: In this case report, we include a different clinical and therapeutic approaches of Tarlov cysts, regardless of their location (lumbosacral, cervical). This is the first case report of a cervical Tarlov cyst treated conservatively without the use of oral or injected steroids. We would also like to suggest the inclusion of a perineural cyst in the differential diagnosis of any patient presenting with radicular symptoms. Finally, we discuss briefly any literature that we considered relevant in history, diagnosis and treatment of perineural cysts.
Keywords
Perineural cyst, Tarlov cyst, Diagnosis, Management, Radiculopathy, Pseudoradiculopathy
Introduction
Perineural cysts, also known as Tarlov cysts from the name of the first author who described them in 1938 as incidental findings during autopsy, are benign Cerebrospinal Fluid (CSF)-filled cysts of the spinal cord [1]. Although these cysts are often multiple and appear on dorsal nerve roots almost along the spinal cord, they are most often found in the sacral spine and they can be asymptomatic [2-4]. Magnetic Resonance Imaging (MRI) is currently the gold standard modality for detection [5].
This is a case report of a patient suffering from radicular symptoms caused by a perineural cyst located in the cervical spine. To our knowledge, only four other cases of symptomatic cervical perineural cysts have been published [6-9].
Case Report
A 44-year-old woman presented with a 3-week history of gradually developing radicular symptoms of the right C6 root. She was complaining about pain 8/10 on Visual Analogue Scale (V.A.S.) in the lateral side of her right forearm and constant burning sensation and numbness of her right index finger. There was no history of trauma. As far as her past medical history is concerned, there were no previous chronic problems, no previous hospital admissions and there was no history of chronic use of any medication. The patient was a heavy smoker. On examination, all deep tendon reflexes were normal. Muscle strength of all upper extremity myotomes was 5/5. Pinprick sensation, light touch sensation, vibration sensation of C5-8, T1 distribution was intact. There was positive response of the Hoffmann's reflex and aggravation of symptoms when tilting the head to the left (opposite direction of the affected nerve root). The patient did not recall any other aggravating or relieving factors. There were no previous visits to other medical facilities for the complaint in question. An MRI of the cervical spine was requested. The radiologist confirmed there was a small disc bulging causing a minor degree stenosis of both foramina as well as the presence of a perineural cyst on the right on the C5-C6 level, near the dorsal ganglion (Figure1). The perineural cyst was considered the cause of the problem as it could explain the patient's symptoms. The patient was treated with a 2-week course of non-steroidal anti-inflammatory drugs (NSAIDs), the use of a soft collar and was asked to limit her activities, especially avoid extreme stretch of her arm and neck. The NSAID used was lornoxicam 8mg twice a day. After the 2 week-course of conservative therapy, there was no pain on the VAS and there was a 90% improvement of burning sensation and numbness. After initial relief of symptoms, physical therapy and changes in her lifestyle were encouraged. Last follow up after 12 months was preservation of an excellent outcome without any pain and recurrence of numbness in her index finger in certain extreme positions of her cervical spine. The patient was happy with the outcome of this approach and there was no need for any further action to be taken.
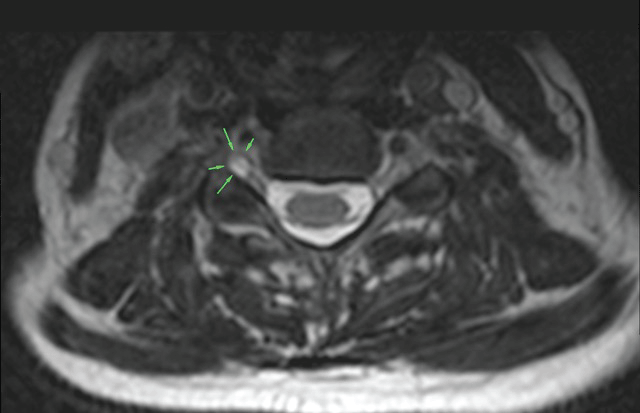
.
Figure 1: View of axial T2 weighted sequence MRI at C5-C6 level, perineural cyst on the right at the C5-C6 level, near the dorsal ganglion around the nerve root (arrows).
View Figure 1
Discussion
Perineural cysts begin in the perineural space between the endoneurium derived from the pia matter and the perineurium formed by the arachnoidal matter [4]. They occur along the nerve roots, at or distal to the junction of the posterior root and the dorsal ganglion [4]. Their wall consists of nerve fibers and/or ganglion cells [2,10]. They have been described as "extradural meningeal cysts with nerve root fibers" (type II) and they are believed to communicate with the subarachnoid space by Nabors et al. [2], in spite of other authors objections [4,10].
They are most often found in the sacral spine with a prevalence of 4.6% in a symptomatic population based on a retrospective review of MRIs of the lumbosacral spine [3]. Should they raise any symptoms, those depend on their location in the proximity of a specific nerve root. Rupture of a Tarlov cyst, rare as it may be, should be considered in patients with cerebral fat embolism, particularly after lower back trauma [11].
As far as the pathophysiology of symptoms raised is concerned, a ball-valve mechanism has been suggested and described. Cysts created by the dilated sheaths usually have microconnections to the subarachnoid space. However, when pulsatile and hydrodynamic forces of CSF cause these cysts to fill and expand in size, they can begin to compress neighboring nerve fibers, resulting in neurological symptoms [12]. The ball-valve theory has been previously postulated as the reason why some large Tarlov cysts cause symptoms that progress whereas others cause only mild symptoms [5]. The onset of symptoms can be sudden or gradual. Usually, patients report that their symptoms are exacerbated by coughing, standing, and change of position. This can be explained by the increase in CSF pressure, leading to an activation of the aforementioned ball-valve mechanism. Symptomatic relief can usually be achieved by recumbent positioning [5].
MRI is currently the method of choice in diagnosis of perineural cysts. The findings that suggest the diagnosis of a perineural cyst are the demonstration of low signal on T-1 weighted images and high signal on T-2 weighted images, similar to CSF [5], as well as its shape and the vicinity of its location to the dorsal ganglion [7]. Myelography showing the filling of the meningocele sac 1 hour after injection of contrast medium is highly suggestive of a perineural cyst [4]. Myelography can have a role in detecting communication of the Tarlov cyst with the subarachnoid space [5].
Because Tarlov cysts are often incidental, the finding can lead to 3 different diagnostic options: 1) another pathology is causing symptoms 2) another pathology is probably causing symptoms, but the Tarlov cyst could be a secondary cause of the symptoms; or 3) the Tarlov cyst is the only pathological finding that can explain the symptoms. Obviously, this requires one to carefully evaluate the correlation between clinical and radiological findings [5].
The surgical options are: 1) diversion of CSF flow (CT-guided percutaneous aspiration and modifications, lumboperitoneal shunt) and 2) direct microsurgical approach (cyst fenestration, cyst imbrication, cyst neck ligation, cyst resection, and combinations of the above) [5]. Each option comes with certain complications such as cyst recurrence and aseptic meningitis of which our patient was thoroughly informed and wished to follow a conservative approach.
Conservative approach of a symptomatic cervical perineural cyst is very seldom described in literature. Mitra et al. specifically describe a conservative approach of a symptomatic cervical Tarlov cyst using oral steroids after initial ineffective course of NSAIDs, as well as epidural steroid injection for a symptomatic Tarlov cyst of the lumbosacral area. A 6-day course of oral steroids was chosen, leading to relief of symptoms as far as upper extremity motor strength is concerned, but with a slight increase in the patient's sense of pain [6]. Bayrakli more recently treated a symptomatic cervical Tarlov cyst with physical therapy and oral steroids [8].
Kim et al. performed a more invasive transforaminal epidural steroid injection for a case of symptomatic perineural cyst in the cervical spine [7]. Epidural steroid injection was primarily employed to reduce neural inflammation causing radicular symptoms, but the follow-up MRI revealed a shrunken cyst in this case, which was an unexpected result of the intervention. The previous study [6] in which steroid was interlaminarly injected, which could never mechanically damage the cyst, resulted in resolution of the cyst. This result implies that mechanisms other than structural disintegration could have reduced the size of the cyst. For example, injected steroid may reduce the oedema of surrounding structures, including the dorsal root ganglion, and relieve the obstruction of CSF efflux from the cyst as suggested by the "ball valve mechanism" [7]. Reducing oedema around the nerve root was the goal behind our approach as well. The cyst had probably been present around the nerve root in our patient for a long time, but gave no symptoms. This scenario is amplified by absence of symptoms at follow-up. Our patient's daily activities probably caused at some point nerve irritation due to proximity of the nerve root with cyst and surrounding structures that lead to inflammation, oedema and symptoms.
In our case, symptoms are most probably raised exclusively from the compression caused by a perineural cyst, making it exclusively responsible for the symptomatology of pseudoradiculopathy. We felt the need to treat this patient initially conservatively, since it was her first visit seeking medical attention for her symptomatology. Since symptomatology pointed towards mild nerve irritation without any muscle weakness, we decided against initial steroid therapy. Instead, we aimed at pain control and more mild anti-inflammatory agents such as NSAIDs. The spectacular improvement of our patients symptoms thanks to her compliance in therapy and relieving aggravating factors made any further intervention unnecessary for the time being. Consequently, significant clinical improvement in a symptomatic cervical perineural cyst after a course of oral NSAIDs suggests that this could be another option and a new entry in literature as far as a conservative approach is concerned in a symptomatic cervical Tarlov cyst.
Conclusion
We would like to clearly point out the clinical significance of attempting an initial conservative approach, including a soft collar, oral NSAIDs, oral and injected steroids, to any symptomatic perineural cyst, before advancing to a surgical intervention. Furthermore, the need to view the clinical entity of "the perineural cyst" as a whole considering the whole length of the spine is becoming more and more obvious, in order to agree to specific criteria and guidelines of treatment. We would like to propose that a Tarlov cyst should always be included in the differential diagnosis in any case of radicular symptoms rising from the lumbosacral or cervical spine, until proven otherwise by surgical or radio graphical diagnostic means. And even when another cause has been identified along with the incidental finding of a perineural cyst, the cyst should always be considered as a secondary cause to the symptoms.
References
-
Tarlov IM (1938) Perineurial cysts of the spinal nerve roots. Arch Neurol Psychiat (Chic) 40: 1067-1074.
-
Nabors MW, Pait TG, Byrd EB, Karim NO, Davis DO, et al. (1988) Updated assessment and current classification of spinal meningeal cysts. J Neurosurg 68: 366-377.
-
Paulsen RD, Call GA, Murtagh FR (1994) Prevalence and percutaneous drainage of cysts of the sacral nerve root sheath (Tarlov cysts). AJNR Am J Neuroradiol 15: 293-297.
-
Tarlov IM (1970) Spinal perineurial and meningeal cysts. J Neurol Neurosurg Psychiatry 33: 833-843.
-
Lucantoni C, Than KD, Wang AC, Valdivia-Valdivia JM, Maher CO, et al. (2011) Tarlov cysts: a controversial lesion of the sacral spine. Neurosurg Focus 31: E14.
-
Mitra R, Kirpalani D, Wedemeyer M (2008) Conservative management of perineural cysts. Spine (Phila Pa 1976) 33: E565-568.
-
Kim K, Chun SW, Chung SG (2012) A case of symptomatic cervical perineural (Tarlov) cyst: clinical manifestation and management. Skeletal Radiol 41: 97-101.
-
Bayrakli F, Kurtuncu M, Karaarslan E, Ozgen S (2012) Perineural cyst presenting like cubital tunnel syndrome. Eur Spine J 21: S387-389.
-
Joshi VP, Zanwar A, Karande A, Agrawal A (2014) Cervical perineural cyst masquerading as a cervical spinal tumor. Asian Spine J 8: 202-205.
-
Voyadzis JM, Bhargava P, Henderson FC (2001) Tarlov cysts: a study of 10 cases with review of the literature. J Neurosurg 95: 25-32.
-
Zubizarreta IK, Menoyo JL, Ojeda JR, Olabarria IV, Carra JC (2014) Cerebral fat embolisms secondary to rupture of a Tarlov cyst. J Neuroimaging 24: 432-433.





